Upgradeable Dentistry
A new treatment paradigm for total patient care.
By Richard B. Winter, DDS
Dental school prepares dentists for technical application of dental principles based, in part, upon the disciplines of chemistry, physics, material science, and prosthodontics as they pertain to the stomatognathic system. A major challenge of the dental school curriculum is to also educate dentists about the psychogenic issues facing patients as well as their economic limitations and how to help patients realize the dentistry that will be most beneficial for them over time.
Restorative dentistry presents a plethora of materials and options. Therefore, philosophical and economic decisions can help guide restorative selection. Further exacerbating the decision-making for patients who are partially dentate or edentulous are the added choices required for prosthodontic rehabilitation. To that end, the education process as it pertains to patients can be simplified by actively engaging them in the selection of dental care that fits their personal situation with an eye toward dynamic realization of their treatment goals over time. Patient education in complex restorative situations requires treatment planning that allows patients to sequence care in a way that keeps them engaged in the dental practice. The author has introduced a concept that defines this sequencing in a manner that can be applied both from a restorative or prosthodontic perspective.
Defined as "upgradeable dentistry," this paradigm enables a dentist to present comprehensive dentistry to patients that will allow them to sequentially change their oral foundation, support, prostheses, and function according to their emotional, financial, and anatomic readiness.1,2
The literature is replete with publications and research to support the sequelae of long-term denture wear from bone loss to nerve dehiscence. Denture principles as outlined by Drs. Pound,3 Turbyfill,4 and Mossad5 provide prototype restoration that can allow patients to prevue their restorative goals. These functional "provisionals" are an art form that when properly applied can allow patients to pursue "upgrade paths" while enjoying proper esthetics, phonetics, and function. This will free the patient to concentrate on restoring the osseous foundation and stabilization of bone loss and dentures with the sequential addition of small-diameter or traditional implants.
Dentists are often guilty of identifying a patient as an event—a "set of dentures" or a 2-implant overdenture—when in reality that would end the patient’s relationship with their practice. Concentrating on proper dialogue will allow patients to remain engaged in their ongoing care.
Clinical Reality with Style
According to Misch, 10.5% of the adult population, or 18 million people, are edentulous in both arches.6 Furthermore, 30 million people, or 17% of the entire US population, have no teeth in a single arch.7 If unilateral quadrant edentulism is factored into the mix, 44 million people are included.7 This translates to 30% of all adults in the United States being candidates for some form of implant dentistry. With any treatment comes proper planning and evaluation, so the process of sequential rehabilitation begins with partials or dentures. These prototypic restorations are carefully fabricated to evaluate vertical dimension of occlusion, esthetics, phonetics, and function and, perhaps most importantly, patient desires and realistic expectations.
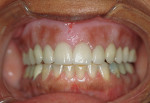
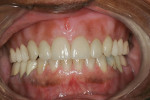
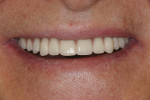
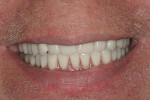
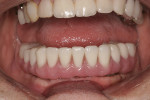
Figure 1 and Figure 2 show Turbyfill deluxe dentures,1,8 which were fabricated as the first upgrade for people whose dentures had been inadequate. The increased self-esteem these dentures afford has allowed many patients to further invest in implant dentistry to take their enhanced esthetics to another level of function.9
The deluxe denture is fabricated with functionally generated impressions and stable baseplates, with tooth arrangement being performed with the patient present. The 2 hours spent setting teeth to ideal esthetics, phonetics, and vertical dimension help create a doctor/patient relationship that is amenable to further discussion about the reasons for the denture being a "stepping stone" to better dental health and not a "destination." The Ivocap (Ivoclar Vivadent, www.ivoclarvivadent.us) or Success injection molding process (DENTSPLY Prosthetics, www.dentsply.com) utilizes Molloplast B (Detax GmBh and Co. KG, www.detax.de) or Lucisoft silicone liners (DENTPLY Prosthetics) and tinted denture bases that offer excellent denture comfort for patients who desire and value this service. In the author’s practice, dentures and partial dentures are referred to as temporary prostheses.
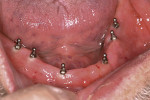
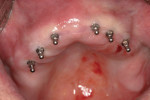
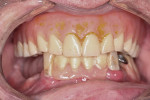
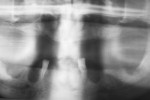
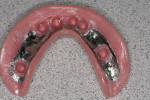
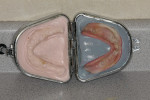
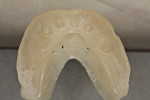
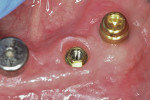
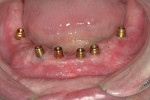
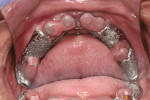
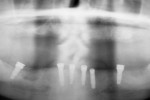
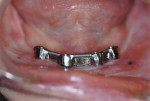
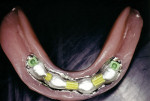
Small-diameter implants, as shown in Figure 3 and Figure 4, are used with a maximum A-P spread to stabilize implant overdentures. This patient had a price point that precluded bilateral sinus grafting with the placement of traditional implants and a bar overdenture, hybrid, or fixed bridgework. So the mini-implants, which can be used for long-term and ongoing care, can also allow for placement of traditional implants if a patient desires a fixed prosthesis in the future, as spaces have been created to accommodate these if desired.2,10 After 4 years this patient has remained satisfied and has no desire to upgrade.
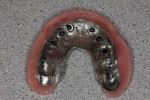
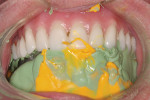
Figure 5 shows a metal-based overdenture with acrylic flanges that allows relines to be done in the future. This frame design has created space for keeper cap replacement or chairside pickup. The keeper caps can be incorporated into the partial denture frame and tried in to verify accuracy of the impression. (This can be seen in Figure 15 where it is done for traditional implants with Locators). Figure 6 shows the full-face smile set to a lingualized occlusion, which is preferred for the Turbyfill dentures and implant prostheses.4,11
When practitioners only follow certain dogma, they lose the ability to individualize treatment in a dynamic fashion. The question of whether or not a 2-implant overdenture is better than a 6-mini-implant overdenture, or a screw-retained hybrid is preferred over a cementable hybrid, or a bar-retained overdenture is superior to a fixed bridge on implants is academic if a patient does not understand any of these options. Financial considerations must be worked out so that a patient can choose an option, but the flexibility in implant treatment options needs to be discussed as well.
Literature supports the fact that implant-retained dentures are better than dentures.12,13 How much better is subjective, but when discussing Locator-based overdentures versus bar-retained overdentures, the cost may be the obstacle that allows one treatment to occur versus no treatment at all.
The Missing Link
The ability to provide surgical as well as prosthetic solutions can help a dentist to work out a case financially based upon a patient’s budgetary limits without worrying that a referral might result in lack of adequate funds remaining to complete the prosthetics of the case. While general dentists may not want to perform their own subantral sinus augmentation or symphysis block grafts, the implant dentist, globally, performs all stages of implant surgery and prosthetics. It is certainly within the scope of general dentistry for practitioners to become involved in whatever level of implant surgery and prosthetics for which they are willing to become comprehensively trained.
In the case presented, a 55-year-old man presented with traumatic bone cysts, pain, and mobility of remaining teeth from prolonged wearing of an upper complete denture and a lower partial denture (Figure 7). After a CAT scan appliance and scan were performed, the area was prepared for 6 BioHorizons® (www.biohorizons.com) implants, grafting, and enucleation of the cysts. The lesions were biopsied and found to be benign hyperplastic tissue (Figure 8). A new set of provisional dentures was fabricated to confirm ideal esthetics, phonetics, and function prior to fabrication of a metal frame reinforced Locator® overdenture (Zimmer Dental, www.zimmerdental.com) (Figure 9). A clear Lang duplicate of this denture was fabricated and the clear acrylic was mixed with barium sulfate to generate a CAT scan appliance that would allow assessment of interocclusal space, tooth positioning, anatomic landmarks, and ideal implant placement. Figure 10 shows the Lang duplicate of the approved denture; Figure 11 shows the barium sulfate clear duplicate, which was to be used as a surgical guide as well. Figure 12 displays the tissue health of the permucosal extension and uncovered implant and placed Locator attachment.
Six Locator attachments are shown in Figure 13, affixed to the implants that had been placed 5 months previously. Once the implants had integrated and PMEs had been allowed to model the soft-tissue contours for a month, the appropriate sizes of Locators were ordered. After placing the attachments, the seating was radiographically verified and the attachments were torqued to 20 Ncm. The clear denture duplicate was used as a surgical guide and as a custom tray for a final impression. To do this, the duplicate was hollowed out around the Locator attachments, vent holes were placed, and passive seating as well as good intercuspation with the opposing denture was verified prior to making the master impression (Figure 14). Impression material was placed in the tray (Aquasil™, DENTSPLY Caulk, www.dentsply.com), and the patient closed into maximum intercuspation.
Impression material was also placed on the occlusal surface so that the laboratory would have incisal edge position, vertical dimension of occlusion, and proper bite registration while loading the condyles into the superior most braced position. This bite was approved from months of the patient wearing his provisional dentures during implant integration and was matched and verified during the impressioning appointment. Figure 15 shows the metal framework with the locator males attached to the frame for chairside verification of fit both visually and tactilely. Should there have been any problems they could have been removed and cold-cured to the frame chairside. Alternatively, a chairside pickup would have been accomplished after processing.
The Panorex in Figure 16 shows implant placement with optimal A-P spread; the lesions have all filled in post-grafting. The completed overdenture in Figure 17 has resulted in increased patient self-confidence and mastication force. The retention was excellent and the patient was thrilled to be able to eat peanuts again. This patient may choose to upgrade this prosthesis by placing two or three more implants. Then an FP-3 (fixed porcelain bridge with pink porcelain for gingival replacement) prosthesis or hybrid can be considered to convert his lower prosthesis from removable to fixed. Figure 17 shows his final smile; he is most satisfied with the functional improvement from the preoperative presentation shown in Figure 7.
Performing the procedure in the office allowed the author to save the patient at least $5,000 by treating him independently. He has now scheduled his bilateral subantral sinus augmentation with a maxillary bar overdenture. Patients may opt to increase their dental budget based on the perceived value of the service they desire. This patient now wants to get rid of his palatal acrylic and wants to place six to nine maxillary implants to continue his oral rehabilitation.
The most salient point of this case presentation is to realize that the patient is now educated and motivated because he understands and wants to avoid "combination syndrome" (further deterioration and atrophy of the bone under the denture opposing a rigid prosthesis).14 Before mandibular treatment is begun, there will be a discussion of the acceptability of the maxillary denture preoperatively with regard to stability and comfort. Once the mandibular denture is stable, however, the mobility of the maxillary denture will be quite noticeable. This should be discussed before the patient accuses the restoring dentist of making the maxillary denture less than satisfactory. The question of what level of care a patient can accept is multifaceted. Clinicians need to be advocates for their patients on their journey toward ideal dental health.15
While providing implants in the ABCDE position between the mental foramina will allow for a screw-retained hybrid, as seen in Figure 18, there are times when a bar overdenture may be a preferred treatment option (Figure 19 and Figure 20 ). This is based on a myriad of factors, which include interocclusal space, patient force factors, financial ability, bone levels, and patient requests, just to name a few.
Conclusion
Treatment planning is a complex discipline that can be confusing and multifaceted. Dentists are often unprepared to discuss complex "upgrade" paths with their patients due to their own incomplete understanding of current implant treatment options and their associated costs. Treatment planning the prosthetics in an implant case cannot occur without a thorough understanding of all surgical fees, laboratory costs, time required to complete the case, and knowledge of a doctor’s overhead. The pursuit of a comprehensive interdisciplinary treatment flowchart will result in providing more complete dentistry for patients over time. The incorporation of implant dentistry both surgically and prosthetically within one’s practice will facilitate lower costs as well as better-educated patients who will be more engaged in the pursuit of ideal dentistry.
Disclosure
Dr. Richard Winter reports no financial interests in anything mentioned in this article.
Acknowledgments
The author wishes to thank Drs. Charles Winter, Leonard Machi, and John Werwie for their selfless mentorship and support and teaching him to "listen to patients" and to always be their advocate for ideal dentistry.
References
1. Winter RW. Upgradeable dentistry, part 1. Dent Today. 2009;28(6):82-87.
2. Winter RW. Upgradeable dentistry, part 2. Dent Today. 2009;28(7):97-100.
3. Pound E. Controlling anomalies of vertical dimension and speech. J Pros Dent. 1976;36(2): 124-135.
4. Turbyfill J. Excellence in complete dentures. Dent Econ. 1994;84(3):80-81.
5. Mossad J. An integrated approach to optimizing orofacial health, function and esthetics: A 5 year retrospective study. Intl J Perio and Rest Dent. 1998;18(1):70-79.
6. Misch CE. Dental Implant Prosthetics. 3rd ed. St. Louis, MO: Mosby Publishing Inc; 2005:4-7.
7. Centers for Disease Control and Prevention. Weekly Morbidity and Mortality Report—March 19, 1999. 1999;48(10):206-210. Available at: https://www.cdc.gov/mmwr/PDF/wk/mm4810.pdf. Accessed August 14, 2009.
8. Turbyfill WF. Impression techniques for removable partial dentures. Gen Dent. 2001;49(4): 358-364.
9. Turbyfill WF. Regaining pleasure and success with complete denture services. Int J Prosthodont. 1989;2(5):474-482.
10. Shatkin TE, Shatkin S, Oppenheimer BD, et al. Mini dental implants for long-term fixed and removable prosthetics: a retrospective analysis of 2514 implants placed over a five-year period. Compend Contin Educ Dent. 2007;28(2):92-99.
11. Misch CE, Bidez MW. Occlusal considerations for implant supported prostheses: implant-protective occlusions. In: Misch CE, ed. Dental Implant Prosthetics. St. Louis, MO: Mosby Publishings Inc; 2005:472-510.
12. Turbyfill WF. The successful mandibular implant denture-part one. Dent Econ. 1995;85(12):70-71.
13. Pavlatos J. The root-supported overdenture using the Locator overdenture attachment. Gen Dent. 2002;50(5):448-453.
14. Tolstunov L. Combination syndrome: classification and case report. J Oral Implantol. 2007;33(3):139-151.
15. Winter RW. Upgradeable dentistry, part 4. Dent Today. 2009;28(12):64-68.
About thr Author
Richard B. Winter, DDS
Private Practice
Milwaukee, Wisconsin