Successful Veneers
Preparation is the critical factor in a successful treatment outcome.
Shradha Sharma, BDS, DMD; Gerard Kugel, DMD, MS, PhD; Larry Hamburg, DDS
Veneers have progressed since 1928 when Dr. Charles Pincus introduced the “Hollywood Bridge” made of porcelain.1 These bridges were worn temporarily for close-ups, and removed as soon as “the shoot” was completed. Later, in 1937, he fabricated acrylic veneers to be retained by denture adhesive, which again were only cemented temporarily because there was very little adhesion.
The introduction of etching in 1959 by Buonocore2 aimed to follow a line of investigation of bonding porcelain veneers to etched enamel.3 Improvement of adhesive dentistry in the decades since has given the profession various types of restorations that avoid reduction of unnecessary tooth structure, out of which porcelain veneers have become the most commonly used restorations for improving esthetics.
Porcelain veneers have, furthermore, gained popularity among patients because of media exposure. The marketing of dental products, media-influenced treatment plans, and dentists eager to please their patients tend to ignore the risks and limitations of the procedures and materials.
Studies have shown that the survival rate of porcelain veneers ranges from 18 months to 15 years or more.4 Studies have also shown the occurrence of irreparable fracture was 7% or less,5 and 36% of veneers needed some type of repair in 10 years. The major reasons of failure were fracture, microleakage, or debonding.6
Although studies have shown a long-term survival rate, it is important to remember that a rigid veneer behaves differently when bonded to rigid surfaces like porcelain versus a surface such as dentin. The tooth–restoration interface is subjected to a great deal of stress, and composite resin cement can endure these stresses to a certain extent.7 Therefore, there are numerous reasons why such failures of porcelain veneers can occur. Nevertheless, the long-term success of porcelain veneers is possible; it depends on careful case selection and as well as accurate technique.
Case Selection
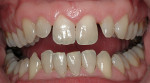
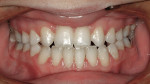
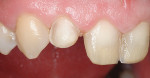
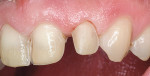
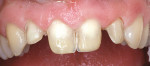
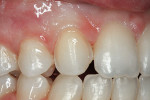
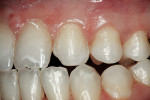
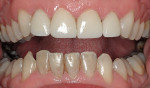
Before starting treatment planning, the patient’s expectations should be completely understood by the clinician (Figure 1 and Figure 2). A complete oral examination must be conducted to note the following conditions:
Patients with poor oral hygiene or mouth breathers should be considered for treatment with prosthetics other than veneers.
One of the most common causes of debonding or fracture is placing veneers on teeth that have insufficient tooth substrate, eg, parafunctional habits (clenching, bruxism), large composite restorations, or endodontically treated teeth with large defects.
Incisal edge position should be noted, as veneers should be avoided in cases with edge-to-edge and cross-bite occlusion.
Soft tissue and periodontal tissue examination is also important. If the patient’s smile line is very high, or the teeth are passively erupted, teeth appear short, or more than 1.5 mm to 2 mm of attached gingiva is visible, crown lengthening or osseous recontouring should be considered.8
When planning for veneers, four key elements of esthetics should be considered. Contour: Observing the shape, contour, symmetry of teeth, and buccal corridor is important in deciding the type of preparation required to achieve the golden proportion.9,10 Position: Excessive interdental spacing, unsupported porcelain, and too much labial or lingual version are also contraindications for veneers. The midline position is an important factor that is generally overlooked. Even though midline discrepancy can be corrected, a significant midline shift with restorative material can lead to compromised interproximal tissue health.11 Color: Shade is critical to the outcome of the final restoration. The shade of the teeth should be considered before preparation. If the patient has discolored teeth and changing the shade is required, whitening before teeth preparation will aid in less removal of tooth structure, and will minimize the need to block out the dark stains. Lip position: Always note the lip line because the position of the teeth plays an important role in lip support.11
While planning for veneers it is important to never ignore the rule of stabilizing the posterior occlusion before placing anterior veneers, and to eliminate any lateral and anterior–posterior excursion interference. Never plan to veneer just six anterior teeth. Literature states that 73% of American women show the mesial of the first molar, thus it is more difficult to make a smile look “natural” with six veneered teeth.12
The oral examination discussed above will aid in treatment planning the type of preparation required for the case. Visualization of the outcome is important for the patient and the clinician. The most convenient method to plan a predictable outcome is by taking impressions of both arches to make a diagnostic wax-up (Figure 3). This will help the clinician with the amount of tooth reduction required to achieve the desired results.
Veneer Preparation
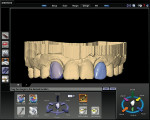
There are different types of porcelain available for fabricating veneers: feldspathic porcelain, pressable ceramics, or CAD/CAM milled veneers using lithium disilicate (Figure 4). These materials require a preparation from 0.3 mm to 0.5 mm for a thin veneer or 0.6 mm to 0.8 mm for a pressable veneer.13
Fractures of veneers have been associated with occlusal stresses and unsatisfactory treatment planning. Even though dentin adhesives have improved dramatically, porcelain bonding to enamel is better than to dentin.14 Failures occurring especially at the cervical margin are due to dentin exposure during preparation.15 However, when the initial enamel is thin and reduction is based on the existing tooth surface, it can lead to significant dentin exposures, which can be regarded as a possible cause of long-term failures.16
In the early days of veneers, no preparation was suggested in order to conserve tooth structure,17-19 whereas some clinicians believe in overpreparation to create more room for the ceramic as requested by their technicians. Neither is recommended. Unprepared enamel is a poor substrate for bonding because it is a prismatic structure that results in inferior bond strength. Additionally, no preparation can result in an overcontoured veneer and a rough marginal interface can result. And, overpreparation can result in dentin exposure that is not reliable.20,21 Hence, a veneer preparation should not be decided according to the material being used or the ideal tooth preparation, rather it should be based on the wax-up model and the use of a reduction guide.
Veneer Preparation Technique
With a 0.5-mm diamond depth-cut bur, scribe horizontal depth-cut grooves on the labial surface of an anterior tooth. Extend these grooves from mesial to distal, taking care not to damage the adjacent teeth that are not being prepared. It may be necessary to angle the bur in relation to the contour of the labial surface to achieve the appropriate depth for these guide cuts. The finish line of the preparation will end gingivally or supragingivally. Ideal preparations should end at the gingival crest, to preserve the gingiva at its current height while hiding the margin of the veneer, if possible. Do not place the gingival depth cut into the cemento-enamel junction (CEJ) area.
Always examine study models before preparation to avoid over-reducing the area of the tooth that may be rotated lingually. The use of reduction guides is recommended. Using a tapered diamond, reduce the remaining labial tooth structure between the depth cuts. Simultaneously create a chamfer ending 0.5 mm incisal to the CEJ. Labial reduction should also extend interproximally. Interproximal contact should be preserved especially if the teeth are in contact. Apical to the contact area, the preparation extends toward the lingual, resulting in an elbow apical to the contact.22 The interproximal margin then continues incisally around the height of contour and then back toward the incisal–lingual. This will conceal the gingival interproximal margin after delivery.
Another type of interproximal margin is the wraparound type, where the margin is extended beyond the contact area. The finish line is placed at right angles to the palatal surface (Figure 5 and Figure 6).This type of design is used for diastema closure and peg-lateral preparation.22
Incisal Edge Preparation
For an incisal butt-joint preparation, prepare 0.5-mm depth-cut grooves in the incisal edge. Using the diamond bur, remove the remaining incisal tooth structure. Then round the facial incisal line angle, leaving a butt-joint margin along the lingual incisal edge. The incisal reduction should be 0.5 mm to 1 mm (Figure 7).
Incisal Chamfer Preparation
The incisal edge is not reduced in length. This type of preparation is occasionally done on canines to preserve the natural guiding palatal surface of the tooth, which is important for function. Add additional space for the incisal porcelain by creating a chamfer along the facial incisal margin using the tip of the tapered diamond.
Incisal Lingual Wrap Preparation
Prepare 0.5-mm depth cuts in the incisal surface of tooth. Reduce the incisal surface in a manner similar to the incisal butt-joint preparation. Reduce the mesial–incisal and the distal–incisal corners an additional 0.5 mm. Then, using the tapered bur, extend the incisal chamfer to the palatal surface. This palatal chamfer should be a straight line mesial to distal. All incisal edges should be rounded. The lingual chamfer line on the wraparound preparation should be above or under the centric lingual contacts to avoid occlusal contact on the interface between the porcelain and the tooth structure (Figure 8 and Figure 9).
The incisal wrap preparation and the incisal butt-joint preparations are popular options for several reasons. The incisal–lingual wrap preparation is done to increase the length of the tooth. The length can be increased from 0.5 mm to 2 mm only. It is also recommended if buccal–lingual repositioning is in order. The lingual wrap can be used in most patients, easily fabricated by the technician, and easily handled by the dentist due to positive seating on delivery.23 However, no relation was seen between survival and incisal butt-joint versus incisal overlap preparation. The path of insertion for veneers is in the labial or incisal–labial direction. Hence, it is critical that all undercuts in relation to this path must be removed or else there is probability of fracture of the veneer.
A reduction guide is a helpful aid that is created from the traditional wax-up. It is designed to allow evaluation of the preparation at the incisal, middle third, and cervical third of the tooth. Reduction guides are particularly important when teeth are misaligned. This also aids in a conservative tooth preparation.
Temporization
Making use of a silicone putty impression material shell to fabricate temporaries reproduces the wax-up or study models very accurately. During the period a patient is in temporary veneers, there is a likelihood of postoperative sensitivity. Therefore, application of a desensitizer is recommended before fabricating the temporaries.
After finishing and polishing, the patient’s feedback and approval helps in communicating with the laboratory. An alginate impression can also be taken as a reference for the technician. Maintenance of periodontal health for the duration of the temporaries can be done by irrigating the marginal area with a chlorhexidine rinse using an irrigating syringe. Use of the irrigating syringe will decrease staining due to chlorhexidine.
Conclusion
Porcelain veneers have been a part of the dentist’s armamentarium for almost 25 years. Research has shown that the failure rate was high when veneers were placed by inexperienced operators and over existing restorations. Bonding to enamel rather than dentin or existing restorations gives the strongest bond and avoids microleakage or debonding. Hence, tooth preparation is one of the important steps in this procedure.
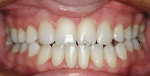
These failures can be easily overcome when the clinician can create an appropriate treatment plan. The treatment plan should include a comprehensive oral examination. The final desired restoration should be compared to the current tooth position, color, and shape using a wax-up. This would aid in a suitable preparation design and, therefore, will give a reproducible clinical technique for successful long-term veneer restorations (Figure 10).
References
1. Pincus CR. Building mouth personality. J South Calif Dent Assoc. 1938;14:125-129.
2. Horn RH. Porcelain laminate veneers bonded to etched enamel. Dent Clin North Am. 1983; 27(4):671-684.
3. Calamia JR. Etched porcelain veneers: the current state of art. Quintessence Int. 1985;16(1):5-12.
4. Zarone F, Apicella D, Sorrentino R, et al. Influence of tooth preparation design on the stress distribution in maxillary central incisors restored by means of alumina porcelain veneers: A 3D-finite element analysis. Dent Mater. 2005;21(12):1178-1188.
5. Sadowsky SJ. An overview of treatment considerations for esthetic restorations: A review of the literature. J Prosthet Dent. 2006;96(6):433-442.
6. Dumfahrt H, Schäffer H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service: Part II—Clinical results. Int J Prosthodont. 2000;13(1):9-18.
7. Gürel G. Porcelain laminate veneers: minimal preparation by design. Dent Clin N America. 2007;51(2):419-431.
8. Wakefield C. Porcelain veneers—preliminary procedures before preparation. Texas Dental Journal. 2006;123(10):940-945.
9. Preston JD. The golden proportion revisited. J Esthet Dent. 1993;5(6):247-251.
10. Javaheri D. Considerations for planning esthetic treatment with veneers involving no or minimal preparation. J Am Dent Assoc. 2007;138(3):331-337.
11. Ward DH. Proportional smile design using the recurring esthetic dental (red) proportion. Dent Clin North Am. 2001;45(1):143-154.
12. Garber D. Porcelain laminate veneers: ten years later. Part I: Tooth preparation. J Esthet Dent. 1993;5(2):56-62.
13. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
14. Van Meerbeek B, Perdigão J, Lambrechts P, et al. The clinical performance of adhesives. J Dent. 1998;26(1):1-20.
15. Smales RJ, Etemadi S. Long-term survival of porcelain laminate veneers using two preparation designs: a retrospective study. Int J Prosthodont. 2004;17(3):323-326.
16. Magne P. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Rest Dent. 2004;16:7-18.
17. Horn RH. Porcelain laminate veneers bonded to etched enamel. Dent Clin North Am. 1983;27(4):671-684.
18. Calamia JR. Etched porcelain veneers: the current state of art. Quintessence Int. 1985;16(1):5-12.
19. Friedman MJ. Current state-of-the-art porcelain veneers. Curr Opin Cosmet Dent. 1993:28-33.
20. Layton D, Walton T. An up to 16-year prospective study of 304 porcelain veneers. Int J Prosthodont. 2007;20(4):389-396.
21. Friedman MJ. Ask the experts. Porcelain veneers. J Esthet Rest Dent. 2001;13(2):86-87.
22. Priest G. Proximal margin modifications for all-ceramic veneers. Pract Proced Aesthet Dent. 2004;16(4):265-272.
23. Peumans M, Van Meerbeek B, Lambrechts P, Vanherle G. Porcelain veneers: A review of the literature. J Dent. 2000;28(3):163-177.
About the Authors
Shradha Sharma, BDS, DMD
Assistant Professor
Tufts University School of Dental Medicine
Boston, Massachusetts
Gerard Kugel, DMD, MS, PhD
Associate Dean for Research
Tufts University School of Dental Medicine
Boston, Massachusetts
Larry Hamburg, DDS
Private Practice
Poughkeepsie, New York