Adhesive Cementation of Direct Ceramic Restorations Using a Self-Etch Technique
Dennis J. Fasbinder, DDS, ABGD
The ability to develop a reliable bond between a ceramic restoration and the tooth is a key element in the clinical success with CAD/CAM direct ceramic restorations. Composite resin luting agents are currently the preferred material of choice for adhesively bonding ceramic restorations.1 They provide several advantages, such as a durable and strong bond to the tooth and ceramic, good color match, polishable marginal areas resulting in good margin adaptation, and convenient delivery systems.
There are several popular techniques for the adhesive cementation of CAD/ CAM direct ceramic restorations. One option is to use an adhesive bonding system with a composite-resin luting agent. This technique includes the use of etch-and-rinse (total-etch) or self-etch bonding systems with a dual-cured or self-cured resin luting agent. Another option is to use a self-adhesive composite-resin luting agent that contains the adhesive bonding agent. This technique includes the automix or precapsulated luting agents that require no pretreatment of the tooth surface to develop an adhesive bond.
The most commonly recognized technique is the etch-and-rinse or total-etch technique. Phosphoric acid is used to etch the surface of the cavity preparation to remove the smear layer, demineralize the dentin surface, and produce an increase in bonding surface area for micromechanical retention. A primer/adhesive is applied to the etched tooth surface before the placement of the composite-resin luting agent. This technique has been well-tested in a number of clinical studies and there is significant clinical evidence for its success.2-4
Many clinicians have elected to use self-etch bonding systems with a composite resin luting agent because of concerns with postoperative sensitivity and the desire for a more efficient cementation process. Self-etch adhesives have acidic monomers that simultaneously make the smear layer permeable and form a hybrid layer in the underlying dentin.5 The acidic monomers are not rinsed from the tooth. Self-etching bonding systems are considered more efficient because they can be applied in one or two steps. The acid-etching and rinse steps are eliminated, thus minimizing the time required for isolation of the cavity preparation to ensure successful bonding.6,7
Self-etching systems may come in single-step or two-step formulations. Two-step formulations contain separate agents for priming and bonding. A hydrophilic primer is applied for self-etching, followed by the application of a relatively more hydrophobic bonding agent.8 One-step self-etch adhesives are packaged as two liquids, which are mixed together before application to the cavity preparation. The reason for separating the two solutions is to isolate the potentially unstable acidic resin monomers from the water that causes their ionization and activation.9 Self-etch bonding systems eliminate the potential disadvantages of total-etching systems, such as excessive etching and/or over drying, leading to an inadequate “moist” surface for optimal bonding.10 Self-etch systems may also reduce postoperative sensitivity because the dentinal tubules are not exposed as a result of a reduction in the number of bonding steps.8 However, their etching potential, especially on unprepared enamel, is not as great as that produced by a total-etch system.11
Considerable time and effort has been devoted to determining the comparable bond strengths of total-etch and self-etch systems. And there is little consensus as to the outcome. Knoblach and coworkers evaluated the microtensile bond strength of three one-step, self-etching adhesives, two two-step, self-etching adhesives, and a total-etch adhesive. Of the bonding agents tested, significantly higher microtensile bond strength was obtained with the total-etch, two-stage adhesive. One-bottle, self-etch adhesive systems exhibited similar bond strengths to the two-bottle, self-etch adhesives.12 DeMunck and coworkers evaluated the microtensile bond strength of three one-step, self-etch (all-in-one) adhesives; two two-step, self-etch adhesives, one two-step, total-etch adhesive, and one three-step, total-etch adhesive. The microtensile bond strength of the total-etch adhesives to enamel was significantly higher than that of the one-step, self-etch adhesives. Comparing the dentin microtensile bond strength, only OptiBond FL® (Kerr Corporation, Orange, CA) performed significantly better than the one-step, self-etch adhesives. The one-bottle, self-etch adhesive bond strengths were significantly lower than those of the two-bottle, self-etch adhesive systems.13 Several other studies have clearly demonstrated that although the simplification in the bonding process may ease handling for the general practitioner, it may not improve adhesive effectiveness.9,14
Selection of an adhesive luting technique for adhesive cementation of direct CAD/CAM restorations involves a number of considerations. The personal preference of the clinician will influence the choice of the viscosity of the cement, the number of shades available, the delivery system, and the product cost. If evaluation of the restoration shade before final cementation is deemed an important part of the process, as it would be for anterior restorations, the option to use try-in pastes would be essential. However, try-in pastes are generally not required for posterior restorations. The polymerization reaction of the cement may also be a consideration. The setting time of a visible light-cured cement can be controlled by the application of the curing light, maximizing the time available to clean up excess cement after placement, whereas self-cured cements would limit the time available to the setting time of the cement after mixing.
Dual-cured composite-resin luting agents are typically favored for posterior ceramic restorations because of the inability to predictably photopolymerize through thicker ceramic restorations. The dual-cured cements provide extended working times and somewhat controllable polymerization. The overwhelming majority of published literature indicate that dual-cured composite resin cements should be light-cured, rather than rely solely on the self-cure components, to achieve a maximum bond to the tooth.15-17 Several in vitro studies have also documented a lower conversion rate for dual-cure resin cements after chemical curing compared to when they are also light-cured.18-20 This would reinforce the recommendation to universally photopolymerize dual-cured cements.
The degree of radiopacity of the cement may also be a consideration for the clinician. Relatively opaque resins are easily visualized on post-cementation radiographs to ensure no retained cement. And they leave little doubt as to the margin integrity of the restoration.
One overriding aspect of the choice of cements seems to be the efficiency of the clinical technique. Although the total-etch technique has considerable clinical evidence as to its effectiveness, clinicians are interested in minimizing the time required for proper isolation for predictable bonding by using materials that require less time to place and cure. The selection of self-etching luting systems can reduce the required time for isolation by several minutes. Many clinicians consider this a significant advantage as it may reduce the risk of less than optimal adhesive bonding. This is especially true with problematic areas to create predictable cavity isolation.
One such self-etching system that is available for adhesive luting of direct ceramic restorations is Futurabond DC with Bifix QM (VOCO America, Inc, Sunnyside, NY). Futurabond DC is a dual-cure adhesive bonding agent (Figure 1). The highly functional SiO2 nano particles (Ø 20 nm) in Futurabond DC facilitate cross-linking of the resin components and enhance its film-building properties. Thus, the adhesive can optimally wet the cavity preparation with a single coat. The manufacturer reports that the nanoparticles also reinforce the hybrid layer helping to create a high bond strength. Futurabond DC comes in a unit-dose blister package to ensure consistent bond strength with each use. Liquid A contains polyfunctional adhesive monomers that only react in aqueous conditions. Liquid B contains water. When the blister pack is activated to mix the two liquids, a pH of 1.4 is created. As the adhesive is applied to the tooth surface, it will solubilize the smear layer and penetrate and demineralize the dentin surface. The acidic solution in the bonding agent is neutralized by the hydroxyapatite crystals in the tooth.
Bifix QM (VOCO America) is a radiopaque, dual-cured resin luting agent. It comes in three shades; universal, white opaque, and translucent with corresponding try-in pastes (Figure 2). The kit also contains a ceramic primer. It has an automix syringe delivery system for ease in application. It has a setting time of 3 minutes without light-curing. It has demonstrated good bond strength to bonded ceramics and zirconium restorations in laboratory studies.21-23
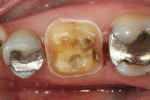
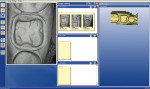
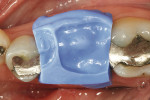
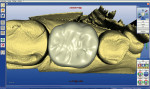
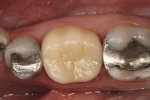
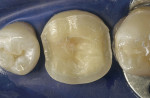
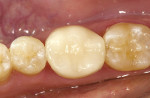
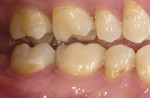
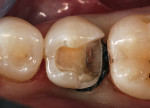
The clinical case in Figure 3 illustrates a patient who presented with a perforated gold crown that had been previously repaired with amalgam. The patient was interested in having the gold crown replaced with a tooth-colored, all-ceramic crown. A crown preparation for a chairside CAD/CAM crown (CEREC 3D, Sirona Dental Systems, Charlotte, NC) was completed after removing all of the previous restorative material from the tooth (Figure 4). Once the preparation was completed, the teeth were powdered with a titanium dioxide spray to provide a uniform reflective surface for the optical imaging process (Figure 5). The CEREC 3D intraoral camera was used to record the cavity preparation to the 3D software design program (Figure 6). A polyvinylsiloxane (PVS) bite registration material (Registrado x-tra, VOCO America) was used to record the opposing dentition to the preparation to design the occlusal contacts on the crown (Figure 7). The rigidity of the bite registration material ensures an accurate replication of the opposing dentition. The PVS bite registration was also powdered with the titanium dioxide spray to facilitate recording the bite registration to the computer design program with the CEREC 3D intraoral camera (Figure 8).
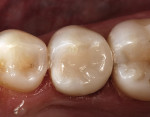
The CEREC 3D software design program was used to fabricate the desired contours and occlusal relationships for the crown (Figure 9). A fine-grained feldspathic ceramic (Vita® Mark II, Vident, Brea, CA) was selected to mill the crown. After adjustment of the contacts and final staining and glazing of the crown, the internal surface was etched with 4.9% hydrofluoric acid, rinsed, and then coated with a silane coupler to create an optimal surface for bonding with the resin luting agent. The self-etching adhesive bonding agent (Futurabond DC, VOCO America) was activated to mix the two liquids within the unit-dose blister package. The blister seal was broken with the bonding brush and the self-etching adhesive was applied and agitated for 20 seconds over the entire surface of the crown preparation (Figure 10). The self-etch adhesive was lightly dried for 5 seconds and then cured with a halogen curing light for 10 seconds. A dual-cured adhesive resin luting agent (Bifix QM) was dispensed with its automix syringe into the crown (Figure 11). The crown was seated, and excess cement was removed before final curing of the luting agent (Figure 12).
Conservation of tooth structure has always been a key element of restorative dental procedures. A preservative approach to tooth preparation is very much in demand instead of macromechanically styled, destructive preparations that are required for the retention of metallic restorations. Although there is ongoing discussion about the relative bonding strength of total-etch and self-etch luting techniques, there is considerable clinical evidence on the long-term success of the total-etch technique. The selection of adhesive luting materials that are clinically more efficient have logical merit, but do not currently have similar long-term clinical evidence to promote their unrestricted use. It would seem more prudent to consider the influence that the cavity preparation may have on the clinical longevity of the adhesive bond. Cavity preparations that are purely adhesive in nature would seem to favor the selection of the total-etch luting technique (Figure 13a, Figure 13b and Figure 13c), whereas cavity preparations that have more internal resistance form may be well-suited for the self-etch techniques (Figure 14a and Figure 14b).
Conclusion
Adequate retention of direct ceramic restorations may be achieved with both total-etch and self-etch adhesive materials. Self-etch adhesives offer the advantage of a more efficient clinical technique that may prevent postoperative sensitivity and be less technique-sensitive compared to total-etch materials. Long-term clinical research will provide valuable information relative to indications and limitations to aid clinicians in selecting the appropriate adhesive technique.
Disclosure
The author receives grant and research support from Sirona.
Reference
1. Caughman WF, Chan DC, Rueggeberg FA. Curing potential of dual polymerizable resin cements in simulated clinical situations. J Prosthet Dent. 2001;86: 101-106.
2. Posselt A, Kerschbaum T. Longevity of 2328 chairside CEREC inlays and onlays. Internatl J Computer Dent. 2003;6(3):231-248.
3. Fasbinder DJ, Dennison JB, Heys DR, Lampe K. The clinical performance of CAD/CAM-generated composite inlays. J Am Dent Assoc. 2005;136(12):1714-1723.
4. Reiss B. Clinical results of CEREC inlays in a dental practice over a period of 18 years. Internatl J Computer Dent. 2006;9:11-22.
5. Tay F, Pashley DH. Have dentin adhesives become too hydrophilic? J Can Dent Assoc. 2003;69:726-31.
6. Peumans M, Kanumilli P, De Munck J, et al. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005;21:864-881.
7. Senawongse P, Harnirattisai C, Shimada Y, Tagami J. Effective bond strength of current adhesive systems on deciduous and permanent dentin. Oper Dent. 2004;29: 196-202.
8. Tay FR, Pashley DH. Aggressiveness of contemporary self-etching systems. I. Depth of penetration beyond dentin smear layers. Dent Mater. 2001;17:296-308.
9. Frankenberger R, Perdigao J, Rosa BT, Lopes M. “No-bottle” vs “multi-bottle” dentin adhesives-a microtensile bond strength and morphological study. Dent Mater. 2001;17:373-380.
10. Kiremitci A, Yalcin F, Gokalp S. Bonding to enamel and dentin using self-etching adhesive systems. Quintessence Int. 2004;35:367-370.
11. Sadek FT, Goracci C, Cardoso PE, et al. Microtensile bond strength of current dentin adhesives measured immediately and 24 hours after application. J Adhes Dent. 2005;7: 297-302.
12. Knobloch LA, Gailey D, Azer S, et al. Bond strengths of one- and two-step self-etch adhesive systems. J Prosthet Dent. 2007;97 (4): 216-222.
13. De Munck J, Van Meerbeek B, Satoshi I, et al. Microtensile bond strengths of one-and two-step self-etch adhesives to bur-cut enamel and dentin. Am J Dent. 2003;16:414-420.
14. Frankenberger R, Strobel WO, Lohbauer U, et al. The effect of six years of water storage on resin composite bonding to human dentine. J Biomed Mater Res Part B Appl Biomater. 2004;69:25-32.
15. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: a review of the current literature. J Prosthet Dent. 1998;80: 280-301.
16. Burke FJ, Fleming GJ, Nathanson D, Marquis PM. Are adhesive technologies needed to support ceramics? An assessment of the current evidence. J Adhes Dent. 2002;4:7-22.
17. Garcia RN, Reis AF, Giannini M. Effect of activation mode of dual-cured resin cements and low-viscosity composite liners on bond strength to dentin. J Dent. 2007;35(7):564-569.
18. Rueggeberg FA, Caughman WF. The influence of light exposure on polymerization of dual-cure resin cement. Oper Dent. 1993;18: 48-55.
19. Peters AD, Meiers JC. Effect of polymerization mode of a dual-cured resin cement on time-dependent shear bond strength to porcelain. Am J Dent. 1996;9:264-268.
20. Shimura R, Nikaido T, Yamauti M, et al. Influence of curing method and storage condition on microhardness of dual-cure resin cements. Dent Mater. 2005;24:70-75.
21. Gernhardt CR, Fechner K, Schallet HG. Microtensile bond strength of four self-conditioning dentin adhesives. J Dent Res. 2005(Special Issue): Abstract #2972.
22. Mohs T, Wappler P, Bekes K, et al. Microtensile bond strength of resin cements used with different ceramics. IADR-European and Israeli Divisions. 2007; Abstract #183.
23. Toman M, Toksavul S, Artunc C, et al. Influence of luting agent on the microleakage of all-ceramic crowns. J Adhes Dent.2007;9(1):39-47.
About the Author
Dennis J. Fasbinder, DDS, ABGD
Clinical Professor
Director, Advanced Education in General Dentistry Program
University of Michigan School of Dentistry
Ann Arbor, Michigan