Mix Disease: Diagnosis and Treatment
V. Kim Kutsch, DMD; Carri Cady, RDH
Medication-induced xerostomia (MIX disease, an acronym first introduced by Edwin Zinman) is becoming a more common problem for Americans. There are many potential causes of xerostomia, or dry mouth, and these causes include loss of saliva production as part of the natural aging process,1 Sjögren’s syndrome,2 radiation to the head and neck,3 and medication-induced xerostomia.4 There are now about 3,000 prescription medications that list xerostomia as a possible side effect,5 but drug companies, by and large, have not included specific labeling to alert the consumer about xerostomia and its increased risk for dental caries.6 MIX disease affects people of all ages. The average person has no idea what xerostomia is, so the current drug labeling has little or no significance for them.
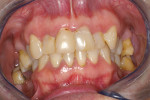
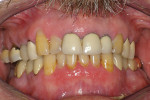
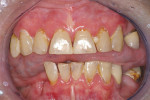
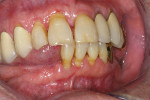
Xerostomia or dry mouth is a condition where the patient hasinsufficient saliva flowto maintain oral health. Symptoms may rangefrom irritation, inflammation, and/or recession of the soft tissues to rapid carious destruction ofthe hard tissues. Othersigns and symptoms include candidiasis and burning mouth syndrome. This is a condition becoming more problematic as people are livinglonger and frequentlytaking multiple medications. It is not unusualin a healthy patient for saliva to naturallydecrease during the aging process. Mouth breathing, particularly when sleeping because the saliva flow decreases, also will lead to dry-mouth symptoms for some patients (Figure 1). Patients with sleep apnea and using a continuous positive airwaypressure (CPAP) device may experiencexerostomia. Other causesfor xerostomia are post-radiation therapy that affects the major salivary glands (Figure 2) and Sjögren’s syndrome, which is an autoimmune disease that affects saliva flow (Figure 3). However, the most common cause of xerostomiatoday is medication-induced (Figure 4).
Many drugs list xerostomia as a potential side effect. The most common classes of xerostomic medications include antihistamines,antihypertensives, and methamphetamines,but many drugs commonly contribute to dry mouth, and the multiple-drug combinations that many patientsare taking compounds the problem. Thiscondition is prevalent in many senior patientsbut also is being seen in children taking antihistamines for asthma, antidepressants, and behavioralmodification drugs forattention deficit disorder.7 It is also common for patients experiencing dry mouth conditions to suck on hard candy to stimulate saliva flow. The continuous exposure to sugar, resulting in continuous periods of acidic pH in the mouth, can have disastrous effects on the dentition of a person with inadequate saliva.
A frequent and serious side effect of MIX disease is dental caries.8,9 The selection pressure in the biofilm for the acidogenic/aciduric bacteria responsible for caries is not sugar availability but rather protracted periods of low pH.10,11 In defense, the body has several protective mechanisms to maintain a near-neutral pH and maintain the calcium phosphate mineral level in the teeth and to prevent the microbial shift from healthy bacteria to acidogenic/aciduric bacteria.12,13 The saliva, however, is the best adaptation for controlling pH as it contains a buffering system that helps to maintain a healthy range of pH in the mouth.14 For patients with xerostomia or MIX disease, the lack of saliva reduces the body’s ability to buffer the acidic conditions, and selection pressure for the acidogenic/aciduric bacteria occurs, which results in dental caries.15,16 It is important to note that the cause of dental caries is not a lack of calcium and phosphate mineral or fluoride, but rather an inability for the dental biofilm to maintain neutral pH conditions.17
A good place to start in any caries risk assessment is with a simple validated caries risk assessment form. Ask the patient if they feelthat they have a “dry mouth” or are taking medications known to cause xerostomia.18 (Many patients with xerostomia actually self-diagnose the condition.) Stimulated saliva flow can be measured by having the patient chew on soft wax and spit into a cup for 5 minutes. Average saliva flow should be about 1 mL of saliva created per minute. Less than 0.7 mL of saliva produced per minute is a sign of xerostomia. A review of the medications thatthe patient is taking will reveal the extent of MIX in the patient’s condition.
Recently, Takahashi and Nyvad19 demonstrated that even bacterial species previously considered commensal are capable of adapting to acidic conditions and becoming causative organisms in dental caries. These include Streptococcus gordonii, S oralis, S mitis, and S anginosus, which they termed low-pH, non-mutans streptococci, in addition to the Actinomyces species.19 Dental caries is now a disease not so much based on which specific bacteria are present, but rather what those bacteria are doing. Their recommendation for treatment strategies included good oral hygiene, effective dietary counseling, and then neutralizing strategies for the biofilm.19 The goal is not only to help neutralize the biofilm and select for healthy bacteria, but also not to cause the low-pH, non-mutans streptococci and Actinomyces species (commensal) to behave badly. For the patient with MIX disease, important treatment strategies might include a saliva-stimulating drug, use of possible saliva substitutes, staying hydrated, and the importance of plaque control and healthy diets, and the daily use of oral care products that neutralize the mouth and keep the pH within healthy ranges. Effective neutralizing products are available in gels, rinses, sprays, gums with combinations of fluoride, xylitol, and neutralizing and buffering agents. 20
For the patient taking medications that result inxerostomia, it is important to alleviate theimmediate discomfort associated with dry mouth and also to educate themabout the potential for dental caries andpotential loss of their teeth. Practitionersmust create individual treatment strategiesbased on the patient’s needs and desires with the goal of creating a healthy pH balance in the mouth. It is incumbent upon the drug manufacturers to clearly label any potential for xerostomia, what that means in lay terms, and thepossibility of severe dental caries with the potential for tooth loss.
Dr. Kutsch is the CEO and founder of CariFree/Oral BioTech, and is a stockholder in the company.
References
1. Gonsalves WC, Wrightson AS, Henry RG. Common oral conditions in older persons. Am Fam Physician. 2008;78(7):845-852.
2. Margaix-Munoz M, Bagan JV, Poveda R, et al. Sjögren’s syndrome of the oral cavity, review and update. Med Oral Path Oral Cir Bucal. March 20, 2009 (epub ahead of print).
3. Marzi S, Iaccarino G, Pasciuti K, et al. Analysis of salivary flow and dose-volume modeling of complication incidence in patients with head-and-neck cancer receiving intensity-modulated radiotherapy. Int J Radiat Oncol Biol Phys. 2009;15: 73(4): 1252-1259.
4. Gallagher L, Naidoo P. Prescription drugs and their effects on swallowing. Dysphagia. December 16, 2008 (epub ahead of print).
5. Oral Biotech. Medications that may cause dry mouth. Available at: https://www.carifree.com/media/Dry%20Mouth%20Medications.pdf. Accessed March 2009.
6. Cassolato SF, Turnbull RS. Xerostomia: clinical aspects and treatment. Gerodontology. 2003;20(2):64-77.
7. Wu AC, Tantisira L, Li L, et al. Repeatability of response to asthma medications. J Allergy Clin Immunol. 2009;23(2): 385-390.
8. Daniels TE. Evaluation, differential diagnosis, and treatment of xerostomia. J Rheumatol. 2000;61(6 Suppl):6-10.
9. Marsh PD. Dental plaque as a biofilm and a microbial community-implications for health and disease. BMC Oral Health. 2006; 6(Suppl 1):S14.
10. Marsh PD, Bradshaw DJ, McKee AS. Effects of carbohydrate pulses and pH on population shifts within oral microbial communities in vitro. J Dent Res. 1989;68: 1298-1302.
11. Alice CL, Harty DWS, Jaques AJ. Stress-responsive proteins are upregulated in Streptococcus mutans during acid tolerance. Microbiol.2004:150;1339-1351.
12. Kleinberg I. A mixed-bacteria ecological approach to understanding the role of bacteria in dental caries causation: an alternative to Streptococcus mutans and the specific plaque hypothesis. Crit Rev Oral Biol Med. 2002;13:108-125.
13. Nascimento MM, Gordan VV, Garvan CW, et al. Correlations of oral bacterial arginine and urea catabolism with caries experience. Oral Microbial Immunol. 2009;24(2): 85-89.
14. Wilson M. Microbial Inhabitants of Humans. Cambridge Press Publishers. 2005;339-352.
15. Coogan MM, Mackeown JM, Galpin JS, Fatti LP. Microbiological impression of teeth, saliva and dietary fibre can predict caries activity. J Dent. 2008;36(11):892-899.
16. Mungia R, Cano SM, Johnson DA, et al. Interaction of age and specific saliva component output on caries. Aging Clin Exp Res. 2008;20(6): 503-508.
17. Featherstone JD. The caries balance: the basis for caries management by risk assessment. Oral Health Prev Dent. 2004; 2(Suppl 1):259-264.
18. Fox PC. Xerostomia: recognition and management. Dent Assist. 2008;77(5):44-48.
19. Takahashi N, Nyvad B. Caries ecology revisited: microbial dynamics and the caries process. Caries Res. 2008;42(6):409-418.
20. Internal data on file. Available at: www.carifree.com. Accessed April 20, 2009.
About the Authors
V. Kim Kutsch, DMD
Private Practice
Albany, Oregon
Carri Cady, RDH
Private Practice
Albany, Oregon