Self-Etch Immediate Dentin Sealing: A Clinical Technique
Randall G. Cohen; Michael V. Razzano
Dental bonding agents create a hybrid zone that is formed by the penetration of monomers into the dentin. This hybrid zone, with tubular occlusion, results in reduced dentin permeability,1 an important factor in decreasing the potential for postoperative sensitivity and pulpal pathology.1 In this article, the authors discuss the use of a self-etching, antibacterial adhesive combined with a flowable composite resin restorative material to achieve effective peripheral sealing of dentin for indirect restorations. The clinical significance of successful dentin bonding is particularly significant in the case of indirect bonded porcelain restorations because the final strength of the tooth?restoration complex is highly dependent on adhesive procedures.2
BACKGROUND
Dentin, a living, vital, sensitive portion of the tooth, can be described as a biologic composite made up of a collagen matrix filled with nanofillers of apatite crystallites.3 This matrix is penetrated by hollow tubules lined by intratubular1,4 dentin that are filled with dentinal fluid under a slight positive pressure.5 The “hydrodynamic theory” of dentin sensitivity is believed to be the primary mechanism through which pain is conveyed in response to chemical, thermal, and tactile stimuli.6
Outward fluid movement will not occur as long as the enamel or cementum seal is intact, but if these seals are lost, then dentinal fluid can slowly seep outward. Under these conditions the tubules will allow fluid and dissolved substances to pass from the oral cavity to the pulp chamber.7 The cut dentin’s resistance to fluid flow is largely due to the presence of the smear layer/smear plug combination or an otherwise intact hybrid zone, and accounts for 86% of the total resistance to fluid flow.8
CROWN PREPARATIONS AND PULPAL INJURY
Depending on the amount of tooth reduction and the size of the tooth, a full-crown preparation can expose from 1 to 2 million dentinal tubules if all the enamel is removed.9 Pashley et al10 noted the potential variables for pulpal irritation following crown preparation as: preparation technique; remaining dentin thickness; retention of the smear layer; amount of microleakage under provisional restorations; the method of cement removal, and the length of time between crown preparation and luting of final casting. In another reference,7 the authors indicated that the permeability properties of dentin determine its sensitivity and the degree of pulpal response to restorative materials and microleakage.
While provisional restorations may have more microleakage—including bacteria and their byproducts—than final indirect restorations do, many studies have also reported dye leakage with permanently cemented restorations.10 The Pashley group discussed the potential for adhesive resins to seal the dentin of crown preparations as a procedure that may provide a measure of protection to the pulp. It is thought that this procedure may prevent the penetration of bacterial products coming from plaque microorganisms that colonize prepared dentin surfaces under leaking provisional crowns.10 The presence of bacteria on the dentin substrate surface has been shown to reach the pulp via the dentinal tubules11 and has been implicated as the prime factor causing pulp inflammation and necrosis.12
ADHESION
Freshly cut dentin is the ideal substrate for optimal dentin bonding; a substrate present only at the time of tooth preparation and before impression making.2,10 Paul and Schaerer13 discussed dentin contamination due to provisional cements, including the subsequent reduction in bond strengths, even without the consideration of salivary and bacterial contamination.
Another factor in optimal bonding is the progressive development of the full dentin bond strength. Dentin bond strength develops progressively over time, probably owing to the completion of the copolymerization process involving the different monomers.14 When indirect restorations are bonded directly to the dentin, the initial dentin bond is immediately under the stress of the polymerization shrinkage of the luting composite cement. If the force generated during polymerization shrinkage exceeds the early bond strength of the resin-bonding agent, gap formation is likely to occur, creating the potential for postoperative symptoms.2
THE HYBRID ZONE: SELF-ETCH VS TOTAL ETCH
The hybrid layer that is formed from fourth-generation “total-etch” adhesives and the sixth-or seventh-generation bonding agents, generally called “self-etching adhesives,” are fundamentally different.
One notable difference between the two systems is that the primers in total-etch systems are far less acidic, and consequently require a preliminary treatment with 32% phosphoric acid to change the dentin surface in a way that facilitates a strong dentin bond. This phosphoric-acid treatment completely removes the smear layer formed during cavity preparation, a layer that otherwise would block the dentinal tubules, thus resulting in increased dentin permeability and, with it, the potential for postoperative sensitivity. This smear layer removal is necessary for the fourth-generation primer and the bond to penetrate the tubules and form the hybrid zone.15 The self-etch technique, on the other hand, leaves the smear layer in place. These dentin bonding systems are based on infiltration and modification of the smear layer by an acidic monomer.15 Accordingly, fluid movement within the dentinal tubules is impeded, thus reducing postoperative sensitivity.
Another notable difference between the two adhesives systems is technique sensitivity. The phosphoric-acid treatment leaves the protein component of dentin completely unsupported, literally floating in the rinse water. If the surface is dried too much, the collagen fiber network collapses and creates an impermeable organic barrier for primer penetration.16 Gaps can form and bond strength decreases. Excessive water left on the substrate creates a different problem in that the primers do not remain dissolved in their solvents. Consequently, resin globules and water trees can form, interfering with bond strength and creating fluid movement within the tubules, promoting postoperative sensitivity.17
Unlike fourth-generation total-etch systems, with self-etching adhesive systems the dentin substrate can be thoroughly dried before application of self-etching primers. Because there is no phosphoric-acid pretreatment, the dentin substrate remains fully mineralized, with complete support for the organic component of the dentin. The dentin substrate remains fully mineralized following preparation prior to the application of the acidic primer. This avoids the question as to how wet the dentin should be prior to bonding.18 Self-etch adhesives simultaneously demineralize and prime the dentin substrate. Total-etch systems demineralize the surface first, then stabilize the dentin surface with the subsequent application of a primer. Accordingly, they treat the cut dentin surface in two fundamentally different ways. This clinical picture stands in stark contrast to the demineralized, highly permeable condition of the dentin that exists after the phosphoric-acid?etch step needed for fourth-generation bonding systems. One could then conclude that the significantly reduced technique sensitivity from the self-etching primer adhesive systems provides a more consistent outcome than what is generally produced by the more technique-sensitive total-etch adhesives.
The hybrid zone with sixth-generation, two-step self-etch systems is thin and strong, and, most importantly, allows the smear plug to stay intact. Immediate dentin sealing (IDS), which is the application of dentin bonding agents (DBA) immediately after tooth preparation and before impression making, can be used to create a hybrid zone on the entire tooth preparation surface, taking advantage of its resilience and reduction of dentin permea-bility. In addition, a self-etching system that contains an antibacterial component will reduce the amount of surface bacteria and their by-products, bacteria that could otherwise have a direct pathway to the pulp via the dentinal tubules.19
CLINICAL TECHNIQUE
After crown preparation, the teeth and surrounding tissues are cleaned of grinding debris with a slurry of pumice (Figure 1) and then rinsed. Isolation is accomplished with retractors, cotton rolls, and the proper placement of the saliva ejector.
As self-etching primers are meant for use on relatively dry dentin, the substrate is air-dried, and the adhesive primer (Protect Bond Primer, Kuraray America, Co (New York, NY) is applied to the entire cut dentin surface (Figure 2 and Figure 3 ) and left in place for 20 seconds. The dentin is then completely dried using a dry air syringe and the hydrophobic bonding component (Clearfil® Protect Bond, Kuraray America)18 applied in a single coat, lightly air-dried, then light-cured. Plastic strips are used to ensure contact clearance before photoactivation of the bonding resin.
At this point the flowable composite resin (Clearfil® Majesty Flow, Kuraray America) is applied to the tooth surface (Figure 4 ) using a dispensing brush (prototype by Kuraray America), and spread in a thin layer on the outside of the crown preparation, keeping it away from the margins of the preparation. The preparation is then cured using a standard halogen curing lamp.
After curing the overlying flowable composite resin, the preparation is scrubbed with ethanol using a syringe and a brush tip (prototype device, Kuraray America) (Figure 5 ) to remove any oxygen-inhibited bonding resin from the preparation surface that had not bonded to the overlying flowable resin. The preparation margins are then polished with a white rubber point on a low-speed handpiece (Figure 6) to remove any bonding resin or composite that might have flowed onto the margin of the preparation. The preparations are then rinsed and dried. Retraction cord is placed and the impression made. The preparations are then coated with a thin layer of separating medium before the fabrication of the provisional crown using methyl methacrylate.
DISCUSSION
Earlier work had described the use of an antibacterial, self-etching adhesive applied to the outside surface of the crown preparation using a glycerin air block gel to fully polymerize the outer, oxygen-inhibited layer of bonding resin.20
The IDS technique using a self-etching antibacterial adhesive can be enhanced with a layer of flowable composite resin restorative material. By following the first IDS layer with a flowable composite, the clinician can address the variables for pulpal injury as previously described by Pashley et al as follows:
? Use an antibacterial agent and create an additional barrier to the flow of pulpal toxins through the dentinal tubules, thus reducing the effects of bacterial microleakage during the provisionalization phase.
? Use a self-etching adhesive system that reduces dentin permeability by maintaining the smear layer and using it as a reliable bonding substrate.
? Create an intact hybrid zone on the external surface of the preparation immediately after preparation, before the dentin surface comes in contact with temporary cements or other contaminants.
In addition, the freshly cut dentin provides the best substrate for the application of the bonding resin, and the interval between provisionalization and final cementation allows for the development of the maximum bond strength before the challenge presented by the polymerization shrinkage of the luting composite resin cement.
CONCLUSION
The use of an antibacterial, self-etching adhesive to the cut surfaces of a crown preparation followed by brushing on a flowable composite resin appears to be a clinical technique that will improve the patient’s experience by reducing dentin permeability, therefore lessening the effects of the operative procedure on the dental pulp, as well as improving the bond strength of the final indirect restoration.
REFERENCES
1. Pashley DH. Dynamics of the pulpo-dentin complex. Crit Rev Oral Biol Med. 1996;7(2):104-133.
2. Magne P. Immediate dentin sealing: a fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17(3):144-155.
3. Marshall GW, Marshall SJ, Kinney JH, et al. The dentin substrate: structure and properties related to bonding. J Dent. 1997;25(6): 441-458.
4. Linde A, Goldberg M. Dentinogenesis. Crit Rev Oral Biol Med. 1993;45: 679-728.
5. Ciucci B, Bouillaguet S, Holz J, et al. Dentinal fluid dynamics in human teeth, in vitro. J Endod. 1995;21:191-194.
6. Brannstrom M. The cause of postrestorative sensitivity and its prevention. J Endod. 1986;12(10): 475-481.
7. Pashley DH, Pashley EL, Carvalho RM, et al. The effects of dentin permeability on restorative dentistry. Dent Clin North Am. 2002;46(2):211-245.
8. Pashley DH, Livingston MJ, Greenhil JD. Regional resistances to fluid flow in human dentine in vitro. Arch Oral Biol. 1978;23(9): 807-810.
9. Richardson DW, Tao L, Pashley DH. Dentin permeability: effects of crown preparation. Int J Prosthodont. 1991;4(3):219-225.
10. Pashley EL, Comer RW, Simpson MD, et al. Dentin permeability: sealing the dentin in crown preparations. Oper Dent. 1992;17(1):13-20.
11. Bergenholtz G. Pathologic mechanisms in pulpal disease. J Endod. 1990;16(2):98-101.
12. Cox CF, Hafez AA, Akimoto N, et al. Biological basis for clinical success: pulp protection and the tooth-restoration interface. Pract Periodontics Aesthet Dent. 1999;11(7): 819-826.
13. Paul SJ, Schaerer P. Effect of provisional cements on the bond strength of various adhesive bonding systems on dentine. J Oral Rehabil. 1997;24(1):8-14.
14. Magne P. Immediate dentin sealing: A fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17:144-155.
15. Terry DA. Prehybridization of indirect restorative preparations. Pract Proced Aesthet Dent. 2004;16:661-662.
16. Carvalho RM, Yoshiyama M, Pashley EL, et al. In vitro study on the dimensional changes of human dentine after demineralization. Arch Oral Biol. 1996;41(4): 369-377.
17. Gwinnett AJ. Moist versus dry dentin: its effect on shear bond strength. Am J Dent. 1992;5(3):127-129.
18. Pashley DH. The evolution of dentin bonding from no-etch to total-etch to self-etch. Adhes Tech Sol. 2002;1(1):1-7.
19. Bergenholtz G. Pathologic mechanisms in pulpal disease. J Endod. 1990;16: 98-101.
20. Cohen RG, Razzano MV. Immediate dentin sealing using an antibacterial self-etching bonding system. Pract Proced Aesthet Dent. 2006;18(9): 561-565.
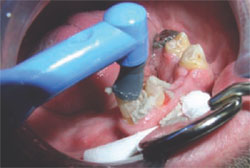 | 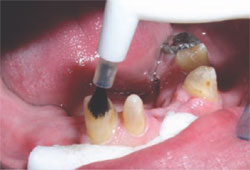 |
| Figure 1 The teeth and surrounding tissues are cleaned of grinding debris with a slurry of pumice. | Figure 2 The self-etch adhesive primer is applied to the entire cut dentin surface and left in place for 20 seconds. |
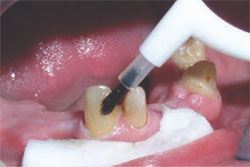 | 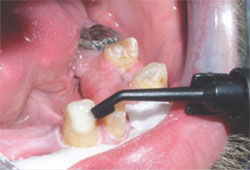 |
| Figure 3 The bonding resin is applied. | Figure 4 The flowable composite is applied. |
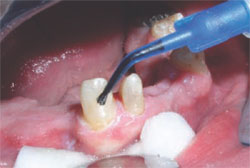 | 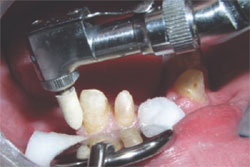 |
| Figure 5 After curing the overlying flowable composite resin, the preparation is scrubbed with ethanol. | Figure 6 The preparation margins are then polished with a white rubber point on a lowspeed handpiece. |
| About the Author | |
 Randall G. Cohen, DDS Randall G. Cohen, DDSPrivate Practice Newtown, PA Michael V. Razzano, DDS Private Practice Woodstock, Georgia | |



