The Perio–Restorative Interface
Francis G. Serio, DMD, MS, MBA
Tooth-colored composite resins. Composite veneers. Porcelain veneers. All-ceramic crowns. Bleaching—at home, in office, or both. Adult orthodontics. Orthognathic surgery. These are the terms usually heard in conversations about cosmetic or esthetic dentistry. Very little is usually said about the relationship of the gingiva and other soft tissues to the teeth. But without paying attention to these factors, all of the time, effort, and expense invested in making teeth straight, whiter, and more attractive may all be for naught. More than lip service (pun intended) must be paid to the soft tissues of the mouth and perioral area, the lips, the gingiva, and the residual ridges in the esthetic zone to maximize the esthetic result sought by patients and practitioners alike. This article will outline the soft tissue factors that will enhance the overall result of esthetic dental treatment.
Sometimes it is easiest to appreciate what should be done by seeing what not to do. Figure 1A and Figure 1Bshow a set of finished all-ceramic crowns from the maxillary right canine to the maxillary left canine. In this example, note the relationship between the adjacent crowns and the crowns and the soft tissues. First, there is an elongated mesial contact of the maxillary central incisors that obliterates the gingival embrasure. This has squeezed the gingival papillae out of the embrasure and has most likely impinged on the biologic width. The facial margin of the right central incisor is slightly open, allowing for plaque to accumulate. The gingival margin of the right lateral incisor is significantly apical to its esthetic position; instead of making this tooth the shortest in the esthetic zone, as it should be, it makes it the longest. The crowns are smooth, with no detail or grooving, and do not allow for the natural breakup of light reflecting from the crown surfaces. Transitional line angles are misplaced, resulting in central incisors that appear too wide and lateral incisors that appear too narrow in appearance. The palatal view shows additional problems. The transitional line angles are incomplete, especially on the mesial aspect of both lateral incisors, and the crown margins are rough and do not meet the prepared finish lines throughout. The resulting inflammation is difficult to control even with exemplary oral hygiene.
So, where to begin? “Extreme Makeover” is not just the name of a popular television program anymore; it has become a part of our lexicon. While the results are dramatic, relatively little time is spent on the television shows presenting the thought process by which such life-changing results are possible. Much has been written about the esthetic examination, smile analysis, and esthetic treatment planning in the dental literature.1 With all of the noise, it is sometimes difficult to see a clear path to develop the trifecta of dentistry— examination, diagnosis, and treatment plan.
THE ESTHETIC EXAMINATION
More than 20 years ago, Dr. Leonard Abrams developed a comprehensive approach to the esthetic examination (personal communication, 1986). While much of his approach may be familiar in one form or another, relevant aspects will be presented here along with treatment possibilities to enhance the esthetic outcome.
The Patient
The first step is to meet the patient. Careful listening, proper interpretation of what the patient says, and frank discussion are important at this stage. The patient’s expectations must be both clear and achievable. Sometimes in an effort to “turn back the clock,” patients may have unrealistic expectations of what can be done. The presence of periodontal attachment loss, pathologic migration, a high smile line, or loss of soft or hard tissues may hamper the achievement of an ideal esthetic result. Obtaining as much historic information as possible—old photographs, radiographs, charting, and other records—is helpful. Patients must be educated about the realities and limitations of modern esthetic care.
The dentist’s ability to meet these expectations must be carefully assessed as well. Not all dentists have the same level of skill in providing esthetic care. It is the wise dentist who knows when he or she will be unable to meet the high but realistic expectations of a patient and instead refers that patient to a more experienced practitioner. Patients appreciate the efforts their dentist makes to place them in situations where they will receive the best possible care. Collaboration with an esthetic facial surgeon must also be considered.
The Face
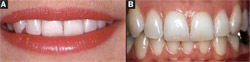
Once a relationship has been established with the patient, it is time to meet the face. The most important thing here is to determine if the interpupillary line is square with the mid-sagittal plane. When these two lines intersect at a right angle, the interpupillary line will then become part of the decision on where to locate both the gingival margins and incisal edges. The line connecting the most apical aspects of the gingival margins of the canines will be parallel to the interpupillary line. The gingival margins of the central incisors will be even and slightly coronal to the canine margins (Figure 2). The gingival margins of the lateral incisor will fall along this line from the canines to the central incisors or slightly coronal to the margins of the central incisors and canines. If at all possible, the gingival margin of the lateral incisor should not be apical to those of the canine and central incisor (refer back to Figure 1A).2 Lip symmetry and profile are also assessed at this step. Some patients may have asymmetrical lip movements (Figure 3). Lip support, both in frontal and profile views, is analyzed and the need for additional lip support may contribute to the design of the final restorations.
The Mouth
If the teeth and intraoral soft tissues are front and center on the stage, the lips serve as the curtain. In meeting the mouth, the upper lip line, lower lip line, and relationship of the incisal edges to the lower lip are determined. A high lip line, particularly with prominent teeth and thin gingiva, presents the ultimate challenge for any type of treatment in the esthetic zone (Figure 4). Patients with these features are more prone to recession and the opening of interdental embrasures even when the gentlest of techniques are used. Horizontal tooth display and the shape of the vestibules are noted. Restorative material selection may differ in patients who show their molars when smiling from those who do not (Figure 5).
The mid-sagittal plane is established when meeting the face. This line is then compared to the dental midline. The midline could have shifted due to eruption patterns, missing teeth, or trauma. Correction of this misalignment may or may not be necessary depending on the patient’s desires (Figure 6A and Figure 6B).
Gingival characteristics are then determined. The following characteristics listed below should be noted. Some are explained in more detail after the list.
• Contour
• Thickness of the gingiva and root prominence (may indicate a propensity for gingival recession)
• Underlying root prominence
• Open embrasures
• Altered passive eruption
• Excessive gingival display
• Collapsed edentulous ridge
• Isolated gingival defects
Open Embrasures
Known as the “dreaded black triangles,” patients must be aware that the closure of these embrasures depends on the local anatomy. It has been determined that papilla will fill an embrasure if the distance from the apical extent of the interproximal contact to the crest of the bone is 5 mm or less.3 Patients who have active periodontal disease must be warned that it is possible for the embrasures to be more open when the inflammation is controlled.
Altered Passive Eruption
Altered passive eruption occurs when the gingival margin does not migrate apically to the cervical area of the tooth during adolescence.4 This migration failure is often related to the thickening of the facial alveolar bone adjacent to the cementoenamel junction (CEJ). The result is that the anterior teeth appear short and boxy. Normally, the maxillary central incisor is between 10 mm and 11 mm high and about 8 mm wide (width-to-height ratio 0.75:0.8).2 Figure 7and Figure 8 show the shortened tooth appearance due to altered passive eruption. Periapical radiographs will give some indication of the true size of the anatomic crown (Figure 9).When the bone is coronally positioned and/or the CEJ cannot be felt with a periodontal probe, esthetic crown lengthening, perhaps with osseous recontouring, is indicated (Figure 10 and Figure 11).5,6 Performing a gingivectomy in these circumstances will result in gingiva regrowth in about 6 months’ time.
Excessive Gingival Display
When not related to altered passive eruption, the excessive display could be skeletal where there is vertical maxillary excess. In this situation, orthognathic surgery is necessary to correct the deformity.
Collapsed Edentulous Ridge
A loss of teeth often leads to resorption of the residual ridge. This resorption may be horizontal, vertical, or a combination of both.7 Severe resorption or traumatic damage may make construction of an esthetic pontic in a fixed prosthesis difficult (Figure 12A and Figure 12B). Autogenous connective tissue grafting can reconstruct these lost dimensions to allow for the fabrication of an esthetic ovate pontic (Figure 12C).8 One major advantage of autogenous connective tissue grafting is the stability of the dimensions of the graft after initial healing. These grafts maintain 95% of their initial thickness more than 10 years after surgery. At times, patients present with multiple esthetic challenges that may be solved with a stepwise surgical and restorative approach. The patient seen in Figure 13A and Figure 13B has been stable for 11 years after her reconstruction, which included a submucosal connective tissue graft and an onlay connective tissue graft7,9 with an ovate pontic for the maxillary right central and lateral incisors.
Isolated Gingival Defects
Isolated recession is a common problem among patients with high levels of oral hygiene. When an example such as the one in Figure 14A is shown to general dentists during continuing education presentations, the treatment of choice for many is to restore the facial defect with composite. Unfortunately, that approach results in a very unattractive fang. Autogenous connective tissue grafting can predictably cover these roots without any type of restoration (Figure 14B).10-13 The amount of root coverage is directly related to the height of the interproximal bone.14
CONCLUSION
After the gingival characteristics have been determined, the esthetic exam is completed by looking at the tooth characteristics and phonetics. When performing fixed prosthodontics care, it is important that the interim restorations be viewed as provisional final restorations, not just temporary restorations. While some may say that this is elementary, it bears repeating that defining the final prosthesis to as full a degree as possible in acrylic or composite resin to achieve final tooth contour, lip support, phonetics, and hard and soft tissue interfaces will result in a more predictable final result. A model of the final provisional restoration should be provided to the ceramist as a guide to the final prosthesis.
Esthetic dentistry is a multidisciplinary segment of our profession. A broader view of the patient’s presenting features is necessary to deliver the best esthetic dental care. The soft tissues, either those that are inflamed or somehow damaged, can detract from the final esthetic result.15 Proper treatment of the gingiva and resorbed ridge can significantly enhance any treatment outcome.
References
1. Garber DA, Salama MA. The aesthetic smile: diagnosis and treatment. Periodontol 2000. 1996;11:18-28.2. Chiche G, Pinaut A. Esthetics of Anterior Fixed Prosthodontics. Chicago, Quintessence, 1994;180.
3. Tarnow DP, Magner AW, Fletcher P. The effect of the distance of the contact point to the crest of the bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12): 995-996.
4. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in adults. Alpha Omegan. 1977;70(3):24-28.
5. Allen EP. Surgical crown lengthening for function and esthetics. Dent Clin North Amer. 1993;37(2):163-179.
6. Jorgensen MG, Nowzari H. Aesthetic crown lengthening. Periodontol 2000. 2001;27:45-58.
7. Seibert JS. Reconstruction of deformed, partially edentulous ridges, using full thickness onlay grafts. Part I. Technique and wound healing. Compendium. 1983;4(5): 437-443.
8. Langer B, Calagna L. The subepithelial connective tissue graft. J Prosthet Dent. 1980;44(4):363-367.
9. Seibert JS, Salama H. Alveolar ridge preservation and reconstruction. Periodontol 2000. 1996;11:69-84.
10. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
11. Rose LF. Surgical therapies for the treatment of gingival recession. Inside Dentistry. 2006;2(4):66-70.
12. Allen EP. Noncarious cervical lesions: graft or restore? J Esthet Restorative Dent. 2005;17(6): 332-334.
13. Bouchard P, Malet J, Borghetti A. Decision-making in aesthetics: root coverage revisited. Periodontol 2000. 2001;27:97-120.
14. Miller PD Jr. A classification of marginal tissue recession. Int J Periodont Restorative Dent. 1985;5(2):8-13.
15. Donovan TE, Cho GC. Predictable aesthetics with metal-ceramic and all-ceramic crowns: the critical importance of soft-tissue management. Periodontol 2000. 2001;27:121-130.
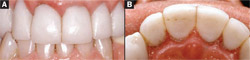 | ||
| Figure 1A and Figure 1B Adverse effect of crowns on the periodontium. (A) Facial view of all-ceramic crowns with associated gingival inflammation. Crown contours crowd the papilla out of the interdental embrasures, the interproximal contacts are too long, the margins impinge on the biologic width, and the crown margins are rough. (B) Rough margins and improper transitional line angles contribute to inflammation. | ||
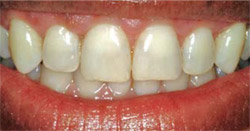 | 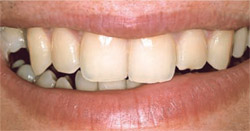 | |
| Figure 2 The natural relationship of the gingival margins of the anterior teeth to each other. | Figure 3 Asymmetrical lip function and irregular incisal edges. | |
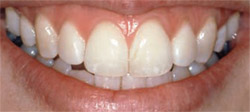 | 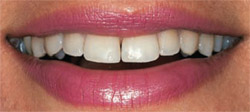 | |
| Figure 4 The most challenging esthetic patient; note the high smile line, thin gingiva, and prominent teeth. Notice how the incisal edges parallel the lower lip. | Figure 5 Patient with a wide smile has light reflecting from the metallic restoration on the mesial of the maxillary left first molar. | |
 | ||
| Figure 6A and Figure 6B Shift of the maxillary midline. (A) The shift in the midline is barely noticeable with the lips in repose. (B) The maxillary midline has shifted to the left after a LeFort 1 fracture in a motor vehicle accident. | ||
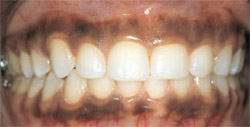 | 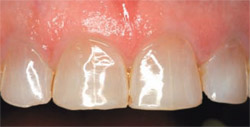 | |
| Figure 7 An example of altered passive eruption. The anterior teeth are short and boxy looking, with uneven gingival margins. | Figure 8 Altered passive eruption in a patient desiring veneers. This is the pretreatment view of the teeth. | |
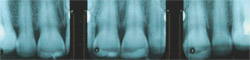 | ||
| Figure 9 Periapical radiographs of the patient in Figure 8 give an estimation of the true size of the anatomic crown. | ||
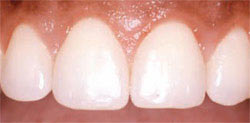 | 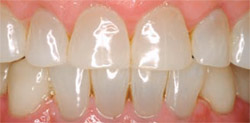 | |
| Figure 10 Esthetic crown-lengthening of the patient in Figure 7. Osseous recontouring established a more esthetic appearance of the teeth and gingival margins. | Figure 11 After esthetic crown lengthening in the patient in Figure 8. The patient is pleased with her new look and is undecided on whether or not to have veneers placed. | |
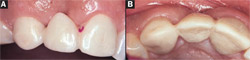 | 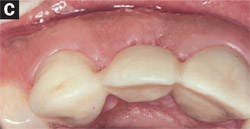 | |
| Figure 12A and Figure 12B An example of a collapsed edentulous ridge. These are both pretreatment views of the ridge. | Figure 12C Ridge contour after an autogenous submucosal connective tissue graft.There is plenty of ridge to form an ovate pontic seat in the soft tissue. | |
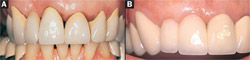 | 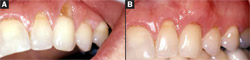 | |
| Figure 13A and Figure 13B Pre- and posttreatment of a patient with multiple esthetic problems including irregular gingival margins and a deficient ridge over the maxillary right lateral incisor. This patient was treated with a submucosal connective tissue graft, onlay connective tissue graft, and ovate pontics for the maxillary right central and lateral incisors. The posttreatment view is at 10 years. | Figure 14A and Figure 14B (A) Severe recession and attrition due to overzealous oral hygiene. (B) An autogenous submucosal graft covered the root completely. The slight area of "recession" is where the enamel of the CEJ was lost. There is no deep probing in this area but a combination of connective tissue and junctional epithelium attachment. | |
| About the Author | ||
 Francis G. Serio, DMD, MS, MBA Francis G. Serio, DMD, MS, MBA Professor and Chairman Department of Periodontics and Preventive Sciences University of Mississippi School of Dentistry Jackson, Mississippi | ||




