Advancements in Hybrid Implant-Supported Restorations
Functional improvements yield more esthetic and durable dentition
The public’s perception of tooth loss is rapidly changing. The replacement of missing teeth in traditional dentistry focused on restoring the lost tooth with dentures and bridges to provide chewing function. This approach did not address the bone condition and prevent future bone loss, however. This bone loss often caused an “aging of the face.” Implantology has opened the door for people to be no longer dentally handicapped. Now they can look more attractive, be healthier, and live fuller lives. Patients’ demands for reaching those goals are increasing as well. They are looking for more lifelike results in a more affordable and efficient manner.
The evolution of materials and technology—a confluence of smile design, biomechanical engineering, and polymer chemistry—has enabled dental teams (ie, restorative dentists, surgeons, and lab technicians) to deliver better results than ever before. No longer does “guesswork” come into play for any immediate prosthetic restoration. Dehabilitation is no longer the norm; rehabilitation is the “new standard.”1
Case Presentation
A 54-year-old woman with a history of Bell’s palsy presented with a chief complaint of, “My front teeth are unstable and shifting, and I am ready to overhaul my teeth.” She was very anxious about pain and treatment effects on appearance and speech. Her previous dental history included generalized crown and bridge work that was esthetically compromised by refractory periodontal disease and two attempted surgical interventions. Over the previous 8 years, the patient had also received episodic care for inflammatory emergencies and bonding to repair root decay and esthetics. Functionally, signs of tooth wear were noted. Esthetically, the patient’s smile was not pleasing and gingival display was moderate. Furthermore, the Bell’s palsy had created an asymmetry in lip dynamics. Because the patient was very demanding, all these factors were noted for managing realistic expectations (Figure 1).2
Given the level of infection, it was agreed to remove the entire dentition and source of periodontal infection and start with immediate dentures that would promote more ideal conditions for implant reconstruction.3 Because the patient was not tolerant of the instability and contours of conventional dentures, she declined the classic sinus augmentation procedures and opted for a plan using NobelActive™ implants (Nobel Biocare, www.nobelbiocare.com). The plan called for using six upper and five lower implants following the American Academy of Implant Dentistry’s recommendations4 and a modified version of Balshi’s Teeth In A Day® protocol.1 In addition, pterygomaxillary implants would be placed distal to the sinus as they have been predictable in decreasing cantilever effects in the maxilla.5
Critical components to the success of hybrid prostheses involve creating enough restorative space above the implant to also create harmonious occlusion, esthetics, and function.6 Because implantology is more successful when it is prosthetically driven, it was critical to do careful presurgical planning not only radiographically, but also when creating a pretreatment facial analysis. This enabled the discovery of the patient’s critical factors in prosthodontic smile design and how to evaluate/capture those details while planning and performing her full-mouth rehabilitation.
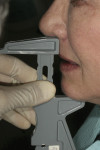
A Kois Dento-Facial Analyzer (Panadent, www.panadent.com) was used to carefully evaluate the vertical dimension/freeway space (Figure 2). The functional/esthetic relationship was then transferred to the laboratory. Esthetics were predictably established using the Stratos® Mounting Plate Plate (Ivoclar Vivadent Inc., www.ivoclarvivadent.com ) (Figure 3). In addition, as implant-supported restorations are nonresilient, proprioception is greatly different for patients who have a history of mobile natural teeth and/or removable prostheses. Therefore, it was critical to design an “implant-protected occlusion” that shared proprioception in protrusion while decreasing anterior wear and torque (Figure 4). Furthermore, the tooth selection must allow for the previous goals to be achieved.
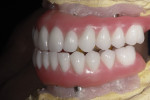
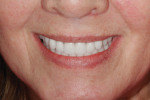
Fortunately, dental manufacturers have responded to meet this growing need in the marketplace. Mondial® teeth (Heraeus Kulzer, www.heraeus-dental.com) have lifelike color and texture, well-documented durability7,8 using 5% to 10% inorganic nanofillers (silica) that can handle the rigors of implant hybrid restorations, and an anatomic design that allows for lingualized axially directed bite forces that creates long-term results prosthetically and for the implants. For this patient, and many others, the future is bright (Figure 5).
Conclusion
The replacement of teeth with implants was once thought to be science fiction. Continual advancement in implant design, bone manipulation, bioengineering, and dental material allows dental professionals to help patients renew their lives with more esthetic and durable dentition.
Acknowledgments
The author would like to thank Robin Johnson, CDT, and Dr. Lawrence Sims for their contributions in successfully planning and performing this case.
References
1. Balshi TJ. Teeth in a day course presented at: The Institute For Facial Esthetics; January 16-17, 2012; Fort Washington, PA.
2. Mills EJ. A clinical method for the diagnosis and treatment planning of restorative dental patients . J Oral Implantol. 2002;28(3):122-127.3. Quirynen M, Listgarten MA. The distribution of bacterial morphotypes around natural teeth and titanium implants ad modum Branemark . Clin Oral Implants Res. 1990;1(1):8-12.
4. Misch CE, Hahn J, Judy KW, et al. Workshop guidelines on immediate loading in implant dentistry . J Implantol. 2004;30(5):283-288.
5. Balshi TJ, Wolfinger GJ, Balshi SF 2nd. Analysis of 356 pterygomaxillary implants in edentulous arches for fixed prosthesis anchorage . Int J Oral Maxillofacial Implants. 1999:14(3):398-406.
6. Misch CE. Preimplant prosthodontics: overall evaluation, specific criteria, and pretreatment prostheses. In: Misch CE, ed . Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby; 2008:233-275.
7. Perry RD, Harsono M, Brown A, et al. Wear abrasion testing methodology for denture teeth. Presented at: AADR/CADR Annual Meeting & Exhibition; March 23, 2012; Tampa, FL.
8. Stober T, Henninger M, Schmitter M, et al. Three-body wear of resin denture teeth with and without nanofillers . J Prosthet Dent. 2010;103(2):108-117.
Hugh Flax, DDS, FICOI
Private Practice
Atlanta, Georgia