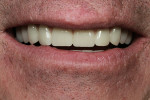
Conversion from an Immediately Loaded Provisional to a Final Hybrid Prosthesis
Placing a long-term provisional is still desirable in order to allow for treatment alteration in the event of a failed restoration.
Implant-borne restorative systems have developed quickly over recent years, and protocols for immediate provisionalization and loading are now well established with similar survival rates to delayed loading and restorative treatment.1 While it is possible to definitively restore a full arch with an immediately loaded prosthesis, delaying the final prosthesis is still desirable. Placing an immediately loaded, long-term provisional allows for altering treatment in the event of a failed implant, as well as evaluating esthetics, phonetics, and the occlusal pattern.
Case Report
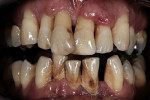
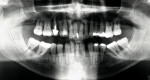
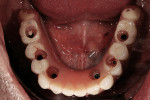
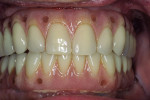
A 54-year-old man was referred for restorative planning by his periodontist. The prognosis of the existing teeth had been deemed hopeless and the patient wanted to understand all of the restorative options before moving forward with treatment. He ultimately decided that he wanted upper and lower hybrid prostheses (Figure 1 and Figure 2).
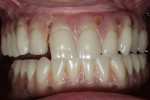
The patient had extensive bone loss throughout his mouth, with active severe periodontitis. Because of the extensive nature of the destruction and the potential poor quality of the projected implant sites, the determination was made to remove all of the teeth and deliver immediate interim full upper and lower dentures. At the time of the extraction surgery, socket preservation procedures were completed and the immediate upper and lower dentures were inserted and lined with a resilient denture liner (Figure 3).
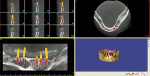
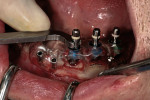
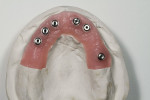
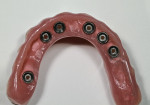
The dentures were relined periodically with a resilient liner to accommodate shrinkage from healing. At 5 months, the implants were placed in the lower arch using computer-guided surgery (Figure 4).
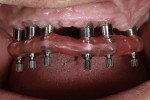
Six Straumann (www.straumann.com) bone-level implants were placed after the cone-beam CT scan was taken to facilitate the treatment plan, and a surgical guide was secured with bone screws. The provisional was fabricated by using a model made from the relined upper denture and Smart Implants’ proprietary process that allows for construction of both the surgical guide and the long-term provisional. Using temporary abutments that were attached to non-rotational Straumann multi-base abutments, the long-term provisional was luted with pink Triad® (www.dentsply.com) (Figure 5 and Figure 6).
Two months later, a similar procedure was completed for the upper arch and the patient was instructed that the provisionals in either arch could be converted to a final prosthesis after 3 months of healing to allow complete integration of the implants.
The provisionals were constructed with a metal framework to add strength and stability and the patient was also instructed that the provisional restorations could be left in place as a long-term provisional prosthesis as long as they were removed periodically to be cleaned and to check the implant/tissue interface. He was also instructed in the use of a Waterpik® (www.waterpik.com) and “fuzzy” floss (Figure 7).
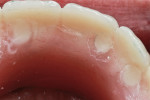
While the original plan was to convert the provisionals to a milled framework and hybrid prostheses within 6 months of the implant surgeries, a job loss prevented the patient from moving forward. He did not comply with periodic examinations, and ultimately presented 3 years post-insertion with a complaint of broken teeth on the upper provisional. He indicated that he would be willing to convert the upper arch but still needed to wait to do the lower arch for financial reasons (Figure 8).
Converting a long-term provisional or creating a final prosthesis on fully integrated implants is a straightforward procedure and requires a high degree of precision to ensure an appropriate fit in the final appliance. The required steps are:
- take an implant-level impression;
- fabricate the verification jig;
- take jaw-relation records and bite rim;
- try-in the denture;
- manufacture the milled framework; and
- deliver the final prosthesis.
Implant-level impressions can be made with either a closed-tray or open-tray technique. Closed-tray impressions use an impression abutment with a shaped head that, when impressed, will create a definitive seat in the impression. Open-tray impressions use a screw-retained impression post and generally require the use of a custom tray. The tray is fabricated and then openings are cut so that the impression-post screws can be accessed through the tray to facilitate removal from the mouth. Although clinically, the accuracy of either method is equal when carefully executed, in this instance the open-tray process was chosen.2 The impression was made using a polyether material because of its rigidity upon setting and ability to hold the impression post accurately in place. In this instance, the multibase abutments were attached to the implants and the impression posts attached to the abutments. The impression was made in the same fashion as an implant-level impression (Figure 9 and Figure 10).
The impression was sent to the laboratory, analogs were placed in the impression posts, and the model was poured with a soft-tissue mask around the implants. The implant analogs simulated the implants with the multibase abutment attached. A verification jig was fabricated on the model by placing the impression posts back into the implant analogs and then luting them together with GC Pattern Resin (www.gcamerica.com). The verification jig was carried to the mouth and the impression posts were screwed into the implants. The verification jig must have a passive fit to ensure no undue force will be placed on the implants with the final framework. Each impression post was verified for an intimate fit against the multibase abutments (Figure 11 and Figure 12).
The verification jig was returned to the laboratory and a bite rim was fabricated using two temporary abutments to stabilize the denture base against the implants in the mouth. The bite rim was used to establish lip support and to mark the proposed anterior tooth position as well as for a base for a bite record and facebow transfer.
The records were returned to the laboratory for the teeth to be set and then returned to the dental office for try-in. Heraeus Mondial® teeth (www.heraeusdentalusa.com) were specified because of the layering, coupled with NanoPearls® filler material because, in the author’s opinion, the nano-technology allows for excellent esthetics and wear resistance (Figure 13).
The case was tried in and the occlusion and tooth arrangement were verified. The need for minor corrections to the midline was noted and the case was returned to the laboratory for the alterations and the final processing of the case. The laboratory model was scanned and the framework was designed and then milled from that scan. Milled frameworks are significantly more accurate in fit than those fabricated from the more traditional lost-wax technique.3 The milled framework was thickened in the right posterior secondary to the long cantilever. Generally, the length of a cantilever is kept below 16 mm to prevent both tooth and/or bar fracture. In this case, the length was 25 mm. However, with the increased thickness of the bar and the adequate intermaxillary space to allow for increased thickness of acrylic, it was hoped that the risk would be lowered (Figure 14).
The case was carried to the mouth and screwed to place. The occlusion was finalized and the teeth were polished and the screws torqued to 35 Ncm. The screw-access holes were protected with a small amount of light-bodied polyvinylsiloxane impression material. Well-fabricated hybrids have very small access openings to protect the integrity of the prosthesis. Larger openings can lead to teeth popping off of the framework, or even acrylic fracture.
The remaining space was filled with Heraeus Venus Pearl composite in a shade that was slightly different than the teeth. Because the screw holes were in a non-esthetic area, the color difference will be useful when the screws need to be accessed for maintenance. Off-color composite is easier to remove without making the hole wider and causing compromise to the strength of the prosthesis. The composite was then polished (Figure 15 and Figure 16).
The patient was instructed to return after 1 week to check occlusion and was also given home-care instructions. In follow-up care, the hybrid is removed on a periodic basis for cleaning and evaluation of the tissue around the implants. The screws are replaced after three cycles of removal and being torqued so that they would not fatigue to the point of breaking.
Disclosure
The author received material support from Heraeus to complete the case presented in this article.
References
1. Mozzati M, Arata V, Gallesio G, et al. Immediate postextraction implant placement with immediate loading for maxillary full-arch rehabilitation: A two-year retrospective analysis. J Am Dent Assoc. 2012;143(2):124-133.
2. Drago C, Saldarriaga RL, Domagala D, Almasri R. Volumetric determination of the amount of misfit in CAD/CAM and cast implant frameworks: a multicenter laboratory study. Int J Oral Maxillofac Implants. 2010;25(5):920-929.
3. Gallucci GO, Papaspyridakos P, Ashy LM, et al. Clinical accuracy outcomes of closed-tray and open-tray implant impression techniques for partially edentulous patients. Int J Prosthodont. 2011;24(5):469-472.
About the Author
Steve Ratcliff, DDS, MS
Executive Vice President
Spear Study Clubs
Resident Faculty
Spear Education
Scottsdale, Arizona