Diastema Closure
Using orthodontics, composite bonding, or porcelain veneers for optimal esthetic results.
Also referred to as a negative space, a diastema creates a dark spot within a smile as the darkness of the back of the mouth shows. Based on modern smile design standards in the United States, closing a diastema helps to improve the appearance of a smile, and more and more patients present for a solution to the gaps in their dentition.1 Diastemas can be closed orthodontically or restoratively. Using brackets, removable appliances, or clear matrixes to move teeth, orthodontics can reposition teeth within an arch to close space.2,3 Restoration increases tooth dimension to close space while the root position remains the same, and can be completed with composite or porcelain placed interproximally to close space. Material is placed on the facial surface as well as interproximally if the tooth color or shape also requires improvement. The appropriate technique and material for a patient is based on time, psychological, physical, and financial limitations.1
Orthodontic Treatment
Orthodontics is an ideal way to close diastemas, and can be comprehensive or limited orthodontic in treatment scope. Comprehensive orthodontic treatment tries to establish a Class I relationship, proper posterior occlusion, and anterior overbite/overjet relationships, which includes space management and diastema closure.2,3 In children, interceptive orthodontic treatment is accomplished with appliances to guide the teeth during the bone growth phase and to minimize treatment with braces as well as diastema formation.4 Removal of interferences such as muscle attachments or dental pathology might be required.4 Upon completion of orthodontic treatment, appropriate retention, such as with an orthodontic retainer, is required. Retention must overcome the forces of the tongue and lips on the teeth as well as grinding forces, or diastemas can form.2,3
As people age, the occlusal surfaces of posterior teeth wear more than anterior contacts. If vertical dimension decreases from occlusal wear, the resulting force on the anterior teeth can cause either the maxillary teeth to flare or the mandibular teeth to crowd each other, resulting in diastemas. Forces on the anterior teeth are more pronounced if the posterior teeth are missing, causing flaring to occur more quickly. Proper retention minimizes or eliminates flaring or crowding.5-7
In adults, comprehensive orthodontics accomplishes diastema closure by moving teeth either laterally along the arch or lingually to make an effectively smaller arch length. The actual bone measurement stays the same, but the size measured along tooth surfaces decreases. Restoration is often required after orthodontics to correct tooth color or lost tooth structure because orthodontics only changes tooth position. If the width of the tooth is inadequate to fill an arch, restoration of the diastema is done in addition to orthodontics.2,3
Limited orthodontics is used to correct anterior tooth position when a good posterior occlusion exists. Tooth movement is accomplished with removable appliances, brackets, and archwire, or with clear matrixes.2,3 Closing diastemas requires space management such that, compared to the arch width, combined tooth width is the same. Small teeth in a large arch results in excess space. When there is too much arch space compared to total tooth width, closing a diastema results in space between other teeth. For example, when closing diastemas between six anterior teeth in an arch with excess arch space, the excess space created results in diastemas between the cuspid and first bicuspids. If this space is large enough, placement of implants or a fixed bridge fills the space. If restoration cannot be done to fill the space, it is a compromised result.8-11
Diastemas also can be closed by bringing teeth to the lingual and reducing the measured width of an arch. Teeth are measured from the distal of the upper right cuspid to the distal of the upper left cuspid. The total arch length would equal the width of each tooth plus the diastema’s measurement. When teeth are repositioned to the lingual and the diastemas are closed, the arch width is reduced to just the total widths of the teeth. Orthodontics, however, can only change tooth position, so if teeth require restoration to change color or restore lost tooth structure or the appearance of lost tooth structure, a diastema may be better closed restoratively since restorative work is already required.12,13
Some of the limitations to orthodontic treatment include psychological, physical, financial, and time factors.1-3 Psychologically, patients may not be able to deal with brackets and arch wire on their teeth. They may be concerned with the appearance, limitations to eating, or the feeling of having braces on their teeth and the effects on their lips, tongue, and cheeks. The clear matrix systems now available may help to overcome many psychological limitations; however, many patients will prefer restoration if they cannot psychologically deal with braces.
Physical limitations include tooth shape and size, tooth-to-opposing-tooth contact, arch form, arch-to-arch relationships, existing dentistry, and any dental disease such as tumors, periodontal disease, or caries.1-3 The size of an arch must be the same size as the total of all teeth when placed into an ideal position; otherwise spaces will occur. Occlusal contacts from opposing teeth limit placement of a tooth if it will hit prematurely after movement. Recontouring or repositioning opposing teeth may solve this problem. Malformed teeth, such as peg laterals, create an image of a diastema even when they are in the correct position.2,3
Financial limitations can also determine the type of, amount of, and the time frame to complete dentistry.1-3 Diastema closure is usually considered cosmetic, except with conditions such as periodontal disease, excessive wear resulting in an increase of tooth shifting, or as part of comprehensive orthodontics. Spending money for caries control, restoration, endodontics, periodontal treatment, extractions, treating oral pathology, and replacing missing teeth are usually all given priority over cosmetic dentistry.14,15 Orthodontic treatment might be too expensive for a patient to close diastemas, in which case composite bonding is more desirable.
Another factor to consider is time. Orthodontics takes months or years to complete. Patients who want instant gratification will not accept treatment with such a long duration until a final result. However, payments for orthodontic treatment can be planned over a longer period of time.
Composite Bonding
Composite bonding between teeth fills spaces and improves the appearance of diastemas.16,17 As part of a comprehensive esthetic treatment plan and part of an overall dental treatment plan, the result of diastema closure must produce a beautiful smile and fulfill the goals of overall smile design. Smile design may include changing any of thirty different defects ultimately included in tooth color, shape, and/or position.1 Bleaching is done before composite bonding to achieve color change; 10 to 14 days are allowed to pass before bonding as the bleaching material oxidizes the teeth, making bond strengths weaker.18,19 After the bleaching period, then composite can be bonded between teeth to increase the size of adjacent teeth and close a space.
The results of diastema closure must conform to the esthetic ideals of smile design.20-22 Because tooth dimension is being changed, maintaining symmetry and tooth proportion (both in terms of height to width and tooth to tooth) is challenging. Symmetry and tooth proportion (one tooth compared to the next) is easier when multiple diastemas are being closed; however, it cannot always be accomplished depending on tooth position.
Psychological limitations include apprehension about composite strength and longevity as well as final appearance. Excessive force will shear and fracture composite. It is the author’s experience that diastema closure limits exposure to direct force on the incisal edge and little fracture occurs. Composite does slightly change color with time, and leakage around the margins can occur. Touch-ups to composite are usually required every 7 to 10 years.23-25
There are several psychological advantages to composite bonding. Patients who worry that the results of diastema closure will result in teeth that look too large in comparison to the other teeth or compared to the framework of the lips and face have the option of composite being easily changed. Composite can be added or reduced to fit a patient’s desired goal. Indeed, it can be completely removed if necessary. Composite also can be placed without bonding to confirm patient acceptance. Flexibility is a very desirable feature. Patients also like that little to no tooth reduction is done and the dentistry can be completed without anesthetic.15,17,26
Physical limitations include tooth position and opposing tooth contacts. Teeth exit from the gingiva in a defined area, which cannot be changed without orthodontics. Composite cannot move roots left or right, so contours start at the mesial or distal aspect where a tooth exits the gums. Placing material subgingivally can change the appearance to look more mesial or distal by retracting the gingiva and making the dimension wider but only slightly. Consequently, tooth width and position are limited.
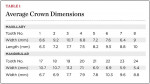
Tooth dimension height-to-width is often defined by the golden proportion, a ratio most pleasing to the eye of 1 to 1.1614, or one to one sixteenth smaller. The dimension starts with the central incisor being the largest and then each subsequent tooth posterior to it looking one sixteenth smaller. More concrete numbers for average dimensions are shown in Table 1.27 It should be noted that the position of teeth adjacent to a diastema should be in the same facial plane. A tooth that is facial to an adjacent tooth makes diastema closure with composite more difficult.
Financial limitations determine the amount of work, the materials to be used, and the time frame to complete work. A patient who can only afford to close one diastema per year would be more likely to accept composite because of its reduced cost and flexibility to do small amounts over a longer period of time. Personal time limitations are important to some patients. Composite bonding is completed in one appointment and patients like the instant results.
Porcelain
Porcelain restoration includes porcelain veneers, three-quarter crowns and full crowns.28,29 Facial tooth reduction is required to place porcelain restorations unless the tooth position is lingual to the desired result. If tooth reduction is not done, teeth look bulky and over-contoured, and improper gingival profiles can result in unhealthy gingiva. Creating proper mesial–lingual and distal–lingual contours with porcelain veneers is difficult when closing diastemas without interproximal tooth reduction. The junction where porcelain veneers extend into the mesial and distal cannot cover the lingual curvature, because rounded tooth contours create undercuts to a facial or incisal path of insertion. Interproximal reduction is often done to overcome contours that trap food or feel foreign to the tongue when reduction is not done. Some dentists fill the space with composite or cement.30
Porcelain is stronger than composite and lasts longer with no staining, but it fractures with excess force of chewing (things such as fingernails, frozen candy, etc) or grinding.31 A nightguard is required for a patient who bruxes. The esthetic results of porcelain are determined by a dentist’s and laboratory technician’s skill. A patient with high esthetic perception is not satisfied with the results of a dentist or laboratory technician with low esthetic skills. It is important to remember that an average laboratory makes an excellent dentist look average and an excellent laboratory makes an average dentist look excellent. Composite might be selected over porcelain restorations if a dentist is able to produce a better result with composite than his laboratory can with porcelain.1
The psychological, physical, and financial limitations to bonded porcelain are similar to bonded composite. Porcelain is stronger and stains less than composite; however, it costs more. Porcelain is more difficult to customize to a demanding patient. However, the results of porcelain are excellent when using an excellent laboratory. Porcelain restoration requires two or more appointments and a transition time with provisional restorations.
Case One
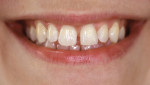
A 45-year-old man presented with a large diastema between the central incisors. The diastema was a hereditary condition seen in several members of his family. It would have been difficult to close spaces with orthodontics alone, because lingual movement is limited by contact with the mandibular incisors and there was more arch length as compared to total tooth width. The patient decided to do orthodontics to move teeth into an improved position, and then bond with composite to close the resulting diastemas (Figure 1).
Case Two
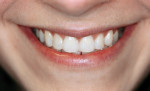
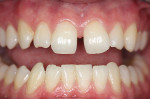
A 22-year-old woman presented with multiple diastemas. Orthodontics, composite, and porcelain bonding were discussed. The patient selected composite bonding after looking at financial constraints, concerns over reducing tooth structure, and the flexibility of esthetic results. The central incisors tipped to the distal. The lateral incisors did not match the shape and form of the central incisors. Composite bonding and esthetic recontouring on the six anterior maxillary closed the diastemas and reshaped the lateral incisors (Figure 2 and Figure 3).
Case Three
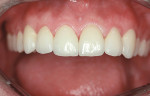
A 25-year-old man presented with a diastema between the central incisors. The central incisors tipped distally. The lateral incisors had severe wear and require restoration. Space analysis revealed small teeth and a large arch. Closing spaces with orthodontics would have resulted in diastemas in other areas. Composite restoration may have been too weak to resist fracture. Restoration of the six anterior teeth with porcelain veneers and three-quarter crowns was the preferred treatment (Figure 4 and Figure 5).
Conclusion
In summary, orthodontics or restorative dentistry presents advantages and disadvantages. Patients should be educated about each procedure and guided as to what is best for them. A summary of advantages and disadvantages for each technique is presented in Table 2. Fortunately, perception of tooth size can be changed by altering or maintaining a tooth face or silhouette of a tooth. The face of a tooth is defined as the line angles, gingival height of contour, and incisal contours. The silhouette is the gingival outline, embrasure areas, contacts, and incisal edge.32,33 Two teeth that have the same face dimensions can look the same size even if the silhouette size is different. Teeth that are larger than the contralateral tooth as a result of diastema closure can look similar in size. A dentist must replicate the face of the opposite contralateral tooth but create a more gradual curvature from the line angle into the contact area. The face is the same size but the silhouette is larger. These teeth will be perceived as the same size. Teeth that require restoration or color change might require more facial coverage in addition to adding composite into the interproximal areas.
Acknowledgment
The author would like to thank Masoud Darvish of MD Dental Studios for his excellent porcelain veneers. Copyright of the photographs printed with permission: https://www.wellesleydentist.com.
References
1. Chalifoux PR. Perception esthetics: Factors that affect smile design. J Esthet Rest Dent. 2007;8(4):189-192.
2. Tuncay OC. Orthodontics: Current Principles and Techniques. 4th ed. St. Louis, Mo: Mosby; 2005.
3. Proffit W. Contemporary Orthodontics. 4th ed. St Louis, Mo: Mosby; 2000.
4. Georgaklis CC. A six-month orthodontic solution to space closure and bite collapse. Dent Today. 2009;28(12):116.
5. Chu FC, Siu AS, Newsome PR, Wei SH. Management of median diastema. Gen Dent. 2001;49(3):282-289.
6. Yaffe A, Hochman N, Ehrlich J. A functional aspect of anterior attrition or flaring and mode of treatment. Int J Prosthodont. 1992; 5(3):284-289.
7. Mulligan TF. Diastema closure and long-term stability. J Clin Orthod. 2003; 37(10):560-574.
8. Kravitz ND. A quick and inexpensive means of treating mild lower anterior spacing. J Clin Orthod. 2006;40(3):175-176.
9. Lohmiller RM. Modified grassline technique for orthodontic space closure. Eur J Esthet Dent. 2006;1(1):30-51.
10. Bishara SE, Fehr DE. Ceramic brackets: something old, something new, a review. Semin Orthod. 1997;3(3):178-188.
11. Sinha PK, Nanda RS. Esthetic orthodontic appliances and bonding concerns for adults. Dent Clin North Am. 1997;41(1):89-109.
12. Chalifoux PR, Noxon S. Changing tooth position with orthodontics or restorative dentistry: both perspectives. Inside Dentistry. 20051(1):52-55.
13. Campbell A, Kindelan J. Maxillary midline diastema: a case report involving a combined orthodontic/maxillofacial approach. J Orthod. 2006;33(1):22-27.
14. Curtis DA, Lacy A, Chu R, et al. Treatment planning in the 21st century: What’s new? J Calif Dent Assoc. 2002;10:780-790.
15. Estafan D, Klodnitskaya L, Wolff MS. Treatment planning in esthetic dentistry requires careful listening to the patient. Gen Dent. 2008;56(3):290-292.
16. Chalifoux PR. Perception aesthetics and light-cured composites. Pract Periodontics Aesthet Dent. 1992;4(5):51-56.
17. Chalifoux PR. Comprehensive composite restoration. Inside Dentistry. 2006;2(4):56-59.
18. Chuang SF, Chen HP, Chang CH, Liu JK. Effect of fluoridated carbamide peroxide gels on enamel microtensile bond strength. Eur J Oral Sci. 2009;117(4):435-441.
19. Barbosa CM, Sasaki RT, Flório FM, Basting RT. Influence of in situ post-bleaching times on resin composite shear bond strength to enamel and dentin. Am J Dent. 2009;22(6):387-392.
20. Morley J. Smile design—specific considerations. J Calif Dent Assoc. 1997;25(9):633-637.
21. Davis NC. Smile design. Dent Clin North Am. 2007;51(2):299-318.
22. Morley J, Eubank J. Macroesthetic elements of smile design. J Am Dent Assoc. 2001; 132(1):39-45.
23. Ardu S, Braut V, Uhac I, et al. Influence of mechanical and chemical degradation on surface gloss of resin composite materials. Am J Dent. 2009;22(5):264-268.
24. Lu H, Roeder LB, Lei L, Powers JM. Effect of surface roughness on stain resistance of dental resin composites. J Esthet Rest Dent. 2005;17(2):102-109.
25. Heintze SD, Forjanic M, Ohmiti K, Rousson V. Surface deterioration of dental materials after simulated toothbrushing in relation to brushing time and load. Dent Mater. 2010;26(4):306-319.
26. Chalifoux PR. Perception esthetics: Setting treatment goals. Esthetic Dentistry Update. 1993;4(6):132-137.
27. Chalifoux PR. Checklist to aesthetic dentistry. Pract Periodontics Aesthet Dent. 1990;2(1):9-12.
28. Chalifoux PR. Porcelain veneers: Concept, preparation, temporization, laboratory, and placement. Pract Periodontics and Aesthet Dent. 1993;5(4):11-17.
29. Chalifoux PR. Anterior porcelain veneers, three-quarter crowns, and full crowns. Contemporary Esthetics and Restorative Practice. 1998;2(1):52-61.
30. Nakamura T, Nakamura T, Ohyama T, Wakabayashi K. Ceramic restorations of anterior teeth without proximal reduction: a case report. Quintessence Int. 2003;34(10):752-755.
31. Chander NG, Padmanabhan TV. Finite element stress analysis of diastema closure with ceramic laminate veneers. J Prosthodont. 2009;18(7):577-581.
32. Singer BA. Principles of esthetics. Curr Opin Cosmet Dent. 1994:6-12.
33. Singer BA. Fundamentals of esthetics. In: Aschheim KW, Dale BG. Esthetic Dentistry: A Clinical Approach to Techniques and Materials. 2nd ed. St. Louis, Mo: Mosby; 2001:5-13.
About the Author
Paul R. Chalifoux, DDS
Private Practice
Wellesley, Massachusetts