A Multidisciplinary Approach
The author outlines how this type of multifaceted approach can be beneficial in a complex restorative–esthetic case.
Aria Irvani, DDS
As the art and science of dentistry advances, there are more tools than ever to treat our patients. Using a multidisciplinary approach, the practitioner can provide the best possible care with minimally invasive dentistry that will ensure the longevity of the restorations and their continued function. Furthermore, this multifaceted approach will allow the patient to benefit from a more comprehensive correction of the problem rather than treating the affected teeth alone. This article presents a case in which the patient was treated using several dental disciplines to achieve both restorative and esthetic objectives.
In the past, given the narrow scope of dental science, patients were treated with whatever the practitioner felt was appropriate or was familiar with at the time. As the saying goes, when all you have is a hammer, everything looks like a nail. For example, up until a few years ago, the routine treatment for severe tetracycline-stained teeth was full-coverage metal-ceramic restorations. Today, the same clinical challenge can be addressed with vital bleaching1 or bonded porcelain laminates in more severe cases. The skilled clinician is no longer limited to one treatment modality.
In a multidisciplinary treatment approach, it is essential that the general dentist be in constant communication with the specialist(s)2 to coordinate appointment or treatment sequence. Sometimes, depending on the skill level, the entire treatment can be accomplished by the general dentist. A vast number of dental conditions can be properly treated with a combination of orthodontics and esthetic dentistry,3 minimizing removal of precious tooth structure. Orthodontic treatment is a vital part of the minimally invasive dentistry philosophy. The case will illustrate how using different disciplines can significantly enhance the treatment outcome and conserve valuable tooth structure along the way.
Case Report
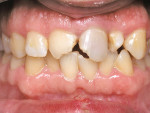
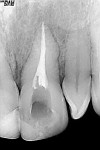
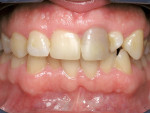
The patient was a 28-year-old man who had a mountain biking accident. The author saw the patient on the first day after the accident. Interestingly enough, there was slight mobility caused by trauma. However, there were two very large incisal-angle fractures on teeth Nos. 8 and 9 and internal pulpal hemorrhaging (Figure 1). Tooth No. 25 had suffered an incisal fracture as well. Because of the extent of the damage and the unknown condition of the pulp4 on tooth No. 8, definitive restorations were postponed. The triage in this case involved root canal therapy on tooth No. 9 (Figure 2) and two very large class IV composite restorations (Figure 3) and another class IV composite on the lower incisor. Tooth No. 8 was tested at every appointment and the pulp tests were normal throughout the course of treatment.
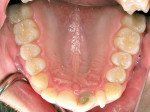
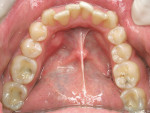
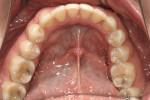
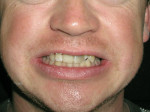
The patient expressed that he had always been conscious of his misaligned and crooked teeth (Figure 4 and Figure 5) and wanted to improve his smile. He stated that this would be the ideal time to take care of the “crooked teeth.” It was determined that the most conservative treatment for teeth Nos. 8 and 9 would be two porcelain laminates instead of full-coverage crowns to conserve as much tooth structure as possible.5 Porcelain laminates were a viable option because of their proven track record.6,7 Because of the translucent nature of the laminates, the author decided to perform internal bleaching8 on tooth No. 8. This allowed him to significantly alter the stump shade so that a more conservative preparation could be performed. The author was not concerned about an exact match because both centrals would later be covered with laminates and any small discrepancy would be corrected with the restorations themselves.
To bleach the discolored tooth, the walking bleach or internal bleach method was used. The gutta-percha root canal filling material was removed to 2 mm below the cementoenamel junction of the tooth9 (Figure 2). Then a 1-mm layer of GC Fuji II LC (GC America, www.gcamerica.com) was placed to seal off the rest of the root and prevent any apical leakage. Next, a mixture of sodium perborate and superoxol were placed in the chamber and sealed using composite without etchant or bonding agent for easier removal. This dressing was changed every 3 days for the next 9 days until the desired shade was achieved. The access hole was then permanently sealed with an etched and bonded composite restoration using a very opaque shade of Vit-l-escence OS White (Ultradent Products, Inc, www.ultradent.com). The author determined that the class IV composites would suffice until the definitive laminates were placed. The patient was ecstatic about not having temporary veneers or crowns.
The next step was to correct the alignment of the teeth by orthodontic movement to facilitate the final restorative and esthetic objectives.10 This allowed the teeth to be placed in an ideal arch form, eliminating the need for excessive reduction of teeth to correct misalignments. Furthermore, this orthodontic phase would allow the teeth to have proper protrusive and excursive relationships reducing uneven wear of the dentition. This approach would produce significantly better-proportioned teeth.11
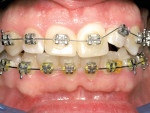
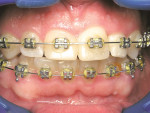
The patient was classified as having a class I malocclusion with significant crowding on the maxillary incisors. Both upper and lower teeth were bracketed and a very light 0.014 nickel-titanium (NiTi) wire was used on both arches to start leveling, aligning, and rotating teeth.
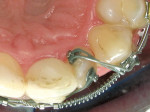
By far, the biggest challenge was tooth No. 10 with a 90° rotation12 (Figure 4). Because a rotated tooth takes up less space, the first step was to create enough space between teeth Nos. 9 and 11 with the use of NiTi coil springs to make room to de-rotate tooth No. 10 (Figure 6 and Figure 7). Next, two buttons were bonded on the buccal and lingual of tooth No. 10 along with elastic chains to exert reciprocal rotational force on the tooth expediting movement (Figure 7). This process took approximately 3 months. Once the tooth was de-rotated, a very light 0.012 NiTi wire was used to bring the tooth down into the arch (Figure 8). In recent years the concept of using lighter forces has gained popularity in orthodontics because it produces faster results with less discomfort to the patient.13
Interestingly enough, the same initial wire placed on the lower arch provided all the alignment necessary for the lower teeth. The final wire on both arches was a 0.019 x 0.025 stainless steel that provided the final root torque. The teeth were left in retention for approximately 6 months (Figure 9). At the end of the treatment, the upper and lower arches were nicely aligned and the crowding and rotations had been eliminated (Figure 10 and Figure 11). Adequate attention to post-orthodontic retention is of paramount importance.14 The last step was permanent restorations on teeth. After removal of the brackets, teeth Nos. 8 and 9 were prepared the same day for porcelain laminates. The composite restorations that had been placed earlier were treated the same way as the tooth structure and prepared as if they were part of the tooth. The preparations were then temporized using Venus® (Heraeus Kulzer, Inc, Armonk, NY) bis-Acryl provisional material. An impression of the arch with provisional restorations was made and an in-office, vacuum-formed Essix retainer (DENTSPLY Raintree Essix, www.dentsply.com) was fabricated to serve as an interim retainer until the definitive restorations were placed.
The patient returned to our office 2 weeks later, at which time the provisionals were removed, the restorations were tried in and, after obtaining the patient’s approval, were bonded in place using the total-etch technique (Figure 14).15 Two sets of impressions were taken after the veneers were cemented. One set was used to fabricate another in-office, vacuum-formed Essix interim retainer until a more definitive retainer was completed at the laboratory, and the second set was sent to the laboratory so that a Hawley appliance could be fabricated to retain the patient’s teeth in the proper position. The patient was instructed to wear the retainer night and day (except when eating) for 3 months after the completion of treatment. He was instructed to wear the retainer at nights only after the initial 3-month wear, and he was educated about the need for lifetime retention.
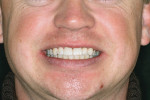
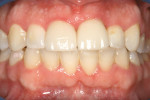
The final results (Figure 12 and Figure 13) show the dramatic improvement in the patient’s smile. The accident was the catalyst in the patient’s decision to improve his dental health and his smile but, more importantly, using a combination of treatment modalities allowed the author to treat the patient in a minimally invasive manner, not only treating the dental problem but also addressing his esthetic concerns. This method of treatment will frequently take longer to perform and is clinically more challenging, but in the end, the results are significantly superior because there is less removal of the tooth structure and fewer restorations are placed.16 As everyone knows, even the best of restorations have a finite service life and at some point they require replacement. This patient admitted to contemplating porcelain laminates on eight of his anterior teeth as “instant orthodontics” to treat his problem because a co-worker had suggested it. And although the thought of being in braces and delayed gratification was not appealing to him at first, upon completion of his treatment, he stated that he was extremely happy with his choice of treatment.
Contrary to popular belief, multidisciplinary dentistry is not limited to large, complex cases. A thorough understanding of the materials and their limitations is essential in achieving predictable results.17 In fact, if properly treatment planned and performed, the vast majority of our patients can significantly benefit from this approach for more functional and longer-lasting results (Figure 14).
References
1. Haywood VB. Frequently asked questions about bleaching. Compend Contin Educ Dent. 2003;24:324-337.
2. Rajendra J. Clear communications between GDP and specialists. Br Dent J. 2003;195:383.
3. Lowe E, Rego J, Rego N. Minimally invasive dentistry combining orthodontic therapy and single-unit restoration. Pract Proced Aesthet Dent. 2008;20(5):273-278.
4. Bahar Özçel'ik, Tülin Kuraner, Banu Kend'ir and Esin Asan. Histopathological evaluation of the dental pulps in crown-fractured teeth. J Endod. 2000;6:271-273.
5. Andreasen FM, Flugge E, Duagaard-Jensen J, et al. Endod Dent Traumatol. 1992;8: 30-35.
6. A prospective ten-year clinical trial of porcelain veneers. J Adhes Dent. 2004;6(1): 65-76.
7. Calamia J, Calamia C. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 51(2):399-417.
8. Five-year follow-up of internal bleaching. Braz Dent J. 1999;10(2):105-110.
9. Sealing evaluation of the cervical base in intracoronal bleaching. Dent Traumatol. 2003;19(6):309-313.
10. Hancher PJ. Orthodontics for esthetic dentistry: the use of orthodontics to facilitate the restoration of anterior teeth. J Cosmetic Dent. 2005;20(4):74-80.
11. Sarver DM. Principles of cosmetic dentistry in orthodontics. Part 1: Shape and proportionality of anterior teeth. Am J Orthod Dentofac Orthop. 2004;126(6):749-753.
12. Experimental evaluation of initial tooth displacement, center of resistance and center of rotation under the influence of an orthodontic force. Am J Orthod Dentofac Orthop. 2001;120(2):190-197.
13. Kohno T, Matsumoto Y, Kanno Z, et al. Experimental tooth movement under light orthodontic forces: rates of tooth movement and changes of the periodontium. J Orthod. 2002;29(20):129-136.
14. Blake M, Garvey T. Rationale for retention following orthodontic treatment. J Can Dent Assoc. 1998;64:640-643.
15. Porcelain veneers bonded to tooth structure: an ultra-morphological FE-SEM examination of the adhesive interface. Dent Mater. 1999;15(2):105-119.
16. Spear F. The esthetic correction of anterior dental mal-alignment conventional vs. instant (restorative) orthodontics. J Calif Dent Assoc. 2004;32(2):133-141.
17. Castelnuovo J, Tjan A, Phillips K, et al. Fracture load and mode of failure of ceramic veneers with different preparations. J Calif Dent Assoc. 2004;32(2):167-177.
About the Author
Aria Irvani, DDS
Private Practice
Lake Forest, California