Using a Vasodilator to Reduce Soft Tissue Anesthesia
Reversal agent can improve patient case acceptance.
With the continued improvements of local anesthetics since the advent of procaine in 1905 (marketed as Novocain), dental procedures can be administered virtually pain-free. Postoperative analgesics and anti-inflammatories can also minimize the postoperative discomfort that may be present after typical procedures are done in the dental office. Offices that follow up on patient experiences based on their report of postoperative discomfort alone can be easily misled on how pleasant the experience was for the patient. What is often overlooked is how long it takes for the patient to resume their normal activities after leaving the office. Prolonged soft tissue analgesia can be present for up to 5 hours after injection, while typical pulpal anesthesia lasts about an hour. This is a common complaint of patients and one that has been often ridiculed in the media. In the author’s 25 years of experience, many appointments have been canceled for the fear that prolonged “numbness” would be a detriment to some important event immediately following the dental appointment. Lingering soft tissue numbness makes speaking, eating, drinking, and smiling awkward at best.
A recent study revealed that as much as 88% of the public was interested in a product that would reverse the lingering “numbness.” A new product, OraVerse®, from Novalar Pharmaceuticals (https://www.novalar.com), was recently introduced. Its active ingredient is phentolamine mesylate, a vasodilator that has been shown to help patients recover from soft tissue numbness about twice as fast as normal when used with popular dental anesthetics.
Phentolamine mesylate is not a new drug. It has been used in medicine since the 1950s in adrenal tumor surgery. The purpose of the vasodilator was to combat hypertensive episodes that sometimes occur in surgery. Phentolamine mesylate is indicated for reversal of soft-tissue anesthesia (ie, anesthesia of the lip and tongue) and the associated functional deficits resulting from an intraoral submucosal injection of a local anesthetic containing a vasoconstrictor.1
Phentolamine mesylate is recommended for use in children 6 years of age and older or weighing more than 15 kg (33 lbs). The drug was used in a well-controlled double-blind study in various centers and was given randomly. For the adult group with the mandibular study, 41% of the OraVerse group had fully recovered, compared to only 7% of the control group. Complete normal recovery of mandibular arch numbness occurred by 85 minutes. The maxillary arch fared even better; 59% of the patients given phentolamine mesylate recovered within 1 hour, compared to only 12% of the control group. Complete return to normal sensation averaged 83 minutes for those patients given OraVerse, compared to an average of more than 3 hours for the control group.2
The toxicology reports show that phentolamine mesylate is safe. It has been shown to be non-toxic with no drug interactions. There was only a 1% increase of pain from the injection site compared to the control group. Other adverse reactions were minor and resolved within 48 hours. Pharmacokinetics shows that the half-life of phentolamine mesylate is 2 to 3 hours.2,3
The following case presentation shows the use of OraVerse in a typical restorative procedure done in a private practice setting. Prolonged soft tissue numbness was a concern for the patient.
Case Presentation
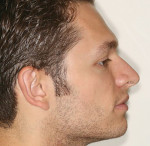
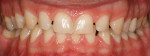
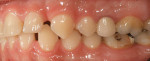
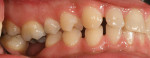
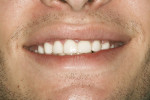
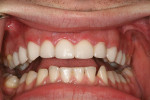
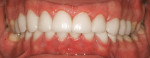
The patient came to our office with the desire to improve his smile (Figure 1, Figure 2, Figure 3). Specifically, he did not like the spaces in both arches (Figure 4, Figure 5, Figure 6). After a complete diagnostic work-up involving an oral examination with radiographs, photographs, and mounted models, the following diagnostic information was noted: soft tissue, periodontal evaluation, and the temporomandibular joint were all within normal limits. Orthodontic diagnosis was Class 1 with normal overjet and overbite, but exhibited a tooth size discrepancy that created 4 mm of spacing. The maxillary anterior teeth were upright and could not be retroclined to close the spaces. A treatment plan was presented to place 18 bonded porcelain restorations to close the spaces that had resulted due to the tooth size discrepancy. Golden proportion was used as a guideline to design the visible widths of the centrals, laterals, and canines. The occlusal scheme was to be designed to have canine disclusion of the posterior teeth during function. The patient was presented with the treatment plan but was concerned about the look of the provisionals as well as the length of lingering soft tissue that would prevent him from going to auditions, because he was an actor.
With this in mind, the use of OraVerse would be included in the treatment plan (Figure 7). The patient was completed in six appointments. At each appointment, when xylocaine with 1:100,000 epinephrine was used (with a maximum amount of two carpules in this case), the vasodilator phentolamine mesylate was used to reverse the “numbing” effect. The following depicts a summary of each appointment and outlines the dosage and administration time when OraVerse was introduced.
First Visit
Two carpules of xylocaine with 1:100,000 epinephrine was used and teeth Nos. 5 through 12 were prepared for minimal-preparation porcelain veneers. A diagnostic wax-up was used and from these a reduction guide was created to keep preparations in the 0.2-mm to 0.5-mm range, with the idea of keeping the restorations in enamel. Polyvinyl impressions were made after a dual-cord technique was used (Ultradent 0 and 1 cords, https://www.ultradent.com), and a centric occlusal record was made with Blu-Mousse (Parkell, https://www.parkell.com) on the prepared teeth. Prior to the fabrication of the provisionals, the patient was infiltrated with two carpules of OraVerse into the same injection sites as the xylocaine. Because the patient was already numb and had been previously informed on why OraVerse was being used, he had given consent. The provisionals were created using a putty matrix from the wax up and a Bis-GMA resin (Luxatemp®, DMG Dental, https://www.dmg-dental.com) that was spot-bonded with phosphoric-acid etch and OptiBond® Solo (Kerr Corporation, https://www.kerrdental.com). The matrix was left on for 3 minutes and then the flash was removed; contours and occlusion were adjusted, then the provisionals were polished. By the time the patient was cleaned up, almost an hour had gone by. He reported that the “numbness” was almost gone. He was set upright and asked to evaluate his provisionals by appearance while both smiling and relaxed and then speaking. Additional adjustments were made and the patient was dismissed with postoperative instructions and his next appointment. The patient was extremely pleased with his provisionals and the ability to return to normal function (Figure 8, Figure 9, Figure 10). He left to make his audition without any concern with soft tissue numbness.
Second Visit
The patient returned 3 days later to re-evaluate his provisionals. Because the patient left the office without numbness, the adjustments were minimal. Embrasures between teeth Nos. 8 and 9 were opened. The cusp tip on tooth No. 11 was rounded off. Photographs of the provisionals were taken along with shade tabs. An alginate of the provisionals was also taken and sent to the laboratory.
Third Visit
Two carpules of xylocaine 1:100,000 epinephrine were used and the provisionals were removed. After remnants of the provisionals were removed, the porcelain veneers were tried in with water-based cement (RelyX™ veneer cement, 3M ESPE, https://www.3mespe.com). Once the patient approved the restorations, they were bonded in after pumice, etching, bonding, and resin cement. Before excess cement removal, recontouring, and occlusal adjustment, two carpules of OraVerse were given. By the time the patient had been cleaned up and had gone to the restroom, he reported that approximately 85% of the numbness had been reversed. He once again was seated upright and occlusal, phonetic, and cosmetic adjustments were made. The patient reported that by the time he returned to his home, 100% normal function had been returned in slightly less than 1.5 hours.
Fourth Visit
Similar to the first appointment, except two mandibular blocks were given with lidocaine with 1:100,000 epinephrine. The lower arch (Nos. 21 through 28) was prepared with the same guidelines discussed previously. Once again, two carpules of OraVerse were given after placement of provisionals. The patient once again reported by the time he was leaving that the numbness was almost gone about 40 minutes after being administered, and completely gone within 30 minutes of leaving the office.
Fifth Visit
The patient was given two mandibular blocks with lidocaine 1:100,000 epinephrine when the provisionals were removed. The porcelain veneers were tried in and evaluated for fit, occlusion, and esthetics and, once they were approved by the patient, were bonded in following the same protocol as mentioned in the third visit (Figure 11). After bonding, the patient was given two carpules of OraVerse so by the time the cement was removed, the patient was already reporting the absence of numbness. The patient was kept in the dental chair and complete soft tissue anesthesia was gone 88 minutes after the OraVerse was given. Adjustments were made for balanced occlusion, esthetics, and phonetics. The patient was then dismissed.
Sixth Visit
The patient was scheduled for follow-up with minimum adjustments made and final photographs were taken (Figure 12, Figure 13, Figure 14).
Conclusion
Patient experience should be a high priority as well as clinical excellence. In the author’s experience, the use of Novalar’s OraVerse as a vasodilator has been extremely successful in reducing patient numbness. It has been shown to be safe, easily administered, and well-received.
Disclosure
Dr. Glassman has received financial support from Novalar Pharmaceuticals..
References
1. OraVerse (phentolamine mesylate) Injection Prescribing Information. January 2009, Novalar Pharmaceuticals, San Diego, CA.
2. Hersh EV, Moore PA, Papas AS, et al. Reversal of soft-tissue local anesthesia with phentolamine mesylate in adolescents and adults. J Am Dent Assoc. 2008;139(8):1080-1093.
3. Moore PA, Hersh EV, Papas AS, et al. Pharmacokinetics of lidocaine with epinephrine following local anesthesia reversal with phentolamine mesylate. Anesth Prog. 2008;55(2):40-48.
About the Author
Steven Glassman, DDS
Glassman Dental Care
New York City, New York