Backrests, Armrests, No Rests
What Does the Research Say?
From an ergonomic standpoint, your operator stool is the most important chair in the treatment room. Patients come and go, but you are there throughout the day, so proper and safe positioning of your body should be paramount. Poor fit or adjustment of the stool can lead to low back, neck, or shoulder pain. Naturally, the stool should adjust to support your body in neutral posture, but with the wide variety of body sizes and heights among dentists, certain stool types will fit you better than others.
When it comes to the selection process, the vast array of designs and features on the market today can make it a perplexing project. Numerous features must be considered and evaluated for their fit to your particular body type. These include cylinder height, seat contour, armrests, seat depth, tilt, backrest, wheel casters, and stool style. Of these, the two most poorly understood ergonomic features are the backrest and armrest—and understandably so. Dental stool models claiming to be “ergonomic” run the gamut from backrests with armrests, to backrests without armrests, to armrests without backrests, to no backrests and no armrests. To add to the conundrum, there is a dearth of dental studies regarding the benefits (or lack thereof) of these two features on the health of the dentist. But what is certain from the literature is that these features definitely have an impact on your health, so they deserve more in-depth evaluation.
The Backrest
A primary function of the backrest is to help maintain the lumbar lordosis in sitting by maintaining contact with a convexity on the backrest called the lumbar support.1,2 This is an especially important feature with a non-tilting seat pan, which tends to flatten the low back curve. When the lumbar curve is allowed to flex (as in slouching), the iliolumbar ligaments and other dorsal soft structures are strained and weakened, predisposing them to injury.2-5 Slouching also disengages the posterior vertebral facets, which play a primary role in supporting the spine when standing. When these are disengaged, the load is transferred to the spinal disc. The disc nucleus is then pushed backward, and can eventually result in a disc bulge or herniation.6 Some secondary benefits of the lumbar support are to reduce lumbar disc pressure, decrease low back and referred leg pain, reduce forward head posture, and decrease muscle activity (rest the back muscles).7-10
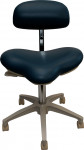
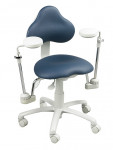
The lumbar support portion of your backrest should be convex from top to bottom to conform to the natural lordosis of your low back. It is the portion that supports your low-back curve and need only be eight inches or so in height to provide adequate support (Figure 1 and Figure 2 ). Many dental stools have no recognizable lumbar support at all. The prominence of the lumbar support can impact disc pressure. Sizes between 1 cm and 5 cm in thickness have been evaluated, with the largest benefits gained from the larger (3 cm to 5 cm) thickness.7,11 Very large backrests should be carefully evaluated to ensure adequate convexity of the lumbar support to properly support the low back and also ensure that the upper portion of a large backrest does not push the thoracic spine forward. [Note: Use of a prominent lumbar support can worsen pain symptoms among patients with spinal stenosis or spondylolisthesis.]
Because of the nature of their work, dentists cannot always maintain contact with the lumbar support of the stool and intermittently must lean slightly forward to view the tooth surface. Spinal disc pressure is highest in this type of anterior sitting,11 which is why it is imperative that the dentist learn to properly stabilize and protect their low back with their internal core stabilizing muscles (primarily the transverse abdominal muscles) whenever they leave the backrest of the stool. When properly used, these muscles have been shown to reduce low back pain.12 An excerpt from the author’s book, Practice Dentistry Pain-Free: Evidence-Based Strategies to Prevent Pain and Extend Your Career, describes how to use these muscles in the operatory to prevent low back pain whenever you lean forward. The exercise stabilizes and protects the lumbar spine by engaging your “internal backbelt.”
Shorter dentists may find that seat pans that are too deep inhibit contact with the backrest. In these cases, a shorter-style seat pan should be considered. Finally, because lumbar disc pressure is lower in standing than in unsupported sitting, dentists should also try to stand periodically when resting against the backrest is not possible.7
The backrest should adjust up and down, as well as toward and away from the dentist’s back. Although studies show that the lowest lumbar disc pressure and muscle activity is with the backrest reclined to about 110° to 120°, it is not possible to practice dentistry in this position.7,11 In occupations where upright posture is necessitated, sitting with the thighs sloping slightly downward can help minimize disc pressure and muscle activity. Because static seated postures should be avoided, it may be beneficial to readjust the backrest and seat pan tilt periodically to move the work load from tissue to tissue to minimize microtrauma.11,13
The shape of the backrest is an especially important consideration. A tall backrest that extends above the lower edge of the scapulae can minimize the benefits of the lumbar support by exerting pressure on the shoulder blades, and should, at its highest point, be 6 cm below the lower edge of the scapulae.2 Because the ribcage is a rigid structure, back support above the lower edge of the shoulder blade is unnecessary, and in dentistry it can inhibit shoulder movement. Wide backrests should be avoided because these can inhibit spinal movement and lateral movement of the arms and shoulders, which is especially important in the prevention of low back pain syndromes.6
No Backrest
Operators often ask why some stools (primarily saddle-style stools) are considered ergonomic when they have no backrest. When you are sitting in a horse saddle, your pelvis (the foundation of your seated posture), is in a near-neutral position, as in standing. This pelvic position allows your spinal curves to balance more easily in proper alignment and reduces muscle strain which is why backrests are considered optional on saddle stools. By design, saddle stools will place more compression on the peritoneal area, and should be carefully evaluated for suitability to the operator.
Armrests
Studies support the use of armrests in the prevention of neck, shoulder, and low back pain.7,14-16 Armrests have been shown to decrease muscle activity in the neck and shoulders of dentists, especially in the upper trapezius on the handpiece, or dominant side.15 Elbow rests also reduce activity in the rhomboid, and thoracic and cervical erector spinae muscles.14
There are several styles of armrests on the market today: fixed but movable, swiveling, pivoting, and telescoping armrests. Armrests should be highly adjustable to provide support to the operator in a neutral working posture.6 Different styles tend to be more appropriate for different team members. So which style of armrest is right for you? Because dentists tend to work in one position longer than hygienists, fixed, movable armrests are preferred by many dentists, especially endodontists. This type of armrest system is highly adjustable in multiple directions: width, height, forward/backward, and the armrest itself tilts for optimal hand positioning (Figure 3). Once the desired position is found, the knobs can be tightened to secure the settings. Swiveling armrests (Figure 4) move freely with the operator, which many dentists find favorable. One drawback may be if the armrests swivel too freely, the operator cannot find it when they need it. A very popular and effective style among general dentists is the telescoping/hydraulic armrest which moves in/out and forward/backward with the operator and can be set at a specific height and resistance (Figure 5). A pivoting, movable armrest (Figure 6) uses a small circular pad on the armrest, which moves with the operator.
Proper adjustment of the armrests is essential in preventing neck and shoulder problems. Adjusting the armrests too high can actually worsen neck pain, as it puts the levator scapulae muscle on slack and can cause neck stiffness and pain at the crook of the neck and shoulder. Muscle activity is lowest when the elbow rests are set slightly low. Proper width adjustment (between armrests) is also important, as armrests set too far apart will cause abduction of your arms. Positioning the armrests too far forward can encourage the dentist to lean forward, compromising operator posture.
From an ergonomic standpoint, it is desirable to operate with two armrests; however, if you have a confined operatory space and find it difficult to maneuver a chair with armrests around the patient, you may want to consider a unilateral armrest fixed to a counter.17 Dentists who operate with the left arm resting have been shown to have less pain than those who do not.18 These are available in a variety of heights to adjust to multiple users and situations.
Conclusion
To be clear, armrests are not an automatic solution for all operators with neck pain. Depending upon the etiology of your pain, taking the arm weight off your neck and shoulders may or may not reduce your symptoms. During in-office consultations, the author performs a specific physical therapy test to determine if individuals with neck pain would benefit from armrests.
Dentists should always request trialing a stool for 1 to 2 weeks before purchasing it to evaluate the comfort and benefits of the armrest, backrest, and other features. Consider alternating between a stool with armrests and backrest and a different style type stool in another operatory to prevent overworking one area of the body. However you choose to do it, it pays to give your muscles a rest.
Pivot Exercise
Even dental operators can benefit from strengthening their core muscles; proper use of these muscles in the operatory can help prevent low back pain.
- Sit tall on the stool with a slight curve in the low back.
- Assume an operating position with the arms.
- To activate the transverse abdominal muscle, exhale, and actively (with your muscles) pull your navel toward your spine. (One common mistake is to suck in one’s breath to pull the spine toward the navel. You should still be able to talk, breathe, and move while holding this contraction.) An alternate method which uses all three abdominal wall layers is to “brace” with the abdominal muscles, as though preparing for someone to hit you in the stomach.
- Using the hips as a fulcrum, pivot forward from the hips, maintaining the abdominal contraction throughout the exercise.
References
1. Carcone SM, Keir PJ. Effects of backrest design on biomechanics and comfort during seated work. Appl Ergon. 2007;38(6):755-764.
2. Snijders DJ, Hermans PF, Nieseing R, et al. The influence of slouching and lumbar support on iliolumbar ligaments, intervertebral discs and sacroiliac joints. Clin Biomech. 2004;19(4):323-329.
3. Adams MA, Dolan P. Time-dependent changes in the lumbar spine’s resistance to bending. Clin Biomech. 1996;11:194-200.
4. Fujiwara A, Tamai K. Yoshida H, et al. Anatomy of the iliolumbar ligament. Clin Orthop Relat Res. 2000;380:167-172.
5. McGill SM, Brown S. Creep response of the lumbar spine to prolonged full flexion. Clin Biomech. 1992;7:43-46.
6. Karwowski W, Marras W. The Occupational Ergonomics Handbook. Florida: CRC Press LLC; 1999:185-86, 1767-1768.
7. Chaffin D, Andersson G, Martin B. Occupational Biomechanics. 3rd ed. New York: John Wiley & Sons Inc; 1999:364-382.
8. Williams MM, Hawley JA, McKenzie RA, Wijmem PM. A comparison of the effects of two sitting postures on back and referred pain. Spine. 1991;16:1185-1191.
9. Majeske C, Buchanan C. Quantitative description of two sitting postures with and without a lumbar support pillow. Phys Ther. 1984;64:1531-1533.
10. Hardage JL, Gildersleeve JR, Rugh JD. Clinical work posture for the dentist; an electromyographic study. JADA. 1983;107:937-939.
11. Harrison DD, Harrison SO, Croft AC, et al. Sitting biomechanics part 1: Review of the literature. J Manipulative Physiol Ther. 1999;22(9):594-609.
12. Richardson C, Jull G, Hodges P, Hides J. Therapeutic exercise for spinal segmental stabilization in low back pain. London, England: J Churchill Livingstone; 1999:4-5.
13. McGill SM. Low back disorders—evidence-based prevention and rehabilitation. Champaign, Ill: Human Kinetics; 2002:175-177.
14. Schuldt K. On neck muscle activity and load reduction in sitting postures. An electromyographic and biomechanical study with applications in ergonomics and rehabilitation. Scand J Rehab Med Suppl. 1988;19:1-49.
15. Parsell DE, Weber MD, Anderson BC, Cobb GW. Evaluation of ergonomic dental stools through clinical simulation. Gen Dent. July/August 2000;440-444.
16. Andersson BJG, Ortengren R, Nachemson A, Elfstrom G. Lumbar disc pressure and myoelectric back muscle activity during sitting II. Studies on an office chair. Scand J Rehabil Med. 1974;6:115-121.
17. Valachi B. Practice Dentistry Pain-Free: Evidence-Based Strategies to Prevent Pain and Extend Your Career. Portland, Ore: Posturedontics Press; 2008:70.
18. Rundcrantz B, Johnsson B, Moritz U. Cervical pain and discomfort among dentists. Epidemiological, clinical and therapeutic aspects. Swedish Dental Journal. 1990;14:71-80.
About the Author
Ms. Valachi is a physical therapist, dental ergonomic consultant, and author of “Practice Dentistry Pain-Free.” She is CEO of Posturedontics® and is also a clinical instructor of ergonomics at Oregon Health Sciences University School of Dentistry in Portland, Oregon. She can be reached at her website, www.posturedontics.com, or by e-mail, bethany@posturedontics.com.