Digital Impressioning Using CEREC© AC Connect
Oh, the places you can go now in dentistry using chairside CAD/CAM.
One of the first gifts I received when I graduated from dental school was the book Oh, the Places You’ll Go! by Dr. Seuss. The book was a gift from my aunt, and I’m sure when she picked it out it was meant more as a “go forth into the world and chase your dreams” gift than a “wow, look how far we have come in dentistry” gift. I can’t help but wonder, in the 8 years I have been involved with digital dentistry, could Dr. Seuss have known the advances Sirona Dental Systems (www.sirona.com) would make with CEREC© in such a short period of time?
CEREC Technology 1985 to Present
The original brainchild of a German dentist, Professor Werner H. Mormann, and an engineer, Dr. Marco Brandestini, CEREC was released in 1985 as the first chairside digital impression system. The original two versions of this technology were single free-standing machines capable of acquiring a digital impression and milling the final restoration (inlay or onlay) in a single appointment. In 2000, CEREC 3 was introduced, with the biggest advance being the separation of the acquisition unit and the milling chamber. This allowed the milling chamber to be placed in a separate area of the office to keep the milling noise to a minimum and condense the size of the acquisition unit when in the operatory. Today, two acquisition versions are available, the CEREC AC, which allows the operator to acquire a digital impression and mill a single-unit crown, inlay, or onlay at chairside, or to electronically transfer the digital impression to a dental lab, such as MicroDental Laboratories, for fabrication of the final restoration. The CEREC AC Connect is the second version. This unit allows the dentist only to acquire a digital impression and transfer it to MicroDental Laboratories electronically. No chairside milling is available with CEREC AC Connect. Two different milling chambers are now available and allow the dentist to mill single-unit ceramic restorations, acrylic bridges, implant abutments, study models, and surgical guides for implant placement.
CEREC AC Connect in Action
CAD/CAM technologies are revolutionizing the way we make an impression and restore teeth. These systems provide the clinician the ability to scan a single tooth, quadrant, or full arch, and create any restoration needed to restore a tooth or multiple teeth to full function and esthetics. Any restoration using ceramics, metals, or composites can be fabricated by electronically sending the digital impression to MicroDental Laboratories using CEREC AC Connect. The process is quite simple.
Preparing and Scanning in the Office
First the tooth is prepared as required by the material chosen for the final restoration; for example, if an all-ceramic (IPS© e.max, Ivoclar Vivadent, www.ivoclarvivadent.com) laboratory-fabricated restoration is planned, proper occlusal and axial reduction will be required for strength and stability. Once achieved, a digital LED camera is used to take a scan of the preparation and adjacent teeth. The opposing arch is then pictured along with the patient’s bite on the prepared side in occlusion (buccal bite). A fine powder is lightly used to coat the teeth before imaging to create a uniform reflective surface for the camera to accurately read all contour changes in the natural teeth or preparation. Once the images have been acquired and the models are digitally fabricated, the margins are marked, and the case is electronically transferred to MicroDental Laboratories.
Once at MicroDental
The laboratory forms are filled out online and transferred with the case through the Sirona Connect portal to MicroDental. Multiple units can be fabricated from one digital impression. Sirona just underwent a complete software rewrite for all CEREC products, including the laboratory version used to design and create cases sent through Sirona Connect. Upon receipt of the case, MicroDental will open the case, verify accurate marginal integrity and reduction, and begin the virtual development of the tooth. The new software allows the technician full design control. The process delivers a crown proposal that requires little modification and can be ready for milling by a MicroDental Laboratories technician in a matter of minutes. The milling time takes anywhere from 5 to 13 minutes, depending on which milling speed is chosen. The restoration is then finished—crystallized, stained, and glazed—and returned to the doctor for delivery. If an all-ceramic restoration is requested, it will be virtually created and milled. This can be done without the need for a physical die or models. Occlusion, contours, and contacts are all confirmed virtually. If a full gold or PFM crown is being fabricated, the laboratory will send the case out to Sirona’s Infinident Lab, where models are fabricated for the porcelain to be fused to the metal in the case of a PFM, or for the wax and casting in the case of full gold. The restoration is then finished by MicroDental and returned to the doctor for delivery.
Case Presentation
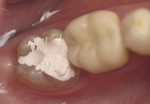
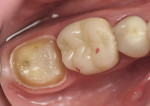
A patient presented following endodontic treatment on tooth No. 31, which required a final full-coverage restoration (Figure 1). It was determined that a laboratory CAD/CAM-fabricated e.max crown (lithium disilicate) would be placed. The tooth was prepared, and a core build-up placed (Figure 2). The prepared tooth and surrounding tissues were sprayed with Sirona Optispray contrast medium and pictured using the author’s CEREC AC unit (LED camera). The case information and laboratory slip were then transferred to MicroDental Laboratories via Sirona (CEREC) Connect.
At MicroDental, the case was opened and the new CEREC 4.0 software was used to design the crown to full contour and occlusion. A prefabricated low-translucency lithium-disilicate block (size C-14, shade A1, e.max CAD) was then milled into the crown for tooth No. 31. Lithium disilicate was the material of choice for the case because it demonstrates high fracture resistance and strength (up to 400 MPa) as well as life-like optical properties. After milling, the crown was crystallized in a porcelain oven according to Ivoclar’s recommendations, characterized, and returned for delivery.
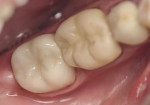
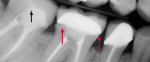
At the delivery appointment, the temporary restoration was removed. The preparation was cleaned, etched, rinsed, and dried. Dual-cure luting composite (Multilink® Automix EZ, Ivoclar Vivadent) was used. Multilink is indicated for use with metal, all-ceramic, metal-ceramic, and composite restorations and provides a strong hold on all surfaces. The primer liquids (A/B) were mixed in a 1:1 ratio before applying to the preparation. A microbrush was used to apply the primer mix to the preparation in a scrubbing motion. Air was used to thin the primer; light-curing is not necessary because Multilink is an auto-cure material. The internal aspect of the crown was carefully covered with the luting composite (Multilink Automix), which mixes and extrudes from the automix tip. The crown was then seated on tooth No. 31 with slight pressure. Excess cement was removed from all cervical and interproximal areas with a microbrush, and additional pressure was applied and held to ensure complete and proper seating during cleanup. Dental floss was then used to complete interproximal cleanup. The crown was cured using an LED curing light (Bluephase, Ivoclar Vivadent) from the buccal, mesial, lingual, and distal aspects, after which it demonstrated exceptional fit, function, and esthetics (Figure 3). A postoperative radiograph was taken to confirm marginal integrity and adaptation (Figure 4).
Conclusion
Many dentists are unaware that chairside CAD/CAM systems also offer the ability to submit laboratory cases electronically. As demonstrated in the case above, Sirona, with CEREC AC and CEREC AC Connect, allows the dentist to order a milled restoration, which is designed digitally, finished, and delivered to the office ready for cementation. Outbound shipping time was eliminated, and the final restoration proved to be of superior quality with regard to esthetics, function, and marginal integrity. How could Dr. Seuss have known?
About the Author
David Juliani, DDS
Private Practice
Rochester Hills, Michigan