A “Resin Cone Technique” Using Giomer Products
Introducing a new type of bioactive composite resin material that contains surface pre-reacted glass ionomer.
John C. Comisi, DDS, MAGD
Composite restorations have become a staple of the dental profession when placing direct restorations. They are very easy to use; however, they do have challenges associated with this use. Bond failure, of course, is one of the primary difficulties with composite. Reliable long-term bond adhesion1,2 has been shown to be difficult to achieve. Polymerization of composite is another challenge. The enamel cusp deformation or C Factor is created in all composite restorations. When clinicians bond to the dentinal structure of the tooth, highly stressed mechanical bonds are set up to the active biological surface.3 Multiple techniques and thoughts on how to overcome this stress have been postulated through the years.4,5 To date there has been limited success in the attempt to overcome this problem.
Flowable composites have been considered an answer to some of the problems associated with this polymerization shrinkage. It has been thought that they can provide an elasticity, higher adhesion, and mechanical integrity to “absorb” and buffer some of the contraction stresses and help reduce this shrinkage.6 These liners are also thought to be able to counterbalance the C factor.7,8
This concept can be challenged by a simple test that can be easily performed by every clinician to determine the ability of their flowable composite to reduce polymerization shrinkage. First, place a Mylar strip on the countertop. Then dispense the flowable composite of choice onto the Mylar strip. Light-cure the material for 10 to 20 seconds. Observe the pulling on the Mylar strip that has occurred. Perhaps flowable composites do not assist clinicians as much as they think in reducing the stresses on the tooth structure.
Resin-modified glass ionomer (RMGI) has long been suggested as a solution to this polymerization shrinkage problem. It has been shown time and time again that this important material exhibits the low modulus of elasticity, low viscosity, self-adhesive properties to dentin and enamel,9 and fluoride release and ability to recharge10 needed for successful restorations. Glass ionomer (GIC) and resin-modified glass ionomers (RMGI) have for many years been found to be extremely useful in reducing polymerization shrinkage and sensitivity. The use of these materials has many advantages as liners and bases. The application is much less technique-sensitive, and they can be bulk filled, which is especially useful in deep cavity preparations. Various types of sandwich techniques have been suggested in the restoration of posterior teeth, and their success has been documented in the literature.11,12
Lately, there have been a number of companies creating “bulk fill flowable composites,” promoted to be the solution to the polymerization shrinkage problems. As much as we all want to be able to bulk fill with these materials, there must come to mind some question as to whether this can really be done. These composites claim the ability to bulk fill up to 4 mm at a time. However, these materials will still shrink when polymerized, and the C factor will likely still be a problem. Many of these products also claim to be fluoride releasing, which they very likely are. However, all but one of the composites currently available cannot recharge with fluoride and provide long-term caries resistance as a GI or RMGI can.
The one exception to the rule that the author has found is Beautifil® Flow Plus (Shofu, www.shofu.com) (Figure 1). This is a giomer product. What is a giomer? It is a new type of bioactive composite resin material that contains surface pre-reacted glass ionomer (S-PRG). This proprietary S-PRG process gives the product properties that enable fluoride release and recharge; properties very much like that of GI and RMGI materials. Yet this flowable material has been reported to have low polymerization shrinkage with the strength and functionality to meet and surpass the leading hybrid composites and can be used in all classes of restoration. This material stays where it is placed.
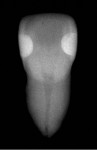
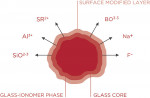
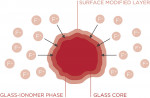
This material comes in two viscosities: the Zero Flow (F00) and Low Flow (F03) (Figure 2). Its delivery system provides precise handling, great adaption, and is self-leveling. The material is more radiopaque than enamel (Figure 3), and has been shown in an 8-year clinical study13 to inhibit secondary caries,14 have no postoperative sensitivity, and maintain a high degree of its luster at recall. It has been shown in these studies to form an acid-resistant layer, reinforce the tooth substance, remineralize dentin, and have an anti-plaque effect and an acid-buffer capacity because of its ability to release various ions into the oral cavity (Figure 4 and Figure 5).
With this in mind, the author sought to devise a methodology to use this material in a way to reduce the stresses placed on the teeth being restored, using the physical properties that the material possesses to enhance the restorations. This led to the development of a modified “Resin Cone Technique.” Simply stated, it is the use of individual resin cones in different parts of the cavity preparation that are then connected together using the two viscosities of Beautifil® Flow Plus to create the restoration. In this case, the two different viscosities are being used to build up the missing tooth structure as illustrated (Figure 6).
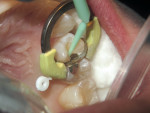
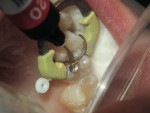
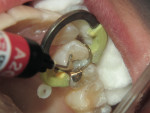
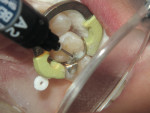
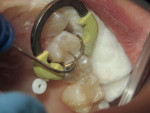
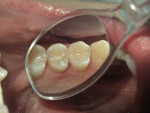
First place the matrix band of choice and then apply a bonding agent (in this case BeautiBond®) and cure. In this Class II preparation, the proximal box is filled with F00 material and cured (10 to 20 seconds), and then the furthest portion of the tooth away from the box is filled with F00 and cured. Finally, the space between the two cured aspects is filled with F03 and cured. The surface is then trimmed to occlusion and polished using polishers such as OneGloss® by Shofu (Figure 7, Figure 8, Figure 9, Figure 10, Figure 11, Figure 12, Figure 13, Figure 14, Figure 15).
This technique can also be used in restoring Class I restorations. Again, place the bonding agent and cure the adhesive. Then, using F00 to create the cuspal inclines on the occlusal surface, curing each incline for 10 seconds before creating the next. Once the inclines have been created, flow F03 material to fill in the valleys and connect all the inclines.
The “resin cone technique” results thus far have been very favorable and the author’s clinical work has shown that it has reduced sensitivity and excellent wear in the cases he has initiated. This technique gives the clinician one more avenue to provide superior easy-to-place direct resin restoration with less stress on the tooth, which provides a bioactive, glass-ionomer like benefit to help reduce plaque build-up, as well as help remineralize and strengthen the dentition.
References
1. DeMunck J, Van Landuyt K, Peumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84(2):118-132.
2. Erhardt MC, Shinohara MC, Bedran-Russo AK, et al. Effect of long-term water storage on etch-and-rinse and self-etching resin-dentin bond strengths. Gen Dent. 2008;56(4):372-377.
3. Carvalho RM, Santiago SL, Fernandes CA, et al. Effects of prism orientation on tensile strength of enamel. J Adhes Dent. 2000;2
(4):251-257.
4. Deliperi S, Bardwell DN. Oblique placement of material to help reduce polymerization shrinkage. J Am Dent Assoc. 2002;133(10):1387-1398.
5. Nash RW, Lowe RA, Leinfelder K. Use of packable composites for direct placement. J Am Dent Assoc. 2001;132(8):1099-1104.
6. Montes MA, de Goes MF, Ambrosano GM, et al. The effect of collagen removal and the use of a low-viscosity resin liner on marginal adaptation of resin composite restorations with margins in dentin. Oper Dent. 2003;28(4):378-387.
7. Alomari QD, Reinhardt JW, Boyer DB. Effect of liners on cusp deflection and gap formation in composite restorations. Oper Dent. 2001;26(4):406-411.
8. McCullock AJ, Smith BG. In vitro studies of cuspal movement produced by adhesive restorative materials. Br Dent J. 1986;161
(11):405-409.
9. Tolidis K, Nobecourt A, Randall RC. Effect of a resin-modified glass ionomer liner on volumetric polymerization shrinkage of various composites. Dent Mater. 1998;14(6):417-423.
10. Forsten L. Fluoride release and uptake by glass ionomers and related materials and its clinical effect. Biomaterials. 1998;19(6):503-508.
11. Miller MB, Castellanos IR, Vargas MA, Denehy GE. Effect of restorative materials on microleakage of Class II composites. J Esthet Dent. 1996;8(3):107-113.
12. Hewlett ER, Mount GJ. Glass ionomers in contemporary restorative dentistry—a clinical update. J Calif Dent Assoc. 2003;
31(6):483-492.
13. Gordan VV, Mondragon E, Watson RE, et al. A clinical evaluation of a self-etching primer and a giomer restorative material: results at eight years. J Am Dent Assoc. 2007;138(5):621-627.
14. Saku S, Kotake H, Scougall-Vilchis RJ, et al. Antibacterial activity of composite resin with glass-ionomer filler particles. Dent Mater J. 2010;29(2):193-198.
About the Author
John C. Comisi, DDS, MAGD
Private Practice
Ithaca, New York



 ® Flow Plus." title="Figure 6">
® Flow Plus." title="Figure 6">