Canine Substitution vs Restoration
Esthetic considerations for the restoration of a congenitally missing lateral incisor and diastema closure.
Appearance is very important in today’s society for both business and social reasons. This increased awareness has fueled a rapid growth in esthetic dentistry, dental materials, and the dental technology to satisfy these needs.1 The successful completion of treatment is predicated on a thorough initial clinical examination, initial esthetic examination, and understanding of the patient’s chief complaint.2 The treatment has to be tailored to the needs of the patient.3 Before the initiation of treatment an esthetic evaluation is needed. The relationship of the teeth, lips, and gingiva have to be taken into account.4 Restoring anterior teeth requires knowledge of esthetics, dental materials, and the knowledge of the functional relationship between the palatal surfaces of the maxillary anterior teeth and the incisal edge of the mandibular anterior teeth.5 This case report will delineate the treatment of a patient having a congenitally missing maxillary left lateral incisor, midline diastema, and worn dentition due to bruxism. Options for treatment, selection of materials, and treatment sequencing will be described.
Congenitally missing maxillary lateral incisors can be managed with three treatment options. These options are canine substitution, a tooth-supported restoration, and a single-tooth implant.6 The amount of space, the patient’s age, type of occlusion, and the status of adjoining teeth have to be considered. The minimally invasive treatment that satisfies the patient’s esthetic needs and provides appropriate function should be the selected treatment. The interdisciplinary approach provides the guidelines necessary to achieve the best possible results. Removable partial dentures, fixed partial dentures, resin-bonded bridges, orthodontic repositioning to close the space, and a single-tooth implant need to be considered.
Tooth agenesis can consist of hypodontia, which is the absence of one to six teeth excluding third molars; oligodontia, which is the absence of more than six teeth excluding third molars, or anodontia, which is the loss of all the teeth. Agenesis of teeth can be either non-syndromic (genetic-based) or syndrome- or systemic disease-based. More than 60 syndromes have been identified that are related to tooth anomalies (eg, ectodermal dysplasia).7 Syphilis, scarlet fever, rickets, or nutritional aberrations during pregnancy can affect both tooth and organ development. The maxillary lateral incisor develops in the area of embryonic fusion between the lateral and median nasal processes and may be more susceptible to modification. Because non-syndromic hypodontia is more prevalent than the syndromic variation, a history of agenesis in the family and the possible cause may allow the treating dentist to advise the parents on the need for early intervention or prosthetic treatment at a later date.8,9
Two types of occlusion allow canine substitution: Angle Class II malocclusion and no crowding in the mandibular arch have the premolars located in the usual canine position and the molars in Class II position, and Angle Class I malocclusion with crowding requiring mandibular extractions. Both of these conditions would require lateral excursion with group function.6 A relatively straight profile or even one with a slightly convex profile may be appropriate but a patient with a convex profile, retruded mandible, and deficient chin prominence are inappropriate for canine substitution. The shape, color, and crown width at the cementoenamel junction of the canine also have to be taken into consideration. The ideal replacement for the lateral would be a canine the same color as the central, narrow at the cementoenamel junction and mid-crown, with a flat labial contour. The visibility of the gingival level on smiling will indicate the necessity for corrective periodontal surgery to place the gingival margins in their appropriate position. The main advantage of space closure is that after finishing the orthodontics, no retainers are needed to maintain the space. The only restorations that may be needed are porcelain veneers if the teeth cannot be conservatively reshaped. Bleaching may be enough to correct shade. A palatal splint may be required for retention. The disadvantage is that a canine-protected occlusion cannot be established and some feel the canine eminence in the wrong position may adversely affect facial esthetics.10
However, many patients do not meet the criteria for canine substitution and a restoration is required. The restoration of the lateral incisor could be a traditional fixed partial denture (FPD), a resin-bonded prosthesis, implant, or a removable prosthesis. The FPD could be either metal-ceramic or entirely ceramic in nature. An all-ceramic bridge will eliminate the grey hue that may occur with the use of a metal collar. Creation of an ovate pontic and reforming lost papilla is critical in eliminating black triangles.11 Resin-bonded FPDs also can be used. The main disadvantage is the possible graying of the abutment teeth if a high degree of translucency exists and the metal retainer shows through. A deep overbite is also a contraindication as less area is available for retention and increased lateral forces are present.12 The lateral incisor also can be cantilevered off the canine with full coverage on the canine or possibly pin retention.
There are three ways to determine the space required for the missing maxillary lateral incisor. Some restorative dentists have used the golden proportion. However, this method only determines the perceived width from the frontal view and a range of lateral widths have been considered esthetic.12 The second method entails the use of the contralateral incisor if its measurements are within normal limits. The Bolton analysis also can be used to determine the width of the lateral incisor. The Bolton ratio is determined by dividing the mesiodistal width of the mandibular anterior teeth and dividing it by the mesiodistal width of the maxillary teeth. This ratio is usually about 0.78. A diagnostic wax-up will confirm the optimal spacing. The central incisors are positioned for esthetics and posterior disclusion. The canines are positioned to allow anterior and posterior disclusion.
Case Report
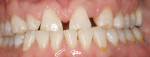
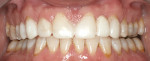
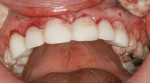
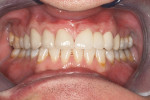
A 36-year-old healthy man presented to the NYU International Program in Aesthetic Dentistry with a chief complaint of “the desire to improve esthetics” because of dark teeth, worn incisal edges, midline diastema, and a congenitally missing left maxillary lateral incisor (Figure 1). He was an actor, so esthetics was critically important to him.
The clinical examination revealed a congenitally missing left lateral incisor and an edge-to-edge occlusion. Periodontal probing discerned no abnormalities. The radiographic examination demonstrated the apices of the central incisors were distal to the coronal aspect. This created a potential restorative and periodontal problem that needed to be addressed.
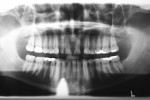
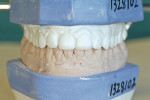
Study models were obtained using a polyvinyl siloxane material for accuracy (Reprosil, DENTSPLY Caulk, https://www.caulk.com) Full-mouth X-rays and Panorex were taken. Photographs also were taken and periodontal charting was completed. The X-rays revealed the two centrals had their roots divergent at their apex and a reverse curve of the incisal edge (Figure 2). The medical history was noncontributory except for the taking of Fosamax 40 mg weekly, which would have increased the length of time for orthodontic treatment if elected.13,14
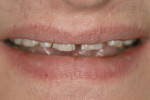
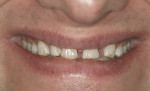
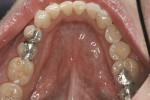
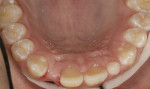
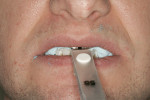
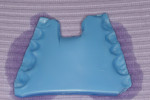
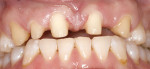
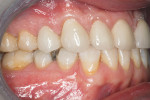
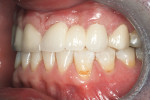
There was no relevant dental history. Extraoral examination indicated a convex profile. With lips at rest there was no incisor display. With a normal smile, there was 1 mm of incisal display (Figure 3) and with a forced smile 2 mm (Figure 4). There was a Class I molar relationship. Maxillary midline and philtrum were not coincidental. Vertical overlap was zero and horizontal overlap was zero due to bruxing. Wear was present on the incisal edges of his maxillary and mandibular anterior teeth (Figure 5 and Figure 6). Oral hygiene and periodontal health were within normal limits. A bite registration was obtained with Blu-Mousse® (Parkell Inc, https://www.parkell.com) in centric relation after using a leaf gauge to determine the first point of contact (Figure 7). An occlusal index of the maxillary arch (Figure 8) and the properly indexed models were sent to the laboratory along with digital photographs and a detailed prescription.
The patient was given the recommended option of orthodontic treatment to close the diastema, parallel the roots, and make space for an implant in the maxillary left lateral position and to open the bite slightly in the anterior to make room for longer central incisors. A second choice was limited orthodontics to correct only the anterior spacing problem. However, orthodontic treatment may have been prolonged due to slower than expected tooth movement because of the bisphosphonate treatment. Orthodontic treatment relies on osteoclastic activity to permit tooth movement. Orthodontic movement also results in increased bone turnover and this may result in the increase of bisphosphonate uptake. The final choice was restorative with full-ceramic crowns (Lava™, 3M ESPE, www.3mespe.com) on teeth Nos. 6 through 8 and an all-ceramic bridge (Lava) extending from teeth Nos. 9 through 11 with Lava crowns on teeth Nos. 5 and 12 to fill out the bilateral negative space in the posterior.
Periodontal Phase
Once the diagnostic wax-up was completed by the laboratory and approved by the treating doctors (Figure 9) and the patient, an intraoral mock-up using a Bis-acryl material (Luxatemp®, DMG, https://www.dmg-dental.com) was fabricated (Figure 10). This allowed the treating doctors and the patient to assess the shade, length, contour, and phonetics. In addition, the amount of gingival display as framed by the lips was assessed to determine if any adjustment were required to the supporting periodontium.4 Teeth Nos. 5 through 9, 11, and 12 were prepared for Lava crowns (Figure 11). The putty preparation guide created from the diagnostic wax-up was used to ascertain that adequate reduction was performed as the midline was being moved and space was created for the upper left lateral incisor. A provisional bridge using acrylic was fabricated for additional strength.
Four distinct adjustments were required for the periodontal phase. The first related to the closing of the diastema without orthodontics. Instead, the restorations for the central incisors would have to be overbuilt toward the mesial. This would have impinged on the existing gingiva in the midline papilla and required a gingivectomy to create space for the additional porcelain on the mesial of each central. Once an adequate amount of gingival tissue was removed to make room for the new restorations, it was necessary to “sound” the bone in the horizontal direction. This would ensure that there was room for the “biologic width” between the new porcelain restorations and the bone.2 Normally biologic width is thought of in a vertical direction probing down along the root surface. This is accepted as being approximately 2 mm; 1 mm of connective tissue and 1 mm of junctional epithelium. However, alveolar bone is always covered by at least 2 mm of gingiva even if a tooth is not present. This would be fine for an edentulous area of alveolar bone. In this case, there would be approximately 1 millimeter of connective tissue and 1 millimeter of keratinized epithelium in place of the junctional epithelium that sealed the periodontium around a tooth. Therefore, it was necessary to ensure that 2 mm of space was available between the new, wider porcelain restorations and the alveolar bone under the midline papilla so that the gingiva could exist in health and harmony with the restorations. Sounding showed that the 2 mm of space was already present in the horizontal direction so it was not necessary to open a flap and perform alveoloplasty. The diastema between teeth will dictate the soft tissue level and the underlying bone will form accordingly.15 If the distance between the contact point and the osseous crest is less than 5 mm there will be a papilla fill; however, the interproximal bone will not be located 3 mm from the coronal aspect of the papilla.16
The second adjustment related to changing the zenith of the central incisor. The zenith of the gingival margin (the most apical point of the gingival margin) is generally slightly to the distal of the midline of the tooth for the maxillary central and the middle for the lateral incisor. Because the central incisors were restoratively being moved to the midline, the zenith had to be moved to the mesial for proper esthetics. The gingival esthetic line (GAL) describes the agreeable evolution of the zenith from the central to the canine. Class I, where the lateral is 1 mm to 2 mm below the line, is the most pleasing.15 The new zenith was sculpted via a gingivectomy with a #15 scalpel blade.
The third adjustment related to creating a site in the alveolar ridge where tooth No. 7 had been removed to receive an ovate pontic (Figure 12). The ovate pontic is probably the most esthetic pontic because it appears that the pontic is growing out of the ridge like the adjacent teeth. However, an ovate pontic requires that the alveolar ridge is relatively intact in the apico-occlusal and bucco-lingual dimensions. If it is not, then either hard and/or soft tissue grafting is required to restore normal contours or a different pontic, such as a modified ridge lap, will be required, even if it is less esthetic. In this case, the ridge did have normal contours so an ovate pontic was chosen for its superior esthetics and possibility of excellent hygiene. The first step was to scallop the facial gingiva so that the facial gingiva would be at the proper height and contour for the lateral incisor. This is generally at a level that is 0.5 mm to 1 mm more coronal than the height of the gingival margin of the adjacent central incisor. Once this was done, the next step was to create a concave depression in the center of the ridge that was 1 mm to 2 mm apical to the newly created facial gingival margin. This concavity will receive the ovate pontic much as an egg sits in a carton. Finally, it was necessary to sound the bone above the apical base of the concavity. For healthy gingiva to exist between the base of the ovate pontic and the alveolar bone, it is necessary to have a space of 2 mm.
An edentulous area of alveolar bone is always covered by 2 mm of gingiva (1 mm of connective tissue and 1 mm of keratinized epithelium). In this case, creating a concavity for the ovate pontic exposed the underlying alveolar bone. Therefore, after the ovate pontic in the provisional was shaped with acrylic and polished, a round carbide bur was used to create a 2-mm concavity in the alveolar ridge. During the next few weeks, this would granulate in with a healthy gingival covering of the alveolar bone, provided that the 2-mm space was maintained.
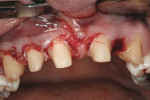
The final step related to raising the midline buccal frenum. In this case, the existing frenum extended very close to the free gingival margin between the two maxillary central incisors and was visible when the patient smiled. This is considered unesthetic. A partial-thickness dissection was used with a #15 blade leaving only the periosteum over the facial portion of the alveolar ridge between the two centrals and extending laterally (the width of the frenum) and apically (approximately 1 cm). The alveolar mucosa can be undermined apically and laterally approximately 5 mm (staying close to the periosteum). No suturing is required. Pressure in the area for 5 minutes with a wet gauze sponge will allow a fibrin clot to form, which will hold the displaced alveolar mucosa in its new location. Some of the displaced mucosa can be excised but this is not absolutely necessary. The provisional bridge was relined and provisionally cemented with Tempbond NE (Kerr Corporation, kerrdental.com) (Figure 13).
Prosthetic Phase
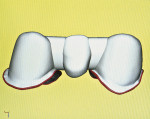
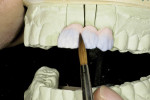
After a healing period of 2 months, a final impression was obtained of the preparations with Reprosil and sent to the laboratory for fabrication of the definitive Lava bridge and crowns. The dies were scanned into the computer at the milling station (Figure 14). The framework and sprueing were designed with the Lava Scan computer (Figure 15 and Figure 16). The final framework created support for the overlying porcelain. Feldspathic porcelain was then built up over the framework (Figure 17).
After receiving the case back from the laboratory and confirming marginal adaptation and occlusion, the restorations were cemented with Fuji-Cem (GC America, https://www.gcamerica.com). The final restoration demonstrates improved esthetics and restoration of anterior guidance (Figure 18, Figure 19, Figure 20, Figure 21).
Discussion
Many patients desire metal-free restorations mainly for esthetic reasons. The development of stronger ceramic core materials has resulted in the increased use of oxide ceramics for shorter all-ceramic bridges.17 With conventional ceramic materials, the distribution of flaws in a particular area, not the thickness of the material, is the main factor contributing to fractures. Yttria-tetragonal zirconia polycrystal (Y-TZP) does not possess a glass phase at the crystalline border. Tensile stress reduces matrix pressure on the tetragonal particles of Y-TZP and shear stress found in the particles results in martensitic transformation. The addition of 3% yttrium oxide as a stabilizing agent allows the sintering of fully tetragonal-phase ceramic to partially stabilized zirconia. When a crack starts to form, high-energy stress is created at the leading edge of the crack. The high energy created in this area causes the change of the tetragonal configuration to a monoclinic formation. Because the monoclinic configuration is 3% to 5% larger, the area where the crack is initiated is placed under compression, which hinders crack propagation. This prevents the opening of cracks and increases the energy required for crack propagation.
Ceramics are also susceptible to subcritical crack growth as a result of water aiding in the breakage of metal oxide bonds at the crack tip while stress is being applied.18 The moisture of the mouth and cyclic loading that occurs during mastication lend themselves to the formation of subcritical crack propagation. This may reduce the effectiveness of the materials’ toughening mechanism and failure may result when no fracture is expected.19 In addition, abutment conditions, such as fixed or mobile, may affect the strength and stress distribution of all-ceramic FPDs.20 A ceramic laminate will always exhibit a constant strain system that results from the mismatch of elastic moduli at the interface between the core and the veneer. This occurs because of wettability factors and trapped air bubbles that often form over the core before firing.21 In addition to existing flaws, small alternating forces taking place all through mastication and the presence of water in a crack tip cause slow, time-dependent growth of cracks.21 The relationship between the inherent strength of all-ceramic restorations, residual and loading stresses, and existing structural flaws and their location is very complex. The fracture mechanisms of all-ceramic restorations include cone cracking, sub-surface quasi-plastic deformation, and radial cracking. The main mechanism of failure of all-ceramic crowns under occlusal load is cone cracking.21
Conclusion
The modifications of function, esthetics, and phonetics have to be carefully planned so that anterior guidance is provided. The relationship between the palatal surfaces of the maxillary anterior teeth and the incisal edges of the mandibular anterior teeth need to be considered.5 The patient had presented with an edge-to-edge occlusion and loss of canine guidance. To allow relaxation of his masseter and pterygoid muscles and reduce forces on his posterior teeth, anterior guidance had to be re-established. The anterior teeth are more sensitive to pressure changes than posterior teeth and anterior teeth serve to suppress the activity of the elevator muscles.22 Although zirconia has become widely used as a restorative material, its long-term clinical use for bridges, especially in patients with parafunction, have to be evaluated.
Acknowledgment
The authors wish to thank Americus Dental Laboratory for fabrication of the restorations.
References
1. McEntire F. Restoring esthetics and anterior guidance in worn anterior teeth. A conservative multidisciplinary approach. J Am Dent Assoc. 2000;31:1279-1283.
2. Serio FG, Strassler HE. Periodontal and other soft tissue considerations in esthetic dentistry. J Esthet Dent. 1989;1(6):177-188.
3. Calamia JR, et al. A multidisciplinary approach to the indirect esthetic treatment of diastemata. Functional Esthetics and Restorative Dentistry. 2007;1(3)8-12.
4. Charruel S, et al. Gingival contour assessment: Clinical diagnosis parameters useful for esthetic diagnosis and treatment. J Periontol. 2008;79:795-801.
5. Brose MO, Tanquist RA. The influence of anterior coupling on mandibular movement. J Prosthet Dent. 1987;57(3):345-353.
6. Kokich VO, Kinzer GA. Managing congenitally missing lateral incisors. Part I: Canine Substitution. J Esthet Restor Dent. 2005;17:5-10.
7. McKusick-Nathans Institute of Genetic Medicine, Johns Hopkins University School of Medicine. Online Mendelian Inheritance in Man.
8. Vastardis H. The genetics of human tooth agenesis: New discoveries for understanding dental anomalies. Am J Orthod Dentofacial Orthop. 2000;117:650-656.
9. Shimizu T, Maeda T. Prevalence and genetic basis of tooth agenesis. Japanese Dental Science Review. 2009;45:52-58.
10. Sabri R. Management of missing maxillary lateral incisors. J Am Dent Assoc. 1999;130:80-84.
11. Priest GF. Esthetic comparison of alternatives for replacement of a single missing tooth. J Esthet Restor Dent. 1996;8(2)58-65.
12. Kinzer GA, Kokich Jr VO. Managing congenitally missing lateral incisors. Part II: tooth-supported restorations. J Esthet Restor Dent. 2005;17(2):76-84.
13. Rinchuse DJ, Rinchuse DJ, Sosovicka MF, et al. Orthodontic treatment of patients using biophosphonates; a report of two cases. Am J Orthod Dentofacial Orthop. 2007:131:321-326.
14. Zahrowsk JJ. Bisphosphonate treatment: An orthodontic concern calling for a proactive approach. Am J Orthod Dentofacial Orthop. 2007;131(3):311-320.
15. Ahmad I. Anterior dental aesthetics: Gingival perspective. British Dent J. 2005;199:195-202.
16. Tarnow D, Magner A, Fletcher P. The effect of the distance from the contact point to the crest of bone in the presence or absence of the interproximal papilla. J Periodontol. 1992; 63:995-996.
17. Vult von Steyern P. All-ceramic fixed partial dentures, studies on aluminum oxide and zirconium based ceramic systems. Sed Dent J Suppl. 2005;173:169.
18. Curtis AR, Wright AJ, Fleming GJP. The influence of surface modification techniques on the performance of Y-TZP dental ceramic. J Dent. 2006;34(5):317-325.
19. Stuardt AR, Filser F, Kocher P, Gaukler IJ. Fatigue of zirconia under cyclic loading in water and its implications for the design of dental bridges. Dent Mater. 2007;23(1):106-114.
20. Luthardt RG, Holzhüter M, Sandkuhl O, et al. Reliability and properties of ground Y-TZp zirconia ceramics. J Dent. 2002;81(7): 487-491.
21. Vult von Steyern P, Carlson P, Nilner. All ceramic fixed partial dentures according to the DC Zirkon technique. A two year clinical study. J Oral Rehabil. 2005;32(3):180-187.
22. Ehrlich J, Yaffe A, Hochman N. Various methods in achieving anterior guidance. J Prosthet Dent. 1989;62:505-509.
About the Authors
Shaloo Sharma, BDS, MDS
Resident
International Program in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Hyang Kyung Kim, DMD, MS, PhD
Resident
International Program in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Kenneth Klonsky, DDS
Clinical Associate Professor, Periodontics
New York University College of Dentistry
New York, New York
Pamela Benito, BDSc
Resident
International Program in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Richard Trushkowsky, DDS
Clinical Associate Professor, Cariology and Comprehensive Care
Associate Director, International Program in Aesthetic Dentistry
New York University College of Dentistry
New York, New York