Conservative Esthetics Using Direct Resin
Clinicians have better choices to conserve valuable tooth structure.
Direct resin restorations are often the ultimate challenge for the restorative dentist as a clinician and artisan. The culminating re sult measures the dentist’s abilities in patient management, smile design, and the understanding of the mechanical and physical properties of dental resins. Chairside, the dentist morphs into the laboratory technician. Resins, opaquers, and tints are layered as a ceramic artist would with porcelain. Today, there is no single direct restorative material that fulfills all the prerequisites for a predictable result: function, esthetics, and biocompatibility, but the combination of materials and techniques can produce a beautiful, synergistic result.1
In an environment of responsible esthetics, it is the clinician’s obligation to design predictable, functional, healthy, and durable restorations that conserve as much of the patient’s original tooth structure as possible.2 Historically, the tendency may have been to digress to heavy-handed preparations of the teeth with complete or partial coverage with ceramic materials. Preparation designs were driven by the clinician’s understanding and choice of materials, instead of by an understanding and diagnosis of the functional design of the system being restored and the existing conditions of the surfaces of the teeth that remained. Our antidotal experience has deepened our appreciation in the conservation of tooth structure. Restorations do not last forever, and clinicians need to weigh the consequences of the latent effect of removal of tooth structure.3 Essential to this approach is the preservation of enamel. The quality and quantity of enamel that remains significantly affects the flexural strength of the teeth and the durability and strength of the bond of the restoration.4,5
Contemporary development of ceramics and resins provide the clinician with alternative choices for a conservative design. The choice of materials is often influenced by the clinician’s experience and skill. The scope and magnitude of the case will also mitigate this decision. Admittedly, direct resin restorations can present a laborious, time-consuming effort. With proper case selection, however, direct resins do remain a viable option for a functionally durable and esthetic result.6
Technique Illustration
The application of direct resin for multiple anterior teeth is a valuable exercise in understanding of the nuances of micro and macro elements of smile design. Although this may be an infrequent restorative selection for many clinicians, simply successfully completing this procedure once will greatly enhance the operator’s ability to predictably complete indirect restorations. Appreciating the concepts of stratification and layering of composites will give the operator insight into the effects of layering ceramic materials and their optical effects, and understand how the influence of the contours and surface effects will help to ensure restorations that predictably emulate nature.7,8
A key element for case selection for direct resin restorations can often hinge on the risk assessment for occlusal forces. Forensic evidence of occlusal disease on the existing dentition will help to define the magnitude of this risk. The ability to move a patient to a Dawson Class I or IA occlusal classification will ensure the predictability of a case. A classic indication for this type of restorative solution is a post-orthodontic case that may exist as a Dawson Class II or IIA that can be equilibrated, with proper analysis, to eliminate any interference in closure to centric occlusion, with deterioration of the facial surfaces of the anterior teeth that support the need for restoration.9
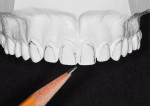
Only after a complete examination and the assessment of the biological, structural, and functional elements can a restorative design be initiated. Model analysis and a diagnostic wax-up will help to illuminate the deficiencies in anterior tooth contours that require restoration. The esthetic examination, through a facially generated diagnostic process, will guide the operator through the essential elements of macro and micro esthetic design parameters. In cases where ultra-conservative preparation design is possible, the foundation shade of the remaining dentition will have an influence of the translucency of the layering resins selected in the restoration. Dental whitening provides an excellent technique to alter this underlying tooth shade, before restoration.10
The selection of resins can then be completed, based on the tooth structure that we are trying to replicate. Dentin is an amorphic layer of the tooth with significantly different optical properties than enamel. Enamel is an essentially transparent crystalline structure that acts as an optical filter over the dentin. With stratification layering of resins, our concept is to use materials that have similar optical properties for each of those layers that we are replacing.11-13 It is important when choosing the appropriate layering resins to do so before preparation. Dehydration of the tooth structure will greatly impact the perceived shade of a tooth. This is best accomplished by creating a custom shade tab, with layers of the anticipated resin in the thicknesses that seem appropriate. Evaluating the cured appearance of the custom shade tab adjacent to the naturally hydrated teeth with which the operator is attempting to harmonize will help ensure the most natural result. Once this shade formulation is discovered, it is critical for the operator to have confidence in it and trust it. The tendency is, during the clinical layering of resin, to begin to modify that formulation based on the appearance at the time of application, which is a visually inaccurate reference to the teeth relative to their naturally hydrated state.14,15
Preparation design is dictated by the inadequacies of the current tooth structure relative to contour, discolorations, and composition. Preparation depths of 0.3 mm to 0.5 mm may be considered reasonable, but may include areas of no preparation because of deficiencies in tooth contour, or more preparation due to previously existing restorations, discoloration, or excessive tooth contour. Resins can then be layered and contoured as desired.16
Contouring, finishing, and polishing resin restorations can often be the greatest challenge. After tremendous effort in design, preparation, and application of the resin, the result can fall short by the elimination of critical line angles, morphology, and surface texture through over-polishing. With patience and experience, this can be accomplished to create a beautifully natural result that harmonizes with the balance of the dentition. One technique to visualize this process is through the use of diagnostic models and photographs. After the initial application of material and contouring, it is often beneficial to stop, take impressions, photograph the case, and reschedule the patient for additional detailing. Operator fatigue often leads to a loss of perspective and a less than optimal result.17-19
Analysis of diagnostic models and photographs give the operator an excellent fresh perspective on the elements of the case that need additional detailing. Observation of line angles, facial embrasures, and surface contours can be better visualized. The operator can then create a specific list of items to be detailed that can then be carried to the operatory at the patient’s next visit to be more effective and efficient in detailing and polishing.
Material Selection
Beyond the obvious parameters of shade and opacity that mimic natural tooth structure, the desired key properties for composite resin materials are strength and the ability to create a sustainable surface luster. In the past, these properties could only be met with a combination of two families of resin materials: hybrids and microfills.20 Hybrids offered the strength and wear characteristics that were required for durability and microfills offered the glass-like luster and translucency needed to mimic the enamel layer. The advance of resin science has launched the development of nano-hybrid composite materials that, through the management of particle size and composition, has given the profession a universal material that can meet functional and esthetic requirements.21-23
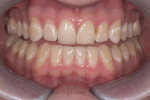
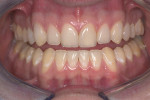
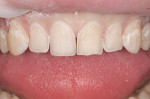
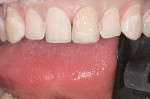
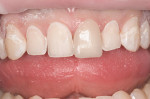
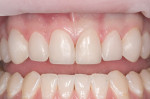
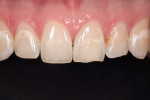
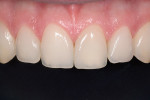
IPS Empress® Direct (Ivoclar Vivadent, https://www.ivoclarvivadent.us) is a nano-hybrid composite that meets these criteria of functional strength and esthetics. It is a light-cured, radiopaque composite, and is offered in 32 different shades and five different degrees of translucency. The interesting property of this material is the luster of surface finish that previously was difficult to obtain and maintain with traditional hybrid restorations. IPS Empress direct also offers the simplicity of stratification by replacement of tooth layers with a resin that mimics those substrates’ physical and optical properties.24 Figure 1, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7, Figure 8, Figure 9 show the excellent results that can be achieved.
Conclusion
In an age of responsible esthetics, the onus is placed on the operator to provide a restorative solution that not only meets the functional and esthetic goals of the patient, but with a design that conserves tooth structure. Direct resin veneers can be a very conservative treatment modality to enhance the smile and restore the confidence of our patients. The frequency with which a dentist may perform these restorations may be limited in many cases, but the insight gleaned is valuable in broader modalities of both direct and indirect restorations. The advent of nano-hybrid composites provides a universal material that will meet treatment requirements in many cases. IPS Empress Direct is a unique system that possesses that attributes of strength, shade compatibility, and finish luster that was not as easily achieved in the past. With the understanding of occlusal concepts and material selection, a predictable result and a happy patient is a validating experience for the dentist.
References
1. Ardu S, Krejci I. Biomimetic direct composite stratification technique for the restoration of anterior teeth. Quintessence Int. 2006; 37(3):167-174.
2. Peters MC, McLean ME. Minimally invasive operative care. II. Contemporary techniques and materials: an overview. J Adhes Dent. 2001;3(1):17-31.
3. Downer MC, Azli NA, Bedi R, et al. How long do routine dental restorations last? A systematic review. Br Dent J. 1999;187(8):432-439.
4. Milicich G, Rainey JT. Clinical presentations of stress distribution in teeth and the significance in operative dentistry. Pract Periodontics Aesthet Dent. 2000;12(7):695-700.
5. Reeh ES, Douglas WH, Messer HH. Stiffness of endodontically treated teeth related to restoration technique. J Dent Res. 1989;68:1540-1544.
6.LeSage BP. Aesthetic anterior composite restorations: a guide to direct placement. Dent Clin North Am. 2007;51(2):359-378.
7. Peyton JH. Direct restoration of anterior teeth: review of the clinical technique and case presentation. Pract Proced Aesthet Dent. 2002;14(3):203-210.
8. Marus R. Treatment planning and smile design using composite resin. Pract Proced Aesthet Dent. 2006;18(4):235-241.
9. Dawson P. Functional Occlusion: From TMJ to Smile Design. Mosby: 2007;104-111.
10.Denehy GE. A direct approach to restore anterior teeth. Am J Dent. 2000;13(Spec No):55D-59D.
11. Blank JT. Simplified techniques for the placement of stratified polychromatic anterior and posterior direct composite restorations. Compend Contin Educ Dent. 2003;24(2 Suppl):19-25.
12. Dietschi D, Ardu S, Krejci I. A new shading concept based on natural tooth color applied to direct composite restorations. Quintessence Int. 2006;37(2):91-102.
13. Terry DA, McLaren EA. Stratification: ancient art form applied to restorative dentistry. Dent Today. 2001;20(9):66-71.
14. Terry DA. Color matching with composite resin: a synchronized shade comparison. Pract Proced Aesthet Dent. 2003;15(7):515-512.
15. Terry DA. Dimensions of color: creating high-diffusion layers with composite resin. Compend Contin Educ Dent. 2003;24(2 Suppl):3-13.
16.Terry DA, Geller W. Selection defines design. J Esthet Restor Dent. 2004;16(4):213-226.
17.Jefferies SR. The art and science of abrasive finishing and polishing in restorative dentistry. Dent Clin North Am. 1998;42(4):613-627.
18.Goldstein RE. Finishing of composites and laminates. Dent Clin North Am. 1989;33(2):305-318, 210-219.
19. Barghi N, Lind SD. A guide to polishing direct composite resin restorations. Compend Contin Educ Dent. 2000;21(2):138-144.
20. Pereira CL, Demarco FF, Cenci MS, et al. Flexural strength of composites: influences of polyethylene fiber reinforcement and type of composite. Clin Oral Investig. 2003;7(2):116-119.
21.Drummond JL, Lin L, Al-Turki LA, Hurley RK. Fatigue behaviour of dental composite materials. J Dent. 2009;37(5):321-330.
22. Ilie N, Hickel R. Investigations on mechanical behaviour of dental composites. Clin Oral Investig. 2009;13(4):427-438.
23. Mahmoud SH, El-Embaby AE, AbdAllah AM, Hamama HH. Two-year clinical evaluation of ormocer, nanohybrid and nanofill composite restorative systems in posterior teeth. J Adhes Dent. 2008;10(4):315-322.
24. Antonson DE. Composite resin materials: nano-what? Dent Today. 2009;28(5):124-127.
About the Author
Scott Finlay, DDS
Coordinator
Advanced Restorative Track
The Dawson Academy
St. Petersburg, Florida
Accredited Fellow
American Academy of Cosmetic Dentistry