Restoring the Functional Zone: Correcting Anterior Constriction with Centric Relation-Based
Leonard A. Hess
One of the great benefits of practicing dentistry is practice autonomy. The patient and the dentist develop a relationship that includes trust in the clinician and need-fulfillment for the patient. The clinician’s skills are developed through practice and continued education. Judgment and reasoning are acquired through experience, whether good or bad. Treatment planning and restorative techniques are a free choice for the dentist as long as the standard of care remains inviolate.
The problem with this great autonomy is an ever-changing personal standard of care. As continuous students, dentists are always reminded of something that in hindsight could have been done better or differently. It seems that most clinicians want their work to be more predictable and longer-lasting. By refusing to become professionally stagnant, a dentist is a different clinician than he or she was last year. That means next year the dentist will be different as well. Does this imply that one should always use the latest and greatest bonding agent or newest restorative material? Perhaps it could also mean that clinicians become more aware of the peripheral ele-ments of success and failure. Is this the year that you begin to treat not only the symptom but recognize the cause? Is it time to become a comprehensive provider who understands a complex (masticatory) system, and not a care provider who only selectively focuses on individual components?
As the age of beauty burns ever brighter, more and more people seek solutions from the dental profession. People want to look younger and feel better about themselves and they understand that dentistry can provide a material result. Patients only recognize a need to look better and can often distinguish esthetic faults in their smile. Color is a given, but this author has seen more interest by patients involving excessive wear, chipping, and cervical defects. A simple smile makeover may not be so simple anymore. Why are teeth chipped and worn? Why are abfractions and wear facets present? This is where being a comprehensive and occlusion-focused provider will matter most. Simply making teeth whiter and longer is not treating the cause. Advancing age is not the only cause for worn-out teeth.
Dr. Peter Dawson makes a great point with his concept of collateral damage. “The point that should not be missed is that masticatory system disorders are rarely ever confined to a single structure. There will almost always be collateral effects from the disorder in the joints, the teeth, or the muscles.”1
Case Presentation
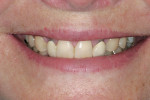
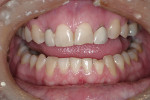
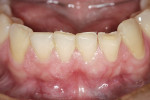
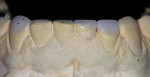
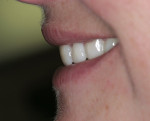
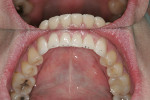
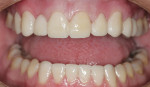
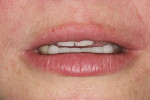
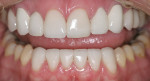
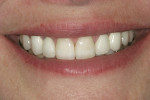
The patient had been coming to the practice for years. As is often the case, the patient was aware of her esthetic problems, but her understanding of the functional issues and reasons to fix them required education. Her readiness to proceed with care was simply a combination of accepting the problems and understanding them and fitting the treatment into her life. Her esthetic deficits included color, generalized anterior wear with severe wear on some teeth, width/length issues, and position of the incisal edges (Figure 1, Figure 2, Figure 3).
Functionally, the situation was nearing a terminal state. The combination of anterior wear and poor canine positioning had resulted in left and right anterior and posterior group function upon lateral movement of the mandible. The lateral incisor crowns were dictating the lateral guidance, resulting in the wear and interferences. The patient had crowns placed on teeth Nos. 7 and 10 more than 15 years ago. The crowns were placed to improve her smile as a result of pegged lateral incisors. Unfortunately, the crowns were doomed to exasperate a functional problem from the start. The incisal edge position and lingual contours further violated the patient’s envelope of function, resulting in a constricted anterior zone.
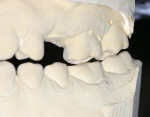
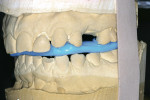
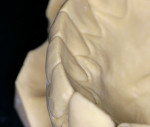
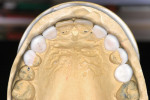
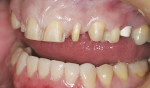
Considering the varied lingual surfaces of maxillary anterior teeth, over-contouring one or more of them can have a very destructive effect on occlusal function.2 The patient described years of an “uncomfortable bite” that never felt normal to her. She also described a history of muscle fatigue when chewing tough food, muscle soreness, tension, and headaches in her temporal muscles. Occlusal analysis revealed the source of the patient’s wear and muscle problems. When placed in centric relation, the patient’s only contact was on teeth Nos. 15 and 18 (Figure 4). This resulted in a profound discrepancy between centric relation and the patient’s maximum intercuspation. To achieve this habitual position, her mandible was required to “slide” almost 2 mm anteriorly from centric relation. Considering the great amount of wear already present on the lower anterior teeth, iatrogenic root canal treatment would be necessary on these teeth to restore them to her habitual bite position. Even if that was an option, the reduction necessary on the lingual aspect of the maxillary anterior teeth to allow normal-length lower incisors was prohibitive, or again would require root canal treatment of these teeth. Something had to be done. But what?
Comprehensive Planning
When presented with a complicated problem, it is often best to break the problem into its manageable components and then reorganize them in a systematic fashion to allow a resolution. Consistency in the planning stages makes for predictable success. Proper planning allows the patient and dentist to be adequately educated and reaffirms their commitment to the process ahead. It is always important to remember that the patient must be just as committed to the process as the dentist.
The data collected should include a complete medical history, periodontal exam, any necessary radiographs, impressions, face-bow, bite records in centric relation and maximum intercuspation, photographs, and a temporomandibular joint (TMJ) workup. The patient was referred to a periodontist for placement of an implant in the No. 13 position and for crown lengthening to improve the width-to-length ratios of the lateral incisors. The TMJ workup included measuring the range of motion, palpation of the muscles of mastication, loading the joints through bimanual manipulation, and Doppler auscultation. It is important that any case involving an occlusal scheme change start with asymptomatic joints. The joints should be pain-free when firmly loaded with bimanual manipulation, and function without pain from a disk derangement.1 If the joints are not comfortable when they are loaded, then they are not in centric relation. The Doppler auscultation provides an added tool to determine the degree of derangement present in the joints.3 This case in particular necessitated an occlusal change to allow functional and esthetic restoration. The repeatable position that is centric relation will provide the starting point at which to begin.
Determining the position and health of the joint is the starting point of any restorative case. Centric relation is not a forced position, and it is not dictated by the teeth. It is the anatomic position that the mandible is designed to function from in relation to the maxilla. The condyles will still rotate and translate down the eminence. However, when the elevator muscles are reaching a point of full contraction, centric relation provides a fixed axial position for the condyles. The position is achieved when the condyle and disk are seated into the most superior position of the glenoid fossa (the maxilla). Ideally, when this fixed axial position is reached, the teeth will have even and simultaneous contact.4 A tripod effect (the two joints and the anterior teeth) will be reached that produces a stable and repeatable position. By having a physiologic position from which to function, an interfer-ence-free occlusion can be reached.
The patient’s centric relation was captured using bimanual manipulation and a rigid bite wax. It is important to use a material that is hard so as to not compress or later distort when mounting. Studies have shown bimanual manipulation to be a very reliable and repeatable technique,5 but there are many acceptable methods for determining and recording centric relation. That topic is beyond the scope of this article, yet it is nevertheless important to become proficient and comfortable with some verifiable technique.
The casts of the maxilla and mandible are then face-bow mounted and related using the above centric relation record (Figure 5). A clinician should not overlook the importance of using a properly recorded face-bow whether using centric relation or maximum intercuspation. This tool allows a 3-dimensional (3-D) transfer of the anatomic relationship between the TMJ and the maxilla. It will also record and reproduce the proper axis of rotation from which the condyles are functioning.6
The models could now be trial equilibrated to determine if it was possible to make centric relation and maximum intercuspation the same position. If the records are accurate, and success can be achieved on the models, the results can then be reproduced in the mouth. Equilibration is not something for the clinician to fear, and its purpose is quite simple. Instead of thinking of equilibration as changing the occlusion, think of it as organizing and refining the occlusion. The clinician is simply removing tooth structure that is interfering with a harmonious joint position and function. Deflective posterior tooth contacts can be eliminated, and the occlusal forces can be transferred to the long axis of the posterior teeth. In this case, by equilibrating and recapturing the patient’s envelope of function, the patient was able to avoid selective endodontic treatment. The lower anterior teeth were restored with stacked porcelain veneers instead of crowns. As is often the case, proper equilibration decreases restorative treatment, saves the patient money, and provides a more stable masticatory system.6
The diagnostic wax-up can then be fabricated on the equilibrated models. A properly fabricated diagnostic wax-up can only increase the probability of success. Treatment pitfalls can be identified, and precise reduction guides and provisional stints can be fabricated from the wax-up.7 If both arches are being restored, it often simplifies the process to begin the wax-up with the mandibular anterior teeth as was done in this case. The goal was to recreate an ideal plane of occlusion and length for the lower anterior teeth that complemented the existing posterior plane of occlusion.8 Care was taken to create functional edges to the lower incisors. The edges should have a labio-incisal line angle present (Figure 6). This allows for smooth protrusive function and a definite holding point with the upper teeth.6 When the casts were mounted in centric relation and equilibrated, room to restore the lower anterior teeth was quite adequate. The waxing of these teeth only required replacing tooth structure that had been worn away (Figure 7).
The next step involved creating ideal lingual anatomy on the maxillary teeth to provide centric stops and canine and protrusive guidance (Figure 8). Achieving complete and immediate posterior disclusion by the anterior guidance should not be overlooked. This scheme has been shown to provide the lowest muscle activity and lessen the level of parafunction.9 After the centric stops and functional pathways have been created, the principles of smile design (length, incisal edge position, axial inclination, width-to-length ratio, incisal embrasures, and contact points)10 can be followed to create pleasing facial contours. The length would be “best guessed” by the preoperative photographs and measurements. The rest position of the upper lip in relation to the amount of visible central incisor is very useful. The average woman will show 3.4 mm when at rest.11 It is important to note that the maxillary incisal edge positions and length are refined and adjusted in the provisional restorations. The patient’s function and phonetics will help to refine these positions and should be closely monitored (Figure 9, Figure 10, Figure 11).12
The Final Restorations
Conservation of existing tooth structure is always a priority. In this particular case, full-coverage crowns were necessary to replace the existing crowns on teeth Nos. 7 and 10, and to restore the implant in the tooth No. 13 position. Crowns were also necessary on the canines to establish proper lingual inclines to allow canine guidance. The remaining teeth were restored with stacked porcelain veneers (Figure 12). Numerous follow-ups were scheduled with the patient to continue to refine the occlusion of the final restorations (Figure 13, Figure 14, Figure 15, Figure 16). Studies have shown that the need for adjustments to significant occlusal changes decreases after 4 months.13
Conclusion
There are many times that a patient’s restorative needs can seem overwhelming and perhaps impossible. Predictability is a win-win situation for the dentist and the patient. A comprehensive and occlusally guided approach to case planning can often “demystify” complicated cases. Comprehensive care is more than providing beautiful teeth. It is also about providing function, stability, and long-term results that improve a patient’s life.
Acknowledgment
The author would like to thank Dental Arts “Signature” Laboratory in Peoria, IL, for its contributions to this case.
References
1. Dawson P. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St. Louis, Mo: Mosby; 1989:92-106.
2. Donegan SJ, Knap FJ. A study of anterior guidance. J Prosthodont. 1995;4(4):226-232.
3. Puri P, Kambylafkas P, Kyrkanides S, et al. Comparison of Doppler sonography to magnetic resonance imaging and clinical examination for disc displacement. Angle Orthod.2006;76(5):824-829.
4. Parker MW. The significance of occlusion in restorative dentistry. Dent Clin North Am. 1993;37(3):341-351.
5. Keshvad A, Winstanley RB. Comparison of the replicability of routinely used centric relation registration techniques. J Prosthodont. 2003;12(2): 90-101.
6. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, Mo: Mosby; 2006.
7. Small BW. Pretreatment wax-ups and provisionals for restorative dentistry. Gen Dent. 2005;53(2):98-100.
8. Ash MM, Ramfjord S. Occlusion. 4th ed. Philadelphia, Pa: WB Saunders Co; 1995:114-121.
9. Okano N, Baba K, Akishige S, et al. The influence of altered occlusal guidance on condylar displacement. J Oral Rehabil. 2002;29(11):1091-1098.
1 0. Hess L. Esthetic conservation: A smile make-over does not always have to be extreme. Inside Dentistry. 2007;3(2):74-77.
11. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
12. Hess L. Interdisciplinary synergy: Managing complex treatment objectives for a predictable esthetic result. Advanced Esthetics and Interdisciplinary Dentistry. 2006;2(2): 10-18.
13. Hammad IA, Nassif NJ, Salmeh ZA. Full-mouth rehabilitation following treatment of temporomandibular disorders and teeth-related signs and symptoms. Cranio. 2005;23(4):289-296.
About the Author
Leonard A. Hess, DDS
Private Practice
Monroe, North Carolina