Lithium-Disilicate Pressed Veneers for Diastema Closure
The indirect materials available today to close diastemas include a pressable material composed of lithium-disilicate glass ceramic.
Among the reasons why patients may decline orthodontics to close diastemas are time constraints, desire for immediate esthetic results, or the perceived stigma associated with their age and wearing braces. Another consideration for older women is the fact that oral administration of bisphosphonates is rising in the form of anti-osteoporosis medications. Although they are powerful synthetic inhibitors of bone resorption, long-term oral administration of these drugs is a concern because the drug accumulates in alveolar bones. Possible retardation of tooth movement and increased orthodontic relapse can be a concern. Further, despite a lack of concrete evidence of osteoradionecrosis resulting from orthodontic tooth movement in patients taking oral bisphosphonates, even the slightest hint of complications may negatively influence a “Google savvy” patient.
Not surprisingly, then, closing a diastema can be a challenge, particularly when the clinician is faced with restoring or working with multiple teeth, equalizing space, or removing some tooth structure to accommodate the diastema closure.1,2 If dentists attempt to close diastemas without removing sufficient tooth structure from surrounding dentition, or without altering or adjusting the gingival zeniths of those teeth, the result could be an unattractive width-to-length ratio that detracts from the outcome the patient wanted.1,3
The indirect materials available today for use in closing diastemas include a pressable material composed of lithium-disilicate glass ceramic (IPS e.max® Press, Ivoclar Vivadent, https://www.ivoclarvivadent.us). When used in conjunction with minimal preparation techniques and smile design principles, lithium-disilicate restorations achieve beautiful, natural-looking, and long-lasting results. Lithium-disilicate glass ceramic is unique in dentistry because it demonstrates high strength, natural optical properties, and the ability to be pressed thin. Skilled ceramists can press lithium-disilicate veneers as thin as 0.3 mm.1 When knowledgeable and skilled ceramists create the restorations, natural and durable results can be achieved.1,4
Pressable lithium disilicate is ideal for inlays, onlays, thin veneers, veneers, partial crowns, anterior and posterior crowns, 3-unit anterior bridges, 3-unit premolar bridges, telescope primary crowns, and implant superstructures.5-7 If minimal tooth preparation is desired (eg, thin veneers), ceramists can press IPS e.max lithium disilicate to as thin as 0.3 mm, and the material will still demonstrate a strength of 400 MPa. When sufficient space is available (eg, retrusion of a tooth), no preparation is required. Lithium disilicate is an esthetic, high-strength material that can be conveniently cemented or adhesively bonded.8
However, despite the fact that lithium disilicate enables the placement of conservative veneers, there are diastema closure cases that require more aggressive preparations. If the midline diastema is large, for example, it may be necessary to prepare the distal aspects of the anterior teeth to provide enough room for the veneers.1,9 If this cannot be achieved and the diastema is closed only by additive techniques, an ideal length-to-width ratio may not be possible and the final results less than ideal.1,3Additionally, if the case involves rotated dentition or challenging shade requirements, tooth preparation may be required when no-preparation veneers may have originally been desired.
This article demonstrates the manner in which lithium-disilicate thin veneers were treatment planned and fabricated for a patient in order to close her diastemas. Communication between the ceramist and the dentist was of paramount importance to the success of the case, from case design to the material selection. Shared conservative goals and in-depth discussions about all aspects of the case before actual tooth preparation took place also were invaluable.
Case Presentation
A 60-year-old woman—who had been advised of the need for orthodontics 20 years earlier—presented with a request to improve the overall appearance of her smile. The patient desired the most conservative treatment possible and specifically requested that it not look like she had her teeth “done.”
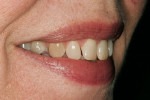
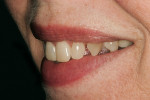
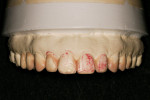
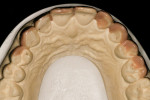
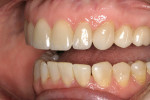
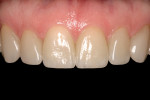
The need for orthodontics to close spaces and correct minor rotations (Figure 1 and Figure 2) was again presented to the patient, who adamantly declined such treatment. A long-term bisphosphonate patient, the slightest possibility of detrimental effects resulting from tooth movement led her to decline this option. The patient also presented with minor lip and gingival asymmetries, but she declined to correct these issues.
A complete examination was performed that included radiographs, mounted diagnostic casts, and intraoral and extraoral photographs. This information was forwarded to the laboratory so that the ceramist could create a diagnostic wax-up, putty matrix, and preparation guides.
Treatment Planning
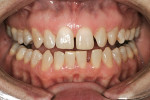
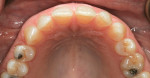
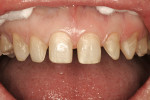
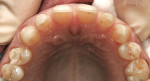
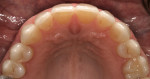
A successful case does not just end with a great ceramist, but it begins with one as well. Through a mutually cooperative relationship, both the dentist and ceramist gained an understanding of each other’s philosophies and requirements, which was extremely helpful in formulating a successful treatment plan for this patient. In particular, the dentist and ceramist collaboratively reviewed the preoperative photographs. At first, it appeared as though the diastemas could be closed with very little or no tooth preparation. However, once the arch form was viewed overall, it became apparent that the patient did not have the slightly lingualized arch form that would have worked well with prep-less treatment (Figure 3 and Figure 4). On the contrary, the patient’s left lateral was out past the wet/dry line of her lip and was visually protrusive. Expanding the arch form to the position of that lateral in order to accommodate no-prep veneers would have created an over-bulked and unattractive result.
Instead, areas of tooth structure that were visually out of ideal position were recontoured or augmented to create an ideal shape and form for the patient. By lingualizing tooth No. 10 and recontouring the distal half of tooth No. 9, the arch form was brought back inside the wet-dry line of the lip, the spaces between the teeth were augmented, and the contour of the individual teeth was adjusted to optimize light reflection and avoid the bulky appearance that is sometimes seen when closing spaces in a smile.
After the case was discussed at length, the ceramist provided an additive/reductive wax-up to guide in preparation design and material selection. Diagnostic wax-ups and preparation guides are invaluable tools that can help to ensure the esthetic, functional, and restorative success of a case by facilitating and enhancing the treatment planning process.1,10 The value of diagnostic wax-ups is their ability to show what will be needed to deliver a predictable clinical protocol in order to achieve the desired outcome.1,10 The diagnostic wax-up was used to create the preparation guides that facilitated ideal tooth preparation.
Ten maxillary veneers and six to eight mandibular veneers were proposed. The goal was to restore the patient’s smile with as little tooth reduction as possible. The patient decided to proceed with the maxillary restorations, but elected to temporarily bond the mandibular anterior dentition, which would be completed at a later date. Therefore, treatment began with traditional teeth whitening.
Preparation and Provisionalization
The limiting factor in the case was tooth No. 10, which was distally rotated and facially positioned. It went from being the no-preparation case requested by the patient to a minimal preparation case. As explained earlier, this was discovered during the initial stages of diagnosis and quantified with the additive/reductive wax-up provided by the ceramist (Figure 5 and Figure 6).
Tooth No. 9 also was slightly facial to tooth No. 8, adding another layer of difficulty relating to the depth of the restorative material and final shade. It was vital to keep tooth preparation to a minimum, conserving as much enamel as possible. The patient’s preoperative shade was Vita A2; the post-bleach shade was Vita A1; and her desired results were in the B1 range. However, the patient did not want the treatment results to be obvious. A small shade shift such as this would also influence preparation planning.
When striving for minimal preparation, the thickness of the material has a great impact on the final shade. Because tooth No. 9 was slightly facially positioned, it required more aggressive preparation. The reduction guide from the additive/reductive wax-up was used to give consistent depth of preparation in relation to the final incisal edge position. By examining where contour was added and where tooth structure was removed in the wax-up and using a matrix from the wax-up, the teeth were prepared in the most conservative manner that would still produce an ideal result (Figure 7 and Figure 8). Over much of the tooth surfaces, no significant structure was removed. Rather, the surface was lightly resurfaced to create a more ideal bonding surface and provide a definitive finish line at the margins.
The wax-up was duplicated with silicone, creating a provisional matrix (Siltec, Ivoclar Vivadent) which was then used to create the provisional restorations. A Bis-acryl material (Perfectemp II, Shade B1, Discus Dental, https://www.discusdental.com) was removed and trimmed, then temporarily seated with spot-etch and translucent flowable composite.
Laboratory Fabrication
After the patient approved the provisional restorations, models and photographs of the provisional restorations became the blueprint that was followed in the laboratory for the fabrication of the definitive restorations. A stick bite and centric relation bite also were sent to the laboratory, along with a facebow transfer. It is important to note that both a stick bite and facebow are needed by the laboratory, because the latter provides information about the distance from the condyles and, thus, the resulting arc of excursive movement. However, it often is not good for information about the horizontal plane, which is why the stick bite is necessary.
An impression of the provisional restorations was used as a matrix to inject wax to the working preparation model. Contour was refined and functional guidance was evaluated. Due to the thinness of the restorations, lithium disilicate (IPS e.max Press) was chosen as the restorative material. The high translucency B1 shade provided the perfect filtering of the underlying tooth color while still being pressed into the 0.2-mm space that had been created throughout many areas of the facial surfaces for the restorations.
A lost-wax pressing technique was used to create the thin IPS e.max Press lithium-disilicate veneers. The patient desired nice incisal effects in the anterior teeth, so the incisal areas of her central and lateral incisors were cut back in the wax prior to investing and pressing the restorations (Figure 9).
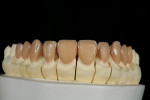
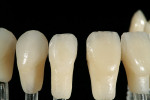
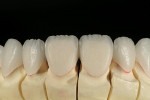
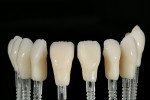
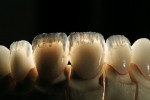
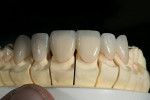
After divesting the lithium-disilicate restorations, the surface anatomy was established by grinding with diamond burs. Composite dies were made to simulate the color effect of the underlying tooth structure, and the restorations were stained to the final desired shade (Figure 10, Figure 11, Figure 12, Figure 13, Figure 14).
Incisal effect powders were built up to create the dentine lobe formations seen in natural teeth. Internal mammelon effects were placed and fired. After evaluating the fired internal effects (Figure 15), a full-contour build-up with opalescent enamel powders was completed, and final contour and a functional evaluation were completed prior to glazing (Figure 16).
Cementation Appointment
Pre-planning, an accurate wax-up, and exquisite provisionalization made delivery of the maxillary restorations uneventful. Traditional bonding procedures included the use of a fifth-generation bonding agent (One-Step Plus, Bisco, https://www.bisco.com) and translucent luting resin (Variolink® II, Ivoclar Vivadent). Rubber dam isolation was essential, not only for moisture control, but for stress reduction as well.
The provisional restorations were carefully removed, and the preparations cleaned with a pumice solution (Consepsis® Scrub, Ultradent Products Inc, https://www.ultradent.com), rinsed, and dried. The veneers were tried in individually with a dry field, which enabled evaluation of fit, marginal integrity, and interproximal contacts. Variolink® Veneer transparent try-in gel (Ivoclar Vivadent) was then used to evaluate color and esthetic integration. After approval from the patient, the veneers were removed and prepared for cementation. Each was etched, silanated, and wetted with bonding agent.
Rubber dam isolation of the preparations was achieved using a split-dam technique. A total-etch 37% phosphoric acid was applied to the preparations for 10 seconds per tooth, then thoroughly rinsed.
The universal adhesive bonding agent (One-Step Plus) was brushed onto the moist preparations, then lightly air-dried. The bonding agent then was light-cured for 10 seconds per tooth.
Translucent Variolink Veneer resin cement was placed in the internal surface of the veneers, after which they were seated. The veneers were spot-tacked at the gingival third by waving the curing light for 3 seconds per tooth from the buccal aspect to initiate the gel-like consistency of the cement. Excess flash was removed before final cure.
Each veneer was cured for 30 seconds from the buccal, lingual, and incisal aspects. Then, the OptraFine diamond polishing paste and bristle brush (Ivoclar Vivadent) were used to polish the margins of the restorations.
Conclusion
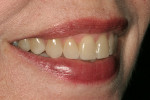
The final results were acceptable to the clinician, ceramist, and, most importantly, the patient (Figure 17, Figure 18, Figure 19, Figure 20). In depth postoperative photographic analysis usually reveals clinical areas that can be improved. It is important to undergo this enlightening process with each case. For the patient in this case, the results delivered a marked improvement in her smile without snowy white cosmetics. The patient was satisfied with the final outcome and beautiful results. The successful completion of this case was the culmination of proper communication between dentist and ceramist and the diagnostic wax-up, preparation guide, and putty matrix used for creating the provisional restorations.1,11
References
1. Dudney TE. Using diagnostic wax-ups and preparation guides to facilitate accurate and esthetic diastema closure and functional bite alternation. Inside Dentistry. 2008;4(7):54-57.
2. Jones A, Robinson MY. A case study: esthetic and biologic management of diastema closure using porcelain bonded restorations for excellent and predictable results. Journal of Cosmetic Dentistry. 2002;18(3):72-83.
3. Gurel G. The Science and Art of Porcelain Laminate Veneers. Chicago, Ill: Quintessence Publishing; 2003.
4. Javajeri D. Considerations for planning esthetic treatment with veneers involving no or minimal preparation. J Am Dent Assoc. 2007;138(3):331-337.
5. Sorensen JA, Cruz M, Mito WT, et al. A clinical investigation on three-unit fixed partial dentures fabricated with a lithium disilicate glass-ceramic. Pract Periodontics Asthet Dent. 1999;11(1):95-106.
6. Höland W, Schweiger M, Frank M, Rheinberger V. A comparison of the microstructure and properties of the IPS Empress 2 and the IPS Empress glass-ceramics. J Biomed Mater Res. 2000;53(4):297-303.
7. Kheradmandan S, Koutayas SO, Bernhard M, Strub JR. Fracture strength of four different types of anterior 3-unit bridges after thermo-mechanical fatigue in the dual-axis chewing simulator. J Oral Rehabil. 2001;28(4):361-369.
8. Fabianelli A, Goracci C, Bertelli E, et al. A clinical trial of Empress II porcelain inlays luted to vital teeth with a dual-curing adhesive system and a self-curing resin cement. J Adhes Dent. 2006;8(6):427-431.
9. Kinderknecht KE, Kupp LI. Aesthetic solution for large maxillary anterior diastema and frenum attachment. Pract Periodontics Aesthet Dent. 1996;8(1):95-102.
10. Garcia LT, Bohnenkamp DM. The use of diagnostic wax-ups in treatment planning. Compend Contin Educ Dent. 2003;24(3):210-214.
11. Chaimattayompol N, Wong SX. Diagnostic management of interdental spacing. J Prosthet Dent. 2000;84(4):467-469.
About the Authors
J.A. Reynolds, DDS, AAACD
Private Practice
Franklin, Tennessee
Matt Roberts, AAACD
CMR Dental Lab
Idaho Falls, Idaho