The Unity of Form and Function: A New Dental Paradigm
Functional orthopedics seeks to improve function first and foremost by optimizing maxillary width and mandibular position.
In this era of evidence-based dentistry, the profession may be somewhat limited by longstanding but unexamined assumptions that still form the framework of our diagnoses and treatment. The experiences of this author and others in working with both children and adults using a system called “functional orthopedics” seems to indicate the possibility of a different paradigm forming based on maxillary expansion and mandibular repositioning. Exploration of the scientific literature finds support and possible explanation for the observed results.
Functional orthopedics strives to convert all malocclusions into Class I dental malocclusions prior to employing fixed mechanics. This is acomplished by using active plates and orthotics or jaw-positioning appliances. The results of treating children and adults in this manner suggest a reexamination of the basic assumptions that exist in dentistry today. In light of the outcomes experienced, this article will explore two of those assumptions and propose a new paradigm in which optimal function is the overriding consideration.
The first assumption, common to all specialties of dentistry, relates to the location of the mandible in the face. The long-held dental paradigm has been to accept the existing jaw position or to reposition it distally. In most malocclusions, except some Class III facial patterns, the mandible may be in a compromised position. Evidence suggests that deep bites, cross bites, and maxillary arch discrepancies likely are examples of a compromise in which the mandible has not been allowed to develop to its full downward and forward potential because of maxillary constriction.
The second assumption, specific to orthodontics, concerns the avoidance of expansion in either dental arch in older children and adults. Because sutures fuse early in life, it was long assumed that rapid maxillary expansion would be ineffective and unstable in patients older than 12 or 13 years of age. Consequently, palatal expansion techniques were limited to younger patients.
The basis for the new paradigm and the goal of functional orthopedics is to allow the mandible to “recover” from its compensatory position. The author will attempt to show that recovery is a result of influences outside the mouth, the dentist’s primary focus. Because the cervco mandibular muscle complex no longer needs to hold the mandible in this compensated position, recovery or normalized posture is possible. Assuming that this is true, dental diagnosis and treatment planning must include those influences.
Functional Orthopedics as a Treatment Option
Functional jaw orthopedics is a philosophy of treatment that seeks to alter the shape of the bony alveolus in the maxilla and, in turn, the location of the mandible and its alveolar processes. This approach not only facilitates maxillary expansion in children with patent sutures but also promotes palatal remodeling and increased maxillary width in adults.
The early use of the articulator and other attempts to replicate in the laboratory the function that occurs in the face may be responsible for the overly simplistic and mechanistic way facial function is viewed. This early model tried to relate the mandible to the skull in a way that allowed for replication. So as long as it was reproducible and related to the model, the mandibular posture with which the patient presented was the one accepted or placed more posterior. Türp stated, “The decisive factor, apart from any preferred method, is that the chosen therapeutic mandibular position must be reproducible.”1
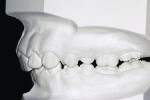
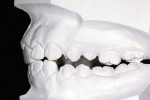
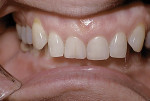
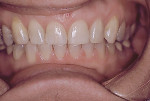
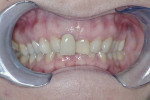
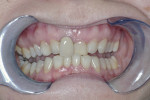
Generally there was little consideration for the functional relationship of the mandible to the cranium or the face, let alone to the rest of the body. Looking beyond the jaw and maxilla leads to a new premise—that the musculature holds the mandible into an altered posture compensatory position) to ensure and maximize contact between the maxillary and mandibular dentitions. Thus, with a maxillary deficiency the mandible is unable to assume its “normal” rest position because the teeth will not fit together (Figure 1 and Figure 2). Enlow proposed that maxillary dental problems are the result of poor maxillary growth and that the teeth erupt into the position of best fit.2
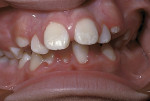
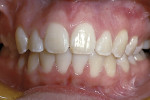
The initial goal for employing functional orthopedics was to eliminate the need for dental extractions in treating adolescent and adult patients by employing removable appliances (active plates and jaw-positioning appliances) and fixed mechanics to correct the pre-existing maxillary deficiencies and reposition the mandible. Results often are dramatic and different than those achieved employing regional fixed appliances (Figure 3 through Figure 6).
Techniques and Bone Remodeling
In maxillary expansion, a palatal acrylic appliance rests intimately on the palatal mucosa (Figure 7). Active plates are attached to the teeth with Adams clasps, holding the appliance firmly against the palate to control buccal tipping of the posterior teeth and increase intermolar width. As the width between the active plates is mechanically increased, the halves of the appliance split. The force and fit of the appliance against the palate start the remodeling process and prevent tipping forces on the teeth (Figure 8). The alveolus may tip, but the teeth go with it. As long as the appliance seats firmly on the palate, it is mechanically impossible to tip the teeth laterally without moving the alveolus.
Because the teeth do not tip, there is little risk to the buccal gingival height. In his research, Bassarelli noted that slow maxillary expansion had no detrimental effects on the gingival height.3 Note that the changes are seen in bone of any age (Figure 9). This does not just affect growth, but also bone physiology. As the bone structure itself is altered, the resultant growth is affected.
Obviously, success demands full-time continuous wear. Torstveit stated, “The magnitude of loading, type of activity, the rate of activity, and the number of repetitions seem to be important factors associated with the effect of physical activity on bone.”4
Considering development of a cross-section of the maxilla, it bes apparent that the width of the dental alveolar processes is a byproduct of the functional matrix of the respiratory portion of the maxilla itself. The cross-section of the adult maxilla reveals that the maxillary alveoli supporting the teeth are in a location as a result of the width of the maxillary sinuses, septum, and nares—a respiratory-type “functional matrix.”
The functional matrix theory posited by Melvin Moss provides an initial explanation of the bone-remodeling process that occurs.5-7 Studies involving bone adaptation to mechanical loading and mechanical stress—particularly in adults—provide the explanation for the response the author has seen in his own cases. Evidence suggests that remodeling is a function of tissue-level and biomechanical mechanisms operating on bone effector cells (osteoblasts and osteoclasts).8-13
Once palatal expansion is established, the question of stability arises. How is this slight maxillary increase (ranging from 4 mm to 8 mm) in molar width supported? The answer lies in the impact of the enhanced maxillary arch width on the mandible. Increased intermolar maxillary width and position of the maxillary molars allow the mandible to reposition forward. A wider mandibular molar width, located under the wider maxilla, supports the change and provides the needed stability.
Reviewing numerous cases treated in this manner suggests that the results are attributable to a muscular repositioning of the mandible in the face once maxillary interference is removed. In children, the results are particularly quick and dramatic, not because they are still growing but because the musculature allows a rapid response.
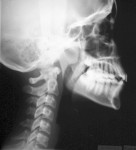
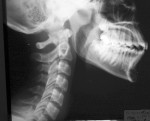
The effects of maxillary expansion and mandibular repositioning on stomatognathic and cranio-cervical function and overall structural health are exciting and worth exploration in a subsequent article. Unexpected but frequently observed functional changes include improvement of the cervical curve (Figure 10 and Figure 11) and relief of temporomandibular disorder-type symptoms including, but not limited to, headaches and muscle spasms.14-16
Developmental Considerations
Craniofacial growth often is delineated in terms of the rate of growth of its various components. The vault and cranial base develop first because of their relationship to the expanding brain. Enlow stated, “90% of cranial width and length are.completed by the age of 7.”2 In close proximity to the cranial base, the second growth area is the mid-face or maxilla. Growth in width of the maxilla is 96% complete for males and 95% complete for females by 8 years of age.17-19
While maxillary width is relatively complete quite early in facial development, the mandible continues to grow downward and forward into early adulthood. These developmental disparities, documented by Bishara et al, have a profound effect on the ultimate location of the mandible in the face.20
Another aspect of maxillary growth is the location and positioning of the maxillary incisors. Their antero-posterior position is established quite early and often compromised as a result of lack of arch width. If they are retruded because of severe crowding or retro-inclined as in a division 2 type malocclusion, they can have a notable impact on mandibular growth, keeping the mandible in a posterior position (Figure 12 and Figure 13). This is evidenced by the often-rapid correction of Class II, division 2 malocclusions when the incisor position is corrected.
Enlow presented the concept of mandibular entrapment.2 During craniofacial growth, the human mandible bes entrapped below and behind the rotated nasomaxillary complex and the upright body posture positioning of the basicranium and cervical regions. Overbite and overjet, or anterior crowding, are an evolutionary and developmental means to compensate for the vulnerable positioning of the mandible and its temporomandibular joint.2,3
The cephalocaudal growth gradient may play a role in developing malocclusions, especially those exhibiting more narrow maxillary width. Because displacement and remodeling are the most fundamental activities of bone growth, maxillary deficiencies or excesses will tend to prevent the mandible from reaching its “correct” Class I position.
Overall mandibular remodeling and condylar growth are geared to accommodate housing for the developing teeth, to adapt to the mandibular displacement, and to adapt to the complex growth changes occurring throughout the craniofacial structures.3 Genetic determination of mandibular length is overridden by the compensation of the soft-tissue matrix.
Condylar cartilage does not develop by differentiation from embryonic primary cartilages; instead, it has secondary growth potential. The condyle does not determine how the mandible grows; rather the mandible determines how the condyle grows. Compared with other cartilages, condylar cartilage reacts faster with a lower threshold to outside mechanical factors.”21
Mandibular growth combines displacement and remodeling. Enlow found that the length of the corpus, height of the ramus, and direction and shape of the condyle are influenced more “by the genetic determinants that reside wholly in the soft tissue not in the hard part of the bone itself.”2 As a result, “the mandible has often been regarded as less responsive to orthopedic forces because of growth pre-programming.”3
Development of the alveolus, however, is highly responsive to local changes in the environment. If the mandible is caught in the closing vice between the mid-face above and the airway, gullet, and cervical column behind, it cannot drop downward and forward.3 Mandibular teeth erupt into a pre-existing environment bringing along the associated, and sometimes deficient, alveolus. Results are as varied as the variety of malocclusions.
An interesting consequence of a shift in mandibular posturing, as in a cross bite, is that the head position may compensate to the opposite side. Not only may this affect the symmetry of the growing mandibular condyles, it also may have a profound effect on the growing spine.22-24
Vertical Dimension
Vertical dimension is another aspect of the mandibular displacement process. Because the height of the ramus is primarily driven genetically by the soft tissue controls (“the vertical height of the ramus must match the vertical height of the nasal and dental parts of the ethnomaxillary complex”2), the dental alveolus must compensate if a deficiency occurs. Enlow stated that, “Overjet, overbite, and anterior crowding are phylogenic means to relieve the mandible and its temporomandibular joint placed in this vulnerable position.”2
Vertical development as it relates to downward and forward positioning is critical to all phases of dentistry, including prosthetics, periodontal therapy, and management of dysfunctional conditions of the temporomandibular joint. If it is possible to reposition the mandible downward and forward, the vertical space created would help in uprighting posterior teeth, leveling the plane of occlusion, and—importantly in periodontal conditions—leveling the alveolus. Posterior dental eruption into the space created is the key to success in many compromised situations. This is the popular notion of multidisciplinary dentistry functionally applied—integrating all the specialties to treat a case where the goal is improved musculoskeletal function, rather than just dental or cosmetic excellence.
A severe Class II malocclusion with deep overbite and excessive curve of Spee in the lower arch is an example of the lack of vertical development. The posterior plane of the occlusion is the result of poor posterior vertical growth. The location of the mandible prevents full and proper posterior vertical growth, but when the mandible is held forward with an appliance, the posterior teeth are allowed to erupt and correction occurs. If maxillary width had been sufficient to allow full forward and downward development of the mandible, this may have happened naturally (Figure 14 and Figure 15).
Because Class II malocclusions occur in the anteroposterior, vertical, and transverse planes, addressing these problems is one of modifying the current growth process, to one that is more beneficial. Under this model, mandibular repositioning would follow maxillary expansion, thus vertical development could catch up.
Conclusion
Long-held assumptions regarding maxillary expansion and mandibular positioning need reexamining in light of functional as well as cosmetic considerations. Most, if not all, malocclusions are the result of inadequate maxillary growth and the subsequent inability of the mandible to attain a full physiologically neutral position. At any age, when the deficiency in the maxilla is corrected and the correct arch form is in place, the mandible will assume a more neutral position within the musculature.
Employing extractions and/or surgery to achieve a cosmetic ideal disregards function. Functional orthopedics seeks to improve function first and foremost by optimizing maxillary width and mandibular position. This, in turn, may impact the stomatognathic and cranio-cervical as well as entire musculoskeletal function.
References
1. Türp JC, Schindler HJ, Rodiger O, et al. Vertical and horizontal jaw relations in reconstructive dentistry. A critical review. Schweiz Monatsschr Zahnmed. 2006;116(4):403-417.
2. Enlow D. Facial Growth. 3rd ed. Philadelphia, Pa: WB Saunders;1990.
3. Bassarelli T, Dalstra M, Melson B. Changes in clinical crown height as a result of transverse expansion of the maxilla in adults. Euro J Orthod. 2005;27(2):121-128.
4. Torstveit MK. Bone adaptation to mechanical loading. Tidsskr Nor Laegeforen. 2002;122(21):2109-2111.
5. Moss ML. The functional matrix hypothesis revisited. 1. The role of mechanotransduction. Am J Orthod Dentofacial Orthop. 1997;112(1):8-11.
6. Moss ML. The functional matrix hypothesis revisited. 2. The role of an osseous connected cellular network. Am J Orthod Dentofacial Orthop. 1997;112(2):221-226.
7. Moss ML. The functional matrix hypothesis revisited. 3. The genomic thesis. Am J Orthod Dentofacial Orthop. 1997;112(3):338-342.
8. Frost HM. From Wolff’s law to the Utah paradigm: insights about bone physiology and its clinical applications. Anat Rec. 2001;262(4):398-419.
9. Skerry TM. One mechanostat or many? Modification of the site-specific response of bone to mechanical loading by nature and nurture. J Musculoskelet Neuronal Interact. 2006;6(2):122-127.
10. Burger EH, Klein-Nulend J, van der Plas A, Nijweide PJ. Function of osteocytes in bone--their role in mechanotransduction. J Nutr. 1995;125(7 Suppl):2020S-2023S.
11. Burger EH, Klein-Nulend J. Mechano-transduction in bone—role of the lacuno-canalicular network. FASEB J. 1999;13(Suppl):101S-112S.
12. Mosley JR. Osteoporosis and bone functional adaptation: mechanobiological regulation of bone architecture in growing and adult bone, a review. J Rehabil Res Dev. 2000;37(2):189-199.
13. Turner CH, Pavalko FM. Mechano-transduction and functional response of the skeleton to physical stress; the mechanisms and mechanics of bone adaptation. J Orthop Sci. 1998;3(6):346-355.
14. Chinappi AS Jr, Getzoff H. A new management model for treating structural-based disorders: dental orthopedic and chiropractic co-treatment. J Manipulative Physiol Ther. 1994;17(9):614-619.
15. Chinappi AS Jr, Getzoff H. The dental-chiropractic co-treatment of structural disorders of the jaw and temporomandibular joint dysfunction. J Manipulative Physiol Ther. 1995;
18(7):476-481.
16. Chinappi AS Jr, Getzoff H. Chiropractic/dental cotreatment of lumbosacral pain with temporomandibular joint involvement. J Manipulative Physiol Ther. 1996;19(9):607-612.
17. Snodell SF, Nanda RS, Currier GF. A longitudinal cephalometric study of transverse and vertical craniofacial growth. Am J Orthod Dentofacial Orthop. 1993;104(5):471-483.
18. Zhou WL, Lin JX. Longitudinal study of the growth of craniofacial widths in 13-18 years adolescents with normal occlusion. Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 2002;24(1):54-58.
19. Lux CJ, Conradt C, Burden D, Komposch G. Transverse development of the craniofacial skeleton. Eur J Orthod. 2004; 26(1):31-42.
20. Solberg ND, Clark GT. Abnormal jaw mechanics diagnosis and treatment. Proceedings of the 2nd International Symposium. 1984 Feb 20-21; Newport Beach, CA; Chicago: Quintessence; 1984:97.
21. Moyer RE. Handbook of Orthodontics. 4th ed. Chicago, IL: Year Book Medical Publishers; 1988.
22. Gregory TM. Temporomandibular disorder associated with sacroiliac sprain. J Manipulative Physiol Ther. 1993;16(4):256-264.
23. Tingey EM, Buschang PH, Throckmorton GS. Mandibular rest position: a reliable position influenced by head support and body posture. Am J Orthod Dentofacial Orthop. 2001;120(6):614-622.
24. Solow B, Siersb1k-Nielsen S. Cervical and craniocervical posture as predicators of craniofacial growth. Am J Orthod Dentofacial Orthop. 1992;101(5):449-458.
To read another article about Functional Orthopedics, visit: dentalaegis.com/go/id425
For product information on Orthopedics, visit: dentalaegis.com/go/id426
About the Authors
Albert S. Chinappi, Jr., DDS, MS
Private Practice
Marlton, New Jersey