Post and Core Foundations for Esthetic Restorations
The “foundation restoration” is an extremely important part of the restorative process.
When large, defective restorations are removed, the remaining tooth structure must be reinforced with a material that will act as a “dentin replacement” that will support and strengthen the resulting preparation. When restoring endodontically treated teeth, the foundation restoration (core) is anchored to the tooth via the root canal system, using a post that is first bonded or cemented in place. When posts are required prior to the restorative process, certain biologic factors must be considered. Conservation of tooth structure during post space preparation is essential, because placement of a post does not reinforce tooth structure, but provides retention and resistance form for the coronal restoration.1 One half of the post length should be surrounded by alveolar bone to prevent lateral forces on the tooth/restoration complex causing potential root fractures by transmitting forces from the end of the post to the adjacent root surface, and prevent separation and/or breakage of the post/core/restoration complex.2 When the post is carefully positioned and cemented to place, the core material must have intimate contact around the post surface to help anchor it in place. It is also important to have sufficient “ferrule” (at least 2 mm) so that loading forces are not concentrated at the core-tooth interface and thus transmitted to the post which can lead to post fracture, debonding of the core or vertical root fracture.The bulk of the “foundation restoration” will then be prepared like tooth structure, incorporating the core into the final preparation design.3
Requirements of a Foundation (Core) Material
Two important features of a core build-up material is that it bond well to enamel and dentin, and it prepare as much like tooth structure as possible so that ditching does not occur during preparation.4 Additionally, the use of the core forms make fabrication of properly formed cores that resemble preparation form fast and simple. The following case presentation will describe the use of prefabricated post-and-core foundation restoration in a decimated root-filled tooth.
Case Presentation
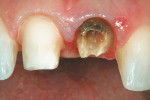
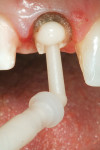
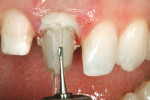
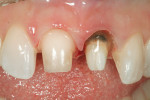
The patient in Figure 1 had root canal retreatment therapy completed on tooth No. 9. As seen in the clinical photograph, there was very little coronal tooth structure remaining. The author felt that the Flexi-Flange® Prefabricated Post System (Essential Dental Systems, https://www.edsdental.com) would be ideal for this clinical situation. A metal post was selected for this case due to lack of remaining tooth structure, but it is important to note that fiber versions of this post system are also available. Flexi-Flange helps to dissipate occlusal forces to eliminate intraradicular stress fractures. The flange portion of the post countersinks completely into tooth structure to maximize fracture resistance of the root and post by safely dispersing occlusal forces over a broad area. Combined with a second tier that adapts to the natural flare of the canal, Flexi-Flange reduces stress concentrations that cause fractures, while post strength and retention are dramatically increased.5-12
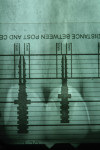
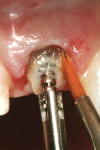
A digital x-ray was taken and the measurement tool was used to determine the amount of gutta-percha to be removed from the root canal space. The post-hole preparation began by using a Gates-Glidden drill to remove all but the apical 5 mm of gutta-percha. The transparent Flexi-Flange Depth gauge was used overlaying the radiograph to help the author select the appropriate size post for the diameter of the root present at the most apical portion of the post (Figure 2). A primary reamer corresponding to the selected post size was used to shape the root canal space coronal to the remaining root canal fill.
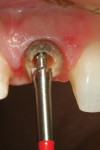
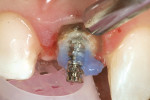
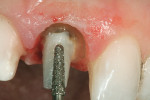
Next, the countersink drill/root facer was used to cut two preparations in one operation. It prepared a seat for the second tier of the post as well as the flange. It is critical that the post fully seat in the prepared space. This is determined by a flush seating of the flange within its preparation (Figure 3). A trial insertion of the Flexi-Post was made to ensure accuracy of fit and position. It is suggested that a radiograph be taken at this point to verify that the apical obturation is still properly positioned and has not been dislodged in the post preparation steps. Should the seal have been disrupted, new obturation material can quickly be placed and the post placement may continue.The wrench was used to create the thread line inside the root canal for the post. Using the wrench to carefully tighten the Flexi-Flange into post preparation will create a thread line into dentin that will be followed when the post is screwed to place during cementation. The flange must fully seat into the internal countersink preparation to strengthen the internal aspect of the tooth and to help dissipate occlusal forces that could cause failure of the post and overlying restoration.
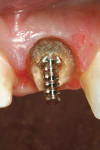
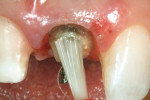
After the post was unthreaded from the root, it could be shortened if necessary to allow complete seating of the flange. An x-ray was taken to verify complete trial seating (Figure 4). Next, a self-curing resin cement was placed in the post space (Flexi-Flow Auto E, EDS) and on the post itself (Figure 5). The post was then placed into the canal space with the wrench and screwed in to complete seat, and the excess cement was removed prior to setting with a sable brush, allowing visual verification of complete seating (Figure 6). Once the Flexi-Post was cemented to place, the appropriate core form was chosen and tried on the tooth, and trimmed with scissors as necessary, to ensure accurate fit. Flexible core forms were used because they could be more easily removed without torquing the set core material. A size and shape resembling a maxillary anterior tooth preparation was chosen and tried in place. The entire tooth surface was then etched with 37% phosphoric acid for 15 seconds, then thoroughly rinsed and air-dried, being careful not to desiccate the dentin (Figure 7). A fifth-generation dentin bonding agent (Figure 8) was applied to all tooth surfaces and light-cured for 20 seconds. The dual-cure core build-up material (Ti-Core Auto E, EDS) was injected into the core form and placed over the tooth, held in place with a plastic instrument, and light-cured through the core form.
Next, the matrix was sectioned using a small carbide bur (Figure 9 and Figure 10), and removed to avoid torquing the core material. The tooth preparation was then completed for the definitive restoration. After preparation, a double-cord technique was used to make the master impression. First, a #00 cord was placed circumferentially into the gingival sulcus followed by a #1 cord immediately above (coronal) to it. After removal of the top cord, a light-bodied impression material was syringed into the retracted sulcus followed by placement of the heavy-bodied filled maxillary full-arch impression tray.
The Definitive Restorations
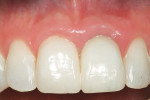
Figure 11 shows the completed preparations for tooth Nos. 8 and 9. Note that the preparation for tooth No. 8 was very conservative and that the preparation color was normal to light. Because of the amount of missing tooth structure on tooth No. 9, and the darkness of the remaining root, both preparations were prepared with intra-crevicular margins. It is recommended to use a material that will adequately block or cover the low-value preparation (such as on tooth No. 9 in this case) and that the same type of restoration is chosen for the adjacent tooth to maximize the ability to esthetically match the restorations. For this case, zirconium (Lava™, 3M ESPE, https://www.3mespe.com) was chosen to predictably match the shade of the two maxillary central incisors being restored. Figure 12 shows the restorations at delivery after cementation. The definitive zirconium restorations were cemented using a self-etching resin cement. A new zirconium primer (Z-Prime™ Plus, Bisco, https://www.bisco.com) was used to increase the bond strength of the cement to the zirconium substrate.
Conclusion
A technique has been described using Flexi-Flange prefabricated posts in conjunction with Ti-Core core build-up material to build a solid post and core in a decimated root-filled tooth prior to fabrication of a full-coverage restoration. The unique design of the post helps to minimize stress by conforming to the root morphology and, due to the flange design, helps to dissipate functional stresses so critical to long-term success of post-filled teeth.
References
1. Sorensen J. Preservation of tooth structure. J Calif Dent Assoc. 1988;16(11):15-22.
2. Quintas AF, Dinato JC, Bottino MA. Aesthetic posts and cores for metal free restoration of endodontically treated teeth. Pract Periodont Aesthet Dent. 2000;12(9):875-884.
3. Perel MI, Muroff FI. Clinical criteria for posts and cores. J Prosthet Dent. 1972; 28(4):405-411.
4. Reality. 2001;15(1):132.
5. Cohen BI, Musikant BL, Deutsche AS. Comparison of photoelastic stress for a split shank treaded post versus a threaded post. J Prosthodont. 1994;3:53-55.
6. Cohen BI, Condos S, Deutsch AS, Musikant BL. Comparison of photoelastic stress properties for four prefabricated post systems. J Dent Res. 1995;74:557.
7. Millstein PL, Yu H, Hsu CS, Nathanson D. Effects of cementing on retention of a prefabricated screw post. J Prosth Dent. 1987;57:171-174.
8. Brown JD, Mitchem JC. Retentive properties of a dowel post system. Oper Dent. 1987;12:15-19.
9. Cohen BI, Pagnillo MK, Neuman I, et al. Torsion tests on endodontic posts. Compendium. 1996;17(9):860.
10. Dietschi D, Romelli M, Goretti A. Adaptation of adhesive posts and cores to dentin after fatigue testing. Int J Prosthodont. 1997;10(6):498-507.
11. Christiansen GJ. Post and cores: State of the art. J Am Dent Assoc. 1998;129(1): 96-97.
12. Assif D, Gorfil C. Biomechanical considerations in restoring endodontically treated teeth. J Prosthodont Dent. 1994;71(6):565-567.
About the Author
Robert A. Lowe, DDS
Private Practice
Charlotte, North Carolina