Using Diagnostic Wax-Ups and Preparation Guides to Facilitate Accurate and Esthetic Diastema Closure and Functional Bite Alteration
Thomas E. Dudney, DMD
Closing a diastema can be a challenging and difficult task that may find the clinician restoring or working with multiple teeth to ensure the equalization of space, or removing some tooth structure—such as from the distal surface of teeth—to be able to “move” subsequent teeth mesially.1 Unfortunately, in some instances, dentists may attempt to close diastemas without removing sufficient tooth structure from the surrounding dentition, or without altering or adjusting the gingival zeniths of those teeth. The result could be the creation of an awkward and unwanted triangular appearance of the teeth, or leaving the teeth with an inappropriate width-to-length ratio that compromises their efforts to create the more pleasing and durable smile their patients wanted.2 To avoid such scenarios, diagnostic wax-ups and preparation guides can be invaluable tools to help ensure esthetic, functional, and restorative success by facilitating and enhancing the treatment planning process.3
For example, when closing a diastema and creating the illusion of tooth movement with indirect porcelain/ceramic restorations, it is important for ceramists to be able to “wrap” the porcelain interproximally through the entire thickness of the tooth, as opposed to just halfway through the interproximal space. This need arises from the fact that the darkness of the mouth will create a shadowy effect in the space between the teeth, thereby necessitating thicker ceramic material. As a result, clinicians may need to perform slice preparations on the distal aspects of the selected teeth and, consequently, move the gingival zeniths in a mesial direction to help maintain the proportionality of the teeth.
Such a plan of action may seem to be common sense. However, in the midst of treatment planning, the value of a diagnostic wax-up is the ability to visualize what will be needed to execute a successful clinical and treatment protocol to achieve the desired end result.3 This article demonstrates the use of a diagnostic wax-up and preparation guides during the treatment of a patient who presented primarily for esthetic concerns (ie, midline diastema, tooth color, ceramometal crown) and who also required alteration of his bite (ie, changing the end-to-end bite relationship of his anterior teeth to a normal overbite and overjet, with anterior guidance within the patient’s envelope of function).
CASE PRESENTATION
A 47-year-old man presented for consultation because he was unhappy with the appearance of his smile. Specifically, he did not like the midline diastema, the color of his teeth, or the ceramometal crown on tooth No. 9 (Figure 1 and Figure 2). An initial examination was performed that included radiographs and diagnostic records, full-arch polyvinyl siloxane impressions (Aquasil Ultra, DENTSPLY Caulk, Milford, DE), a centric relation bite record, and a facebow transfer (Artex® Facebow, Jensen Industries, North Haven, CT). It was during this examination that it became apparent that the patient demonstrated an end-to-end bite relationship of his anterior teeth (Figure 3); any treatment plan developed would need to alter this relationship to one with a normal overbite and overjet. Multiple photographs showing the teeth in full-facial smile, occlusal (Figure 4 and Figure 5), and retracted views were also obtained.4 All of this information was forwarded to the laboratory so that the ceramist could create a diagnostic wax-up, putty matrix, and preparation guides.
Treatment Planning
After the initial examination and after reviewing all of the recorded information, the treatment goals were developed. These included addressing the patient’s concerns and additionally changing the end-to-end bite relationship of his anterior teeth to one with a normal overbite and overjet, with anterior guidance within his envelope of function. Specifically, the diastema would be closed, which required that the size and shape of his teeth be altered,5 and he would be given a whiter, brighter smile. Therefore, the diagnostic wax-up—and the related clinical tools (eg, putty matrix and preparation guide)—were imperative to the success of the case. The resulting treatment plan called for 10 maxillary and 10 mandibular restorations (ie, teeth Nos. 4 through 13 and 20 through 29 with feldspathic porcelain veneers [Ceramco®, DENTSPLY Prosthetics, Burlington, NJ] and a feldspathic all-porcelain crown on tooth No. 9).
The diagnostic wax-up enabled the preoperative visualization of the proposed changes (Figure 6), as well as the creation of the provisional restorations that would simulate the proposed changes intraorally. To accomplish that, a putty matrix was fabricated (Sil-Tech putty, Ivoclar Vivadent, Amherst, NY) from the diagnostic wax-up. Furthermore, the diagnostic wax-up was used to create incisal reduction and facial reduction preparation guides that aided in ideal tooth preparation (Figure 7A and Figure 7B). Such guides are especially beneficial in a case such as this when a diastema is being closed and a bite is being changed.
Preparation Protocol
During preparation, a .05-mm depth-cutting bur (843-016, Brasseler USA, Savannah, GA) was used to establish uniform depth of the preparations, after which a 6844-016 bur (Brasseler USA) was used to complete the preparations. All margins were equi-gingival at the facial aspect and slightly subgingival interproximally to allow for the proper emergence profile of the restorations6 (Figure 8 and Figure 9).
A soft tissue diode laser (Twilight, Biolase Technologies, Irvine, CA) was used to create ideal gingival symmetry and move the gingival zenith in a mesial direction to avoid the appearance of restorations with an excessive mesial-axial inclination and/or an exaggerated triangular shape.7,8 The literature has demonstrated that if the mesiodistal spaces are not symmetrical and the gingival scallops are not in alignment, the esthetics associated with diastema closure can be compromised (Figure 9 and Figure 10).1
It is important to note that in cases such as this with a large midline diastema, it is often necessary to reduce the distal aspect of all the anterior teeth slightly to ensure sufficient room for widening each subsequent tooth in a mesial direction, as suggested earlier. When this is not accomplished and space is closed only by adding porcelain to the mesial aspect of the central incisors, it is very difficult to achieve an ideal length-to-width ratio (ie, 75% to 80%); the final result will be teeth that appear too wide and unesthetic.2 Rather, in this case a slice preparation in the form of a feather edge was extended in a palatal direction to the mesio-lingual or disto-lingual line angle of the tooth to allow the ceramist to wrap porcelain through the interproximal contact area.9 When the preparations were completed, they were verified using the preparation guides to ensure proper incisal and facial reduction and sufficient spacing for the diastema closure.
Full-arch polyether impressions (Impregum™, 3M ESPE, St. Paul, MN) were taken, along with an occlusal record (Vanilla Bite Registration, Discus Dental, Culver City, CA), stick bite, a facebow transfer (Artex Facebow), and a shade of prepared teeth (stumpf shade 9). In addition to the preoperative photographs, additional images of the preparations were taken for use by the dental laboratory in fabricating the definitive restorations. A detailed laboratory prescription discussing the goals for the case, the patient’s concerns, and the final desired shade was also sent. Feldspathic porcelain was chosen because the prepared tooth color was fairly light, and powder/liquid ceramics are highly translucent yet very durable when bonded to the tooth;10 in the hands of a talented ceramist, they can create very natural, life-like esthetics.
Provisionalization
The provisional restorations were created using a putty matrix of the diagnostic wax-up and a temporary material (Luxatemp®, Zenith DMG, Englewood, NJ) in shade B1. The margins were finished, the gingival embrasures opened, and the occlusion adjusted, after which the temporaries were polished (Figure 11). The provisionals were critical to the success of this case because they served as a blueprint for the final restorations and allowed the patient to evaluate a simulated result and offer feedback. Furthermore, the patient was able to return for a post-provisionalization appointment to evaluate function and esthetics, at which time the new bite (Figure 12 ) was evaluated in all excursive movements; the length was also verified with phonetics.
The goals for the occlusion were equal-intensity centric stops, no posterior contact in lateral and protrusive movements, and anterior guidance within the patient’s envelope of function.11 By simulating the final result in the provisional restorations, it was possible to achieve the desired results and then communicate this information to the laboratory for the fabrication of the definitive restorations. All of this information was transferred to the laboratory with impressions and photographs of the approved provisionals to further facilitate communication.
Cementation of the Final Restorations
At the insertion appointment, the provisional restorations were carefully removed, and the preparations were cleaned with hydrogen peroxide and disinfected with a chlorhexidine rinse (Consepsis®, Ultradent Products, Inc, South Jordan, UT). The definitive restorations were tried in with water individually and then altogether to evaluate fit, marginal integrity, color, and esthetic integration. After approval from the patient, the restorations were set aside to be etched, rinsed, dried, and silanated in preparation for cementation while the teeth were isolated with a rubber dam.
The restorations were bonded to the teeth using a total-etch technique with a fifth-generation bonding agent (Prime & Bond® NT™, DENTSPLY Caulk) and a light-cured luting cement (Variolink® Veneer, Ivoclar Vivadent) in shade +1. Excess cement was cleaned from the facial surfaces with cotton rolls and brushes. The restorations were then tacked in place at the gingival margin using a 3-mm curing light tacking tip for 5 seconds per tooth. Excess cement was then removed interproximally with dental floss, after which the restorations were light-cured for 1 minute each from the facial and lingual surfaces using an LED curing light (bluephase® 16i, Ivoclar Vivadent).
The interproximal contacts were polished using diamond finishing strips (Brasseler USA), and the occlusion was checked and adjusted where necessary. Finally, the restorations were polished using rubber points (Ceramisté™, Shofu Dental Corporation, San Marcos, CA) and polishing paste (Porcelize™, Cosmedent, Chicago, IL) on a felt wheel.
The patient returned for a postoperative follow-up appointment, at which time minor occlusal adjustments were made and the restorations were repolished. The patient was able to function normally, with both lateral and protrusive guidance, was able to speak normally, and stated that he was very happy with the appearance of his smile and his appearance overall. It was determined that the goals of the case had been achieved (Figure 13 ; Figure 14 ; Figure 15 ).
CONCLUSION
The primary objectives of this case included closing the maxillary midline diastema while maintaining the proportionality of the teeth, thereby ensuring that they would not appear too wide or artificial. Additionally, the crown on tooth No. 9 needed to match seamlessly with the surrounding veneer restorations to restore the patient’s happiness with the color and appearance of his smile. Therefore, a whiter, brighter smile was created for the patient. Finally, the patient’s end-to-end bite was corrected to a proper bite relationship, one with an overbite and overjet and anterior guidance that would give him long-term function. Paramount to the successful completion of this case was proper communication between the dentist and the laboratory technician/ceramist, as well as between the dentist and the patient. To this end, the diagnostic wax-up, preparation guides, and putty matrix used to create the provisional restorations were essential to the communication process, proving instrumental in aiding both dentist-laboratory and dentist-patient communication during the treatment planning stages.12 By developing an ideal treatment plan with proper communication and execution, the goals of treatment were met and patient satisfaction was achieved.
ACKNOWLEDGEMENT
The author wishes to acknowledge Adrian Jurim from Jurim Dental Studios in Great Neck, NY, who fabricated the ceramic restorations featured in this article.
References
1. Jones LA, Robinson MY. A case study: esthetic and biologic management of a diastema closure using porcelain bonded restorations for excellent and predictable results. Journal of Cosmetic Dentistry. 2002;18(3):72-83.2. Gurel G. The Science and Art of Porcelain Laminate Veneers. Chicago, IL: Quintessence Publishing. 2003.
3. Garcia LT, Bohnenkamp DM. The use of diagnostic wax-ups in treatment planning. Compend Contin Educ Dent. 2003;24(3):210-214.
4. Snow SR. Strategies for successful esthetic dental treatment. J Calif Dent Assoc. 2007;35(7):475-484.
5. Kinderknecht KE, Kupp LI. Aesthetic solution for large maxillary anterior diastema and frenum attachment. Pract Periodontics Aesthet Dent. 1996;8(1):95-102.
6. Grel G. Predictable, precise, and repeatable tooth preparation for porcelain laminate veneers. Pract Proced Aesthet Dent. 2003;15(1): 17-24.
7. Stabholz A, Zeltser R, Sela M, Peretz B, et al. The use of lasers in dentistry: principles of operation and clinical applications. Compend Contin Educ Dent. 2003;24(12):935-948.
8. Kokich VO, Kokich VG, Kiyak HA. Perceptions of dental professionals and laypersons to altered dental esthetics: asymmetric and symmetric situations. Am J Orthod Dentofacial Orthop. 2006;130(2): 141-151.
9. Rouse JS. Full veneer versus traditional veneer preparation: a discussion of interproximal extension. J Prosthet Dent. 1997;78(6): 545-549.
10. Nash RW. Ultrathin porcelain veneers: esthetics without aggressive tooth reduction. Contemporary Esthetics and Restorative Practice. 2007;11(11):12-17.
11. Parker MW. The significance of occlusion in restorative dentistry. Dent Clin North Am. 1993;37(3):341-351.
12. Chaimattayompol N, Wong SX. Diagnostic management of interdental spacing. J Prosthet Dent. 2000;84(4): 467-469.
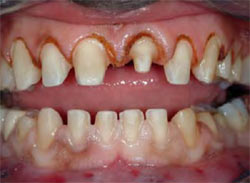
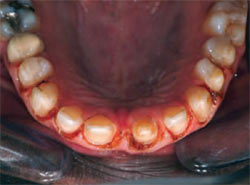
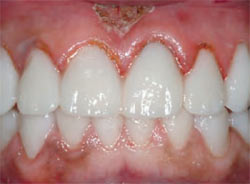
 Figure 1 and Figure 2 Preoperative fullfacial and close-up views of the patient and his smile. The midline diastema is obvious, as is the tooth discoloration, particularly of tooth No. 9. | 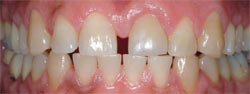 Figure 3 This preoperative retracted view of the patient demonstrates his end-to-end bite relationship. This would be altered to a normal overbite and overjet, with anterior guidance within the patient's envelope of function. 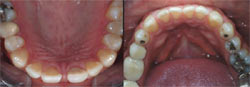 Figure 4 and Figure 5 Maxillary and mandibular occlusal view photographs were taken of the patient as part of the initial examination and forwarded to the laboratory for creation of the diagnostic wax-up. Note the midline diastema. The size and shape of the patient's teeth would be changed in the final restorations. | |
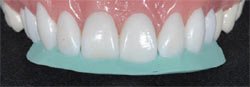 | 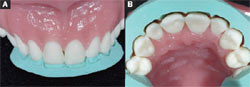 | |
| Figure 6 Photograph illustrating how a diagnostic wax-up is used to demonstrate how a patient's smile would be changed. A putty matrix/reduction guide is in place on this wax-up. Note: this wax-up is not of the current case. | Figure 7A and Figure 7B Facial and palatal photographs illustrating how a preparation guide is used to assist in the reduction of the affected teeth. Note: this putty matrix/reduction guide is not of the current case. | |
 |  | |
| Figure 8 Facial view of the completed maxillary and mandibular preparations. | Figure 9 Occlusal view of the maxillary preparations after alteration of the gingival zeniths. Note that the gingival zeniths have been moved in a mesial direction to allow for the new position of the restorations. | |
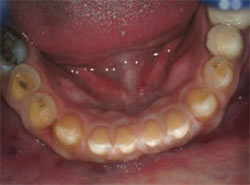 |  | |
| Figure 10 Occlusal view of the mandibular preparations demonstrating the reduction and movement effect of the slice-preparation technique. | Figure 11 View of the provisional restorations, which are critical to the success of the case because they serve as a blueprint for the final restorations. | |
 |  | |
| Figure 12 Close-up retracted view of the provisional restorations demonstrating the new bite relationship of the overbite and overjet that were copied from the diagnostic wax-up. | Figure 13 Final postoperative full-facial view of the patient in natural smile. | |
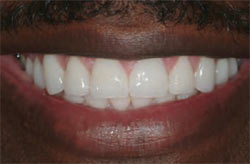 | 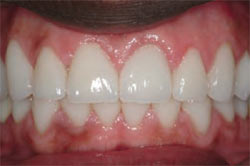 | |
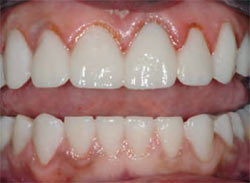
| Figure 14 Final postoperative close-up view of the patient in natural smile. Note the natural-looking and esthetic length-to-width ratio of the teeth and seamless color blending of the restorations. | Figure 15 Final postoperative retracted view demonstrating the patient's corrected bite relationship. | |
| About the Author | ||
 Thomas E. Dudney, DMD Thomas E. Dudney, DMD Private Practice Aesthetic, General, and Restorative Dentistry Alabaster, Alabama | ||



