Using In-Office CAD/CAM and Lithium Disilicate in Restorative Makeovers
Modify, finalize, and verify essential components of smile design with these tools.
Ceramists and clinicians both face inherent challenges when creating harmony among multiple units in restorative smile makeovers. Every laboratory technician and dentist performing smile makeovers undergoes a strategic sequence of design protocols that encompass the principles of smile design, symmetry, proportion, length/width ratio, contact placement, and embrasures. These intuitive rules for smile design apply to CAD/CAM-created makeovers, also. A benefit of creating restorative makeovers with CAD/CAM is that the interactive design software enables ceramists and clinicians to change smile makeover proposals instantaneously to more quickly create a harmonious result than traditional waxing methods. As with restorations fabricated for conventional smile design cases, attention to shape, composition within the arch form, incisal plane accuracy and levelness, and length-to-width proportions are addressed in CAD/CAM-created restorations.
Materials and Methods
Many CAD/CAM instruments have been introduced into the clinical and laboratory dental marketplace to meet the needs of emerging technologies. One such system, the E4D Dentist (D4D Technologies, www.e4d.com) enables dentists and ceramists to create restorations more simply and efficiently than with traditional methods. Its 3-dimensional software, DentaLogic, provides ease of use in designing and milling multiple restorations compared to other CAD systems.
The E4D’s 3D high-speed laser scanner scans hard and soft tissues without the need for CAD/CAM scanning powder for digital impressions. The E4D is versatile in its ability to digitally impress intraoral full arches, full-arch impressions, and full-arch models. The system’s multiple design tools assist dentists and ceramists in verifying essential smile design makeover components. Also, smile-design considerations that are worked out with diagnostic wax-ups and temporaries can be cloned into the E4D system, and the E4D software facilitates whatever changes are required to improve and finalize restorative designs. These changes in smile-design considerations can be made in much less time than traditional laboratory methods. Rendered restorative designs can be sent wirelessly to the E4D precision milling system, which uses dual spindles and fine diamond burs to efficiently fabricate CAD materials into restorations that demonstrate excellent fit, higher strength, and lifelike esthetic designs.1,2
Among these CAD materials is IPS e.max® CAD lithium-disilicate glass-ceramic (Ivoclar Vivadent, www.ivoclarvivadent.com), an innovative all-ceramic material demonstrating exceptional monolithic strength.3,4 Designed for CAD/CAM processing in the dental office or dental laboratory, IPS e.max CAD blocks demonstrate a high flexural strength (360 MPa) and are highly resistant to long-term mastication forces. As a result, IPS e.max CAD is indicated for inlays and onlays, veneers, partial and full crowns, and implant superstructures.3,4
IPS e.max CAD lithium-disilicate glass-ceramic blocks are available in high translucency (HT) and low translucency (LT) formats to provide a variety of esthetic solutions that demonstrate lifelike optical properties and naturally appearing esthetics. Esthetics can be further enhanced using stains, glazes, and powders to ensure that restorations appear indistinguishable from the surrounding dentition.
Case Presentation
A 50-year-old patient presented with 20-year-old laminate veneers (Figure 1). The treatment plan objectives were to create whiter and more natural-looking laminates, leveling the apices of the free gingival margins by lengthening the inciso-cervical length of the clinical crowns, and maintaining the appearance of the incisal and occlusal planes of the maxillary arch. In-office CAD/CAM technology (E4D Dentist) and lithium disilicate (IPS e.max CAD) would be used to fabricate the restorations.
The maxillary arch was scanned and the model was analyzed for information capture and accuracy, preparation review, margin detection, and margin identification. Then, the first step in developing multiple digital restorations was to orient each individual preparation in terms of mesio-distal, bucco-lingual, and inciso-cervical orientation. This was crucial to ensure that the restorations would be designed in similar dimensional planes.
The tooth in question was centered in the center of the compass. This was accomplished by beginning with the incisal view to set the bucco-lingual orientation. It is best to orient the tooth as if looking right down the longitudinal center of the tooth.
Then, once the perceived bucco-lingual dimension was attained, the view was switched to the buccal view or facial view (anterior) of the tooth. The compass appeared as the visible red line. The line was oriented with the desired incisal plane and/or occlusal plane. Orienting each prepared tooth in a similar fashion orients the restorative proposals in the makeover to establish a sound and harmonious foundation on which to build the restorations.
Note that with careful orientation of each individually prepared tooth, the emergence profile of the predefined autogenic proposal was oriented in the same plane as the preparation. Each individual restoration was manipulated for thickness, length-to-width proportions, incisal plane relation, occlusal plane relation, emergence profile, longitudinal developmental lobe and groove shapes, and contact and embrasure space anatomy (Figure 2).
Color codes indicated the proposal thickness. This gave the ceramist/clinician good intuitive data to study regarding the restoration’s strength. All of the proposed thicknesses were viewed simultaneously for more in-depth analysis of the makeover composition (Figure 3). Individual proposals were isolated and altered for margin placement, contact anatomy, and anatomic shape (Figure 4).
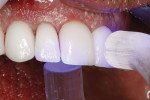
The appropriate milling blocks were selected and milled. Once milled, the restorations were fit on a master model and adjustments made, readying the restorations for “vitalization.” Vitalization began by staining the restorations according to a pre-determined colorization scheme that was rendered in a drawing prior to placement (Figure 5 and Figure 6). Ceramic powders (the e.max porcelain system) were layered onto each restoration to create depth and luminosity according to the rendering, after which the restorations were ready for finishing (Figure 7).
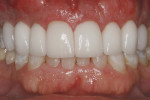
After finishing, the restorations were placed on the master model and demonstrated depth of color (Figure 8). Once the CAD/CAM-fabricated makeover restorations were cemented into place, they demonstrated a vital appearance (Figure 9).
Conclusion
Using the E4D Dentist system to simultaneously modify, finalize, and verify the essential components of smile design for all restorations in this smile makeover case helped to ensure the accuracy and predictability of the final result. Additionally, using the system to mill a highly esthetic material such as IPS e.max CAD lithium disilicate enabled the dentist to deliver a highly esthetic result customized to provide individualized optical properties and lifelike characteristics.
References
1. Helvey GA. The current state of digital impressions. Inside Dentistry. 2009;5(9):86-90.
2. Fasbinder DJ. Digital dentistry: innovation for restorative treatment. Compend Contin Educ Dent. 2010;31(Spec No 4):2-12.
3. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
4. Culp L, McLaren EA. Lithium disilicate: the restorative material of multiple options. Compend Contin Educ Dent. 2010;31(9):716-725.
About the Author
John Schwartz, DDS
DirectorIntegra Institute Center For Advanced Dental Learning
Assistant Clinical Professor
Department of Prosthodontics
Louisiana State University Health Sciences Center
School of Dentistry
New Orleans, Louisiana
Private Practice
Metairie, Louisiana