Eliminating a Removable Transitional Prosthesis
Using immediate implants and immediate fixed provisionalization to replace the mandibular anterior sextant.
By Douglas H. Mahn, DDS | Mariano A. Polack, DDS, MS
Replacement of the mandibular anterior sextant using immediate implants and a non-occlusally loaded fixed partial denture (FPD) represents a viable treatment modality. This approach is beneficial because it eliminates the need for a transitional removable prosthesis, reduces the number of surgical appointments, and decreases the time of treatment. This article describes a case in which the mandibular anterior sextant was treated with immediately placed and non-occlusally loaded provisionalized implants.
Using Immediate Implants
Traditionally, implants are placed in healed edentulous sites and allowed to heal for 3 to 6 months.1 Two common forms of provisionalization include tooth-supported FPDs or a removable interim prosthesis. Interim removable dentures can be uncomfortable and difficult for patients to accommodate. In addition, they may require frequent adjustments and relines, possibly increasing treatment time. Tooth-supported FPDs require adjacent teeth suitable for use as abutments. However, as the span of the edentulous site increases, this provisionalization method may not be viable.
The success of implants immediately placed into fresh extraction sites has been documented for years.2 More recently, reports of immediate implant placement and restoration have become common. These cases include single teeth,3 multiple teeth,4 and fully edentulous arches.5 Success rates in these cases have been reported to be similar to implants with traditional loading protocols.6,7
Immediate implants supporting a full-arch restoration are thought to benefit from the stability of cross-arch splinting that minimizes micro-movement during the initial stages of healing.8 Immediate provisionalization may be more difficult when the anterior sextant is involved because the benefits of cross-arch stabilization are lost. Furthermore, this area presents several challenges. The patient must be compliant with dietary restrictions including not biting into food, and protrusive contacts should be eliminated while maintaining esthetics. Nonetheless, the use of an immediate, non-occlusally loaded implant FPD may help prevent the aforementioned provisionalization challenges.
Case Report
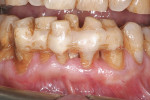
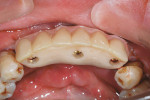
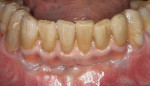
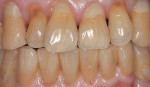
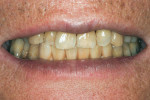
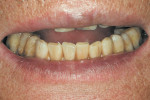
A 64-year-old man, a non-smoker with poor oral hygiene, presented with the chief concern of mobile mandibular anterior teeth. After clinical and radiographic examination, teeth Nos. 22 through 27 were found to have severe periodontal bone loss (Figure 1). These teeth had been splinted several years previously with composite resin on the buccal and lingual aspects. The entire group of teeth had Class II mobility and generalized tooth staining. After the findings were discussed with the patient, it was agreed to replace the anterior sextant with implant restorations. The patient’s objections to an interim removable restoration mandated the need for an immediate, non-occlusally loaded, provisional FPD.
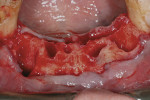
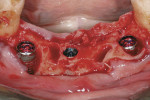
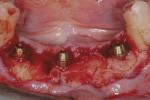
Profound local anesthesia was achieved using 2% lidocaine with 1:100,000 epinephrine. Intra-sulcular incisions were made with a No. 15 surgical scalpel. A full-thickness mucogingival flap was carefully elevated. Teeth Nos. 22 through 27 were removed as atraumatically as possible (Figure 2). Dehiscences in the alveolar bone were found associated with teeth Nos. 22 and 27. Implant osteotomies were made in site Nos. 22, 25, and 27. The goal was to position the implants in the lingual aspects of the extraction sites. Cylindrical, RBM-textured, threaded implants (PrimaConnex®, Keystone Dental, www.keystonedental.com) were placed in each site (Figure 3). Site No. 25 received a regular-diameter, 4-mm x 13-mm implant. Site Nos. 22 and 27 received wide-diameter, 5-mm x 13-mm implants. Insertion torque values greater than 35 Ncm were achieved with each implant.
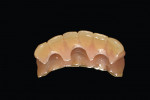
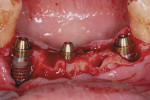
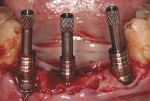
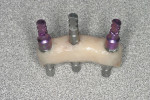
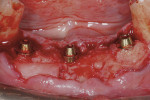
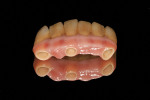
A provisional resin-based FPD, relieved on the lingual to allow space for implant components, was fabricated prior to the appointment (Figure 4). Conical multi-unit abutments (PrimaConnex) were placed on the implants and torqued to 30 Ncm (Figure 5). Next, gold cylinders (PrimaConnex) were connected to the abutments using waxing pins (Figure 6). Perforations were made on a rubber dam to allow the waxing pins and gold cylinders through, to protect the abutments and surgical wound. The provisional prosthesis was evaluated to ensure proper occlusion and clearance with the gold cylinders. Using a thin mix of polymethyl methacrylate (PMMA) the FPD was luted to the gold cylinders, thereby making the prosthesis implant-supported and retained (Figure 7). The restoration was then removed and implant analogs were connected to the gold cylinders (Figure 8) to prevent alterations in the inner surface of the latter during finishing procedures. The prosthesis was trimmed, and voids were filled with PMMA. The tissue side was contoured for hygiene accessibility and highly polished, while the occlusion was adjusted to prevent contact in centric and eccentric positions. It is important that the immediate provisional not have direct contact with the adjacent natural tooth to prevent any pressure during functioning that could create micromovement in the implant fixtures during healing.
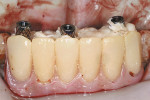
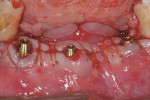
The osseous defects were grafted using demineralized freeze-dried bone paste (DynaBlast™, Keystone Dental) (Figure 9) and a resorbable regenerative membrane (BioMend® Extend, Zimmer Dental, www.zimmerdental.com) was placed over site No. 27 to further facilitate bone regeneration (Figure 10). The gingival flaps were secured around the conical multi-unit abutments with a continuous 4.0 chromic gut suture (Figure 11). The provisional FPD was secured to the multi-unit abutments using prosthetic screws torqued to 20 Ncm (Figure 12). The screw access holes, lingual to the acrylic teeth (Figure 13), were filled with cotton pellets and sealed with composite resin. The patient took 875 mg of amoxicillin twice a day for 10 days and used a chlorhexidine rinse twice daily for 2 weeks. He was instructed to brush and floss thoroughly after that. The patient was also instructed to maintain a soft diet and not to bite on the provisional prosthesis.
After 5 months of healing, the implant sites were found to be healing well. No implant mobility or sensitivity was found. Periodontal probing depths measured 2 mm to 3 mm. Mild gingival recession exposing the multi-unit abutment was found, especially around site No. 27. This prompted the decision to use implant-level abutments for the definitive prosthesis.
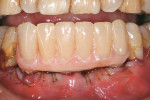
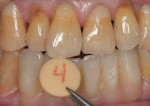
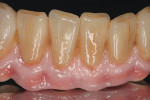
The provisional restoration was removed and an implant-level impression was made with closed-tray impression posts (PrimaConnex). A soft-tissue master model was fabricated and stock zirconia abutments (Esthetic Contour Zi Abutment, PrimaConnex) were prepared and adjusted in the laboratory (Figure 14). To replicate the patient’s low value, intense chroma, and highly characterized dentition, custom porcelain shade tabs were fabricated. Intraoral photographs were taken with the tabs placed next to the patient’s teeth (Figure 15). With this information, a CAD/CAM zirconia framework was fabricated and veneered with compatible porcelain after its accuracy and passive fit had been verified. Gingival-colored ceramics were used to develop harmonious tooth proportions (Figure 16 and Figure 17).9 The prosthesis was tried in and the interproximal contacts, occlusion, and esthetics were evaluated (Figure 18 and Figure 19). Access for oral hygiene was facilitated by the convex surface on the tissue side of the restoration. The abutments were torqued to 30 Ncm and the screw-access channels were sealed with gutta-percha and composite resin. The definitive FPD was cemented with resin cement (Figure 20 and Figure 21).
Discussion
Immediate placement of implants into fresh extraction sockets reduces morbidity and decreases time of treatment.2 Even in periodontally susceptible patients, implant survival rates are found to be comparable with those of healthy patients.10 The anterior mandible is typically an excellent site for immediate implant placement and provisionalization because of its good bone density and lack of anatomical limitations.4,11 However, some bone remodeling and gingival recession should be expected with this approach.12
Primary implant stability plays a critical role in implant success.13 This is achieved with insertion torque values greater than 35 Ncm, empirically believed to keep micro-movement below 150 µm.8,14,15 Greater mobility is assumed to bring about fibrous encapsulation.16 Additional recommendations by some authors include implants with a platform-switched connection and a soft diet during the healing stages.17-19 All of these were followed during the course of treatment.
The clinical team must determine the number of implants necessary to support a given restoration. Two immediately placed implants have been used to support an immediate, non-occlusally loaded provisional FPD replacing the mandibular incisors.4 Customizing this protocol, three implants were used because the restoration would replace the entire mandibular anterior sextant.
Implants were lingually placed due to concerns of buccal plate remodeling.12 Bone defects and open spaces around the implants were grafted with a demineralized bone matrix putty.20 This material has physical characteristics that facilitated proper placement and graft management during gingival flap replacement and suturing.
Conclusion
Immediate fixed provisionalization can be beneficial because it avoids the need for a removable prosthesis and second-stage surgery. In addition, the reduction in the number of surgical and restorative appointments may reduce costs for the clinician.
In full-arch, immediately loaded prostheses, cross-arch stabilization is thought to prevent micro-movement during the initial healing stages.17,21 On the other hand, single, immediately provisionalized implants are protected by keeping the interim restoration out of occlusion.22 Multiple implants in the same sextant may also lack the benefit of cross-arch stabilization if placed in a straight line. Therefore, they may need to be treated with non-occlusally loaded provisionals. The quality and quantity of bone in the anterior mandible, however, usually provides a sound foundation for successful immediate loading.19,21
Prosthesis design is of primary importance for accelerated protocols. A screw-retained provisional restoration is preferred because it may reduce extreme forces that could cause implant failure.21 In addition, the absence of cement avoids the risk of bone loss that could come from its inadequate clean-up.23 The provisional restoration should lack distal cantilevers and, if possible, have a group-function occlusal scheme.
References
1. Albrektsson T, Branemark PI, Hansson HA, Lindstrom J. Osseointegrated titanium implants. Requirements for ensuring a long-lasting, direct bone-to-implant anchorage in man. Acta Orthop Scand. 1981;52(2):155-170.
2. Lazzara RJ. Immediate implant placement into extraction sites: surgical and restorative advantages. Int J Periodontics Restorative Dent. 1989;9(5):332-43.
3. Cornelini R, Cangini F, Covani U, Wilson TG Jr. Immediate restoration of implants placed into fresh extraction sockets for single-tooth replacement: a prospective clinical study. Int J Periodontics Restorative Dent. 2005; 25(5):439-447.
4. Smith RB, Tarnow DP, Brown M, et al. Placement of immediate implants and a fixed provisional restoration to replace the four mandibular incisors. Compend Contin Educ Dent. 2009;30(7):408-418.
5. Crespi R, Cappare P, Gherlone E, Romanos GE. Immediate occlusal loading of implants placed in fresh sockets after tooth extraction. Int J Oral Maxillofac Implants. 2007;22(6):955-962.
6. Belser UC, Grutter L, Vailati F, et al. Outcome evaluation of early placed maxillary anterior single-tooth implants using objective esthetic criteria: a cross-sectional, retrospective study in 45 patients with a 2- to 4-year follow-up using pink and white esthetic scores. J Periodontol. 2009;80(1):140-151.
7. Weber HP, Morton D, Gallucci GO, et al. Consensus statements and recommended clinical procedures regarding loading protocols. Int J Oral Maxillofac Implants. 2009;24 (Suppl):180-183.
8. Brunski JB. Biomechanical factors affecting the bone-dental implant interface. Clin Mater. 1992;10(3):153-201.
9. Polack MA, Mahn DH. The aesthetic replacement of mandibular incisors using an implant-supported fixed partial denture with gingival-colored ceramics. Pract Proced Aesthet Dent. 2007;19(10):597-604.
10. Machtei EE, Frankenthal S, Blumenfeld I, et al. Dental implants for immediate fixed restoration of partially edentulous patients: a 1-year prospective pilot clinical trial in periodontally susceptible patients. J Periodontol. 2007;78(7):1188-1194.
11. Attard NJ, Zarb GA. Immediate and early implant loading protocols: a literature review of clinical studies. J Prosthet Dent. 2005;94(3):242-258.
12. Covani U, Cornelini R, Barone A. Bucco-lingual bone remodeling around implants placed into immediate extraction sockets: a case series. J Periodontol. 2003;74(2):268-273.
13. Esposito M, Grusovin MG, Achille H, et al. Interventions for replacing missing teeth: different times for loading dental implants. Cochrane Database Syst Rev. 2009 (1):CD003878.
14. Lindeboom JA, Frenken JW, Dubois L, et al. Immediate loading versus immediate provisionalization of maxillary single-tooth replacements: a prospective randomized study with BioComp implants. J Oral Maxillofac Surg. 2006;64(6):936-942.
15. Ostman PO, Hellman M, Sennerby L. Direct implant loading in the edentulous maxilla using a bone density-adapted surgical protocol and primary implant stability criteria for inclusion. Clin Implant Dent Relat Res. 2005;7(Suppl 1):S60-S69.
16. Cochran DL, Morton D, Weber HP. Consensus statements and recommended clinical procedures regarding loading protocols for endosseous dental implants. Int J Oral Maxillofac Implants. 2004;19(Suppl):109-113.
17. Ganeles J, Rosenberg MM, Holt RL, Reichman LH. Immediate loading of implants with fixed restorations in the completely edentulous mandible: report of 27 patients from a private practice. Int J Oral Maxillofac Implants. 2001;16(3):418-426.
18. Jaffin RA, Kumar A, Berman CL. Immediate loading of implants in partially and fully edentulous jaws: a series of 27 case reports. J Periodontol. 2000;71(5):833-838.
19. Romanos GE, Nentwig GH. Immediate functional loading in the maxilla using implants with platform switching: five-year results. Int J Oral Maxillofac Implants. 2009; 24(6):1106-1112.
20. Babbush CA. Histologic evaluation of human biopsies after dental augmentation with a demineralized bone matrix putty. Implant Dent. 2003;12(4):325-332.
21. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12(3):319-324.
22. Polack MA, Mahn DH. The use of a customized prefabricated zirconia abutment and zirconia crown in the restoration of an immediately provisionalized implant in the esthetic zone. Compend Contin Educ Dent. 2008;29(6):358-362.
23. Cooper LF, De Kok IJ, Rojas-Vizcaya F, et al. The immediate loading of dental implants. Compend Contin Educ Dent. 2007; 28(4):216-226.
About the Authors
Douglas H. Mahn, DDS
Private Practice
Manassas, Virginia
Mariano A. Polack, DDS, MS
Private Practice
Gainesville, Virginia