Esthetic Replacement of Failing Amalgam Restorations
Daniel H. Ward, DDS
Conservative treatment has become the paradigm in healthcare.1 Minimally invasive procedures that remove only diseased tissue are expected by today’s patients. Dentists should incorporate this concept of preserving natural tooth structure when restoring teeth.2
Amalgam restorations are relatively easy to place and predictable. Further, they were the standard for years. However, more than diseased tooth structure must be removed to allow for adequate bulk and mechanical retention.3 In addition, many patients have concerns about the atoms that reside within the molecular makeup of amalgam restorations and demand alternatives. Composite restorations have become the most prevalent direct placement procedure in the United States.4
Tooth–Colored Restorations
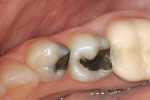
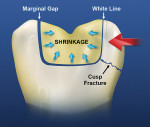
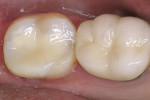
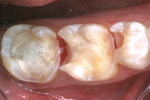
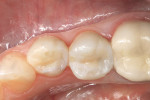
When patients present with decay visible under existing amalgam restorations, many treatment choices are available (Figure 1). Tooth-colored restorations are preferred by a significant number of patients, yet the ability of many dentists to perform predictable, long-lasting direct composite restorations has been varied.5 Frustrations include postoperative sensitivity, difficulty obtaining consistent anatomical interproximal contacts, increased wear, and de-creased restoration longevity.6 Today’s composite restorative materials shrink 0.5% to 4% by volume after polymerization. Polymerization shrinkage stress may result in the formation of marginal gaps, visible white lines, or actual cusp fracture7 (Figure 2). Because of these challenges, many teeth are restored using heavily prepared full-coverage procedures, which though predictable, are not conservative and are visibly noticeable.8 All-ceramic, full-coverage restorations require even more tooth structure to be sacrificed to allow for the proper thickness and contour of the crown. Some dentists view direct composite restorations as interim restorations, which will serve as the core for the inevitable placement of a full-coverage crown. Others, struggling with the ethics of providing treatment they know will not last, place amalgam restorations in spite of patient objections.
Tooth-colored indirect inlays and onlays are one answer to solving the challenges inherent with direct composite procedures. These restorations have much greater potential to exhibit properly formed interproximal contacts.9 Polymerization shrinkage stress is virtually eliminated and only occurs within the very thin resin cement layer.10 Ceramic or composite materials may be used with a one- or two-visit technique. Indirect composite inlays and onlays optically blend into the tooth structure because of the layering of different composites within the restoration. The margins are generally more precise, and the restorations are easier to finish and polish properly after intraoral adjustment. Insufficient interproximal contacts can be added chairside, eliminating the need for the patient to return to the office if they need to be enhanced. Ceramic inlays and onlays have better wear resistance and are stronger than composite restorations, but they are more difficult to polish in the mouth. When opposing natural tooth structure, composite restorations are worn by the natural tooth; whereas porcelain restorations will create wear on the natural tooth.
In–Office, Single–Visit CAD/CAM Ceramic Restorations
In-office, all-ceramic computer-aided design/computer-aided manufacturing (CAD/ CAM) restorations have become well publicized. The ability to complete a restoration at a single visit is of benefit to patients and dentists. The reported long-term prognosis for these restorations has been excellent.11,12 The ease of fabrication and marginal fit of the restorations have been improving steadily with developing technology. Multicolored porcelain blocks have become available, reducing the monochromatic appearance of unglazed restorations. Critical principles of preparation design must be followed carefully for the computer to be able to mill acceptable restorations successfully. The dentist must be willing to devote adequate time and effort to mastering the techniques. The learning process can be stimulating for the dentist who enjoys learning new technology. The cost of the units required for ceramic design and fabrication may prevent many dentists from embracing this mode of treatment.
Two–Visit, All–Ceramic Restorations
All-ceramic, laboratory-fabricated restorations have been placed successfully for a number of years. Pressed ceramic inlays and onlays have enjoyed the most widespread use. In most posterior cases the restoration is fabricated from a single ingot using the lost-wax technique. The outer surface is glazed and returned to the dentist for seating. These restorations have a predictable record of long-term success.13 CAD/CAM restorations also may be fabricated by the dentist who makes impressions and fabricates the ceramic restoration from a model or sends the impressions to a dental laboratory that uses this technology.
In–Office, Single–Visit Indirect Composite Restorations
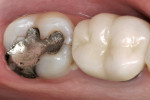
Direct composite restorations may be placed when the width of the restoration is < 50% of the intercuspal width of the tooth.14 This optimal width often is exceeded when replacing faulty existing amalgam restorations (Figure 3). A study by Brunthaler et al15 showed a linear relationship between the size of the restoration and the number of failures. To prevent the problems resulting from polymer-ization shrinkage stress, in-office direct/indirect procedures may be used.
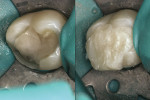
Class 1 restorations can be excavated, based, and prepared with walls that diverge toward the occlusal (Figure 4). A water-soluble separating medium, such as glycerin, is painted inside the preparation, and composite is placed into the tooth (Figure 4). The composite is light-cured and removed from the tooth for additional light- and heat-polymerization (Triad®, DENSTPLY Prosthetics, York, PA) or light-, heat-, and pressure-polymerization (Tescera™ ATL™ BISCO Inc, Schaumburg, IL) (Figure 5). The internal surface is sandblasted, and the restoration is bonded to the tooth. The anatomy on the outer surface of the restoration can be shaped and polished after proper bonding has occurred (Figure 6). Any space created during polymerization shrinkage is filled with the luting resin cement. Polymerization shrinkage stress virtually is eliminated, and the composite is polymerized more highly.
Similar procedures can be used for Class 2 restorations, but require more skill and experience. Firm, properly contoured interproximal contacts can be accomplished using this technique by adding a slight excess of composite resin to the contact area before final polymerization. The area is shaped for ideal contact during the try-in and adjustment phase before adhesive cementation.
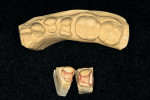
In-office indirect composite restorations also can beneficial when a patient has a difficulty coming to the office because of health, scheduling, or travel distance and multiple restorations must be placed (Figure 7a). In this case it was decided to place a direct composite restoration on the lower right second premolar (tooth No. 29) and indirect composite onlays on the two molars (teeth Nos. 30 and 31). The teeth were shaped and impressions were made (Figure 7b). Dies made of quick-setting plaster were made (Figure 7c). The restorations were fabricated and seated at the same 2-hour appointment (Figure 7d).
Two–Visit Indirect Composite Restorations
Many patients are drawn to offices offering the latest technology. Dentists often are willing to invest in new equipment and techniques in which they are not well acquainted. Often only after the financial outlay has been committed does the dentist develop the skills and techniques needed to incorporate the new procedures the equipment makes possible. Becoming experienced with the preparation and seating procedures of tooth-colored inlays and onlays may be helpful for a dentist contemplating the purchase of an expensive CAD/CAM system.
The use of an in-office composite restorative system is an excellent way to implement tooth-colored inlay/onlay restorations into the practice. The materials and equipment required to fabricate indirect composite restorations cost a small fraction of a CAD/CAM system. Fabricating restorations can be educational and return the artistic elements of dentistry to the dentist’s hands. When the person making the restoration is the same person who shapes the tooth, the quality of the preparation improves.
In-office, two-visit indirect composite inlays were chosen to replace the faulty amalgam restorations discussed earlier (Figure 1). With significant missing tooth structure, direct composite restorations were deemed to have the potential to induce excessive polymerization shrinkage stress on the remaining tooth struc-ture and make obtaining proper interproximal contact and contour difficult. Full-coverage crowns were deemed to be too invasive. Porcelain inlays could have been used, but indirect composite inlays offered the best choice for esthetic, long-lasting restorations at the most reasonable cost.
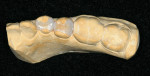
Fabrication of in-office, two-visit indirect composite inlays is relatively simple and can be performed in short intervals totaling approximately 1 hour. In an office where inadvertent last-minute cancellations occur, this time can be used to make the composite restorations. After tooth preparation and impression making, provisional restorations are placed and the patient reappointed, usually within 1 week. The impression is poured twice, and individual dies as well as a solid model are made. The margins on the individual dies are marked, the dies coated with die sealer, and then with a layer of rubber-die spacer. The solid model is scraped below the margin of the interproximal area to allow space for the eventual try-in of the inlays (Figure 8).
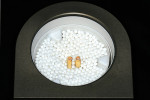
The first layer applied is dark opaque hybrid composite, which mimics the shade of the dentin and allows for optimal bonding to occur between the luting resin cement and the intaglio surface of the restorations. If using the Tescera ATL system, each layer is pressurized before light polymerization to reduce porosity (Figure 9). The restorations are built up in layers, simulating the natural inherent colors of the tooth (Figure 10). Outer “enamel” is created with microfill composite, which is more translucent and offers better wear resistance. The formed restorations are polymerized fully in the curing unit, which pressurizes, light-cures, and heats the restorations to 130°C. The solid model is used to shape the interproximal contacts of the fully polymerized composite material, and the inlays are shaped and polished (Figure 11).
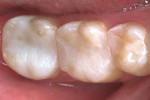
At the seating appointment, the provisional restorations are removed, the interproximal contacts adjusted, and the margins evaluated. The internal aspects of the restorations are sandblasted and dual-curing composite resin cement is used to bond the restorations to the tooth. Final occlusal adjustments, finishing, and polishing are performed in the mouth. The resulting restorations blend beautifully, exhibit excellent contacts, and should enjoy a long lifetime (Figure 12).
Conclusion
Though no restoration should be considered “permanent,” each restoration should be designed to have reasonable longevity. The use of materials and techniques that fulfill this requirement should be considered when satisfying the desires of the patient for esthetic restorations. Dentists need to make greater use of conservative long-lasting tooth-colored restorations.
Disclosure
The author receives material support from BISCO Inc.
References
1. Ericson D. The concept of minimally invasive dentistry. Dent Update. 2007;34(1):9-18.
2. Christensen GJ. The advantages of minimally invasive dentistry. J Am Dent Assoc. 2006;137(3):296-300.
3. Sturdevent CM, Heymann HO, Roberson TM, et al. Classes I, II, and VI cavity preparations for directly placed composites. In: Sturdevent CM, ed. The Art and Science of Operative Dentistry. 3rd ed. St. Louis, MO: Mosby; 1995:594.
4. Berthold M. Restoratives: trend data shows shift in use of materials. ADA News. 2002;33(11): 1,10.
5. Ritter AV. Posterior composites revisited. J Esthet Restor Dent. 2008;20(1):57-67.
6. Puckett AD, Fitchie JG, Kirk PC, et al. Direct composite restorative materials. Dent Clin North Am. 2007;51(3):659-675.
7. Davidson CL, Feilzer AJ. Polymerization shrinkage and polymerization shrinkage stress in polymer-based restoratives. J Dent. 1997;25(6): 435-440.
8. Jackson RD. Aesthetic inlays and onlays: the coming of age. Br Dent J. 2008;204(7): 407-408.
9. Ward DH. Predictable esthetic indirect restorations. Compend Contin Educ Dent. 2003;24(8 Suppl):48-52.
10. Jackson RD. Indirect resin inlay and onlay restorations: a comprehensive clinical overview. Pract Periodontics Aesthet Dent. 1999;11(8):891-902.
11. Reich SM, Wichmann M, Rinne H, et al. Clinical performance of large, all-ceramic CAD/CAM-generated restorations after three years: a pilot study. J Am Dent Assoc. 2004;135(5): 605-612.
12. Sjögren G, Molin M, van Dijken JW. A 10-year prospective evaluation of CAD/CAM-manufactured (CEREC) ceramic inlays cemented with a chemically cured or dual-cured resin composite. Int J Prosthodont. 2004;17(2):241-246.
13. Stoll R, Cappel I, Jablonski-Momeni A, et al. Survival of inlays and partial crowns made of IPS empress after a 10-year observation period and in relation to various treatment parameters. Oper Dent. 2007;32(6):556-563.
14. Albers HF. Tooth Colored Restoratives: Principles and Techniques. 9th ed. Hamilton, ON: BC Decker Inc; 2001:203.
15. Brunthaler A, König F, Lucas T, et al. Longevity of direct resin composite restorations in posterior teeth. Clin Oral Investig. 2003;7(2):63-70.
About the Author
Daniel H. Ward, DDS
Assistant Clinical Professor
Section of Restorative and Prosthetic Dentistry
College of Dentistry
The Ohio State University
Columbus, Ohio
Private Practice
Columbus, Ohio