Resurfacing Resin-Modified Glass-Ionomer Restorations
Theodore P. Croll, DDS; Richard R. Cavanaugh, DDS
When glass-ionomer silver cermet (“ceramic/metal”) restorative cement (Ketac-Silver™, 3M ESPE, St. Paul, MN) was introduced in the early 1980s, it became a valuable restorative material for certain purposes.1-3 It proved durable and reliable for the repair of primary teeth and for certain applications in permanent teeth, especially when high fracture strengths were not critical. To this day, the silver-modified glass-ionomer is an especially good interim repair material for partially erupted permanent first and second molars having class I caries lesions. The rationale is to prepare the groove conservatively while debriding all carious substance, then, with a fine-tipped syringe, inject the cermet cement to fill the cavity preparation. Mechanical interlocking retention form is inherently included in the preparation, so the relatively weak bond strength of the cermet material is not of concern. The chemical bonding of the material to dentin and enamel is much more important for maintaining intimate contact of the material to facilitate fluoride ion hydrodynamics (release from the cement and uptake by tooth structure), and reducing marginal leakage. The plan is to cut down the cermet “interim” repair material as necessary, years later, leaving a portion as a dentin replacement base. Using the standard acid-etch protocol, an overlay of resin-based composite (RBC) material then is bonded into place. This “resurfacing” procedure can often be achieved without the use of local anesthetic, because the dentin remains completely protected by the residual glass-ionomer cermet material.
In the late 1980s, when the industry’s experiences with Ketac-Silver were limited to only several years, dentists expected that resurfacing would need to be accomplished within a few years after initial placement. Surprisingly, it has been discovered that in the first decade, or even longer, little wear or erosion of the silver cermet material occurred, so additional treatment was not needed. Conservative glass-ionomer silver cermet “temporization” was far more durable and longer lasting than traditional zinc-oxide/eugenol temporary fillings, by many years. An example of this phenomenon is seen in Figure 1. In January 1991, a half-erupted permanent second molar having two occlusal caries lesions was restored with Ketac-Silver, for a 12-year-old girl. In March 2008, more than 17 years later, she returned for an initial appointment for her 3-year-old daughter. The cermet restorations were still intact, with insignificant wear or erosion, and there was still no need for repair or replacement. In the authors’ practices, numerous other conservative cermet restorations also have lasted well into their second decade, with no signs of wear or breakdown.
With the advent of resin-modified glass-ionomer (RMGI) restorative cements in the early 1990s, silver-modified glass-ionomer systems were phased out in many practices. The resin component of the new RMGI materials enhanced physical properties of the cement, especially fracture strengths and wear resistance, and “on-command” light-hardening made for much clinical convenience and time savings compared with using the self-hardening materials. The use of one RMGI (Vitremer™, 3M ESPE) for use in permanent teeth has been described.4-6
When any type of glass-ionomer interim restoration wears down under masticatory, occlusal, and chemical influences (abrasion, impact, and erosion), a RBC overlay can be placed easily, so that many additional years of service can be achieved. This brief report documents that procedure.
Case Report and Technique
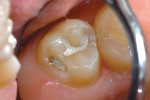
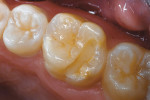
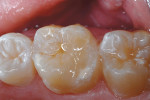
A 6-year-old girl had an erupted maxillary permanent first molar with enamel hypoplasia and associated caries in the occclusolingual groove. The tooth was repaired with Vitremer RMGI restorative cement in 1996. After 11.5 years, approximately 0.5 mm to 1 mm of RMGI material had worn and eroded away (Figure 2). The restoration was resurfaced in the following manner:
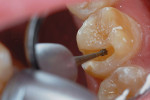
1. Without local anesthesia and using an absorbent cheek pad for isolation, an inverted cone bur was used to remove a thin layer of residual RMGI material. Slight mechanical undercutting was included in the preparation at the junction of the cavity floor and walls (Figure 3).
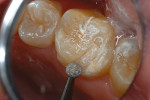
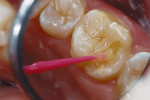
2. A round diamond bur at slow speed roughened enamel at the cavosurface region to enhance acid etching7 (Figure 4).
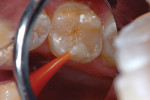
3. A self-etching bonding agent (Adper™ Prompt™ L-Pop™, 3M ESPE) was applied and agitated for 30 seconds (Figure 5).
4. A first increment of RBC was syringe-injected and pressed into place with a ball burnisher, using care to avoid incorporation of any air bubbles (Figure 6). The curing light beam (1,100 mW/cm2) was applied for 8 seconds.
5. Two more increments of RBC were applied and cured in a similar fashion (Figure 7 and Figure 8), and occlusion was evaluated with articulating paper.
6. Figure 9 shows the re-repaired molar immediately after the RBC was overlaid on the residual RMGI material.
Discussion
Because of chemical bonding, biocompatibility, and similar coefficients of thermal expansion, the residual RMGI material serves as an ideal biomimetic, radiopaque dentin replacement material underneath the newly bonded RBC overlay.8 RBC resurfacing is rapid and easily accomplished without the need for local anesthesia. Besides conservation of tooth structure and preservation of pulpal vitality, this easy repair mode gives good justification for use of glass-ionomer cements, particularly RMGIs, as long-lasting restorative materials for permanent teeth.
In 2007, a “nano-ionomer” (Ketac™ Nano, 3M ESPE) was introduced into the dental marketplace.9,10 This RMGI restorative material reportedly has better physical properties than other RMGI cements because of the high filler loading associated with nanoparticle technology. The primary author has been using the nano-ionomer as an interim class I restorative material for more than 2 years, and so far, no discernible wear has been observed in dozens of patients. Comparative longevity of class I restorations using silver cermet material, original RMGI, and the new nano-ionomer would be a worthy subject for in vitro and in vivo investigations.
References
1. McLean JW, Gasser O. Glass-cermet cements. Quintessence Int. 1985;16(5): 333-343.
2. Croll TP, Phillips RW. Six years experience with glass ionomer-silver cermet cement. Quintessence Int. 1991;22:783-793.
3. Croll TP, Killian CM. Glass ionomer-silver cermet interim class I restorations for permanent teeth. Quintessence Int. 1992; 23(11):731-733.
4. Croll TP, Cavanaugh RR. Vitremer cement for class I restoration of permanent teeth. Pract Periodontics Aesthet Dent. 1994;6(8): 25-33.
5. Croll TP, Cavanaugh RR. Direct bonded class I restorations and sealants: six options. Quintessence Int. 1997;28(3):157-168.
6. Croll TP, Helpin ML, Donly KJ. Vitremer restorative cement for children: three clinician’s observations in three pediatric dental practices. ASDC J Dent Child. 2000; 67(6): 391-398.
7. Kanemura N, Sano H, Tagami J. Tensile bond strength to and SEM evaluation of ground and intact enamel surfaces. J Dent. 1999;27(7):523-530.
8. Croll TP, Cavanaugh RR. Posterior resin-based composite restorations: a second opinion. J Esthet Restor Dent. 2002;14(5): 303-312.
9. Croll TP. Nano-filled resin-modified glass ionomer restorative cement. Contemporary Esthetics. 2007;11(9):14-17.
10. Croll TP, Nicholson JW. Glass-ionomer cements: History and current status. Inside Dentistry. 2008;4(3): 76-84.
About the Authors
Theodore P. Croll, DDS
Private Practice
Pediatric Dentistry
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry
University of Washington School of Dentistry
Adjunct Professor
Department of Pediatric Dentistry
University of Texas Health Science Center at San Antonio
Dental School
San Antonio, Texas
Richard R. Cavanaugh, DDS
Private Practice
Fixed and Implant Prosthodontics
Doylestown, Pennsylvania