Indirect CAD/CAM Porcelain Restoration Cementation Simplified
Christopher Pescatore, DMD
Longevity, sensitivity, and technique-related issues must be taken into consideration for predictable results.
Today’s current economic environment has caused the restructuring and rethinking of virtually every business in operation. This includes the healthcare professions, especially dentistry. Patients today are looking for faster solutions to minimize time away from work and family. Luckily, revolutionary changes in products and the techniques in which they are used are allowing dental professionals to provide more efficient dental care and, at the same time, satisfy the esthetic concerns and time constraints of their patients. This article will focus on using a more simplistic tissue management system, adhesive cementation protocol, and a chairside in-office CAD/CAM restorative system, providing the ultimate in predictability and customization.
One of dentistry’s main growth areas has been in esthetic indirect restoratives.1 This has heightened the attention on adhesive systems and permanent resin cements, specifically total-etch products, because of their consistent and longer track record, good bond strength, and improved esthetics.2 The traditional total-etch adhesive protocol features a disinfectant prior to etching, an etching gel for the enamel and dentin, and wetting agent, all followed by the primer and adhesive application.3 The resin cement is then applied to the internal aspect of the indirect restorative (and possibly the preparation). The restoration is inserted, any excess cement is cleaned, and the final cure of the restoration is accomplished before finishing and polishing.
Preparation
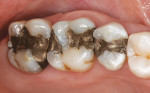
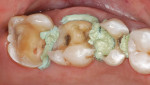
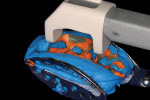
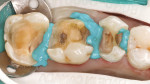
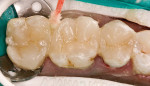
A 40-year-old woman presented with silver amalgam fillings that required replacement because of recurrent decay and compromised margins (Figure 1). The teeth to be replaced were the upper left second bicuspid and first and second molars. It was decided that these new restorations would be fabricated in-office with the chairside CAD/CAM restorative system E4D Dentist® (D4D Technologies, https://www.d4dtech.com). The existing restorations were removed and the presence of decay was verified with both a caries detector as well as a spoon excavator. All decay was removed from the teeth and the preparations were finished, keeping in mind the proper inlay/onlay preparation guidelines and requirements.4 Before scanning the preparations for restoration design, soft-tissue management was obtained with a soft-tissue diode laser and a putty-type retraction system (Expasyl™, Kerr Corporation, https://www.kerrdental.com) (Figure 2). A putty retraction system was specifically chosen over a traditional retraction cord or other hemostatic agent because of their potential for tissue (epithelial attachment) damage and recession.5-7 After 2 minutes, the putty retraction material was thoroughly rinsed away with air/water spray and dried (Figure 3). Because of the ease of impression scanning on multiple-quadrant restorations with E4D Dentist, a polyvinyl siloxane impression using a heavy-body/wash material (Take 1® Advanced™, Kerr Corporation) was made. A dual-arch tray was used to capture the detailed impression for scanning (Figure 4).
Restoration Fabrication
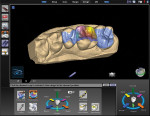
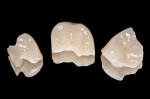
As an in-office CAD/CAM restorative system, E4D Dentist possesses the unique feature of being able to scan an impression (Figure 5) and then create a 3D model for restorative fabrication. This is especially helpful for patients who have a hard time staying open or for more difficult areas in the posterior regions of the mouth. This increases the appointment time by only several minutes at most, while at the same time minimizing clinician frustration and patient discomfort. After the optical images of the impression were accomplished, the restorations were then fabricated using the E4D Dentist library of teeth (Figure 6). After the restorations were milled, they were then tried in to verify fit and contact strength. These factors being acceptable, the restorations were then stained and glazed and placed in a porcelain oven to maximize the esthetic properties, inherent strength, and fracture resistance of the porcelain blocks (Figure 7).8
The internal aspect of the all-porcelain restorations was then steam cleaned before being tried in again to verify fit, contacts, and esthetics. Seeing that the desired results were obtained, the restorations were removed and readied for insertion. A 9.5% hydrofluoric acid gel was applied for 1 minute, rinsed with water for approximately 20 seconds, and dried thoroughly. A silanating agent was then applied and air-dried. An unfilled resin was applied to the internal aspect of the restoration at this time and placed in a light-protective container, ready for insertion.
Insertion
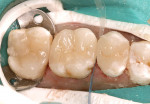
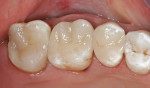
An isolation device was applied using a rubber dam. Tissue management was then obtained by applying a hemostatic agent (Hemostasyl™, Kerr Corporation) (Figure 8). After 2 minutes, the hemostatic material was thoroughly rinsed away with air/water spray and dried. The teeth were then re-cleaned with 2% chlorhexidine, rinsed, and dried, but not to the point of dessication.9 A phosphoric-acid etchant was then applied to the enamel first and then dentin using the standard time protocol of 15 seconds on enamel, 10 seconds on dentin.10 Thorough rinsing was then accomplished for 20 seconds. A wetting agent (Gluma® Desensitizer, Heraeus Kulzer, https://www.heraeus-kulzer-us.com) was applied to the teeth and then lightly dried with a contamination-free air dryer. Once the tooth surface had achieved a moist (matte) finish, the adhesive (OptiBond® Solo Plus, Kerr Corporation) was applied for 20 seconds to each preparation, and again a contamination-free air dryer was used to evaporate the solvent. The restorations were then removed from the light-protected container and the resin cement (NX3 Nexus® Third Generation, Kerr Corporation) was applied to the internal aspect generously, and inserted one by one. To avoid movement while cleaning the resin cement interproximally, the restorations were tacked down with a 4-mm turbo tip in the Demi™ LED Light Curing System (Kerr Corporation). Interproximal cleaning was then accomplished with waxed floss and microbrushes (Figure 9). Final curing was then performed both buccally and lingually with two LED lights simultaneously for 20 seconds, followed by occlusal curing for 20 seconds. Marginal and occlusal finishing was performed with super-fine diamond burs. Interproximal finishing involved using medium and then fine composite finishing strips (Figure 10). Occlusion was then checked and slight adjustments were performed before final finishing and polishing of the restorations with porcelain polishing points. The final results exhibited natural beauty and esthetics while at the same time conserved as much tooth structure as possible (Figure 11).
Conclusion
Because of the high esthetic demands of our patients, dentists are performing more and more tooth-colored procedures than ever before, especially bonded porcelain restorations.11 Therefore, it behooves clinicians to educate themselves about the latest improvements in dental products and technologies so that patients receive the most advanced and effective form of treatment. In cases using newer tissue management materials, in-office CAD/CAM systems, traditional adhesive protocols, and newer resin cements, the dentist has the ability to place a highly esthetic porcelain (or resin) restoration with very predictable results, not only when it comes to longevity but also with regard to lack of sensitivity and other technique-related issues.
Disclosure
The author has received an honorarium from Kerr Corporation.
References
1. Christensen GJ. Considering tooth-colored inlays and onlays versus crowns. J Am Dent Assoc. 2007;139(5):617-620.
2. Miller MB. Dental adhesives. In: Miller MB, ed. REALITY: The Information Source for Esthetic Dentistry. 20th ed. REALITY Publishing Co: 2006;197-236.
3. Freedman G. Bonding systems. Dentistry Today. 1996;15:68-75.
4. Della Bona A, Kelly JR, Wang WC, et al. The clinical success of all-ceramic restorations. Eur J Prosthodont Restor Dent. 2007;15(4):183-189.
5. Azzi R, Tsao TF, Carranza FA Jr, et al: Comparative study of gingival retraction methods. J Prosthet Dent. 1983;50(4):561-565.
6. Donovan TE, Gendara BK, Nemetz H. Review and survey of medicaments used with gingival retraction cords. J Prosthet Dent. 1985;53(4):525-531.
7. Shaw DH, Krejci RF, Kalkward KL, et al. Gingival response to retraction by ferric sulfate (Astringedent). Oper Dent. 1983;8(4): 142-147.
8. Chen HY, Hickel R, Setcos JC, et al. Effects of surface finish and fatigue testing on the fracture strength of CAD/CAM and pressed ceramic crowns. J Prosthet Dent. 1999;82: 468-475.
9. Gwinnett AJ. Effect of cavity disinfection on bond strength to dentin. J Esthet Dent. 1992;4(Suppl):11-13.
10. Lopes GC, Thys DG, Klaus P, et al. Enamel acid etching: review. Compendium. 2007;28 (1):18-25.
11. Leinfelder KF. Indirect posterior restorations. Compendium. 2005;26(7):495-503.
About the Author
Christopher Pescatore, DMD
Private Practice
Danville, California