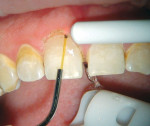
Laser Soft Tissue Crown Lengthening
By any other name, it is still the same.
Confusing and often misleading technology is used by both clinicians and salespeople to describe laser dentistry; the term “soft-tissue crown lengthening” is one of the most common. According to the ADA’s Current Dental Terminology 2009-2010 (CDT 2009-10), the procedure does not exist.1 However, this does not negate the need to perform a procedure to correct soft-tissue asymmetry, or to establish the proper clinical crown length, or crown-to-root ratio, or a healthier and more esthetic gingival contour.
The CDT 2009-10 does list the procedure “D4249 clinical crown lengthening—hard tissue.”1 This is a periodontal procedure in which gingival and osseous tissue is removed in order to expose more clinical tooth structure. As the terminology implies, for appropriate reimbursement, some osseous recontouring or removal must be performed as part of the treatment. It requires reflection of a flap and is performed in a healthy periodontal environment.2 This code is appropriate where the preparation of a restoration violates the biologic width of the periodontal attachment apparatus, or where there is less than 3 mm of tooth structure remaining between the alveolar crest and the restorative margin as noted by radiographic review or bone sounding.3 Because of this code’s requirement of an osteotomy or an osteoplasty, it would be inappropriate to use it for a strictly soft-tissue procedure.
Code “D4211—Gingivectomy or gingivoplasty—one to three contiguous teeth or bounded teeth spaces per quadrant”4 is a soft-tissue procedure. By definition it involves the excision of the soft-tissue wall of the periodontal pocket and is performed to eliminate suprabony pockets after adequate initial preparation, to allow access for restorative dentistry in the presence of suprabony pockets, or to restore normal architecture when gingival enlargements or asymmetrical or unesthetic topography is evident with normal bony configuration.5 Gingivectomy may be the appropriate code to use for the “soft-tissue crown-lengthening” procedure, as it is strictly a soft-tissue procedure.
However, there may be specific plan restrictions that exclude coverage in some situations. These exclusions vary and may include but are not limited to: other procedures performed on the same tooth on the same date, optional treatment performed for cosmetic (esthetic) purposes, or to correct congenital or developmental defects and gingival pocketing of less than 5 mm.
When submitting any periodontal procedure for third party (insurance) reimbursement, all practices need to follow the ANSI/ADA Specification No. 1047—Standard Content of an Electronic Periodontal Attachment, which was adopted by the ADA in 2006. It was developed to standardize the uniform content requirements for the documentation to be included in a periodontal attachment to the original claim form to enable claims adjudication for various periodontal procedures.
A clinician should never determine a patient’s treatment needs based on their third-party coverage. However, both the patient and the clinician need to set realistic goals, treatment objectives, and expectations that are financially realistic and acceptable to the patient.
With all that being said on procedural terminology, clinicians should always consider the benefits and techniques of a laser-assisted, soft-tissue crown-lengthening procedure. The goal of this procedure is to create gingival contours and anatomy that is healthy, maintainable, and esthetically pleasing. This enables the creation of the proper symmetry, clinical crown-to-root ratio, and incisal–cervical to mesial–distal ratios in the dentition.
The proper use of a dental laser can simplify the procedure for both the patient and the clinician with very predictable outcomes. Almost any wavelength of surgical lasers can be used for this procedure with slightly differing degrees of ease and success. The precise control over the tissue interaction that lasers provide minimizes, if not eliminates, any postoperative discomfort and enables a very predicable outcome, with minimal to no bleeding both during and after the treatment.
This ability to manage the soft-tissue interactions with a laser is very desirable for both the patient and clinician and enables multiple procedures of both periodontal and restorative nature to be performed in the same appointment. However, this can also cause some patient management and reimbursement issues at the same time. Often, when any soft tissue treatment is performed on the same day as a restorative procedure it will be perceived, by the patient and especially insurance carriers, as an incidental process that is part of the restorative care. An example of this is the use of a laser for soft-tissue troughing around a crown preparation instead of using retraction cord for tissue management. The troughing should be considered an incidental process and part of the methodology of the crown procedure.
However, soft-tissue crown lengthening or a gingivectomy/gingivoplasty is often perceived as an incidental procedure, which it is not. One of the best ways to manage these perceptions is with proper documentation as mentioned above. A strictly soft-tissue procedure such as this will not show any radiographic changes between the pre- and post-treatment images. Nevertheless, diagnostic radiographs are required to assist in determining the osseous architecture and ruling out any other pathology. Additionally, the use of photo-documentation with both pre- and posttreatment images can demonstrate what was needed and what has been accomplished.
Laser Principles
While any dental surgical laser can be used to accomplish this procedure, the goal is the same. The techniques vary from device to device, or maybe more appropriately, from wavelength to wavelength. The absorption of laser light energy in the tissue is directly related to the light’s wavelength, which is expressed in nanometers. The greater the absorption of laser energy in the target tissue, the more ablation (vaporization) of the tissue. With the soft tissue of the oral cavity being approximately 70% water, it is the primary chromophore (absorber of light) that is of interest for this procedure. When selecting a laser to use for any procedure, the effects it has on the surrounding and adjacent tissue to the treatment area has to be considered, and its wavelength especially needs to be considered. Incidental contact with non-target areas should be avoided, but unfortunately may occur.
The amount of time the laser energy interacts with the tissue also has a significant impact on the outcome of the procedure. The temporal mode of a laser refers to the timing that energy is emitted by the device; it can be continually emitted (continuous wave/CW) or emitted in a pulsed interval. For this procedure, the pulsed emission is usually the preferred mode, as it allows for greater control of the tissue interaction. Pulsed laser energy assists the clinician in controlling the temperature of the remaining tissue by allowing the remaining tissue to cool before the next pulse of laser energy. Pulsing assists in keeping the remaining tissue from overheating, which can cause tissue sloughing and additional loss of tissue height, and assists in managing its temperature to enable hemostasis.
Power, most often expressed in Watts (W) or Joules (J) (1 W equals 1 J of energy per second) is another variable that the clinician has the ability to control to regulate the amount of laser energy that interacts with the tissue. A high-fluence technique that uses a high amount of energy (expressed mJ/cm2) for a very short pulse duration is yet another way to control the laser’s interaction with the target tissue and its collateral effects on the surrounding tissue.
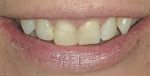
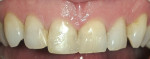
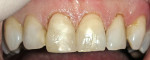
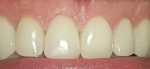
When performing a soft-tissue crown lengthening/gingivectomy, a healthy, predicable outcome is a primary objective, and combining the proper wavelengths with the appropriate power and temporal mode allows the clinician to have a “what you see is what you get” successful result (Figure 1, Figure 2, Figure 3 and Figure 4). The additional ability of some wavelengths (Erbium-class lasers and the 980-nm class diode lasers) to use convection cooling with water irrigation while ablating even further facilitate the clinician’s ability to achieve their desired outcomes.
When diagnosing and performing this procedure, the clinician must still follow all of the basic principles and concepts of proper periodontal care. Even though the clinician is using a laser, they must remember that the laws of physics and principles of treatment do not change. The questions of whether there is an adequate amount of attached gingiva, what is the proper crown-to-root ratio to be obtained, whether there will be proper biological width, is the osseous architecture appropriate, and can hygiene be maintained postoperatively all need to be addressed.
Laser Techniques
Because of the control and precision that lasers provide along with the proper training and experience, practitioners can perform many these soft-tissue procedures with only the use of liquid topical anesthetics. The bloodless nature of laser therapy enhances the clinician’s visualization of the tissue contours and properties during surgical treatment. This greatly reduces the anxiety and stress for both the patient and clinician and increases the efficiency and comfort in which these treatments are performed.
There are two basic techniques that can be used in a soft-tissue crown-lengthening procedure, and the amount of tissue to be removed usually determines which technique might be more appropriate. If a small amount of tissue is to be removed, an ablation technique is often preferred. With this technique the laser energy is delivered in a back-and-forth motion to ablate (vaporize) the tissue in small increments with each stroke (Figure 5). The movement of the laser handpiece is very similar in concept to using a pencil eraser to remove writing from a piece of paper. This process is continued until the appropriate amount of tissue has been removed and the desired treatment objective has been accomplished.
When a large amount of tissue is to be removed, an excisional technique, in which the laser is used in a manner similar to a scalpel, is usually most appropriate. The laser is used to make an incision and a bulk volume of tissue is removed. The clinician often starts this procedure with the laser energy directed perpendicular to the long access of the tooth, moving the handpiece back and forth until there is approximately a 0.5-mm (500-µm) thickness of tissue covering the tooth surface. The laser tip is then placed in the pocket and the remaining 0.5 mm is removed with the laser energy directed away from the tooth structure. The excisional technique is almost always followed up with small amount of the ablative technique to give the remaining tissue the desired contours.
The excisional technique is a similar procedure to performing a biopsy, where a section of tissue is detached as if it is a specimen to be sent to the oral pathologist. If the tissue appears to be clinically healthy, there is normally no need for it to be submitted for a histological examination. However, if there is any suspicion that any abnormality might be present, the tissue should be submitted to a pathology laboratory for examination. Histopathologic examination of such tissue should be performed by an oral and maxillofacial pathologist. When submitting the specimen, a gross description of the clinical findings should be reported on the laboratory requisition form and entered into the patient’s record by the clinician. Clinical photographs of the area are also helpful to the pathologist in establishing the proper diagnosis. It should also be noted on the laboratory requisition form that a laser was used by the clinician to harvest the specimen and that extreme care needs to be taken during the procedure to minimize any heat artifact caused by the laser in the submitted specimen.
Regardless of what technique is used, clinical diligence and preventive measures need to be taken to ensure that the dentition and remaining soft tissue is not inadvertently damaged in the process so that the desired outcome can be achieved.
Conclusion
The laser-assisted soft-tissue crown-lengthening/gingivectomy procedure is a valuable treatment that can establish a healthier and more esthetic appearance regardless of what terminology is used to describe the procedure. With the proper use of most dental surgical lasers, it can be accomplished with relative ease and with minimal discomfort to the patient and less stress to the clinician with an extremely predictable outcome.
References
1. American Dental Association. Current Dental Terminology, CDT 2009-2010.
2. American Dental Association. Current Dental Terminology, CDT 2009-2010. Page 25.
3. Delta Dental of Virginia Clinical Policy Bulletin #409. Available at: https://www.DeltaDentalVA.com. Accessed March 30, 2010.
4. American Dental Association. Current Dental Terminology, CDT 2009-2010. Page 23.
5. American Dental Association. Current Dental Terminology, CDT 2009-2010. Page 23.
About the Author
Scott D. Benjamin, DDS
Private Practice
Sidney, New York