Laser-Assisted Crown Lengthening
V. Kim Kutsch, DMD
Lasers have been used in dental soft tissue treatment since the early 1980s. The pioneering use of lasers in dental soft tissue procedures involved oral maxillofacial surgery. Pick1 introduced the CO2 laser gingivectomy for periodontal surgery in 1985, and further research by Myers2 with the Nd:YAG laser resulted in the first soft tissue dental laser developed specifically for the dental profession in 1990. Advances in diode technology have made diode lasers the standard among lasers in soft tissue procedures today. More recently, hard tissue lasers like the Er:YAG and Er,Cr:YSGG have been developed that provide a wide range of applications on dental and osseous tissues.3,4 Since laser technology’s first introduction in dentistry, the adoption of lasers and the diversity of applications have grown steadily. Lasers are currently proving very effective in a broad range of restorative and esthetic procedures, including crown lengthening.5
Discussion
In clinical practice there are many reasons that a clinician may elect to perform a crown-lengthening procedure. Typical reasons for crown lengthening involve violation of the biologic width of the periodontal tissues. The biologic width is the measurement from the free marginal gingival to the osseous crest level. A normal biologic width includes the sulcus depth, junctional epithelium, and connective tissue attachment measurements. This metric has been determined to be 2.04 mm in healthy tissue,6 but while absolute values determine a statistical average, they do not reflect variations in individual clinical situations. However, for practical purposes, it is a safe course to consider that the biologic width should be about 3 mm. When teeth are fractured and additional vertical ferrule is needed for restoration retention, or have carious lesions that approach the osseous crest and impinge on this normal biologic width, placement of a restoration requires a surgical recontouring of the hard and soft tissues. The goal of this procedure is to allow for adequate restoration of the tooth and to re-create a normal biologic width for the periodontium.
Restorations placed too close to the osseous crest violate this normal anatomy, resulting in a long-term chronic inflammatory response of the periodontium. This inflammatory response appears as a swollen red ring of tissue at the free gingival margin, and creates several practical problems for the patient. While this inflammatory response does not typically lead to further periodontal disease and alveolar bone loss, it can be an esthetic concern on anterior teeth in the smile zone, and generally bleeds easily. In addition to new fractures and decay, the patient may have an existing restoration that violates the biologic width and either needs to be replaced or the periodontal tissues should be recontoured.
Esthetic concerns are also reasons for crown lengthening. The normal architecture of the free gingival margin on maxillary anterior teeth demonstrates horizontal symmetry from the left cuspid to both centrals and then to the right cuspid. The free gingival margin of the lateral incisors is generally 1 mm to 1.5 mm coronal to this line.7 For patients who display the free gingival margins in their biggest smile, having a normal architecture of the gingival tissues ultimately improves the esthetic result.
Insurance Considerations
Like many emerging technologies and clinical techniques, the ability to perform a procedure less invasively may not meet established clinical criteria for third-party reimbursement. There are several alternative techniques that may be available to accomplish the clinical goal of normal biologic width. For example, if the problem results from an existing anterior crown margin placed too close to the osseous crest, the thin labial plate of bone may be easily removed without reflecting a flap by using a Wedelstaedt chisel marked at 3 mm. A fractured molar with a thicker plate of bone on the palate may require a more aggressive surgical technique by reflecting a full-thickness flap and reducing the bone level with a high-speed handpiece and a diamond or carbide bur. Crown lengthening assisted with laser technology is less invasive than using a scalpel and high-speed handpiece to accomplish the same end result. However, the CDT VII is very clear in the definition or clinical description of a crown-lengthening procedure (Code D4249):
“This procedure is employed to allow restorative procedure or crown with little or no tooth structure exposed to the oral cavity. Crown lengthening requires reflection of a flap and is performed in a healthy periodontal environment, as opposed to osseous surgery, which is performed in the presence of periodontal disease. Where there are adjacent teeth, the flap design may involve a larger surgical area.”8
Dentists and patients need to be aware of this requirement for third-party reimbursement when performing crown-lengthening procedures. The technique used, while it might be more desirable and less invasive, may not meet the requirement for reimbursement under this code.
Clinical Case
In addition to cutting and coagulating soft tissue, hard tissue lasers can also safely be used to removed both bone and tooth structure. Each laser wavelength has specific interactions with the different tissues. These tissue interactions are a result of a variety of issues, including: specific wavelength; absorption characteristics; tissue pigments and variations; pulse vs continuous delivery model; pulses per second or Hertz; power density and duration of laser exposure; and bare or conditioned fiber tip. Typically the laser/tissue interactions are thermal in nature, although the Er,Cr:YSGG laser hard tissue interaction is more complex. The Er,Cr:YSGG laser is an excellent choice for this application as it rapidly removes and recontours the gingival tissues with good hemostasis, and also very efficiently removes bony tissue.
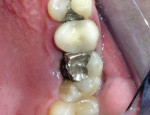
A 37-year-old healthy man was referred by a local practitioner for a crown-lengthening procedure on his maxillary right first molar. The tooth had a large existing mesial-occlusal amalgam restoration and previously had root canal treatment. The entire mesial and distal lingual cusps had fractured diagonally to the osseous crest level. The gingival tissue had collapsed into this space and hypertrophied onto the clinical crown (Figure 1). There was no sign of periodontal or peri-apical pathology on the radiograph (Figure 2), and no contraindications to treatment. After a review of the proposed treatment, reasonable treatment outcomes, potential complications, and alternative therapies, the patient elected to have the laser-assisted crown-lengthening procedure. Because of the anesthesia, hemostasis, and predictability of the procedure, the patient could be appointed to visit his referring dentist immediately after the crown lengthening to complete the crown preparation appointment on the same day.
After administration of local anesthesia, the redundant gingival tissue was removed with the Waterlase MD Er,Cr:YSGG laser (Biolase, Irvine, CA) set on S mode, at 2.0 W, 20 pulses per second, with 10% water and 30% air using an MG 6 tip 9 mm long in near contact with the tissue (Figure 3). The tissue was incised and removed, and the remaining tissue was reduced to the approximate desired level. An internal bevel was placed into the tissue to allow for re-establishment of a normal biologic width during the healing phase.
At this point there was good hemostasis and the lingual aspect of the palatal root was clearly visible. A crown finish margin was placed on the palatal root immediately apical to the existing fractured margin. This was accomplished with the same laser and tip set on H mode at 4.00 W, 15 pulses per second and 30% water and 60% airflow, with the tip in near contact and with a sweeping motion to establish a chamfer margin. This could also be accomplished with a high-speed handpiece and diamond bur. Note that if the crown margin will be slightly apical to the final free gingival margin, the osseous crest needs to be reduced to about 3 mm apical to the crown margin to allow for a normal biologic width.
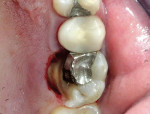
The bone was now reduced and recontoured to this level on H mode, at 3.0 W, 30 pulses per second and 20% water and 60% air, with the 9-mm tip in near contact (Figure 4). A mark can be made on the laser tip with a Sharpie pen at 3 mm to gauge the bone level during the procedure. The final surgical result displayed good hemostasis, with the osseous crest 3 mm below the new crown margin (Figure 5). The patient returned immediately to his referring dentist for the new crown preparation, final impression, and temporization procedure.
Conclusion
Lasers have become very useful clinical instruments in dental practice. The Er,Cr:YSGG laser is a versatile instrument for crown-lengthening procedures because it provides good hemostasis and recontouring of the gingival tissues and efficient recontouring of the osseous tissue as well. The procedure is less invasive than traditional surgical procedures and allows the entire crown lengthening and crown preparation to be performed in one appointment with predictable clinical results.
References
1. Pick RM, Pecaro BC. Use of the CO2 laser in soft tissue surgery. Lasers Surg Med. 1987;7(2):207-213.
2. Myers TD, Myers WD, Stone RM. First soft tissue study utilizing a pulsed Nd:YAG dental laser. Northwest Dent. 1989;68(2):14-17.
3. Yu DG, Kimura Y, Kinoshita J, Matsumoto K. Morphologic and atomic analytical studies on enamel and dentin irradiated by an ErCr:YSGG laser. J Clin Laser Med Surg. 2000;18(3): 139-143.
4. Kimura Y, Yu DG, Yamashita A, et al. Effects of ErCr:YSGG laser irradiation on canine mandibular bone. J Periodontol. 2001;72(9):1178-1182.
5. Dederich DN, Bushick RD. Lasers in dentistry separating science from hype. J Am Dent Assoc. 2004;135(2):204-212.
6. Vacek JS, Gher ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Perio Rest Dent. 1994;14: 154-165.
7. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51:24-28.
8. American Dental Association. CDT VII.ISBN #1-932305-96-3; 2006;23.
About the Author
V. Kim Kutsch, DMD
Private Practice
Albany, Oregon