Repairing Worn Dentition with Lithium-Disilicate Glass-Ceramic
This versatile restorative material provides a predictable approach for achieving esthetics, function, and patient satisfaction.
By Andre Michel | Hannah A. Lewis, DDS
In an era of highly publicized, media-driven dentistry, patients often come to the dental office seeking the perfect “Hollywood” smile.1 Dentists must approach such procedures cautiously.1 Therefore, dentists and technicians must openly communicate with their patients and each other throughout all stages of treatment.3,4 By doing so, a higher standard of care can be provided and the best in esthetics, function, and patient satisfaction can be achieved.5
For example, diastemas, discolorations, and other characteristics of a patient’s dentition may be viewed by a dentist as defects or unesthetic.2 However, the patient may desire to keep these traits to maintain their sense of individualism.2 When proper communication between the dentist, technician, and patient is not facilitated, the defining characteristic of the patient may be lost during the restorative process,2,6 which could lead to patient dissatisfaction and possibly further restorative work.2
Material selection is also important in any restorative or smile design case and must be undertaken carefully to provide satisfactory long-term results for the patient.7 With the variety of restorative materials available to dentists and technicians today, dental professionals must be sure that the material chosen will not only withstand the masticatory forces placed upon it, but that it is indicated for use in the specific region of the oral cavity being restored.7 Although proper function is a necessity, esthetics must be considered as well because restorations in the anterior and posterior do not always require the same optical qualities.7
Lithium Disilicate
Lithium-disilicate glass-ceramic contains approximately 70% by volume needle-like crystals in a glassy matrix.8,9 This unique crystalline structure enables size, shape, and density to be controlled, allowing for greater strength and durability.8-10 With its relatively low refractive index, outstanding optical properties, such as translucency, are easily achievable and provide the optimal esthetics required for restoring anterior teeth.8-10
Currently available in two different processing techniques, lithium-disilicate glass-ceramic provides dentists a multitude of options when using it to restore their cases. Fabricated with a wax hot-press technique, pressable lithium-disilicate restorations (IPS e.max® Press, Ivoclar Vivadent, www.ivoclarvivadent.us) demonstrate a flexural strength of 400 MPa.9,11 Milled lithium-disilicate restorations (IPS e.max® CAD, Ivoclar Vivadent) can be fabricated either in the laboratory or chairside using CAD/CAM technology and demonstrate a flexural strength of 360 MPa.9,11 Although all other material properties are similar, the variation in strength between the two processing techniques is due to the size and length of the lithium-disilicate crystals. Furthermore, because of the increase in strength and the presence of the glassy matrix, lithium-disilicate restorations can be either adhesively bonded or conventionally cemented, which provides dentists even further flexibility.9,12,13
Lithium-disilicate materials exhibit high edge strength, low viscosity, and superb dimensional stability, allowing pressed restorations to be finished as thin as 0.3 mm. These qualities make lithium disilicate ideal for no-preparation and minimal preparation veneers.10,14,15 In addition to veneers and thin veneers, pressable lithium disilicate can be used as an effective treatment option to fabricate anterior three-unit bridgework up to the second premolar, anterior and posterior crowns, inlays/onlays, telescopic crowns, and implant restorations.8 For posterior crowns, lithium disilicate does not require a layering ceramic when pressed or milled to full contour because of its monolithic strength of 360 MPa to 400 MPa.
Aside from providing improved function, pressable and CAD forms of lithium disilicate also allow for characterization to make the restorations indistinguishable from the patient’s natural dentition, which is important when patients wish to maintain their own unique characterizations. Available in a variety of translucencies, high-translucency (HT) ingots are ideal for anterior esthetic cases, while ingots with more opacity are well-suited for cases involving dark teeth and core build-ups that require masking. To further enhance esthetics, dentists and technicians may also use either a cutback-and-stain or stain-and-glaze technique.8,11
Smile Design
In an ideal setting, smile design cases would call for minimal to no-preparation veneers on teeth with acceptable coloring using translucent powder-liquid porcelain or pressed glass-ceramic material to achieve an esthetic result. However, most clinical situations often involve worn, broken-down, dark teeth; old or unesthetic restorations; and/or missing teeth. In these indications, a treatment plan must be developed that incorporates a combination of different treatment modalities and materials within the same arch.
When faced with these difficult cases, dentists and technicians may benefit from using either form of lithium disilicate. With high strength, proven physical properties, ease of fabrication, versatility, and predictable results, lithium-disilicate glass-ceramics provide ideal functional and esthetic outcomes.9 The following case represents how lithium-disilicate glass-ceramic restorations (IPS e.max Press) can be used in a variety of indications to complete a full smile design case that satisfied the patient’s desire to maintain the defining characteristics—chiefly the diastemas—of his smile. Of paramount importance to this process was communication among the patient, dentist, and laboratory ceramist.
Case Presentation
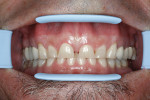
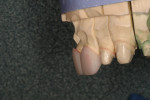
A 45-year-old man who was a musician/entertainer presented to the office with major problems of decay, broken porcelain-fused-to-metal (PFM) restorations, excessive wear, and isolated gingivitis (Figure 1). He also had a history of bruxism and acid reflux that caused secondary decay on the second molars. Upon further examination, the patient was found to have a lack of cuspid guidance, over-closed vertical dimension, uneven gingival architecture, and excessive incisal wear (Figure 2). However, the patient’s midline and gingival health were relatively acceptable.
The patient desired to restore his teeth to a more youthful appearance with a natural shade appropriate for his skin tone and that would match his unrestored lower anterior dentition. Although the patient presented with a diastema between the central incisors, he wished to keep it because he felt it was part of his professional and personal identity.
Treatment Plan
After discussions with the patient, it was decided that treatment would include laser recontouring of the gingival zeniths on teeth Nos. 7 through 10. Full-coverage maxillary posterior lithium-disilicate restorations (IPS e.max Press) would be placed on teeth Nos. 2 through 5 and 12 through 15. Additionally, full-coverage mandibular posterior lithium-disilicate restorations (IPS e.max Press) would be placed on teeth Nos. 18, 19, and 30. Lithium-disilicate veneers (IPS e.max Press) were planned for teeth Nos. 6 through 11 while maintaining the diastema between his central incisors. The treatment plan also included mandibular anterior enameloplasty, direct bonding, and whitening. Due to the lack of solid tooth structure, tooth No. 20 would not be involved in the restorative treatment, and a dental implant was planned for the future.
Clinical Protocol
Initially, diagnostic wax-up records were taken, along with clinical photographs, facebow bite records, polyvinyl siloxane (PVS) impressions, and a detailed laboratory prescription. To begin designing the case, length was added to the centrals. Coming to a compromise with the patient, spatial issues caused by the diastema were addressed and the teeth were made less triangular. After the centrals were completed, the remaining teeth were developed.
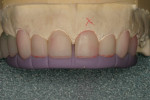
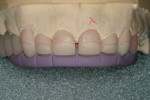
Provisional restorations were then created from the diagnostic wax-up and transferred to the preparations using a silicone putty matrix (Sil-Tech®, Ivoclar Vivadent) (Figure 3). The gingival tissues were recontoured using a soft-tissue laser with the provisional restorations in place. During the laser gingivectomy, recontouring was left incomplete on tooth No. 9 because it demonstrated biological width issues and could not tolerate further laser treatment (Figure 4).
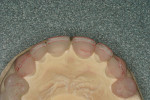
The gingival architecture was idealized with the diagnostic wax-up and transferred intraorally with temporary material and a vacuum matrix (Figure 5). Measurements were then taken with a periodontal probe. It was noted, however, that the idealized gingival contour for tooth No. 9 would impinge upon the biological width. Therefore, it was decided that the laboratory technician would correct the issue in the laboratory with a partial pontic. To create all other gingival contours, excess tissue was removed with a soft-tissue laser.
Once recontouring was complete, bite records, a facebow, clinical photographs, and a detailed shade map were submitted to the ceramist. This information was essential for fabricating restorations that would meet the patient’s expectations in terms of esthetics, particularly maintaining the natural characteristics of his dentition and matching the maxillary and mandibular anterior teeth.
Laboratory Protocol
After the ceramist received the necessary case information from the clinician, the laboratory was ready to create the final restorations from pressable lithium disilicate (IPS e.max Press). Wax was first injected through the matrix of the provisionals onto the master dies. The margins were then sealed, and form and function were developed in the wax. The completed wax-ups were then sprued, invested, burned-out, and pressed using the proper shade of pressable lithium disilicate (IPS e.max Press). The pressed restorations were then devested and placed in a dissolving liquid to eliminate the surface reaction layer. The restorations were then cut from the sprues, scrutinized against the model of the provisionals, and ready for cutback and ceramic veneering powders.
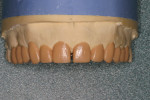
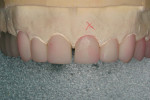
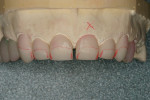
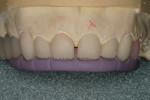
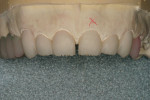
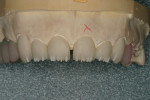
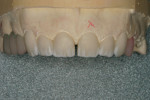
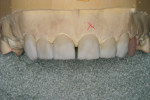
The pressings were fitted to the solid model (Figure 6). It was determined from the pressing of the restoration for tooth No. 9 and through evaluation of the clinical photographs and provisionals that gingival symmetry could be achieved with the contour of the partial pontic design (Figure 7). Once this was established, the restorations were marked with a red pencil and underwent a 0.5-mm vertical cutback (Figure 8). Additionally, the incisal edges of the restorations were marked with the red pencil and given a 0.5-mm facial taper (Figure 9 and Figure 10).
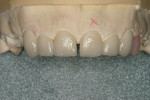
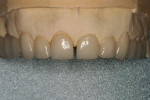
Using the red pencil once again, outlines of the material to be troughed in order to mimic natural translucency were made on the restorations (Figure 11). Using the matrix, a final cutback was then completed and the mamelon structures developed (Figure 12).
To facilitate shading and create restorations that were indistinguishable from the patient’s natural dentition, internal stain (I1, IPS e.max, Ivoclar Vivadent) was placed in the mesial and distal trough, with vanilla, silver, and orange on the middle lobes (Figure 13). MM Light (IPS e.max) was placed on the mesial and distal lobes, followed by further characterizations to the middle lobes with OE4 (IPS e.max) and Salmon (IPS e.max) (Figure 14). OE1 (IPS e.max) was then placed in the mesial and distal troughs and in between the mamelons (Figure 15).
Once the restorations were brought to full contour with TI1 (IPS e.max), they were bisque-baked and ready for final contouring (Figure 16 and Figure 17). Then, prior to delivery to the dentist for placement, the lithium-disilicate restorations were glazed and polished (Figure 18).
Final Seating
After receiving the completed restorations from the laboratory, the provisionals were removed and the teeth were polished with flour pumice. All definitive restorations were then seated with a temporary try-in paste. After margins were verified, the teeth were re-polished, treated with a desensitizing agent (Gluma® Desensitizer, Heraeus, www.heraeus.com), and prepared with multi-purpose adhesive bonding cement (Multilink® A/B, Ivoclar Vivadent). The restorations were then re-etched with a hydrofluoric acid solution and prepared with a universal primer (Monobond, Ivoclar Vivadent). After all preparation work was complete, the definitive restorations were cemented in place with self-curing luting cement (Multilink).
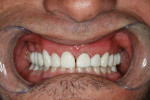
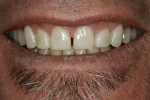
Upon final seating of the definitive restorations, the patient demonstrated a natural-appearing smile that retained his personal characteristics, specifically his diastema (Figure 19). Additionally, gingival symmetry was created, the occlusion was protected with canine guidance, his vertical dimension was increased, and the restorations were seamless (Figure 20). Overall, the patient’s expectations for lifelike characterization and shade were far exceeded by the restorative treatment.
Conclusion
When patients seek restorative dentistry, they expect to receive exactly what they desire, even if their esthetic preferences contradict conventional solutions.2 Although proper protocol must be followed at all times, including informing patients of the advantages and disadvantages of treatment or non-treatment, dentists must still take into consideration the individual goals of the patient before any restorative procedures can begin.2 When the dentist, technician, and, most importantly, the patient openly communicate through all phases of treatment, the best in function, esthetics, and standard of care can be provided in the most comprehensive and conservative manner.3-5
References
1. Ahmad I. Risk management in clinical practice. Part 5. Ethical considerations for dental enhancement procedures. Br Dent J. 2010;209(5):207-214.
2. LuBovich R Sr. Smile designing for the malcontent patient. Compend Contin Educ Dent. 2010;31(6):412-416.
3. Marzola R, Derbabian K, Donovan TE, Arcidiacono A. The science of communicating the art of esthetic dentistry. Part I: Patient-dentist-patient communication.J Esthet Dent. 2000;12(3):131-138.
4. Nanchoff-Glatt M. Clinician-patient communication to enhance health outcomes. J Dent Hyg. 2009;83(4):179.
5. Schultz C. Making standard of caring part of the standard of care. J Calif Dent Assoc. 2009;37(9):639-645.
6. Narcisi EM, Culp L. Diagnosis and treatment planning for ceramic restorations. Dent Clin North Am. 2001;45(1):127-142.
7. Spear FM. Treatment planning materials, tooth reduction, and margin placement for anterior indirect esthetic restorations. Advanced Esthetics and Interdisciplinary Dentistry. 2005;1(4):4-13.
8. McLaren EA, Phong TC. Ceramics in dentistry—Part I: classes of materials. Inside Dentistry. 2009;5(9):94-103.
9. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
10. Reynolds JA, Roberts M. Lithium-disilicate pressed veneers for diastema closure. Inside Dentistry. 2010;6(5):46-52.
11. Helvey GA. Chairside CAD/CAM. Lithium-disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-67.
12. Dudney TE. Unlock that combination. Dental Products Report. 2009;43(3):60-62.
13. Fabianelli A, Goracci C, Bertelli E, et al. A clinical trial of Empress II porcelain inlays luted to vital teeth with a dual-curing adhesive system and a self-curing resin cement. J Adhes Dent. 2006;8(6):427-431.
14. Ritter RG, Rego NA. Material considerations for using lithium disilicate as a thin veneer option. J Cosmetic Dent. 2009;25(3):111-117.
15. Lowe RA. No-prep veneers: a realistic option. Dent Today. 2010:29(5):80-86.
About the Authors
Andre Michel
Private Practice
Dana Point, California
Member, Board of Directors
American Academy of Cosmetic Dentistry
Hannah A. Lewis, DDS
Private Practice
Dana Point, California