Using Computerized Occlusal Analysis
Alvin W. Neff, DDS
The interpretation of articulating marks has long been an inexact science.1,2 It requires subjective analysis with possible iatrogenic consequences. This protocol has led dentists to make irreversible adjustments to human anatomy without measuring and analyzing the existing problems and hopeful outcomes. Dentists have been taught to ask patients questions: How does that feel? Do you notice any one tooth hitting too much? Which tooth do you feel is touching first?
But patients are not trained in occlusion, and the literature supports that this method can be unreliable.3 Even experienced dentists cannot direct occlusal adjustments by proprioception alone. Therefore, dentists should consult the literature and question further the theories they were taught in dental school and textbooks regarding articulating paper.4,5 It has been documented in the literature that articulating paper is a poor indicator of occlusal disharmony.1,2,6 Studies show that mark size varies with the same applied load or different thicknesses of paper. Mark interpretation is operator-subjective and paper cannot measure the timing or forces of occlusion.1,2,3,6 A complete occlusal adjustment by today’s standards should include computerized occlusal analysis.
This author has used computerized occlusal analysis instrumentation (T-Scan® III, Tekscan Inc, South Boston, MA) for several years as a more accurate way to refine occlusion.7-9 Despite its proven force reproduction capability,10 this technology has been underused in the profession. In the author’s opinion, it is the only accurate way of measuring the timing sequence or force of occlusal contacts.11 It can be used with any occlusal philosophy to determine interocclusal relationships. Instrumentation to analyze occlusal forces was introduced by Tekscan Inc in 1984 as the T-Scan® I.12 Over the past 24 years, the technology has evolved into a very precise diagnostic and treatment tool, which can be incorporated into any restorative practice.
A Paradigm Shift
In dental school, most dentists were taught to adjust the large, dark paper markings. They also were taught to avoid adjustment of the small scratchlike markings, which were believed to be artifacts or false markings. This philosophy has been disproved by computerized analysis. In fact, the reality is the exact opposite: The areas with the highest force are usually the smaller pinpoint or scratchlike markings.13 Adjustments made using the older, dental school philosophy may actually make things worse. A law of physics helps to make this paradigm shift crystal clear: Pressure = Force/Surface Area.
Forces are inversely proportionate to the surface area over which they are distributed. A large area of surface contact distributes the load more evenly than a small pinpoint-sized area. Pinpoint-sized markings will often exhibit the highest forces. This law clearly can be better understood using an analogy; “dancing with a woman in high heels or tennis shoes.” If the high heel (smaller pinpoint-sized surface area) steps on your foot, it will hurt. If the tennis shoe (larger surface area) steps on your foot, the forces will be distributed and result in a lower, less painful force. With this law of physics in mind, dentists must be attentive to the small markings that may represent the areas with the highest forces of occlusion. Dentists, as healthcare professionals, should use all existing technology to provide a better standard of care. Using this scientific approach and the T-Scan III system to analyze occlusal forces can help to avoid arbitrary, irreversible, and possible iatrogenic adjustments.
Clinical Examples
This article details three clinical scenarios where computerized occlusal analysis was used to solve existing problems and prevent potential future problems.
1. Esthetic all-ceramic restorations are at a high risk of fracture with undetected heavy occlusal forces. Precise adjustments were made postcementation.
2. Implant restorations fail catastrophically with accompanying vertical bone loss secondary to heavy occlusal and/or lateral forces.14 Computerized analysis allowed occlusal contact to be delayed purposefully and occlusal loads to be minimized on the restorations.15,16
3. Symptomatic teeth often require endodontic therapy or develop cracks or abfractions.17 The symptomatic teeth were isolated and adjusted easily to eliminate the noxious heavy force.
Case 1: All-Ceramic Restorations
The popularity of all-ceramic bonded restorations has led to a change in clinical protocols for adjusting occlusion.18 Gone are the days of bisque-bake try-ins, occlusal refinement, and reglazing. Today’s materials require occlusal adjustments to be made after insertion. This major shift in clinical technique makes it of paramount importance to adjust and polish the restorations accurately; porcelain cannot be added back to over-adjusted restorations. The strength of all-ceramic restorations has improved, yet porcelain fractures are still too prevalent. These fractures are caused largely by heavy occlusal forces. Through the use of computerized occlusal analysis, dentists can eliminate the guesswork of occlusal adjustment and limit the possibility of future porcelain fracture.18
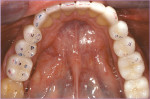
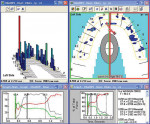
During the postcementation adjustments of a full-mouth reconstruction using all-ceramic restorations, the patient complained about the left side “feeling high.” He wanted teeth Nos. 19 and 20 adjusted. The articulating paper marked several contacts on the left side (Figure 1a), but the T-Scan III showed that 60% of the force (right/left) was on the right side (Figure 1b). Tooth No. 11 was the only heavy contact on the left side that required correction. Adjustments directed by patient proprioception to the posterior left quadrant would have imbalanced the occlusion even more than 60% right to 40% left, possibly leading to fractures of porcelain or joint symptoms.
Case 2: Implant Restorations
Implant dentistry is commonplace these days, and its continued growth presents a unique challenge to the profession. An early prematurity or heavy occlusal force on an implant restoration can result in catastrophic failure (ie, vertical bone loss, porcelain fracture, eventual loss of implant).19,20 Many dentists resort to leaving these restorations completely out of occlusion to avoid potential problems. However, dentists should question why they are placing implants if they do not function properly, as well as be concerned about the supraeruption of opposing teeth. It is ideal to delay the forces of occlusion to the implant slightly until the adjacent teeth can depress the periodontal ligaments enough for proprioception.15,16 At this point, the implant can safely be loaded with a balanced force. This precise timing can be measured to approximately a 0.2-second delay.
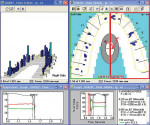
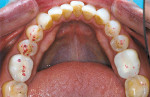
A patient’s implant restoration (Tooth No. 9) had a premature and heavy force compared with the adjacent teeth. The incisal contact was premature (Figure 2a) and the scratchlike tail marking on the mesial exhibited heavy force caused by the small surface area (Figure 2b). The T-Scan III showed that the implant experienced heavier force compared with the adjacent teeth (Figure 2c). The lower right panel detailed how precise adjustment could balance the forces by delayed loading of the implant restoration (Figure 2d). After adjustment, the restoration had a 0.2-second delay in occlusion time.16
Case 3: Symptomatic Teeth
Patients who present with pain on occluding can puzzle clinicians. Many times, dentists are unable to isolate the tooth or reproduce the symptoms during clinical examination. Often, this symptom is associated with cracked tooth syndrome or hyperocclusion. Many patients will suffer needlessly with trial-and-error treatment approaches (ie, crowns, endodontics, and extractions). However, many of these symptomatic teeth can be isolated and treated with simple occlusal adjustments.
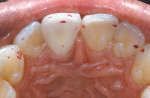
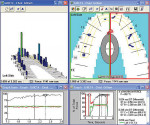
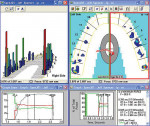
A patient presented with the complaint of a nagging pain on applied occlusal force and cold temperatures. The patient pointed to tooth No. 19 as being the painful location. On examination, dark, large paper markings appeared on tooth No. 19 (Figure 3a). The T-Scan III revealed heavier forces present on both second molars (teeth Nos. 18 and 19) (Figure 3b). Further occlusal force testing accomplished with the Tooth Slooth® II (Professional Results, Inc, Laguna Niguel, CA) confirmed the T-Scan III finding that tooth No. 18 was the offending tooth, despite no presence of prominent, dark, articulating paper markings. Adjustments were performed on the tooth No. 18 composite restoration in centric occlusion and lateral excursions, which relieved the pain. This problematic tooth was quickly identified through the use of T-Scan III technology.
Conclusion
Computerized occlusal analysis instrumentation can be a useful tool in any restorative practice. The time has come for the dental profession to be more precise with all occlusal adjustment while doing no harm to a healthy dentition. Unfortunately, dental school education and many occlusion textbooks4,5 have misled dentists regarding what articulating paper marks actually describe. And these marks have misled dentists into making iatrogenic adjustments. Join the revolution of technology and consider computerized occlusal analysis to be the new standard of care.
Acknowledgment
The author wishes to acknowledge Dr. Robert Kerstein for his mentorship in the use of T-Scan III instrumentation.
References
1. Carey J, Craig M, Kerstein RB, et al. Determining a relationship between applied occlusal load and articulation paper mark area. The Open Dentistry Journal. 2007;1: 1-7.
2. Saad MN, Weiner, Ehrenberg D, et al. Effects of load and indicator type upon occlusal contact markings. J Biomed Mater Res B Appl Biomater. 2008;85(1):18-22.
3. Millstein P, Maya A. An evaluation of occlusal contact marking indicators descriptive quantitative method. J Am Dent Assoc. 2001; 132(9):1280-1286.
4. Glickman I. Clinical Periodontics. 5th ed. Philadelphia, PA: Saunders and Co; 1979: 951.
5. Okeson JP. Management of Temporomandibular Disorders and Occlusion. 5th ed. St. Louis, MO: Mosby and Co; 2003:416, 418,605.
6. Reiber T, Fuhr K, Hartmann H, et al. Recording pattern of occlusal indicators, influence of indicator thickness, pressure, and surface morphology. Dtsch Zahnarztl Z. 1989;44(2): 90-93.
7. Kerstein RB. Using the T-Scan II occlusal analysis system during intraoral occlusal case-finishing. Dental Products Report. 2002;36(1): 102-103.
8. Clinical Research Associates. Occlusal analysis, computerized system. CRA Newsletter. 1989;13(5).
9. Cranham JC. Optimum dental care, part 3: case finishing. Dent Today. 2003;22(5):78-83.
10. Kerstein RB, Lowe M, Harty M, et al. A force reproduction analysis of two recording sensors of a computerized occlusal analysis system. Cranio. 2006;24(1):15-24.
11. Garrido García VC, García Cartagena A, González Sequeros O. Evaluation of occlusal contacts in maximum intercuspation using the T-Scan system. J Oral Rehabil. 1997; 24(12): 899-903.
12. Maness WL, Benjamin M, Podoloff R, et al. Computerized occlusal analysis: a new technology. Quintessence Int. 1987;18(4):287-292.
13. Kerstein RB, Grundset K. Obtaining measurable bilateral simultaneous occlusal contacts with computer analyzed and guided occlusal adjustments. Quintessence Int. 2001;32(1):7-18.
14. Misch CE, Suzuki JB, Misch-Dietsh MF, et al. A positive correlation between occlusion trauma and peri-implant bone loss: literature support. Implant Dent. 2005;14(2): 108-116.
15. Kerstein RB. Computerized occlusal analysis in implant prosthodontics. Implant News and Views. 2000;2(1):1-2.
16. Kerstein RB. Delayed implant loading in cases with implants and natural teeth. Aesthetic Dentistry. Fall 2006:16-20.
17. Coleman TA, Grippo JO, Kinderknecht KE. Cervical dentin hypersensitivity, part II: associations with abfractive lesions. Quintessence Int. 2000;31(7):466-473.
18. Kerstein R. Adhesive aesthetic occlusal case finishing employing computerized occlusal analysis. AACD Monograph. February 2005;2:17-22.
19. Chapman RJ. Principles of occlusion for implant prostheses: guidelines for position, timing, and force of occlusal contacts. Quintessence Int. 1989;20(7):473-480.
20. Kaptein MLA, DePutter C, Delange GL, Blijdorp, PA. A clinical evaluation of 76 implant supported superstructures in the composite grafted maxilla. J Oral Rehab. 1999;26:619-623.
About the Author
Alvin W. Neff, DDS
Private Practice in Restorative Dentistry
Rogers, Arkansas
Senior Clinical Instructor
Aesthetic Advantage
New York, New York