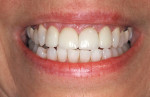
Anterior Implant Esthetics
Esthetic gingival contour transfer in an anterior implant prosthetic case.
David Kurtzman, DDS; Gregori M. Kurtzman, DDS; Lee H. Silverstein, DDS, MS; Peter Shatz, DDS
Anterior implant esthetics—three words that imply numerous and treacherous pitfalls and strike fear into the hearts of restorative dentists. Among the challenges is the accurate and predictable communication of proper final tissue contours to the dental laboratory.1,2 Only with proper communication of the gingival architecture can the laboratory provide a natural-appearing restoration.
Anatomical and esthetic gingival contours make or break the anterior case. A natural, healthy gingival architecture that mimics and blends with natural dentition is not only highly desirable but, in most cases, attainable. With proper placement of the implant body, adequate soft tissue, and a temporary restoration that guides and shapes the tissue into lifelike contours, an implant restoration in the anterior region can appear natural and beautiful.3-5
Placement of the fixture is facilitated by good communication between the restorative dentist and the surgeon and is achieved through accurate surgical guides.5 Proper orientation of the fixture is required in the mesial-distal, buccal-lingual, and occluso-gingival planes. When deficiencies in the hard and/or soft tissue prevent ideal placement of the fixtures, then allografting and autografting techniques may be used to supply abundant soft tissue with which to create esthetic contours.
Once the implant is placed and the tissue has healed, the interproximal papillae and buccal crescent of the gingiva are sculpted with sequential fixed temporaries.6,7 Step-wise addition of temporary material manipulates tissues to place and creates proper esthetic contours. Once accomplished, these contours must be accurately and predictably conveyed to the laboratory.
Enter the custom impression coping. By copying the final contours of the fixed esthetic temporary restoration to an impression coping, gingival tissue is supported in the correct anatomical position during the impression procedure. This prevents tissue collapse during the impression phase and allows accurate communication of the position of the soft tissue.
Case Presentation
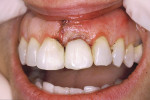
A 55-year-old woman was sent by her surgeon to treatment plan an implant in the edentulous area of tooth No. 9. The space had been occupied by an ill-fitting and unesthetic bonded pontic. The patient desired a more natural and harmonious smile.
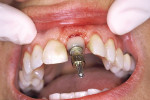
A surgical guide created by the restorative dentist in concert with the surgeon was used to place the implant in proper position. Healing took place over 6 months, at which time the fully integrated fixture was surgically exposed by removing a “plug” of tissue with a surgical trephine. A 5-mm healing abutment was placed and the patient was immediately sent to the restorative dentist to begin tissue manipulation with the temporary restoration.
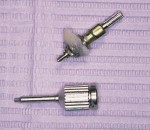
A screw-retained temporary abutment (Biomet 3i, https://www.biomet3i.com) was air-abraded using 50-μm alumina oxide. The roughened temporary abutment was then coated with a bonding agent (Prime & Bond® NT™, DENTSPLY Caulk, https://www.caulk.com) and a hybrid composite resin (Esthet-X®, DENTSPLY Caulk) was added to the screw-retained temporary abutment head to shape the tissue to the desired gingival contours. The supragingival portion was created intraorally with the temporary abutment cylinder screwed into place. Once this was formed, the subgingival portion was created extraorally in the laboratory.
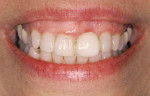
Over a period of several weeks, the temporary was modified by adding and subtracting composite subgingivally until it reached final esthetic contour and the surrounding tissues were in proper position. When these tissues were pink, firm, stable, and healthy, an open impression tray was fabricated (Triad® TranSheet®, DENTSPLY Trubyte, https://trubyte.dentsply.com) (Figure 1 and Figure 2).
It has been noted and documented that once the temporary restoration is removed, the gingival tissues tend to collapse and “slump” rather rapidly over the implant platform. Even a relatively fast impression with a standard impression coping will result in an inaccurate model of proper esthetic gingival contour. While some laboratories may be able to compensate for this by manipulation of the models, it is unpredictable and seldom as esthetically correct as the temporary restoration. The custom impression coping solves this problem.
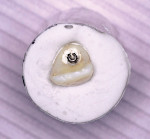
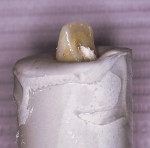
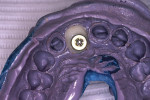
Because the gingival portion of the temporary supports the tissue, this is the area that must be copied. The temporary restoration was secured to an appropriate laboratory analog and the tissue surface was lubricated with Triad model release agent. A quick-set laboratory stone was mixed and placed into a container. The laboratory analog and the attached temporary restoration were inserted to the height of the contour of the restoration and allowed to set (Figure 3 and Figure 4). Once the stone was completely set, the temporary was unscrewed from the analog and removed from the stone. The analog remained at the bottom of a smooth, accurate impression of the contours of the temporary restoration, making a mold to create the custom impression coping.
A “stock” open-tray impression coping was used next to create the custom impression coping. To aid in the adhesion of the custom material to the coping, the end of the coping facing the implant analog was roughed up with a diamond and air-abraded as previously described, avoiding the portion in contact with the analog’s platform, to roughen the temporary abutment (Figure 5). The stone impression was lubricated with model release agent and the impression coping, after being coated with bonding agent (Prime & Bond NT), was screwed onto the implant laboratory analog embedded in the stone mold (Figure 6 and Figure 7). Flowable composite (Flow-It®, Pentron Clinical Technologies, https://www.pentron.com) was carefully injected around the coping into the stone mold and light-cured in layers to ensure complete curing of the resin within the mold (Figure 8). Alternatively, a self-cure resin may be used in place of the flowable composite resin.
Once cured, the coping was unscrewed from the implant analog and removed from the stone mold. The perfect replica of the tissue portion of the temporary was then wiped with alcohol to remove uncured resin in the air-inhibited layer. This replica—the custom impression coping—was ready for the final impression .
After orienting intraorally on the implant after removal of the temporary restoration, the custom impression coping was fixed to the implant via a long impression pin, supporting the soft tissue as the temporary restoration had previously. The tissues, properly supported, regained the desired contours created by the temporary. An open-tray impression using a custom tray (Triad TranSheet,) previously fabricated and filled with a polyether impression material (Impregum™, 3M/ESPE, https://www.3mespe.com) was taken and sent to the laboratory along with an interocclusal bite record using a rigid vinyl polysiloxane bite material (Correct VPS®, Pentron Clinical Technologies) and an opposing model. Additionally, an impression of the temporaries was taken intraorally to aid the laboratory in seeing the desired crown contours and a stick bite to further define the incisal plane and midline.
The laboratory, using the open-tray impression with the custom impression coping, was able to fabricate a soft tissue model. This replicates sulcus dimensions and gingival margin position as developed intraorally, permitting the laboratory to design a restoration that mimicked what had been developed intraorally and provided natural esthetics.
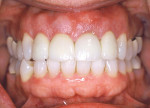
On delivery, the restoration fit precisely and harmoniously with the natural and esthetic contours of the gingiva. The implant-supported restoration was indistinguishable from the adjacent teeth and was a functional and esthetic success. The guesswork as to where the tissue would position after restoration placement was eliminated (Figure 9).
Conclusion
The key to esthetic results with implant-fixed restorations is the communication of the soft tissue position to the laboratory. We work hard to develop the position of the gingival margin and the emergence profile but when impressions are captured, the soft tissue changes position. Tissue collapse occurs as soon as the provisional restoration is removed from the implant fixture.
The methods described herein detail a technique to replicate the soft tissue support and, thus, replicate the gingival margin position developed with the provisional restoration. Thus, the final restoration provides the esthetic results both the practitioner and patient have worked to develop in the provisional phase.
References
1. Sava CN, Kamposiora P, Papavasiliou G, Orfanou AV. Intrasurgical implant position transfer and interim restoration placement. J Prosthodont. 2008;17(8):648-653.
2. Shor A, Schuler R, Goto Y. Indirect implant-supported fixed provisional restoration in the esthetic zone: fabrication technique and treatment workflow. J Esthet Restor Dent. 2008;20(2):82-97.
3. Neale D, Chee WW. Development of implant soft tissue emergence profile: a technique. J Prosthet Dent. 1994;71(4):364-368.
4. Buskin R, Salinas TJ. Transferring emergence profile created from the provisional to the definitive restoration. Pract Proced Aesthet Dent. 1998;10(9):1171- 1180.
5. Elian N, Tabourian G, Jalbout ZN, et al. Accurate transfer of peri-implant soft tissue emergence profile from the provisional crown to the final prosthesis using an emergence profile cast. J Esthet Restor Dent. 2007;19(6):306- 315.
6. Biggs WF, Litvak AL Jr. Immediate provisional restorations to aid in gingival healing and optimal contours for implant patients. J Prosthet Dent. 2001;86(2):177-180.
7. Davarpanah M, Martinez H, Celletti R, Tecucianu JF. Three-stage approach to aesthetic implant restoration: emergence profile concept. Pract Proced Aesthet Dent. 2001;13(9):761- 768.
About the Authors
David Kurtzman, DDS
Private Practice
Marietta, Georgia
Gregori M. Kurtzman, DDS
Private Practice
Silver Spring, Maryland
Lee H. Silverstein, DDS, MS
Associate Clinical Professor of Periodontics
Medical College of Georgia School of Dentistry
Augusta, Georgia
Private Practice
Marietta, Georgia
Peter Shatz, DDS
Private Practice
Marietta, Georgia