Monolithic Zirconia Crowns and Bridges
New all-ceramic, CAD/CAM-fabricated crowns and bridges are unbreakable and less expensive than traditional full-coverage PFM restorations.
Every type of full-coverage restoration, from single unit to the classic roundhouse, has been fabricated using the workhorse of modern dental practice, the porcelain-fused-to-metal crown (PFM).1 When full coverage is required, the PFM has become the restoration of choice for most dentists. A new all-ceramic, CAD/CAM-fabricated, inexpensive, and unbreakable dental crown may be ready to replace the traditional PFM without any change in clinicians’ current full-coverage armamentarium or techniques.
Full-Contour Monolithic Zirconia Crowns
The development of full-contour monolithic zirconia (MZ) crowns2 promises an end to the heartbreak of fractured esthetic porcelain on posterior crowns and bridges. MZ crowns can be prepared just like conventional PFM crowns using either a butt shoulder, a chamfer, or a knife-edge finish line.3 MZ crowns may be fabricated with as little as 0.5-mm of occlusal reduction, and most importantly, MZ crowns can be cemented using the clinician’s choice of favorite conventional cement.4 The only difference between an MZ crown and a conventional PFM crown can be summed up in one word—unbreakable.
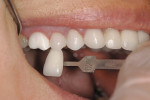
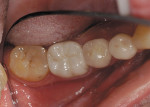
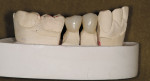
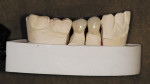
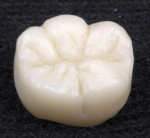
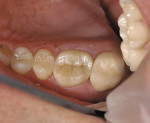
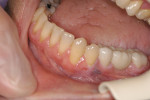
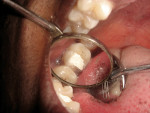
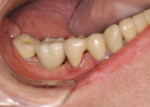
The author has noted positive results with new MZ crowns and bridges in his practice during the past 2 years. The early restorations were often rather boxy-looking and although the color was close to the desired shade, the final restoration was usually too high in value ( Figure 1 and Figure 2). However, the shapes and contours of the new MZ crown are easily altered using a low-speed green stone.5 MZ is very easy to shape and it is equally easy to polish using conventional low-speed porcelain-polishing materials.6 It only takes a few minutes to correct the occlusion and any contour issues and achieve a very smooth finish for the final restoration ( Figure 3). Because MZ crowns are the same color all the way through, they will not exhibit the opaque show-through so often seen when adjusting the occlusal portion of a PFM crown.
Wear Characteristics of MZ Crowns
Although the author has not conducted research regarding the wear factor against opposing natural-tooth enamel, the smoothness of the surface of the MZ restoration—along with point-fossa contact with the opposing arch—has not caused any noticeable wear on the opposing natural dentition during his 2 years’ experience with MZ crowns.
Controlled studies of MZ crowns have shown wear against opposing natural-tooth structure to be only slightly less abrasive than natural tooth enamel.7 When comparing highly polished and glazed MZ crowns and IPS® e.max crowns (Ivoclar Vivadent, www.ivoclarvivadent.com), studies have documented that MZ crowns are just slightly less abrasive against natural tooth enamel than e.max crowns.6 When compared to other less robust full-coverage options, the MZ crown is unbreakable and less abrasive to natural enamel than any other full-coverage ceramic system.8
Chemistry and Technical Aspects
Zirconium is one of the most abundant elements in the earth’s crust.9 Zirconia is formed by the addition of oxygen to the pure, elemental zirconium metal.10 The addition of minor components to the zirconia, such as yttrium, can produce a crystal that is both strong and resistant to crack generation because of the unique “transformation toughening” that occurs when zirconia goes from a tetragonal phase to a monolithic phase.11 It is this monolithic phase of zirconia that is so resistant to breakage when used in full-coverage restorations.12
Monolithic zirconia restorations begin their journey as chalky white blocks ( Figure 4). They are milled to their designed shape and then are soaked in a dyeing liquid to approximate the requested VITA® shade (Vident, www.vident.com) ( Figure 5 ).13 The dyeing liquids have improved over the past 2 years and likely will continue to evolve. The final VITA shades of the MZ crowns now being shipped by laboratories seem to be more consistent than was imaginable only 2 years ago ( Figure 6 ).
Recent changes in coloration protocol for MZ restorations have seen the introduction of a three-zone coloring system. First, the un-sintered restoration is brushed with the desired final color around the cervical zone of the crown. Next, the body of the crown is brushed with the desired body shade. Finally, effect shades are used to characterize the occlusal area of the crown.14
After the milled crown has been shade-adjusted in the coloring solution, it is sintered in an oven for 6.5 hours at 1,560ºC.15 Sintering drives the tetragonal zirconia to its monolithic phase and the gives the milled crown its great resistance to fracture and breakage.16 During the sintering process, the zirconia shrinks and becomes much more dense. A computer program is used to increase the size of the crown during the milling process to compensate for the shrinkage that occurs during the sintering process.17
Resistance to fracture and crack propagation makes full-contour MZ an ideal material to fabricate bridges for posterior teeth ( Figure 7). To be sure the bridge will not fracture, each connector must have a calculated number of 27 or higher. The number is determined by measuring the connector area. The height, width, and depth of the connector, when combined, must equal 27 or greater.5,18 The connector is measured in millimeters and the results are multiplied to obtain the final number.
With adequate connector size, three-, four-, and even six-unit bridges are very predictable using full-contour MZ.19 Using conventional PFM cementation techniques, these bridges are easily cemented and the clean-up is very simple.
Soft-Tissue Response to MZ
The soft-tissue response to MZ crowns has been very encouraging. They promote a soft-tissue response very similar to porcelain veneers; the tissue stays pink and stippled and healthy ( Figure 8). The high biocompatibility of zirconia is evidenced by the success rate when using zirconia medical implants for procedures such as hip replacement.20-22 Advantageous clinical properties—such as reduced bacterial adhesion, ease of manipulation, high strength, and polishability, along with superior resistance to fracture—combine to make MZ crowns the ideal choice for posterior full-coverage restorations.5
Highly polished ovate pontics are easily cleaned and maintained, and the resistance MZ restorations show to bacterial adhesion encourages a healthy response from surrounding soft tissues. The ease of shaping and polishing MZ restorations provides a nature-mimicking environment that contributes to the health of soft tissues surrounding these crowns and bridges ( Figure 9 and Figure 10).
Because the MZ crowns are tooth-colored, finish lines may be either supragingival or subgingival. Very often the length of the clinical crown determines the position of the finish line. A short clinical crown may require a subgingival finish line in order to have a significant ferrule for retention of the MZ restoration.
MZ for Implant Restoration
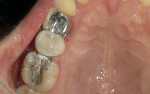
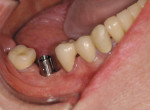
Full-contour MZ is ideal for the restoration of dental implants on posterior teeth. The natural opacity of the material combined with the full depth of color hides even the darkest metal abutments without having a grey cast ( Figure 11 and Figure 12). If space is a problem, the MZ crown or bridge can be fabricated to a thickness of 0.5 mm and will still be resistant to breakage and will not demonstrate the opaque show-through of the metal so often seen on occlusally thin PFM restorations.
Discussion
MZ full-coverage restorations have begun a revolution that just may lead to the demise of the PFM. The advantages of MZ crowns are numerous. They can be prepared just like the preferred posterior full-coverage preparation. Full-shoulder, chamfer, or even knife-edge finish lines are acceptable for MZ crowns. In tight occlusal areas, like second molars, as little as 0.5 mm of occlusal reduction is adequate for strength and block-out of underlying tooth structure. Three-, four-, and even six-unit bridges may be fabricated using MZ, as long as the connectors are developed using the suggested guidelines.
Final impressions for MZ restorations can be made with the clinician’s preferred impression material. Polyethers, polyvinylsiloxanes, or even digital impressions using a CAD/CAM camera may be used to capture the MZ crown-preparation impression. The digital images may be e-mailed to the dental laboratory for fabrication of MZ restorations.
The marginal adaptation of MZ crowns is exceptional. The restorations are milled in a CAD/CAM process that produces a precise marginal fit. Whether the restorations are produced from a conventional impression and scanned at the dental laboratory or from a dental office-generated digital image, the finish margin fit of the final restorations is excellent.
When adjusting the occlusion on an MZ restoration, there is no need for concern about opaque or metal show-through because the color of the restoration is homogeneous throughout the restoration. Shape and contour adjustments are easily accomplished using a diamond or small green stone and any conventional extraoral ceramic polishing kit. The restorations are very strong, and occlusal adjustments can be made before the unit is cemented, allowing for final polishing of the restoration in the laboratory, rather than in the patient’s mouth.
Because the restoration is so resistant to fracture, conservative preparation is encouraged; because the restoration is homogeneous in nature, there is no esthetic ceramic component to fracture during occlusal loading. Research has found MZ crowns are less abrasive to opposing natural dentition than most other full-coverage restorations. The tissue response to MZ is very favorable. Resistance to bacterial colonization helps keep the soft tissue surrounding MZ restorations much healthier-looking at re-care visits.
Perhaps the greatest advantage of MZ crowns is the fact that they require less time to fabricate and are, therefore, less costly than conventional PFM restorations. For those who send digital impressions to their dental laboratories, the cost of MZ crowns is even less, because the laboratory does not need to make a stone model for fabrication of the MZ crown. Less laboratory time translates into a lower cost to the dental office.
The disadvantages of MZ crowns are mostly related to development of the final shade of the restorations. Although the restorations are fabricated using a color dip that is prepared to mimic the VITA shade guide selection system, some units can appear to be a higher value than the shade requested. This problem was more significant with the restorations that were fabricated during the author’s earliest experience with MZ crowns; while there may be an occasional restoration that is too high in value, for the most part the color of the restorations is very close to the requested VITA shade now.
Although MZ crowns can be used anywhere in the mouth, their esthetic value is lower than full- coverage esthetic restorations such as IPS e.max. MZ crowns are presently fabricated as one homogeneous color from gingival to incisal edge. Although these restorations can be fully contoured and their appearance at conversational distances may be satisfactory, upon close inspection they lack incisal translucence and highlight and as well as the transitional coloration seen in natural dentition. While surface colorants have been added to help adjust the color of MZ crowns and to make the units look better for anterior applications, these surface colorants can wear and leave the underlying MZ crown exposed in its original color. Also, crowns with surface stains are not as smooth as highly polished and glazed monolithic zirconia, so these units may be more abrasive to the opposing natural dentition. An additional disadvantage may be increased bacterial colonization where the stain has been applied.
MZ crowns may be just the answer for patients with CNS (central nervous system) clenching or grinding, who find it difficult to wear a guard and are generally not as concerned about high esthetic value because they are accustomed to badly worn and broken anterior teeth.
Conclusion
Analysis of current literature indicates that not much has been written yet about monolithic zirconium full-coverage restorations. It remains to be seen how these seemingly indestructible restorations will evolve and how they will be embraced or rejected by the profession. The author’s initial impression is that there will be great improvement in the esthetic development of MZ crowns and that their ease of use and many other advantages will exert considerable pressure on the traditional PFM restoration.
MZ crowns were initially developed for use in patients with a tendency to break the esthetic ceramic material of conventional posterior crowns. Patients who are known CNS bruxers, habitual grinders, chronic clenchers, and have broken conventional restorations are the best candidates for MZ crowns. In their present state, MZ crowns are appropriate for use on molars, bicuspids, and cuspids that are not in the esthetic zone. Their ease of use and advanced resistance to breakage makes them ideal for use in all posterior full-coverage restorations.
Acknowledgments
The author would like to extend thanks to those at Glidewell Dental Laboratory, Newport Beach, California, and Great White Dental Laboratory, Santa Maria, California for their dedication to the continued development of the MZ restoration for use in all posterior teeth, which promises an exciting future for the dental profession.
References
1. Shenoy A, Shenoy N. Dental ceramics: An update. J Conserv Dent. 2010;13:195-203.
2. Comlekoglu K, Dundar M, Ozcan M, et al. Influence of cervical finish line type on the marginal adaption of zirconia ceramic crowns. Oper Dent. 2009;34(5):586-592.
3. Rekow ED, Silvia NR, Coehlo PG, et al. Performance of dental ceramics: challenges for improvements. J Dent Res. 2011;90(8):937-952.
4. Guess PC, Zhang Y, Kim JW, et al. Damage and reliability of Y-TZP after cementation surface treatment. J Dent Res. 2010;89(6):592-596.
5. Moving to monolithic: New price-competitive materials and techniques give laboratories affordable and automated CAM solutions. Inside Dental Technology. 2011;2(1):70-71.
6. Jung YS, Lee JW, Choi YJ, et al. A study on the in-vitro wear of the natural tooth structure by opposing zirconia or dental porcelain. J Adv Prosthodont. 2010;2(3):111-115.
7. Shah S, Michelson C, Beck P, et al. Wear of enamel on polished and glazed zirconia. 2010; AADR. Abstract No. 129615.
8. Krebs RE. The History and Use of Our Earth’s Chemical Elements: A Reference Guide. Westport, Connecticut: Greenwood Press; 2006:123.
9. Wolf C. Sol-Gel formation of zirconia: preparation, structure and rheology of sols. J Mater Sci. 1992;27(14):3749-3755.
10. McLaren EA. Zirconia-based ceramics: materials properties, esthetics, and layering techniques of a new veneering porcelain, VM9. Quintessence. 2005;28:99-111.
11. Wachtman JB. Mechanical Properties of Ceramics. Hoboken, New Jersey: Wiley and Sons; 2009:228.
12. Yaunfu Y, et al. Strength and fracture mode for dental colored ZrO2 ceramics coated with dental porcelain. Key Engineering Materials. 2008;368-372:1248-1251.
13. Tauro V. Evolution to revolution: creating a highly esthetic full-contour monolithic restoration. Dental Lab Products. 2011;5:28-31.
14. Curran DJ, Fleming TJ, Towler MR, Hampshire S. Mechanical properties of hydroxyapatite-zirconia compacts sintered by two different sintering methods. J Mater Sci Mater Med. 2010;21(4):1109-1120.
15. Sato K, Abe H, Ohara S. Selective growth of monoclinic and tetragonal nanocrystals. J Am Chem Soc. 2010;132(8):2538-2539.
16. Curran DJ, Fleming TJ, Towler MR, Hampshire S. Mechanical properties of hydroxyapatite-zirconia compacts sintered by two different sintering methods. J Mater Sci Mater Med. 2010;21(4):1109-1120.
17. Lee HH, et al. Factors Affect Fracture Resistance of Three-Unit Zirconia Posterior Bridge. Study: School of Dentistry, Department of Biomaterials Science, Dancock University, Cheonan, South Korea. 2011; IADR/AADR/CADR 89th General Session and Exhibition. March 16-19, 2011.
18. Data on file. Technical Update: Do Not Use Discs to Finish Full Contour Zirconia. Blog.Bruxxir.com. 2010. Glidewell Laboratories.
19. Blaschke C, Volz U. Soft and hard tissue response to zirconium dioxide dental implants: a clinical study in man. Neuro Endocrinol Lett. 2006;27 Suppl 1:69-72.
20. Data on file. Yttrium Stabilized Zirconia. Scientific Review, Astra Tech Dental. 2009:1-4.
21. Hisbergues M, Vendeville S, Vendeville P. Zirconia: established facts and perspectives for a biomaterial in dental implantology. J Biomed Mater Res B Appl Biomat. 2009;88(2):519-529.
22. Aherne T, Aherne S. Zirconia abutment for the single tooth implant. Implant Practice. 2008;1(1):8-14.
About the Author
Harry A. Long, DMD
Private Practice
Wayne, New Jersey