Caries Detection Technologies
Dentists are routinely using caries risk assessment employing advanced detection technologies to identify patients who are at increased risk for dental caries.
In 1926, G.V. Black foresaw a day when the dental profession would be truly prevention-oriented and dentists would so well understand the pathogenesis of dental caries that they would be able to effectively treat and prevent its damaging results.1 Yet in the United States today, the dental caries rate in children continues to increase and senior patients are challenged with increasing medication-induced xerostomia (MIX disease), elevating their risks for decay.2,3 The sum result is that dentists continue to spend the majority of their time preventing, actively treating, and/or restoring the real damages from dental caries, and the dream G.V. Black had remains unrealized.
We have long understood dental caries to be a bacterial-mediated disease, involving the two primary pathogens Mutans streptococci and Lactobacillus. However, recent biofilm science has expanded this disease model to include numerous pathogens in a biofilm community. Current biofilm research indicates dental caries is a pH dysfunction of the biofilm that may be a result of the behavior as well as the actual make-up of the biofilm.4,5 This biofilm disease model is changing the way the profession views dental caries. In the past, dentists diagnosed dental caries as lesions of the teeth that required restoration strategies.6This was accomplished with a visual examination, radiographs, and a sharp explorer. The age of Bob Barkley and preventive dentistry added homecare and dietary education, fluoride application for remineralization, and pit-and-fissure sealants to the therapy mix in an attempt to prevent carious lesions. Evidence-based fluoride application recommendations are now established by the American Dental Association and include the routine use of fluoride varnish every 3 months on moderate and high-risk patients.7 Additionally, resin-based pit-and-fissure sealants are recommended for all “at risk” posterior teeth in both children and adults.8 Now dentists are also routinely using caries risk assessment to identify both patients who are at increased risk for dental caries, and the individual risk factors for each patient to design an individual-specific treatment protocol. With the biofilm science changing the understanding of this disease, new strategies will emerge to help medically manage the dysfunctional behavior of the biofilm.9 As the profession becomes more involved in risk assessment and early identification of the disease indicators, it becomes paramount to identify caries activity at its earliest stages. Several technologies have evolved to help dentists identify the earliest physical sign of dental caries, demineralization. The restorative strategies can then also be minimally invasive and provide patients with the best possible treatment outcomes.
Caries Detection Technologies
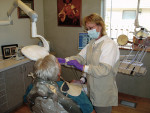
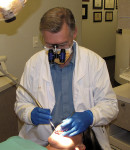
Numerous new technologies have been developed recently to identify demineralization, the earliest sign of dental caries, but several other improvements to existing technologies have also occurred and deserve mention here. Radiographs played an early role in identifying carious lesions, but as the speed of the film increased, and the radiation dosage decreased, the contrast in density of tissue became more difficult to interpret. This was also compounded, perhaps, by the expanded use of fluoride making enamel more resistant to demineralization, and, suddenly, the issue of hidden-decay became a daily reality for practitioners. Improvements in digital radiography and sensors (Figure 1), coupled with the development of software tools to manipulate images, has certainly overcome many of these issues.10 However, digital radiography alone is not enough. Magnification and accessory illumination, or loupes and headlights, have definitely enhanced the visual examination and the dentist’s ability to be more accurate in identifying caries activity (Figure 2). Combined, these improvements have dramatically improved the old “pick and stick” technology of the past. Sensitivity and specificity in caries detection can be enhanced even further yet with several new emerging technologies. This results in more accurate diagnosis and overall treatment planning and outcomes.
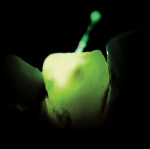
Laser fluorescence has been reported in the dental literature for a long time, now often referred to as QLF, or as laser-induced-fluorescence. When laser light is directed at hard dental tissue, there is a shift in the wavelength of the light being reflected back from the tooth depending on the nature and density of the tissue. This spectral shift in the emission light was identified and reported early on with the Argon laser (Figure 3). Laser light also had the ability to provide better transillumination of the tooth to identify demineralized zones.11,12
Digital imaging fiber-optic transillumination (DIFOTI®, Electro-Optical Sciences, Inc, https://www.eosciences.com) is a transilluminating camera that identifies zones of demineralization and captures images of the illuminated tooth using visible light.13 The examination can be made in real time as the practitioner moves the camera throughout the patient’s mouth. DIFOTI also has the advantage of being able to demonstrate changes in density even interproximally. In fact, a recent study concluded that the DIFOTI, when used in conjunction with radiography, could improve the identification and, to some degree, the depth of interproximal lesions, even in very small lesions.14 As with the pit-and-fissure lesion, this could be a real advantage in trying to determine when to remineralize and when to surgically intervene in cavitated lesions. The challenge for DIFOTI, and all transilluminating technologies, is that while they can successfully show zones of change, they cannot provide data as to whether or not the zone is active, inactive, or actually remineralizing from one single real-time examination.
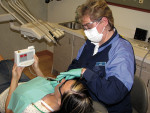
DIAGNOdent (KaVo USA, www.kavo usa.com) is a 655-nm diode laser caries detection device that was first introduced to aid in the identification of pit-and-fissure lesions.15 The device (Figure 4), is calibrated to the reflectance for each individual patient’s teeth, and there is both a two-digit and audible display. Pit-and-fissure lesions often progress unidentified under seemingly intact and healthy enamel and may lead to serious internal lesions and even pulpal death before the overlying enamel fractures become visibly evident. Many authors have previously described these hidden lesions, attempted to explain their cause, and provide rationale for the best treatment. There has been controversy over when and how to deal with these lesions, and whether the routine microscopic opening and exploration (caries biopsy) of suspicious-looking fissures results in any long-term savings of healthy tooth structure.16 Frankly, there probably has been both overtreatment and undertreatment of these lesions as dentists struggled to figure out a best evidence-based solution in addressing them. The DIAGNOdent brings additional quantitative data to the examination of occlusal pits and fissures, with recommendations for initial surgical intervention. Repeated studies indicate that the DIAGNOdent increases both the sensitivity and specificity in diagnosis when used as an adjunct to visual and radiographic examination.17
The Caries I.D.™ (DENTSPLY Professional, https://www.cariesid.com) handheld device is also a diode or LED laser device that uses a green wavelength of light to look for areas of demineralization. When zones of demineralization are displayed, the LED changes to a red color and there is also an audible beep tone. The tip is moved in light contact along tooth surfaces. The device is lightweight and highly portable and gives the dentist the feel of using traditional handheld instruments. A PubMed search revealed no published studies on this newly introduced device.
The Spectra instrument (Air Techniques, https://www.airtechniques.com ) is yet another laser caries illumination device that uses a 405-nm blue-violet LED or diode laser and an image capturing technology (Figure 5). This illumination technology also is coupled with analytical (Visix) software (Air Techniques), which then displays the zone of demineralization as a photograph of the tooth, and varying zones in differing colors of green, blue, red, orange, and yellow. The images can be stored and then repeated examinations can demonstrate specific changes in density of the tooth. This can provide objective data to determine the progression of lesions or the effectiveness of remineralization therapy. A Pub Med search did not reveal any published studies on this device.
The Sopro-Life system by the Acteon Group (https://www.acteongroup.com) is a handheld LED camera (Figure 6) that has a specific CCD sensor enabling tooth surfaces to be illuminated in the visible spectrum and provides a diagnostic fluorescence image superimposed on a picture of the tooth. There are three modes with the camera: daylight mode for capturing intraoral images, and both diagnostic and treatment fluorescence modes. The diagnostic mode helps identify lesions in the occlusal and interproximal regions and the treatment mode is designed to aid in the removal of caries lesions.
In the near future a handheld ultrasound device may be available to dentistry. Currently under development by S-Ray Corporation, the ultrasound handpiece will provide real-time 3-dimensional images that will detect cracks and dental caries lesions without any radiation. The dental professional will be able to view the color 3-dimensional image from any angle.
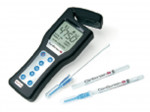
Other emerging technologies in caries diagnosis include measuring the biofilm activity and diagnostics for the caries potential of the saliva. The CariScreen system (CariFree, https://www.carifree.com) is a chairside real-time test using a meter and swab (Figure 7), combined with ATP bioluminescence technology, which has been demonstrated in studies to identify the potential caries biofilm activity and caries risk.18 The Saliva-Check Salivary Testing Kit (GC America, https://www.gcamerica.com) is a chairside real-time test designed to check the quantity, pH, buffering capacity, and sugar metabolism potential of the patient’s saliva. These technologies are directed at identifying the potential biofilm or systemic dysfunction of the patient, not identifying carious lesions per se, and aid in the correct risk assessment and treatment recommendations for the patient.
Conclusion
The emerging biofilm science is changing how the dental profession looks at dental caries as a disease model. This more accurate, but also more complex, picture of dental caries anticipates the need for new technologies to better assess, detect, and diagnose signs of disease presence, progression, and activity levels. By early and accurate identification of dental caries, medical model therapies and minimally invasive surgical procedures provide patients with the best predictable treatment outcomes possible today. Tomorrow they may provide the answers to the prevention-oriented profession G.V. Black envisioned so many years ago.
Disclosure
Dr. Kutsch is the CEO of CariFree/Oral BioTech.
References
1. GV Black. Operative Dentistry. 1926.
2. Bagramian RA, Garcia-Godoy F, Volpe AR. The global increase in dental caries: a pending public health crisis. Am J Dent. 2009; 22(1):3-8.
3. Kutsch VK, Cady C. MIX disease: diagnosis and treatment. Inside Dentistry. 2009;5(7):80-83.
4. Marsh PD. Dental plaque as a biofilm and microbial community—implications for health and disease. BMC Oral Health. 2006;6(Suppl):S14.
5. Takahashi N, Nyvad B. Caries ecology revisited: microbial dynamics and the caries process. Caries Res. 2008;42(6): 409-418.
6. Young DA, Kutsch VK, Whitehouse J. A clinician’s guide to CAMBRA: a simple approach. Compend Contin Educ Dent. 2009;30(2):92-98.
7. American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride: evidence-based clinical recommendations. J Am Dent Assoc. 2006;137(8):1151-1159.
8. Beauchamp J, Caufield PW, Crall JJ, et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants. J Am Dent Assoc. 2008;139(3):257-268.
9. Filoche SK, Soma D, van Bekkum M, Sissons CH. Plaques from different individuals yields different microbiota responses to oral-antiseptic treatment. FEMS Immunol Med Microbiol. 2008;54:27-36.
10. Kutsch VK. Digital radiography: improving image quality. Pract Proced Aesthet Dent. 2006;18(5):289-290.
11. Kutsch VK. Caries Illumination with the Argon Laser: A Clinical Trial. ISLD 3rd International Congress, SLC UT. 1992. Abstract #044.
12. Kutsch VK. Lasers in dentistry: comparing wavelengths. J Am Dent Assoc. 1993;124(2):49-54.
13. Schneiderman A, Elbaum M, Shultz T, et al. Assessment of dental caries with digital imaging fiber-optic transillumination (DIFOTI): in vitro study. Caries Res. 1997;31(2):103-110.
14. Bin-Shuwaish M, Yaman P, Dennison J, Neiva G. The correlation of DIFOTI to clinical and radiographic images in class II carious lesions. J Am Dent Assoc. 2008;139(10):1374-1381.
15. Khalife MA, Boynton JR, Dennison JB, et al. In vivo evaluation of DIAGNOdent for the quantification of occlusal dental caries. Oper Dent. 2009;34(2):136-141.
16. Hamilton JC, Dennison JB, Stoffers KW, et al. Early treatment of incipient carious lesions: a two-year clinical evaluation. J Am Dent Assoc. 2002;133(12):1643-1651.
17. Goel A, Chawla HS, Gauba K, Goval A. Comparison of validity of DIAGNOdent with conventional methods for detection of occlusal caries in primary molars using the histological gold standard: an in vivo study. Indian Soc Pedod Prev Dent. 2009;27(4):227-232.
18. Pellegrini P, Sauerwein R. Plaque retention by self-ligating vs. elastomeric orthodontic brackets: quantitative comparison of oral bacteria and detection with ATP bioluminescence. AJO-DO. 2009;135(4):426-427.
About the Author
V. Kim Kutsch, DMD
Private Practice
Albany, Oregon