Direct Bonding
The use of direct composites offers a less costly but equally effective alternative to porcelain restorations.
By Chris W. Campbell, DMD
Even as early signs point to a recovery from the recent recession, dentists and patients alike are still feeling the pressure of an uncertain economic climate. As a result, many patients are seeking treatment options that can deliver excellent results, but at fee levels that are more financially palatable. A logical answer is the use of direct composite in areas where porcelain restorations have typically been used.
Case Report
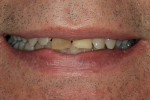
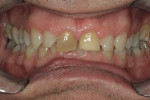
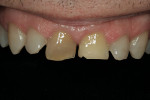
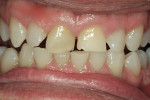
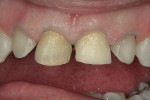
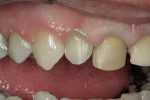
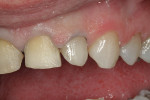
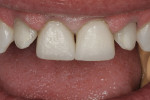
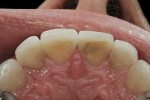
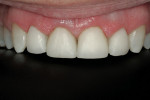
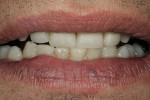
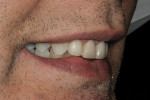
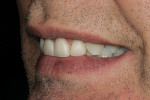
The patient was a 57-year-old man who frequently spoke in public and had been very self-conscious about his smile for a long time (Figure 1, Figure 2 and Figure 3). After completing diagnostic records consisting of study models, centric-relation record, facebow, and photographs, the patient was scheduled for a consultation two weeks later. Many functional and esthetic issues were noted during the treatment-planning phase. The patient exhibited heavy wear, large diastemas, and generalized moderate discoloration in his anterior teeth (Figure 4, Figure 5 and Figure 6). The discoloration was further complicated by an extremely discolored tooth No. 8, which surprisingly still tested vital.
During the patient’s consultation appointment, the treatment options discussed included orthodontics followed by porcelain veneers to address the patient’s esthetic and functional concerns. While the patient understood the benefit of this ideal course of treatment, it was not financially realistic for him. In search of other options, the pros and cons of direct bonding were discussed. The patient was encouraged by the prospect of initially avoiding orthodontics, the ability to repair, the almost immediate treatment result, and, perhaps most importantly, the restorative fee being roughly one third of what it would have been with porcelain.
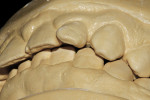
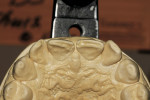
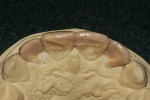
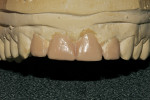
The first step was to begin the patient on take-home tray bleaching (Opalescence® 10%, Ultradent Products, Inc, www.ultradent.com), which he did nightly for approximately 5 weeks (Figure 7). While the patient was bleaching, the models were prepared similarly to the anticipated preparation design for the bonding procedure. At this point, teeth Nos. 7 through 10 were waxed (Pro-Art® wax, Ivoclar Vivadent, Inc, www.ivoclarvivadent.com) to proper contour. Careful attention was paid to incisal edge position, as this is a critical aspect in developing proper esthetics, phonetics, and anterior guidance (Figure 8 and Figure 9). The author prefers to wax up cases such as these in order to become familiar with the preparation design, and to have total control over the incisal edge position.
Once the diagnostic wax-up was complete, a putty matrix (Zhermack Platinum 85, Zhermack, https://en.zhermack.com) was fabricated to establish the lingual contours as well as the incisal edge position (Figure 10).
The author chose a microhybrid composite (Amaris®, VOCO America, www.vocoamerica.com) for this procedure; his selection was based on his experience of its straightforward shading approach and exceptional handling. The patient was administered 4% Septocaine® (Septodont, www.septodontusa.com) and 1:200,000 epinephrine, to allow for preparation into the dentin and provide tissue comfort during finishing and polishing. Once the teeth were prepared, a 000 retraction cord was placed on all four teeth (Figure 11, Figure 12 and Figure 13). Each tooth was bonded, one at a time, to full contour, in order to maintain the tooth shape established in the wax-up. Each tooth was etched, dried, and blotted with G5—to ensure that any exposed dentin was properly hydrated—and coated with dentin adhesive (Singlebond™, 3M ESPE, www.3m.com). The Singlebond was air-thinned with a warm air dryer and then polymerized for 10 seconds.
The matrix was seated after the adhesive was cured, and a thin layer of Amaris TL was applied to set the incisal edge position and the lingual contour. Once this first layer was cured, the matrix was removed, and O1 Amaris was applied to begin establishing the facial contours. The O1 composite, which serves as a "body" color, was layered more at the gingival than at the midfacial, and was ended just short of the incisal edge, to allow for lobe formation and incisal translucency. Amaris TL, which has optical properties that result in an increase in value of the final restoration, was used as the final layer, once the proper thickness of the O1 was cured. An initial polish was developed on the restoration before the next tooth was bonded in the same manner.
There are several ways to establish proper interproximal contacts. In this case, teflon tape was used on the adjacent teeth, which allowed for the enamel material to be teased into the contact area and cured. This technique is made possible by the handling properties of the chosen composite, and requires minimal finishing. Minimal occlusal adjustment was necessary after each tooth was bonded to full contour, as a result of the accuracy imparted by the matrix from the wax-up. All excursions were tested for proper canine guidance, and, most importantly, the lateral protrusive or "crossover" position. A final polish was established with the Enhance® Finishing and Polishing System (DENTSPLY International, www.dentsply.com) (Figure 14 and Figure 15).
The patient was reminded that the gingival architecture would continue to improve around his new restorations throughout the next few weeks. The patient returned for a 1-week post-operative appointment to verify esthetics, phonetics, and function, and was very pleased with the result (Figure 16, Figure 17 and Figure 18). Ultimately, the patient was quite appreciative of the effort taken to achieve his esthetic goals with a greatly reduced financial investment compared to what was considered "ideal" treatment.
About the Author
Chris W. Campbell, DMD
Private Practice
Lexington, South Carolina
Part-Time Faculty
Palmetto Health Richland GPR
Columbia, South Carolina