Replacing Full-Mouth Worn Restorations and Restoring Gingival Architecture
With advanced technology and materials, a collaborative approach helps to achieve optimal esthetic results.
Color schematics has always been a challenging and daunting process for laboratory ceramists. Natural dentitions are irregular and rarely monochromatic, often possessing different shade distributions, degrees of color, hues, and textures that vary depending on individual cases. For instance, in cases requiring a reduction in opacity and creation of a suitable incisal translucency, the lingual cutback may be implemented to provide the opportunity to recreate esthetics of the adjacent teeth.
Modern dental standards require the implementation of smile design principles and esthetic results that mimic a patient’s natural dentition. Advanced materials and technology have evolved and simplified this process over the years. Ceramists now have at their disposal visual communication techniques, such as identification molds and esthetic prescription forms that coincide with the Shade Indicator Chart system. These communication methods facilitate visualization of the expected outcome and enable the ceramist’s artistic expression to create intrinsically vital-appearing restorations that synchronize with the patient’s natural dentition.
In implant and restorative cases, a consistent problem facing ceramists and clinicians is how to meet smile design principles and achieve optimal esthetics that blend seamlessly with natural dentition. The answer lies in using highly esthetic abutment materials. However, this material selection is determined by several factors, including implant position, alignment, and angulation.
This process sometimes can be further complicated when patients lack the proper gingival architecture necessary for maintaining gingival health and obtaining a natural and esthetically appealing smile. This can only be accomplished when hard and soft periodontal tissue surrounding each tooth are properly managed. In many of these restorative cases, periodontal smile sculpting is performed and can be beneficial in determining both the pre-restorative treatment for dentition and for creating a blueprint to enhance the patient’s esthetic treatment results.1 All gingival architecture cases vary; for instance, in implant cases, gingival recession is typically a factor. Research shows that 80% of these cases exhibit gingival recession on the buccal aspect.2 Patients presenting with a high gingival smile line require the construction of interdental papillae.
Before papillae can be constructed or maintained, an esthetic triangle of adequate bone volume, proper soft-tissue thickness, and esthetic-appearing restorations is compulsory.3 In order to frame the restoration and give the illusion of natural papillae, pink porcelain is frequently used due to its ability to imitate the color, shape, and health of the surrounding tissue and complement white esthetics for a natural-looking smile.4,5 A nonsurgical option is tissue-colored porcelain used for hard- and soft-tissue replacement and to provide lip support, in addition to restoring symmetrical gingival architecture and replacing lost papillae.6
Esthetic restorative cases require comprehensive treatment planning and a multidisciplinary approach that necessitates a collaborative partnership and communication between the dentist and ceramist in order to achieve the goals of the case and attain optimal results. Durable, functional, long-lasting, and esthetically pleasing, high-quality restorations are predictably produced by implementing these communication techniques,7 especially in esthetic zone cases.8
The following case describes a full-mouth reconstruction using lithium disilicate abutments (IPS e.max® Press, www.ivoclarvivadent.com). The presentation elaborates on the communication materials and techniques that facilitated the successful completion of the case.
Case Presentation
A 58-year-old woman presented with existing amalgam buildups underneath worn bridges, in addition to extremely dark and discolored teeth. The patient explained she had tetracycline-stained natural dentition, but because all of her teeth contained existing restorations, this could not be verified. The patient’s mouthful of restorations had been placed by an assortment of dentists over a 30-year period. At first, the patient underwent single-tooth dentistry, but over 3 decades, almost every tooth required a crown or veneer. As a result, the patient was constantly forced to repair broken restorations. The patient also experienced symptoms of temporomandibular joint disorder—pain and discomfort—due to a misaligned bite.
Treatment Planning
After the initial consultation, a full-mouth rehabilitation was presented to the patient, agreed upon, and planned. The longest part of treatment would be the tissue grafting necessary for the area surrounding the patient’s anterior bridge, which spanned teeth Nos. 6 through 9, in order to prepare for implants in the Nos. 7 and 8 positions. Implant placement was needed for teeth Nos. 7 and 8. A joint consultation between the periodontist and clinician determined there would still be a tissue deficiency, even with applied tissue grafting. Consequently, the use of pink porcelain and/or splinted implants was discussed and ultimately agreed upon.
Material Selection
A chief concern in this case was the need for a material that would mask the dark tetracycline color of the natural underlying tooth structure while concurrently being as conservative as possible and providing a natural translucency. The challenge lay in matching and maintaining an even color transition among all the combinations of restorations in the patient’s anterior region—which consisted of veneers, crowns, and implants—that would seamlessly blend with her smile.
Clinical Protocol and Laboratory Perspectives
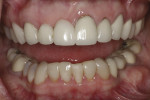
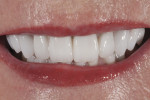
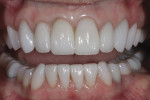
The patient presented with previously restored dentition and a maxillary cant on her right side (Figure 1) with which she was dissatisfied. The patient desired an improved cosmetic appearance and better function (Figure 2).
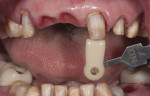
A preoperative model was constructed and mounted with a centric relation (CR) bite. The first point of contact was made between Nos. 11 and 21. A diagnostic wax-up was completed to address esthetic and functional concerns (Figure 3). The old restorations were removed (Figure 4), and the patient’s teeth were prepared for lithium-disilicate restorations. A photograph with a shade tab of the existing preparation color was taken and sent to the ceramist.
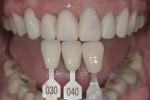
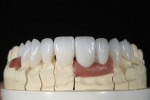
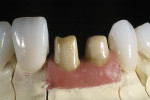
A silicone matrix of the diagnostic wax-up was constructed and used to fabricate the provisional restorations. Another photograph of the shade tab and preparations was taken and sent to the laboratory (Figure 5). A gingival deficiency between teeth Nos. 7 and 8 required the use of pink ceramic to create the illusion of papilla. A pink composite piece was fabricated chairside to meet the desired color and size objectives. (Figure 6). The use of pink porcelain required shade imaging to aid the ceramist in visualizing the actual color being used and photographed in the mouth. The ceramist would also receive a physical sample of the pink composite for use.
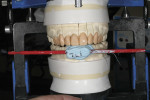
A photograph of the patient and the provisional restorations was taken for visual representation and sent to the laboratory. The new restorations would model the provisional restorations in shape and arrangement. A provisional stick bite photograph was taken. It was crucial for this photograph to be taken from a straight-on view to indicate that the stick bite was level with the patient’s facial features. This would help to avoid any angular distortion in the picture. The provisional stick bite was used to verify the vertical midline of the initial wax injection (Figure 7).
Laboratory Protocol
Once the ceramist received all diagnostic tools—including preoperative photographs and impressions, master impressions, bite registrations, a horizontal plane reference (ie, stick bite), and an eyebrow-to-chin photograph of the patient with stick bite in place on the lower incisors—work began for fabrication of the case.
A silicone matrix of the provisional restorations was placed on the working model. A wax injection mold process was used to transfer the shape, form, and position of the provisional restorations for the final wax-up. The injection was then refined to achieve the final contour wax-up.
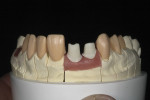
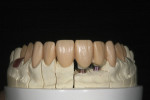
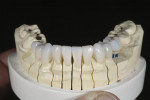
Restorations for the implants were waxed over the tissue to replicate the emergence position of the adjacent prepared teeth (Figure 8). The gingival silhouette of the wax over the implants was scored into the stone using a sharp blade over a very fine red pencil. The wax-up was completed on the titanium abutment base, and was contoured to create the shape of where the initial full-contour wax-up contacted the tissue. A silicone matrix of the diagnostic wax-up was used to evaluate room for restorations over the abutments.
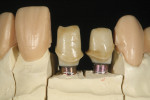
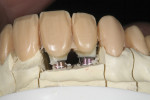
A matrix of the full-contour wax-up was used to evaluate the shape of the wax abutments (Figure 9). The wax abutments were pressed from a high-opacity lithium disilicate. The abutments were then shaded to match the color of the adjacent prepared teeth (Figure 10), then bonded to the titanium abutment bases using a universal cement (Multilink® Automix, Ivoclar Vivadent) (Figure 11).
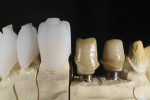
A matrix was used to recreate the full-contour wax-up over the pressed lithium-disilicate abutments. The incisal area was cut back in wax to allow room for micro-layering of the incisal edges (Figure 11). A reamer was used to align the access hole with the screw path in the abutment, and screw access holes were created in the wax-ups (Figure 12). The restorations were then pressed from HT Opal 2 IPS e.max ingots.
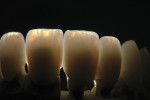
The incisal effect layering was carefully segmented using various enamel and mamalon effect ceramics (Figure 14). The effect buildup was fired, then built to full contour with OE1 enamel. The contoured enamels were placed on the restorations and fired at 750°C. The internal effects and natural opalessence of the lithium-disilicate restorations were visible when backlit (Figure 15). After firing, the facial lobes and surface texture were created using an 863 012 diamond bur.
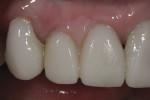
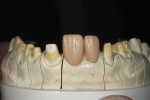
The finalized restorations were placed on the working models (Figure 16 and Figure 17) and determined to replicate the natural tooth structure (Figure 18). The restoration surfaces were glazed and polished, after which the final case was delivered for placement (Figure 19 through Figure 21).
Conclusion
Achieving optimal esthetic results and fulfilling patient desires in restorative, implant, and gingival architecture cases dictate the use of a combination of advanced technology and materials. Additionally, successful functional and esthetic outcomes are predicated on collaborative teamwork between the dentist and ceramist.
Disclosure
The authors received honoraria from Ivoclar Vivadent for this manuscript.
References
1. Bitter RN. The periodontal factor in esthetic smile design—altering gingival display. Gen Dent. 2007;55(7):616-622.
2. Small PN, Tarnow DP. Gingival recession around implants: a 1-year longitudinal prospective study. Int J Oral Maxillofac Implants. 2000;15(4):527-532.
3. Zetu L, Wang H-L. Management of inter-dental/inter-implant papilla. J Clin Periodontol. 2005;32(7):831-839.
4. Zalkind M, Hochman N. Alternative method of conservative esthetic treatment for gingival recession. J Prosthet Dent. 1997;77(6):561-563.
5. LeSage BP. Improving implant aesthetics: prosthetically generated papilla through tissue modeling with composite. Pract Proced Aesthet Dent. 2006;18(4):257-263.
6. Priest GF, Lindke L. Gingival-colored porcelain for implant-supported prostheses in the aesthetic zone. Pract Periodontics Aesthet Dent. 1998;10(9):1231-1240.
7. Weston JF, Haupt E. Creating esthetic success through proper clinician and laboratory technical communication. Dent Clin North Am. 2011;55(2):371-382.
8. Almog DM, Meitner SW, Even-Hen N, et al. Use of interdisciplinary team approach in establishing esthetic restorative dentistry. NY State Dent J. 2005;71(5):44-47.
About the Author
Matt Roberts, CDT
Laboratory Ceramist
CMR Labs
Idaho Falls, Idaho
Amanda Seay, DDS
Private Practice, Park West Dentistry
Mount Pleasant, South Carolina