Minimal Preparation Porcelain Veneers
Using the intraoral composite mock-up to treat orthodontic relapse.
Over the past two decades, porcelain veneers have evolved into the restoration of choice for anterior teeth because they provide the ability to change the shape, color, size, and angulation of teeth with conservative preparation. The development of greater bond strengths to tooth structure and porcelain, combined with increased fracture resistance as well as improved marginal adaptation of ceramic materials, has proven the porcelain veneer to be a durable and esthetic restoration. The porcelain veneer continues to evolve. This evolution has led to the current and popular use of minimal- and no-preparation veneers.
Proper patient identification and case selection is critical in obtaining a natural result when treating the dentition with minimal-preparation veneers. Patients have long welcomed this concept of a long-lasting, minimally invasive procedure that favors the preservation of enamel. It cannot be overemphasized that case selection is critical in the application of this technique. If a patient is already naturally protrusive or has a bulky dentition, a no-preparation or minimal-preparation may have undesirable results. The ideal scenario is when a minimal change in shade is required and the teeth are in slight lingual version. In this particular case, the patient had adolescent orthodontic treatment with premolar extractions, which resulted in a less than ideal lingually inclined arch form. In addition, the orthodontic relapse resulted in a drifting of the dentition that directly affected the esthetics of the smile. Because orthodontic relapse is a common phenomenon, there are countless dentitions that can benefit from the minimal- or no-preparation veneers when treated in combination with shade change and incisal edge restoration.
Patient History
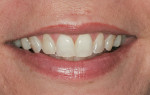
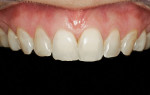
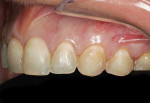
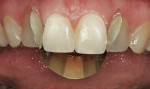
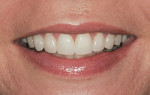
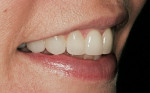
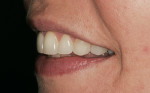
The patient was a healthy 39-year-old woman. Poor alignment and discolored and worn teeth were her chief complaints. The patient wanted a fuller, more attractive smile. The patient’s heightened awareness of her dental appearance led her to the author’s practice in search of a conservative smile makeover. She displayed a unique dental esthetics awareness not typically seen in a patient. This acuity was exemplified by her dissatisfaction with the wear and angulations present in her current smile. She did not wish to proceed with orthodontic treatment to the correct the relapse that had taken place (Figure 1).1
Clinical Data
Clinical examination revealed no periodontal disease. An oral cancer screening and soft tissue examination revealed no significant findings. Oral hygiene was reviewed and recommendations for improvement were made. A full series of radiographs revealed normal bone levels with no periapical pathology present. The occlusion was a bilateral Class 1 molar relationship with no temporomandibular disorder. History of adolescent orthodontic treatment with premolar extractions was revealed and noted. In lateral excursions, canine rise was present. In protrusion, the maxillary central incisors provided the anterior guidance. Posterior disclusion existed in both lateral and protrusive movements. After many years, some orthodontic relapse had occurred.
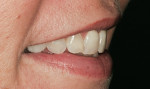
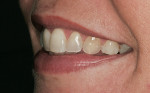
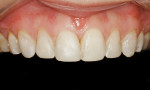
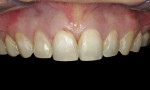
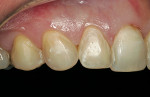
Careful analysis revealed incisal wear on teeth Nos. 7 through 10. The right maxillary central incisor was in a slight lingual version secondary to orthodontic relapse. In general, teeth Nos. 4, 6 through 11, and 13 revealed a negative axial inclination (Figure 2 and Figur 3). In addition, the shade of the maxillary central incisors was D2.2
Diagnosis
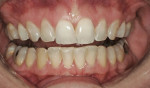
The patient presented with a smile that showed signs of normal wear and orthodontic relapse. Because the general shade was D2 and the dentition displayed lingualized axial inclinations, this case was ideal for minimal-preparation porcelain veneers. After lengthy discussion with the patient, she concluded that she wanted fuller and more youthful and balanced smile (Figure 4).3,4
Treatment Plan
Before commencing treatment, digital photographs were taken and diagnostic study casts were fabricated from alginate impressions. A preliminary intraoral composite mock-up using Venus® Diamond and Venus® Flow (Heraeus, https://www.heraeus-dental-us.com) was sculpted to create the smile design.5,6 After viewing and discussing the subtle but important elements of the composite mock-up, it was decided that the treatment plan would consist of the following:
- Prophylaxis and oral hygiene instruction
- Maxillary and mandibular tray whitening using Venus® White 16% (Heraeus)
- Eight minimal-preparation porcelain veneers on the maxillary incisors, canines, and second premolars (the first premolars were not present) using Venus® Porcelain (Heraeus)
Orthodontic referral was offered to this patient. Although an orthodontic appliance for treatment of relapse could have been used, this would not restore the incisal edge wear present nor alter the shade of the teeth.1,7 The patient preferred not to exercise this treatment option and was interested in a more immediate result.
Preparation
Alginate impressions taken at the diagnostic appointment were used to fabricate study models for analysis by both the doctor and patient.8,9 Tray whitening was performed prior to the restorative treatment, lightening the shade of the teeth from D2 to A1. Because minimal-preparation veneers are in the range of thickness of 0.5 mm, whitening the underlying tooth structure would benefit the final result.
On the day of impressioning, an intraoral composite mock-up (Figure 5 and Figure 6) was performed.10,11 After being approved by the patient, photographs and an alginate impression of this mock-up were taken. The actual composite mock-up veneers were preserved and sent to the ceramist as a guide.12-13
Local anesthetic was administered only on teeth Nos. 4, 6, 11, and 13 because of cervical sensitivity. A minimal-veneer preparation was performed beginning with the central incisors with a Brasseler 8856 Fine Round End Taper 30 micron bur (Brasseler USA, https://www.brasselerusa.com). This bur was used at the cervical area to provide a finishing line for the laboratory technician to create space for a smooth gingival emergence profile. The incisal preparation involved simply smoothing any rough edges and was not extended onto the lingual. The facial margins were placed approximately 0.5 mm into the gingival sulcus. The interproximal facial embrasures were deepened to accommodate the veneer contact point. Contacts were left untouched. Incisal edges were rolled and smoothed with the diamond bur and then with a medium Soft-Lex™ disc (3M ESPE, https://www.3mespe.com). This disc was also used to prepare all facial-treated surfaces and to smooth all sharp line angles.
The prepared teeth (Figure 7, Figure 8, Figure 9) were cleansed thoroughly with water and the SIROlaser 980 nm diode laser (Sirona Dental Systems, https://www.sirona.com) was used for sulcus retraction and subtle recontouring of tooth No. 8 at the zenith of the gingival tissue. The final impression was made with Flexitime® Xtreme Correct Flow and Heavy Tray impression material (Heraeus). No provisionals were placed. An application of Gluma® Desensitizer (Heraeus) was applied to all prepared teeth to reduce postoperative sensitivity.
Laboratory Instructions
Communication of every desired feature must be conveyed to the ceramist.13 The ceramist was given highly detailed information regarding the smile design, including photographs, preoperative models, a composite mock-up model, a model of the mock-up composite veneers, and the actual veneers. Surface texture, translucency, and internal anatomy were all determined in collaboration with the patient and communicated to the ceramist.14 The color map of the new and stump shade was also submitted to the laboratory. This detailed information allowed the ceramist to clearly understand the exact characteristics that were desired in this case. The decision to use Venus® Porcelain (Heraeus) was based on the fact that its opaques, with their high chroma and fluorescence, would provide rich color in a thin layer. Since Venus Porcelain is 100% synthetic quartz glass, no impurities exist. This is an important factor when fabricating a 0.5-mm ceramic veneer, where any defects would be readily obvious. Using the system’s modifiers and incisal porcelains, the desired incisal effects could be created.
Insertion and Finishing
After the laboratory returned the porcelain veneers, they were placed onto the master model and the marginal integrity was evaluated. Inspection of the internal aspect of each veneer was also performed. Note that handling a 0.5-mm porcelain veneer requires great care to prevent breakage.
Local anesthesia was again administered in the premolar areas. The veneers were placed onto the prepared teeth for evaluation. Marginal fit on the prepared teeth was then evaluated. The veneers were then carefully replaced with NX3 Nexus® try-in paste (Kerr Corporation, https://www.kerrdental.com) to determine the shade of cement to be used. Note that the translucent nature of an ultra-thin veneer allows for minimal modulation of shade with the luting agent. The patient viewed her new smile at this try-in stage and was very pleased. There were no surprises at the insertion visit, as every detail of the design had been clearly articulated and conveyed to the patient in the previous visit. She immediately gave approval for final cementation.
This author prefers to initiate veneer placement using the central incisors as a starting point. This ensures that perfect symmetry and balance is achieved because placement of multiple veneers may require contact adjustment, and these adjustments, by default, will occur on the more posterior veneers, which are less cosmetically sensitive to width discrepancies. After the central incisor veneers were placed, then the subsequent left and right side veneers were placed using the same technique.
At the start of the insertion of the central incisors, a Spandex lip retractor was inserted. The maxillary central incisors were mechanically etched with the MicroEtcher IIA (Danville, https://www.danvillematerials.com) and then acid-etched with Ultra-Etch® 35% phosphoric acid (Ultradent Products, https://www.ultradent.com) for 15 seconds and rinsed thoroughly. The use of mechanical etching is very effective in providing a meticulously clean surface before acid-etching and bonding.
The internal aspect of Nos. 8 and 9 veneers were prepared by micro-etching with 50-µm aluminum oxide particles for approximately 20 seconds, rinsing with water, acid-etching with 35% phosphoric acid, rinsing with water, and thoroughly drying. A silane primer coupling agent was applied for 1 minute and then a bonding agent, Gluma® Comfort Bond (Heraeus) was placed, thinned, and dried. The veneers were then set aside in a light-shielded box.
Then both centrals were isolated with a conventional stainless steel matrix before micro-etching with 50-µm aluminum oxide particles for approximately 20 seconds (Figure 10). Etching with 35% phosphoric acid was then performed. Again, micro-etching ensures that the enamel surface is meticulously cleaned before acid-etching. When the acid-etching is complete, placement of the bonding agent was preformed using Gluma Comfort Bond. This was thinned and dried thoroughly. NX3 Nexus resin cement clear base was gently placed into each veneer and the veneers were carefully seated into position. Because of the fragile nature of an extremely thin veneer, great care must be taken when handling and seating them. Gentle pressure was used to seat each veneer, giving ample time for excess luting agent to be expressed peripherally.
When seated fully, each veneer was tack-cured for 3 seconds using a 2-mm curing tip at the gingival margin, staying away from the interproximal. This tack-curing was then performed on the incisal edge in a similar fashion. Flossing was then performed, dragging through facial to lingual to remove excess luting agent as well as ensuring a clean contact. Final curing was performed with the Translux® Power Blue® LED curing light (Heraeus) for 60 seconds facially (gingival and mid-body), incisally, and at all interproximals. Because the luting agent or composite in general cannot be over-cured and under-curing allows for inferior physical properties of the material, one must err on the side of safety.
Residual cured cement was trimmed with a periodontal scaler and the Brasseler ET diamond bur was used to reduce lingual excess. Occlusion was preliminarily adjusted at this time. Interproximals were finished with Brasseler interproximal strips.
The occlusion was evaluated and adjusted in centric occlusion and in lateral and protrusive excursions. Final polishing was accomplished using the Brasseler Dialite porcelain polishing kit of cups and points. The Porcelize Kit™ (Cosmedent, https://www.cosmedent.com), with its 3-µm and 1-µm polishing pastes, was used to obtain the final luster (Figure 11, Figure 12, Figure 13).
Conclusion
Traditionally, composite has been the preferred treatment modality when thin restorative veneering was needed. But today, with the introduction of minimal-preparation veneers, a longer-lasting and more durable result can be provided. Ceramic offers a virtually stain-free surface, permanent high luster and polish, and superior incisal edge strength, which is far greater than the microhybrid composite of today.5 Fabrication of a veneer, which involves a laboratory procedure, offers more control than composite because the ceramist has several days to fabricate veneers.
Because there is no need to fabricate temporary veneers, patient chairtime is reduced. But the disadvantage of not giving the patient the opportunity to test drive their new smile in the temporary stage makes performing the intraoral composite mock-up even more critical. This composite mock-up becomes the primary tool allowing for direct communication between the patient, dentist, and ceramist.13 The guesswork and the unknown is eliminated and every detail of the design is in the hands of all three parties so that, in the end, the patient is best served. The selection of Venus Porcelain, a pure synthetic quartz glass with unique physical properties, was ideal for this thin veneer application.
Ultimately, outstanding results were achieved through effective and detailed communication with the patient and laboratory ceramist.11,13 By listening carefully and attentively, it was possible to accurately identify this patient’s expectations. When the author encountered this patient outside of his office, she expressed great satisfaction, and he observed a more radiant person behind a youthful smile.
Disclosure
The author has received honoraria from Heraeus Kulzer.
References
1. Kim J, Chu S, Gurel G, Cisneros G. Restorative space management: Treatment planning and clinical considerations for insufficient space. Pract Proced Aesthet Dent. 2005;17(1):19-25.
2. Magne P, Belser U. Natural oral esthetics. In: Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, Ill: Quintessence Publishing; 2002:57-98.
3. Ricketts RM. Divine proportion. In: Goldstein RE. Esthetics in Dentistry. 2nd ed. Hamilton, Ontario: BC Decker; 1998:187-206.
4. Goldstein RE. Composite resin bonding. In: Goldstein RE. Esthetics in Dentistry. 2nd ed. Hamilton, Ontario: BC Decker; 1998:277-338.
5. Terry DA. Contemporary composite resins. In: Terry DA. Natural Aesthetics with Composite Resin. Mahwah, NJ: Montage Media Corporation; 2004:20-37.
6. Cosmetic mockups. In: Reality. 15th ed. Houston, Texas: Reality Publishing Co; 2001: 429-432.
7. Chiche G, Pinault A. Esthetics of Anterior Fixed Restorations. Carol Stream, Ill: Quintessence Publishing; 1990.
8. Touati B. Defining form and function. Pract Periodont Aesthet Dent. 1998;10(7):800-807.
9. Lombardi RE. The principles of visual perception and their clinical application to denture esthetics. J Prosthet Dent. 1973;29:358-382.
10. Levin EI. Dental esthetics and the golden proportions. J Prosthet Dent. 1978;40:244-252.
11. Marus RD. Treatment planning and smile design using composite resin. Pract Periodont Aesthet Dent. 2006;18(4):235-241.
12. Feigenbaum NL. Aspects of aesthetic smile design. Pract Periodont Aesthet Dent. 1991;3(3):9-13.
13. Kesseler JC. Dentist and laboratory: Communication for success. J Am Dent Assoc. 1987;(Spec No):97E-102E.
14. Adolfi D. Surface texture and superficial gloss. In: Adolfi D. Natural Esthetics. Carol Stream, Ill: Quintessence Publishing; 2002:55-72.
About the Author(s)
Robert D. Marus, DDS, AAACD
Private Practice
Yardley, Pennsylvania