Minimal Intervention Cosmetic Dentistry: Expanding Horizons in Cosmetic Dentistry
Wynn H. Okuda, DMD
Over the last few decades there has been a tremendous interest in recreating the natural appearance of dentition. Preservation of the human dentition through minimally invasive care is essential in today’s dentistry. As esthetic dental materials continue to evolve, so should the philosophical modality of treatment. The advancement in developing biomimetic dental materials gives dentists the opportunity to restore the human dentition in the most conservative manner. Delivering cosmetic dentistry in a more minimally invasive manner expands the number of treatment options for long-term success. In this article a variety of applications and benefits of minimal-intervention cosmetic dentistry (MICD) will be discussed.
PHILOSOPHY OF MINIMAL INTERVENTION IN COSMETIC RESTORATIVE TREATMENT
The current philosophy of MICD attempts to combine esthetics, prevention, remineralization, healing, adhesion, and restoration with the objective of removing carious damage in the least invasive manner. According to Mount and Ngo1,2 the potential for minimal intervention operative dentistry is dependent on:
1. the demineralization-remineralization cycle;
2. adhesion in restorative dentistry; and
3. biomimetic restorative materials.
In correcting problems associated with the human dentition, one must understand the importance of approaching treatment from the proper perspective. It is essential that esthetic results be attained with the least amount of tooth removal. MICD is a progressive idea that uses the technological advancements in material science to restore dentition to its natural beauty.
BIOMIMICRY: RECREATING NATURE
Biomimicry is defined as the application of engineering systems and modern technology to life forms in creating systems found in nature. One of the greatest challenges in esthetic dentistry is predictably creating color harmony between esthetic restorative materials and tooth structure. Understanding the structure of natural dentition and tooth morphology is essential in developing natural esthetics. Whether it is in the anterior or posterior dentition, being able to meet the optical as well as the physical properties of enamel and dentin is important in biomimicry.3
Understanding tooth coloration is a study of its color dimension: hue (actual color), chroma (the saturation of color), and value (the level of lightness and darkness of the color). While dentin is highly rich in hue, chroma, and fluorescence, it is covered by an exterior shell of enamel that is transparent and/or translucent with opalescent characteristics.4,5 Translucency is an important element that allows light to only pass through an object diffusely, therefore creating depth of color. This is an especially important property to have in a composite material to create a natural transition between tooth and restorative material or an invisible margin.6,7 This characteristic has been labeled the "chameleon effect."6
Esthetically, the different structures of a tooth reflect, refract, and absorb light at various degrees (eg, enamel rods, dentinal tubules, dentino-enamel junction, etc). When exposed to light, certain wavelengths are absorbed and reflected. However, the remaining light is refracted and the different qualities of color are seen.8 This is especially true for anterior teeth because light is readily abundant in comparison to its posterior counterparts. Therefore, for an esthetic material to be successful it must mimic tooth structure in the absorption, reflection, and refraction of light.
In MICD, biomimetic materials must match the optical properties of the surrounding tooth for the restoration to be esthetically successful. Presently, there are restorative materials that are biomimetic in their visual and physical properties. Biomimetic materials in conservative treatment include composite resin (eg, Gradia Direct X™, GC America, Alsip, IL; Filtek™ Supreme Plus, 3M ESPE, St. Paul, MN; and Aelite™ Composite Systems, BISCO Inc, Schaumburg, IL), resin-modified glass ionomer (eg, Fuji II LC, GC America; and Geristore Syringeable, Den-Mat Corporation, Santa Maria, CA), and ultra-conservative porcelain veneers (eg, Lumineers®, Den-Mat Corporation, DURAthin® Veneers, Experience Dental Studio, Provo, UT). These materials can be used in many different applications in MICD restorative dentistry.
WHY MINIMAL INTERVENTION COSMETIC DENTISTRY?
As dentists we are taught to treat as conservatively as possible. Whether to resolve defects resulting from carious lesions, correct failing existing restorations, or address esthetic-related reasons, restoring teeth to a natural finish is essential.9 By minimizing tooth preparations we can preserve dentition, reduce the potential negative effects of pulpal tissue, and safeguard hard tissue for future use.10
In addressing the esthetic needs of patients, cosmetic dentistry serves a tremendous purpose. With the progress of innovative esthetic materials, we are able to revisit cosmetic dental procedures with minimal intervention purposes in mind. MICD is a modality of treatment in recreating nature with minimal removal of tooth structure.
MINIMAL INTERVENTION APPLICATIONS
In applying MICD to esthetic problems, it is essential to look at the applications for long-term success. Materials have evolved over the last several years; composite resin is one example. Its progress allows dentists a chance to approach treatment in a variety of different ways.11
The latest generation of composite resins is now able to predictably blend to tooth structure, even using a simple layering technique (Figure 1 and Figure 2).12 These new high-tech composite resins exhibit excellent modulus of elasticity, fracture toughness, wear resistance, flexural strength, and compressive strength. In addition, their ease of handling, easy blending to tooth structure, and high polishability make it clinically effective for the dentist to achieve great results easily (Figure 3).13
With direct resin, conservative dentistry can be accomplished. From straightforward Class V restorations to direct resin veneering, MICD restorations can correct esthetic problems that affect the self-esteem and self-confidence of patients in a single appointment.
Case 1
A 15-year-old patient with severe postorthodontic decalcification was devastated after the orthodontic brackets were removed. Even after bleaching, the level of decalcification left her dentition compromised from an esthetic viewpoint (Figure 4). Because of her age it was decided that MICD treatment with no-preparation direct resin veneers was the best treatment option. These were completed along teeth Nos. 5 through 12 with a complex layering technique using a micro-fine hybrid composite (ie, Gradia Direct) (Figure 5 and Figure 6). Because the direct resin veneers were adhered to enamel, predictable long-term success can be attained. The restorations are still successful after 5 years (Figure 7).
Case 2
Decay of dentition is still part of our society (Figure 8). Caries is a bacterial disease process that must be first eliminated through methods of control.14 With advances in material science, the ability to remineralize and heal demineralized tooth structure with resin-modified glass ionomer (RMGI) reduces future caries incidence and allows for less tooth removal during the restorative phase.15,16 Conservative correction of this problem can be achieved with MICD using a combination approach with composite resin and RMGI.
In this case, after removal of decay with minimally invasive preparation burs (eg, Micro-prep bur kit, Brasseler USA, Savannah, GA), plaque and dental pellicle were removed with pumice paste along the teeth to be restored (Figure 9). A RMGI (Fuji II LC) was placed along the root area to reduce the chance of recurrent decay. Because the depth of shade of the RMGI is similar to natural dentition, blending to dentin is predictably possible (Figure 10).
Dental adhesion (One-Step® Plus, BISCO, Inc; All Bond 2®, BISCO, Inc; G-BOND™, GC America) can be accom-plished over the RMGI in a closed sandwich technique.17-20 To reproduce the shade of the root in this case, a biomimetic root-shaded composite resin was first incrementally layered on the cervical aspect (Gradia Direct X-A3.5). Next, a biomimetic enamel (Gradia Direct X-A2) was layered over the area where enamel was being replaced (Figure 11).7,21,22
Light-curing after each increment, the proper finishing of the restoration was accomplished with anatomically correct burs. Final finishing using composite resin finishing burs (Composite Resin Finishing and Polishing Kit, Brasseler USA) helped contour and marginate accurately. A 12-fluted composite finishing bur (#H50A, Brasseler USA) was used to develop initial anatomy. Then, a 20-fluted bur (H50AF, Brasseler USA) and finally a 30-fluted finishing bur (#H50F, Brasseler USA) refined the surface smoothness (Figure 13).24-26 The complex layering of composite resin creates the proper visual illusion and recreates lost dentition in the most conservative way.
Case 3
At times there are failures that can occur in dentistry. During those times MICD may be applicable in the correction of the failed area. Restorative failures can be corrected using proper materials and techniques (Figure 15).27 Fractured or failing restorations can be remedied using biomimicry with negligible sacrifice of tooth structure.
In this case an old, broken direct resin veneer was restored with a more highly engineered micro-fine hybrid composite resin (Gradia Direct X) without any tooth removal (Figure 16). Using a complex layering approach, composite resin was placed biomimetically so it blended with the adjacent dentition (Figure 17).
CONCLUSION
MICD gives the dentist options when correcting the appearance of the smile. Advancements in dental technology allow dentists to perform procedures with minimal invasiveness compared to the past. With the progressive development of biomimetic materials, conservative applications can be achieved in the area of esthetics. These bioactive materials optically and physically create a result that is highly indistinguishable from the natural dentition. With MICD, dentists are able to expand the horizon of cosmetic dentistry.
References
1. Mount GJ, Ngo H. Minimal intervention&8212;a new concept for operative dentistry. Quintessence Int. 2000;31(8): 527-533.2. Mount GJ. Minimal intervention dentistry: rationale of cavity design. Oper Dent. 2003;28(1):92-99.
3. Ubassy G. Shape and Color&8212;The Key To Successful Ceramic Restorations. Chicago, IL: Quintessence Publishing; 1993.
4. Muia P. Four-Dimensional Color System. Chicago, IL: Quintessence Publishing; 1993.
5. Duarte S Jr, Perdigão J, Lopes M. Composite resin restorations&8212;natural aesthetics and dynamics of light. Pract Proced Aesthet Dent. 2003;15(9):657-666.
6. Sieber C. Voyage: Visions in Color and Form. Chicago, IL: Quintessence Publishing; 1994.
7. Magne P, Holz J. Stratification of composite restorations: systematic and durable replication of natural aesthetics. Pract Periodontics Aesthet Dent. 1996;8(1): 61-68.
8. Terry DA. Direct reconstruction of the maxillary anterior dentition with composite resin: a case report. Pract Periodontics Aesthet Dent. 1999;11(3):361-367.
9. Milnar F. A minimal intervention approach to the treatment of a Class IV fracture. Journal of Cosmetic Dentistry. 2006;21(4): 106-112.
10. Mount GJ, Ngo H. Minimal intervention: advanced lesions. Quintessence Int. 2000;31(9):621-629.
11. Mitra SB, Wu D, Holmes BN. An application of nanotechnology in advanced dental materials. J Am Dent Assoc. 2003;134(10): 1382-1390.
12. Okuda W. Simplified posterior aesthetics using microhybrid composite resins: techniques for success. Pract Proced Aesthet Dent. 2004;16(2):135-142.
13. Kugel G, Perry R. Direct composite resin: an update. Compend Cont Educ Dent. 2002;23(7): 593-608.
14. Mount GJ, Ngo H. Minimal intervention: early lesions; Quintessence Int. 2000;31(9):536-546.
15. Hicks J, Garcia-Godoy F, Donly K, Flaitz C. Fluoride-releasing restorative materials and secondary caries. J Calif Dent Assoc. 2003;31(3);229-245.
16. Lin A, McIntyre NS, Davidson RD. Studies on the adhesion of glass-ionomer cements to dentin. J Dent Res. 1992;71(11):1836-1841.
17. McLean JW. Dentinal bonding agents versus glass-ionomer cements. Quintessence Int. 1996;27(10): 659-667.
18. Tay FR, Sidhu SK, Watson TF, Pashley DH. Water-dependent interfacial transition zone in resin-modified glass-ionomer cement/dentin interfaces. J Dent Res. 2004;83(8):644-649.
19. Trushkowsky RD, Gwinnett JA. Microleakage of Class V composite, resin sandwich, and resin-modified glass ionomer. Am J Dent. 1996:9(3):96-99.
20. Davidson CL. Glass-ionomer bases under posterior composites. J Esthet Dent. 1994;6(5):223-226.
21. Fahl N Jr, Denehy GE, Jackson RD. Protocol for predictable restoration of anterior teeth with composite resins. Pract Periodontics Aesthet Dent. 1995;7(8):13-22.
22. Fahl N Jr. Achieving ultimate anterior esthetics with a new microhybrid composite. Compend Contin Educ Dent. 2000;26(Suppl): 4-13.
23. Peyton JH. Finishing and polishing techniques: direct resin restoration. Pract Proced Aesthet Dent. 2004;16(4):293-298.
24. Barghi N. Surface polishing of new composite resins. Compend Cont Educ Dent. 2001;22(11): 918-924.
25. Lu H, Roeder LB, Powers JM. Effect of polishing systems on the surface roughness of microhybrid composites. J Esthet Restor Dent. 2003;15(5):297-304.
26. Da Costa J, Ferracane J, Paravina RD, et al. The effect of different polishing systems on surface roughness and gloss of various resin composites. J Esthet Restor Dent. 2007;19(4):214-224.
27. Okuda WH. Troubleshooting aesthetic dentistry. Dent Today. 2007;26(6): 66-70.
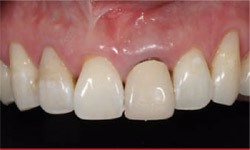 | 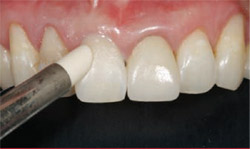 | |
| Figure 1 Preoperative photograph shows gingival recession along the central incisor. | Figure 2 Simple layering technique was used with Gradia Direct X. | |
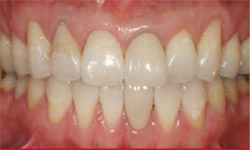 | 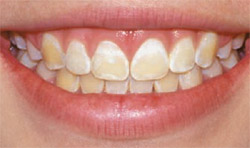 | |
| Figure 3 Esthetic correction was done to match the anatomic contours of the adjacent central incisor. | Figure 4 Severe postorthodontic decalcification can affect an individual's self-esteem and self-confidence. | |
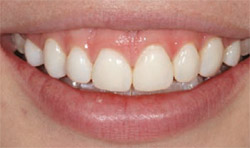 | 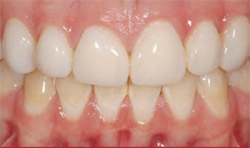 | |
| Figure 5 Direct resin veneers were placed on teeth Nos. 5 through 12 with micro-fine hybrid composite resin. | Figure 6 MICD was attained with no-preparation veneers. Complex layering technique recreated the natural appearance of anterior teeth. | |
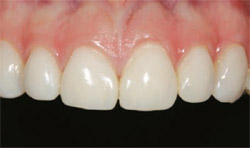 | 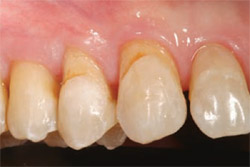 | |
| Figure 7 This 5-year postoperative photograph shows the success of direct resin veneers. | Figure 8 Root decay present on teeth Nos. 5 and 6. | |
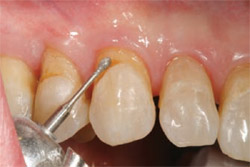 | 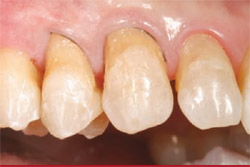 | |
| Figure 9 Micro-preparation burs were used for minimally invasive tooth removal. | Figure 10 Resin-modified glass ionomer was placed along the root to reduce recurrent decay. | |
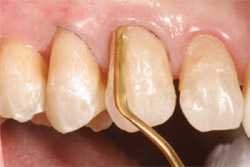 | 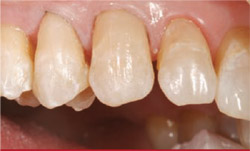 | |
| Figure 11 Biomimetic layers of composite resin were placed to recreate natural esthetics. | Figure 12 Complex layering with the new micro-fine hybrid created a depth of color similar to the natural dentition. | |
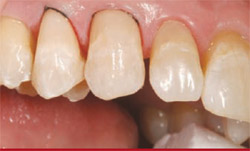 | 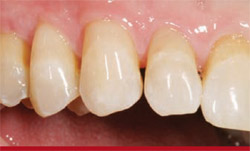 | |
| Figure 13 Preliminary finishing with anatomically contoured burs produced a natural surface contour. | Figure 14 Finishing disks, aluminum-oxide finishing cups and points, and a micro-diamond polishing paste attained an enamel-like finish and polish. | |
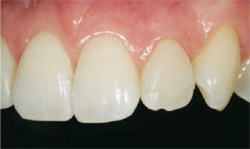 | 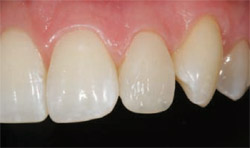 | |
| Figure 15 Fracture of an existing restoration can be remedied with an MICD approach. | Figure 16 Initial layers of biomimetic composite resin were placed in recreating this lateral incisor. | |
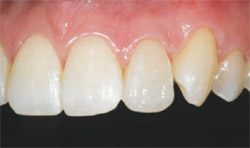 | ||
| Figure 17 Troubleshooting the esthetic failure (tooth No. 10) with a complex-layered direct resin veneer provided a conservative alternative to treatment. | ||
| About the Author | ||
 Wynn H. Okuda, DMD Wynn H. Okuda, DMD Past President and Accredit Member American Academy of Cosmetic Dentistry Private Practice Honolulu, Hawaii | ||



