Cements for PFM and All-Metal Restorations
A cementation guide to reduce confusion and bolster success
Dental cements are a critical link in the placement of many types of restorations in dentistry, but matching cements to the crown material can be challenging. Beyond improper or incorrect cement selection for the restorative material being cemented, poor technique during cementation of the restoration can lead to premature restoration failure. Although the initial cost involved in cementation—ie, time and material—is relatively low, the cost of restoration failure—requiring additional chairtime, laboratory fees, and other replacement costs—can be significant, making an understanding of cements and their application critical in restorative dentistry.
Choosing the Right Cement
For definitive cementation of metal and porcelain-fused-to-metal (PFM) restorations, as well as metal posts, water-based cements that undergo an acid-base setting reaction can be used. This class of cements includes the legacy cements—zinc phosphate, zinc polycarboxylate, and conventional glass ionomer cements—as well as the contemporary cement, resin-modified (resin-reinforced) glass ionomer. The fastest-growing category of definitive cements is resin-based cements with a chemistry based upon current composite resins and bonding adhesives1; they include self-adhesive composite resin cements, cements that require an additional bonding adhesive before placement, and compomer cements.
Within each class, these cements have physical properties that allow for a consistency appropriate for cementation and a film thickness that allows for complete seating of a restoration during cementation. Dental professionals should be aware that there is variability in the handling characteristics of each class of cement, and even differences within the same class of cement. They should not assume that cements within the same class are mixed and manipulated the same way, so it is essential that they read instructions related to material dispensing and mixing before use.2,3
Glass Ionomer Cements
Glass ionomers are the primary cement used for all-metal and PFM restorations, as they are excellent for teeth and metal implants, cast-metal post and cores, and for prefabricated metal posts. They are classified as either conventional glass ionomer cements—which are water-based without any resin—and resin-modified glass ionomer—which have approximately 10% resin added to the formula to improve physical properties. Both are adhesive to enamel and dentin via ionic chemical bonding of the glass ionomer to the calcium and phosphate ions of the tooth. An additional benefit of glass ionomers is the caries prevention provided by the fluoride they contain.
Conventional glass ionomers come as a powder and liquid that can either be hand dispensed for mixing on a mixing pad with a cement spatula or in a preloaded single-use capsule that is mixed in a mechanical mixer (eg, amalgamator, triturator). The capsule usually has a dispensing tip and the cement is syringed using an applicator gun onto the restoration and preparation. The applicator guns are usually manufacturer-specific. It is advisable not to clear away excess cement until it is fully set.
Resin-modified glass ionomers (also referred to as resin-reinforced and hybrid ionomer) are supplied as a powder-liquid, paste-paste, or a unit-dose mixing capsule with a dispensing tip. They are easier to mix than the conventional powder-liquid glass ionomer and have improved physical properties while retaining the properties of self-adhesion and fluoride release. Excess resin-modified glass ionomer cement can be cleared away when it reaches the gel stage or after complete setting. Resin-modified glass ionomer cements are less vulnerable to early moisture contamination.
When using glass ionomers, the tooth should not be over-dried, and the dentin should be lightly moistened using a microapplicator or a damp cotton pellet so it is slightly glossy with no water pooling of the surface.
Composite Resin Cements
This class of resin-based cements includes self-adhesive composite cements and multistep composite cements. These cements are relatively insoluble compared with other dental cements and have the highest mechanical physical properties, including high compressive strength, high flexural strength, good fracture toughness, low coefficient of thermal expansion and contraction, and the highest stiffness of any dental cement.1,3 These cements are based upon the chemistry of direct placement restorative composite resins and are wear- and abrasion-resistant.
Self-adhesive composite resin cements are the easiest to use for all-metal and PFM cementation because they don’t require the separate bonding agents and composite cement used with the multi-step cements. Self-adhesive composite cements are typically mixed with automixing tips or in unit-dose dispensed capsules.
Self-Adhesive Resin Cements
Self-adhesive resin cements can be used for all applications with zirconia and alumina core ceramics, cast metal, PFM, and for cementation of cast post and cores and prefabricated metal and fiber posts. These cements are dual-cure and allow an easy clean-up at a gel phase. Many of the cements in this category are available in dual-tube automixing configurations or in some cases in preloaded capsules that are mixed in a high-speed triturator.
Cementation Tips
Success with cementation depends on attention to detail. The tooth must be clean. The tooth preparation should be cleaned with either paste of pumice and water or a prophy paste using a prophy cup to remove all temporary cement (Figure 1). Isolation is critical to control all oral fluids.
For post cementation when restoring an endodontically treated tooth, some cements have small tips that can be snapped on the end of either an automixing tip or a unit-dose capsule for placement of the cement within the root canal. Another choice for ease of placement of cement into root canals is a needle tip–like delivery device created for this purpose.4
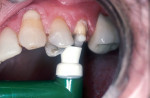
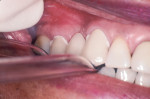
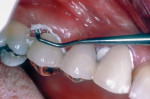
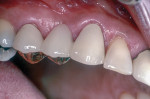
If cementing with a base metal (non-precious metal), whether all-metal or PFM, air abrading the metal surface adds to the retention of the crown (Figure 2). Research has shown that resin-based cements and resin-modified glass ionomers are thixotropic.5,6 When cementing with any of the contemporary cements, the patient should bite down on a stick or saliva ejector7 (Figure 3 and Figure 4).
Self-mixing cements and unit-dose mixed capsules provide for a more uniform mix for cementation. When automixing the cement directly into the crown, the first small increment from the mixing tip should be extruded onto a paper pad for disposal because it may not have equal amounts of base and catalyst. Once the cement is in the crown, the authors recommend using a disposable brush (not microbrush) to paint the cement over all internal surfaces and to make sure the cement is covering all the margins of the crown.
Conclusion
With the increase in the number of options for materials used for indirect restorations, the choices of what cement to use where has become more difficult and confusing for the clinician. Although no one cement fulfills all the needs for all cementation, understanding the differences between the classes of dental cements contributes to clinical success in restorative dentistry.
References
1. Platt JA. Resin-based luting cements. Compend Contin Dent Educ. 2000; 21(9):40-44.
2. Rosensteil SF. Luting agents and cementation procedures. In: Rosensteil SF, Land MF, Fujimoto J, eds. Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby Elsevier; 2006:909-927.
3. Strassler H, Suh BI, Wang Y. Compatibility of oxalate desensitizer with glass ionomer cements. J Dent Res. 2006;85(special issue A). 2006: Abstract #1885.
4. Strassler HE, Campbell R, Wycall B, VonFraunhofer JA. Evaluation of two techniques for cement application into root canals. J Dent Res. 2000;79 (IADR Abstracts): Abstract #2332.
5. Asmussen E, Attat J, Degrange M. Adherence of resin-based luting agents assessed by the energy of fracture. Acta Odontol Scand. 1993; 51(4):235-240.
6. Wang CJ, Millstein PL, Nathanson D. Effects of cement, cement space, marginal design, seating aid materials, and seating force on crown cementation. J Prosthet Dent. 1992;67(6):786-790.
7. Strassler HE, Levine E. Contemporary dental cements. In: Contemporary Esthetic Dentistry. Freedman GA, ed. Elsevier, St. Louis, MO; 2012:
537-546.
For “Cementation of Indirect Restorations: An Overview of Resin Cements,” visit: dentalaegis.com/go/id913
About the Authors
Howard E. Strassler, DMD, FADM, FAGD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Roseanna J. Morgan, CDA
Postgraduate Prosthodontics
University of Maryland Dental School
Baltimore, Maryland