Modern Restorative Dentistry: Anterior Application
New restorative protocol uses adhesive bonding resins to restore form and function.
Jeffrey M. Rosenberg, DDS
A new type of dentistry is emerging. This new restorative protocol, called Modern Restorative Dentistry (MRD),1 appears to be minimally invasive but is actually “maximally embracive.” The protocol “embraces” the concept that all good tooth structure should be left during tooth preparation and modern, adhesive bonding resins should be used to restore form and function. Restorative resins are used as a wetting agent for etched enamel to adhere the restoration in a cohesive manner, much the way a porcelain veneer is attached to the tooth.
Technique
The physical and mechanical characteristics of resin-based composites have improved considerably, yet the literature indicates that the same cannot be said for the operative decisions and techniques associated with their insertion and finishing.2
Deciding whether to include enamel pits, fissures, defects, and grooves have been discussed, yet no clear science-based recommendations have been made.3 To eliminate the possibility of posttreatment problems associated with challenging determinations, this author published a protocol for cleaning and pre-etching the enamel surrounding cavity preparations (see Technique Steps on this page). The “pre-etch” technique was developed to help improve final restoration success through better adhesive bonding and sealing, plus removing bacterial biofilm that can be stuck deep in the grooves of what appears to be healthy enamel.4
The “pre-etch” procedure is the starting point for the MRD technique—clean, etched enamel surrounds the restoration. From this “pre-etch” procedure, caries removal is performed, conserving as much dentin as possible. Then, enamel rod alignment is optimized with bevels and chamfers. The prepared enamel is etched and the dentin hybridized using a self-etch primer. The etched enamel is wetted with unfilled resin (uncured), flowable composite is added to the unfilled resin, and composite paste is injected into the resin “sandwich.” Most anterior restorations are single-loaded. In deep gingival or deep axial cases, the author does an increment or two before the injection into the resin “sandwich.” The specific steps for the restorative technique are shown in “Technique Steps.”
Materials
Improvements have been made in the filler and resin compositions of the new composite materials, as well as the emergence of new filler types.2 One company with a long history of high-quality adhesive and resin materials is Kuraray Medical (www.kuraraydental.com). The case presented uses Kuraray’s adhesive bonding agent, Clearfil® Protect Bond, and the new restorative composites Clearfil® Majesty Esthetic and Clearfil® Majesty Flow. The Majesty restorative composites fulfill the requirements for an ideal restorative material for the MDR protocol. Majesty is strong, has high wear rates and minimal shrinkage, and is highly polishable.5,6
Technique Steps
- Teeth are initially marked with articulating paper to evaluate existing contacts, forces, and esthetics.
- Tooth isolation is established; a rubber dam is preferred.
- Initial debris, stain, and marking ink are cleaned with air abrasion (sodium bicarbonate, aluminum oxide, or pumice).
- The clinician may elect to pre-etch4 uncut enamel to create a preventive seal of grooves and an infinite edge margin to finish.
- If interproximal tooth structure is being treated, pre-wedging begins the process of tooth separation, tissue, and rubber dam retraction.
- Tooth preparation includes caries removal (with the aid of caries detectors), chamfers for bulk of materials, and bevels (for esthetics and completely sealed margins).
- Cleaning and disinfection of the preparation is done with flour of pumice and chlorhexidine gluconate, then full-strength sodium hypochlorite for 60 seconds.
- A matrix system is placed as needed for anterior or posterior situations. The matrix is sealed with a wedging system.
- Total-etch or self-etch is applied. Exposed dentin is hybridized for adhesion.
- Unfilled resin is applied but not cured.
- Flowable resin is brushed thin over the entire surface of the restoration to act as a stress breaker as well as to facilitate a sealed and polished margin.
- The paste composite is injected into the preparation, displacing the flowable resin onto all of the margins. For deeper posterior preparations, flowable resin is injected into the gingival proximal and axial areas and cured in a ramp mode or from a distance of 2 inches for 10 seconds initially; then it is cured at full strength.
- The composite is cured through the tooth wherever possible to redirect polymerization forces positively against the enamel of the tooth.
- Finishing is completed by bulk shaping and refinement of the restoration with carbide finishing burs (G- Block™, Garrison Dental Solutions, www.garrisondental.com). Continue finishing with a medium-grit disc (Sof-Lex™ XT, 3M ESPE, www.3mespe.com). Pre-polish with coarse pumice.
- Final polishing with rubber points then diamond/Kevlar brushes: Brownie® silicone point wet and Greenie® silicone point wet (Shofu Dental, www.shofu.com), then Groovy Diamond™ Brushes (Clinician’s Choice, www.clinicianschoice.com).
Anterior Case
This case illustrates how the principles of MRD can be applied to an anterior restoration. The restoration was simple to place, it was done quickly, and it required very little finishing and polishing.
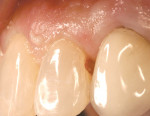
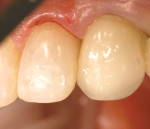
A proximal gingival carious lesion was detected on a maxillary lateral incisor at the hygiene visit of a healthy, 51-year-old woman (Figure 1). The caries risk assessment was determined to be moderate and dietary modifications were made as follows: no nighttime snacking of sugary foods. Nighttime flossing was reinforced.4,7
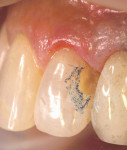
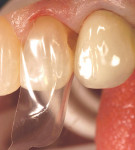
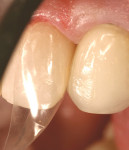
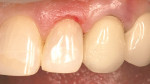
Local anesthesia was obtained, the bite was marked with articulating paper, and a sectional retraction cord was placed. The tooth was pumiced clean and 2 mm of enamel was pre-etched with phosphoric acid within the confines of a dead soft metal strip. Caries removal was aided with high magnification and a caries detector. The enamel was beveled 2 mm to 3 mm surrounding the preparation (in Figure 2, the bevel is colored blue for illustration purposes). A clear anterior matrix (Bioclear, www.bioclearmatrix.com) was placed (Figure 3). The bonding procedure occurred according to the technique, making sure not to cure the unfilled resin on the preparation margins. Majesty Flowable Resin (shade B1) was placed in the matrix but not cured. Majesty Esthetic Resin (shade BL2) was selected to be used in a compule form (Figure 4 ). The paste resin was injected into the uncured flowable resin, displacing it to the periphery of the margins (Figure 5). Curing occurred through the matrix. Very little finishing and polishing was needed (Figure 6). The final restoration was completed in less than 20 minutes (Figure 7).
Conclusion
The current economy challenges us as private practice clinicians to deliver efficient, affordable, yet profitable restorative dentistry. Fortunately, the concepts of MDR8,9 allow us to deliver restorative care in a productive manner with reliable long-term clinical outcomes. Tooth preservation is the goal of MRD and is achieved with protocol that reinforces the restoration cohesively into the tooth.10 This article illustrated MDR concepts using restorative resins and adhesive bonding. Future articles will demonstrate our protocol in other clinical procedures.
References
1. Clark, DC. Is all minimally invasive dentistry better dentistry? Dent Today. 2009;28(5): 98-103.
2. Mazer RB, Leinfelder KF, Russell CM. Degradation of microfilled posterior composite. Dent Mater. 1992;8:185-189.
3. Isenberg BP, Leinfelder KF. Efficacy of beveling posterior composite resin preparations. J Esthet Dent. 1990;270-273.
4. Rosenberg JM. The pre-etch technique. Pract Proced Aesthet Dent. 2004;16(10):764-766.
5. Data on file. Kuraray Medical Inc.
6. Leinfelder KR. Advances in biorestorative materials. What does the future hold? JADA. 2000;131(1):35-41.
7. Petersson GH, Fure S, Twetman S, Bratthall D. Comparing caries risk factors and risk profiles between children and elderly. Swed Dent J. 2004;28(3):119-128.
8. Christensen GJ. Restorative dentistry for times of economic distress. JADA. 2009; 140(2):239-242.
9. Cooper MB. The New Age of Dentistry: Possible Consequences of the Recession. The Newsletter that Makes You Think. January 21, 2009.
10. Opinion Leaders Forum, Modern Restorative Dentistry, Tacoma WA Meeting. August 23, 2008.
About the Author
Jeffrey M.Rosenberg, DDS
Private Practice
The Dental Healthcare Group
Philadelphia, Pennsylvania