Treatment Planning Decisions: Endodontics vs Implants
Gregori M. Kurtzman, DDS
Endodontic therapy has advanced to provide long-term clinical success, and preservation of the natural dentition is a primary goal of dentistry. Yet endodontic success is closely linked to the restorability of the coronal aspect of the tooth. Lack of sufficient coronal structure to retain a crown often leads to failure of the coronal seal and subsequent failure of the endodontic obturation.
Patients who present with significant coronal breakdown of a tooth present challenges with regard to treatment planning decisions for that tooth. Does the practitioner endodontically treat the tooth and augment that treatment with crown lengthening to permit sufficient ferrule (a band of natural tooth that is circumferentially grasped by the crown that prevents lateral displacement of the crown from the tooth) of the remaining root structure to allow restoration, or is it more prudent to extract the tooth and place an implant?
The literature has suggested that a 1.5-mm to 2-mm ferrule is minimally necessary to prevent fracture of the endodontically treated tooth and provide resistance to displacement of the fixed restoration.1-3 Unfortunately, with today’s improvements in adhesive dentistry, the emphasis has drifted away from the principle of the restorative ferrule. Practitioners may be relying too heavily on the strength of the bond to keep fixed prosthetic restoration margins sealed, and thought should be given to how much coronal structure remains when deciding if a tooth should be treated endodontically or replaced with an implant. These restorative decisions need to be made before the initiation of endodontic treatment, and the practitioner must determine which additional procedures will be necessary to achieve the restorative goals required.
Raise the Bridge or Lower the Water?
When analyzing how a tooth may be restored after endodontic treatment, one has to determine if sufficient root length remains to allow stability of the tooth once it is restored. Is there adequate supracrestal tooth structure present to provide a restorative ferrule? What ancillary procedures may help increase the ratio of supracrestal tooth to ferrule?
Osseous Crown Lengthening to Improve Restorative Ferrule
Traditionally, when insufficient tooth structure presented supracrestally, osseous crown-lengthening procedures were employed to increase the available coronal tooth structure.4 This presents challenges in treatment. When the tooth requiring treatment is bound by adjacent teeth, osseous crown lengthening will require the removal of crestal bone on the adjacent teeth to create osseous slopes that will allow soft tissue maintenance. One cannot just remove bone around an individual tooth because this leads to isolated pocketing and abrupt slopes in the bone, which lead to adjacent bone loss as the body attempts to create gentle slopes that it can maintain over time. So we can see that to create adequate coronal tooth structure for restorative purposes the periodontal structures adjacent to that tooth may have to be compromised.
Additionally, the removal of crestal bone may expose furcations on posterior teeth that would complicate home care and expose other areas that may be difficult to maintain over the long term. This may also be a factor in maxillary first premolars, which typically have a mesial root concavity that itself can create restorative challenges. When the tooth being treated has a short cervical trunk or the furcation is already at or just above the crestal margin, removal of additional bone may be contraindicated and extraction of the tooth and subsequent placement of an implant may be a more prudent option.
Forced Orthodontic Eruption
An alternative to osseous crown lengthening when additional tooth structure is needed restoratively is the use of forced orthodontic eruption.5 After the completion of endodontic treatment, orthodontic forces are used to erupt the tooth cor-onally, exposing more root structure upon which a ferrule may be placed.6 When considering this option, one needs to assess how much root length will remain within the osseous housing and whether this will allow an adequate crown-to-root ratio to maintain tooth stability over a period of time. As with crown lengthening, forced eruption of multi-rooted teeth may create furcation issues and may be a contraindication to this treatment modality. This approach does work well on single-rooted teeth.7
Under normal orthodontic extrusion, slow forces with low intensity are exerted on the tooth. As the tooth extrudes, the crestal bone and gingival apparatus move together coronally. When heavier traction forces are exerted, as seen in rapid extrusion, coronal migration of the tissues supporting the tooth is less pronounced, as the rapid movement exceeds their capacity for physiologic adaptation, and the tooth erupts coronally beyond the crestal bone.8 When rapid extrusion is used it must be followed by an extended period of retention to allow remodeling and adaptation of the periodontium to the new tooth position.9
Clinical Decisions For Single-rooted Teeth
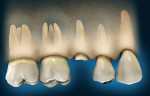
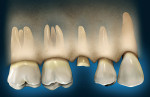
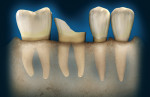
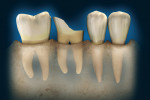
A patient presents with coronal breakdown of a single-rooted tooth that is at or close to the crestal bone margin (Figure 1). First, the length of the root subcrestally must be determined. Is there sufficient root length that movement of the crestal margin in relation to the coronal of the remaining tooth will not compromise the crown-to-root ratio of the restored tooth? If the answer is “yes,” then there are two options: clinical crown lengthening (Figure 2) or orthodontic extrusion (Figure 3). Should the answer be “no,” then extraction and replacement with an implant is the indicated treatment.
Clinical Decisions for Multi-rooted Teeth
A common occurrence involves the presentation of a molar with significant coronal breakdown either as a result of fracture or decay (Figure 4). The presence of furcations present unique variables compared to single-rooted teeth. When analyzing the restorability of the molar, practitioners need to ask: Will repositioning the crestal bone margin either through osseous crown lengthening (Figure 5) or extrusion (Figure 6) expose the furcation and complicate maintenance? Teeth with short cervical trunks limit what treatments may be performed to provide restorative ferrules. Teeth with long cervical trunks or fused roots may be better suited to these procedures and provide clinical outcomes that can be maintained over the long term. When these objectives cannot be met, extraction and implant placement offer a better prognosis.
Conclusion
Dentistry is restoratively driven, supplemented by endodontic and surgical components. When a tooth cannot be restored, then it does not matter whether endodontic treatment can be or is rendered. Treatment planning decisions need to focus on the restorability of the tooth when deciding what treatment will provide reasonable long-term success. If the tooth can be restored, then pursuing endodontic treatment is the best treatment decision. But when this cannot be accomplished or the restorative prognosis cannot provide reasonable long-term success, then extraction and implant placement is the more prudent treatment option.
References
1. Libman WJ, Nicholls JI. Load fatigue of teeth restored with cast posts and cores and complete crowns. Int J Prosthodont. 1995;8(2):155-161.
2. Tan PL, Aquilino SA, Gratton DG, et al. In vitro fracture resistance of endodontically treated central incisors with varying ferrule heights and configurations. J Prosthet Dent. 2005;93(4):331-336.
3. Ichim I, Kuzmanovic DV, Love RM. A finite element analysis of ferrule design on restoration resistance and distribution of stress within a root. Int Endod J. 2006;39(6):443-452.
4. Planciunas L, Puriene A, Mackeviciene G. Surgical lengthening of the clinical tooth crown. Stomatologija. 2006;8(3):88-95.
5. Camargo PM, Melnick PR, Camargo LM. Clinical crown lengthening in the esthetic zone. J Calif Dent Assoc. 2007;35(7):487-498.
6. Kocadereli I, Taşman F, Güner SB. Combined endodontic-orthodontic and prosthodontic treatment of fractured teeth. Case report. Aust Dent J. 1998;43(1):28-31.
7. Delivanis P, Delivanis H, Kuftinec MM. Endodontic-orthodontic management of fractured anterior teeth. J Am Dent Assoc. 1978;97(3):483-485.
8. Bach N, Baylard JF, Voyer R. Orthodontic extrusion: periodontal considerations and applications. J Can Dent Assoc. 2004;70(11): 775-780.
9. Antrim DD. Vertical extrusion of endodontically treated teeth. US Navy Med. 1981;72:23-28.
About the Author
Gregori M. Kurtzman, DDS
Private Practice
Silver Spring,Maryland