Interdisciplinary Synergy: Managing Complex Treatment Objectives for a Predictable Esthetic Result
Leonard A. Hess; Don Franklin
Many clinicians would agree that dentistry has never been in a better position to provide options for patients. At the same time, patients are also demanding more from the dental profession. Many patients come into the clinical setting with predetermined plans for their care, and expect high-quality results. This can often be a difficult situation for the clinician. Patients are many times only familiar with results, with no appreciation for the process involved. Nevertheless, esthetic change can have a profoundly positive effect for a patient.1 Many times, elective treatment offers an opportunity to improve not only esthetics for a patient, but more importantly, function.
The esthetic boom in the dental profession continues to intrigue more patients with complex situations to seek possible solutions. These complex cases often require the involvement of multiple specialties, which should work as an interdisciplinary team and not independently. To achieve predictable success, a consistent approach to treatment planning is necessary. A patient’s needs and goals should be well documented. A functionally derived approach to smile design will lay the foundation for the interdisciplinary treatment plan. Each clinician must understand the biologic and functional ramifications of the proposed treatment, and his or her role in the process.
Pretreatment Parameters
Medical and Social History
Every restorative procedure must begin with respect for its impact on systemic health and vice versa. A systemic issue may contraindicate or complicate many dental procedures or surgeries. Dental implants offer an excellent example. Many health issues, such as diabetes or previous radiation therapy, may increase risk, but not necessarily prohibit treatment. These issues should be discussed and noted in a patient’s consent for care.2 Additionally, a patient’s social habits or diet could also place the longevity of treatment in jeopardy. These types of issues should be noted as well.
Psychological History
Interdisciplinary treatment plans may take years to complete. It is important that patients are fully informed of the length and complex nature of the proposed plan. Also, the time required to be in the chair for active treatment should be made clear. This author has found that patients cannot be educated enough when complex treatment is planned. Patients must know that they are a part of the team, and their attitude and level of commitment will impact the overall results.
It is also important to gauge the expectations of the patient before a commitment is made by either party. This is espe-cially true when considering elective orthodontics and restorative care. For example, studies have shown people with a more complicated malocclusion usually have higher expectations of treatment outcome.3 Veneer and other esthetic procedures are becoming very popular, yet patients treated with porcelain veneers may feel satisfied with the outcome only up to 80% of the time.4
Dental History
A critical component of pretreatment evaluation is assessing the patient’s biologic risk. Any restorative plan must be based on a sound periodontal foundation. An unhealthy oral environment will complicate or prohibit any phase of treatment whether periodontal, endodontic, orthodontic, or prosthodontic. Causative factors should be identified and remedied. Issues such as loss of attachment, periodontal pocketing, and biologic width violation must be resolved before restorative care is begun.5 Patients with a poor history of adequate hygiene should exhibit an ability to improve their plaque control. Orthodontic studies have shown that a patient’s current caries risk factors are a reliable predictor of decalcification risk during treatment.6
The patient’s occlusal history should also be examined and the etiology of severe wear should be addressed. It is important to consider the effect of poor occlusion on tooth mobility and the supporting periodontal structures.7 The health of the patient’s temporomandibular joint should be examined and considered. The joints should be capable of bilateral loading in centric relation without pain or tension. The condyles should be able to function in their most seated position in a repeatable fashion. In addition, any joint pathologies should be identified and considered before initialization of treatment.8
Diagnostic Data
Every advanced esthetic case should begin with the collection of the same data set. These include the necessary bitewing, periapical, and panoramic radiographs; a full set of extraoral and intraoral digital photographs; study models mounted on a fully adjustable articulator using a face-bow transfer; and a diagnostic wax-up of the proposed treatment which will transfer to the mounted case.
Case Study
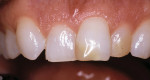
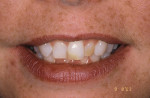
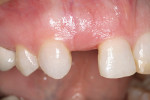
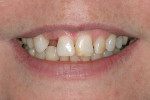
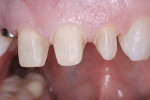
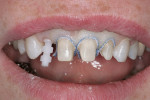
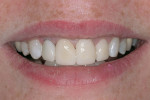
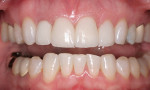
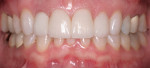
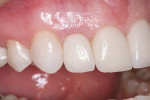
A 37-year-old woman expressed interest in improving her smile and was seeking options (Figure 1 and Figure 2). Her first inclination included porcelain veneers to improve her maxillary anterior color and tooth shape (Figure 3). The patient was informed that this was not an option because it would require excessive tooth preparation and the end result would be less than acceptable for this clinician. Of significance was a congenitally missing lateral incisor (tooth No. 7). The room for this tooth in the arch form was completely lost. Furthermore, excessive mandibular crowding made proper anterior function very difficult if not impossible. Through education, the patient decided on a combination of orthodontics, periodontics, and restorative care to satisfy her esthetic needs.
Consultation with the patient and interdisciplinary communication allowed the creation of the treatment plan. The principles of smile design allowed a seemingly complicated case to be broken down into manageable components. Each specialty contributed key elements to allow the formation of an esthetic and functional smile. It is often easier to evaluate the smile design deficiencies for an esthetic case and then consider what can be accomplished to create a more ideal situation.
Orthodontic Treatment
Maxillary Midline
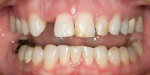
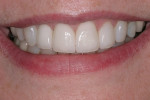
The patient had an approximate midline shift of 4 mm to the right side (Figure 4). Ideally, the maxillary midline would coincide with the midline of the face. The reality is that not every patient can have true midline symmetry. Many people have asymmetric noses or other less-than-perfect features. Generally speaking, the threshold for a midline deviation becoming noticeable is approximately 2 mm from center. More than this number denotes an unattractive smile from a layperson. In addition, nose and maxillary midline position deviations are the least attractive variables in relation to total face symmetry.9
Anterior Inclination
The inclination of the maxillary anterior teeth during orthodontics was established through cephalometric measurements.10 By increasing the angulation toward the labial, more arch width could be created. This would allow room for the missing lateral incisor and help to alleviate crowding in the maxillary arch.11 Communication between the orthodontist and restorative dentist was very important during treatment. The orthodontist requested input for anterior tooth final positioning, making the restorative component more predictable.
Occlusal Plane
This patient’s occlusal plane was in need of functional improvement. If a proper envelope of function for the anterior teeth is expected, the occlusal plane must be addressed. Posterior disclusion during excursive movements is a priority.12 For this patient, excessive crowding in the mandibular arch necessitated the removal of a mandibular incisor. As the maxillary inclination changed the position of the anterior teeth, some maxillary posterior teeth were intruded. The arch width was increased, establishing the new Curve of Wilson and the new maxillary occlusal plane. The mandibular anterior teeth were then intruded and brought into function with the maxillary teeth. When orthodontic treatment was finished, the patient had bilateral canine guidance without posterior interferences (Figure 5, Figure 6 and Figure 7).
Periodontal Treatment
At the initial examination, the patient was in the finishing stages of orthodontic treatment. The patient was in need of implant placement at the tooth No. 7 position and esthetic gingival recontouring (Figure 8).
Gingival Form
Evaluation of the gingival outline showed asymmetry along the maxillary incisors. The height of the gingival outline was positioned more coronally at teeth Nos. 8 and 10. It was evident that the resulting gingival margin of the proposed implant at tooth No. 7 would be apical to the gingival margin at tooth No. 8 and its contralateral, tooth No. 10. This result would be esthetically unacceptable. Esthetic crown lengthening of teeth Nos. 8 and 10 would be necessary to create the desired symmetry and gingival form (Figure 8).
Careful consideration was also given to the implant recipient site. The interdental space between teeth Nos. 6 and 8 was radiographically measured at 5 mm. The facial-lingual dimension of the ridge appeared to be within normal limits clinically with no hard or soft tissue deficiency. The area was anesthetized and sounded with bone calipers, revealing a 5-mm facial-lingual crestal ridge width. These dimensions would not accommodate a standard diameter implant, but did indicate adequate bone for the use of an ITI® Narrow Neck Solid Screw implant (Straumann USA, LLC, Andover, MA). With a 3.3-mm body and a 3.5-mm shoulder, this fixture is designed for use in the maxillary lateral incisor or mandibular central or lateral incisor positions. These positions often have limited mesial-distal space between adjacent teeth (5 mm) and require a minimal faciolingual crest width of 4.8 mm.13
At the surgical appointment, the first step was to establish the correct gingival margin at teeth Nos. 8 and 10. The gingival plane should be parallel to the interpupillary line and perpendicular to the facial midline. The height of contour of the gingival margins may form a straight line along the central, lateral, and canine. Or, it may have a sinuous form with the gingival margin of the lateral incisor just coronal (2 mm or less) to the adjacent canine and central margins.14 The planned margin of the implant site was the primary determining factor for the design of the gingival outline. In this case, it would be possible to have a straight line along the height of contour from canine to lateral incisor.
The next step was to measure the patient’s biologic width. There was a greater gingival sulcus at teeth Nos. 8 and 10, noting the gingival margin to be more coronal to the cementoenamel junction (CEJ) than at the adjacent teeth. Probing revealed 3 mm at teeth Nos. 8 and 10 and sounding to bone was 5 mm. Sounding with a periodontal probe indicated the crestal bone to be 2 mm apical to the CEJ consistently from canine to canine. It was also noted that the patient demonstrated a thin, scalloped biotype devoid of bony ledges. In this case, a gingivectomy without osseous contouring would correct the gingival form.15 An inverse bevel incision was made and a 1-mm collar of gingival was excised at tooth No. 8 and 2 mm at tooth No. 10.
Study models and a diagnostic wax-up allowed fabrication of a vacuum-formed surgical stent. The stent provided guidance for proper implant position and angulation. Because it eliminates the need for disruption of the peri-implant soft tissues with a second-stage surgery, a single-stage implant system was selected for optimum esthetics. Preservation and restoration of the papillae in the implant site was essential for the desired esthetic outcome. To generate a papilla, the distance from the bone to the contact point cannot be >5 mm.16 In this case, the contact point was at 5 mm, so regeneration of the papilla was possible. There was a wide band of facial keratinized gingiva and the bone sounding revealed an adequate ridge; therefore, a tissue punch access was made. This method provided no trauma to the adjacent papillae and no exposure of bone, which would result in crestal resorption. This would increase the distance from bony crest to the contact point.
Once the tissue punch was made, the thickness of the gingiva was measured and the osteotomy was performed according to ITI protocol. The implant was placed so that the shoulder of the fixture (crown margin) was 2 mm apical to the planned gingival margin and 2 mm apical to the neighboring CEJ.17 An ITI® NNI healing cap (Straumann USA, LLC) with labial bevel (4 mm ¥ 3.4 mm) was placed to shape the gingival margin and support the papillae.
Restorative Treatment
After 6 weeks of healing, the patient was ready to begin the prosthodontic phase of treatment. The case had already been face-bow mounted on an articulator, and a diagnostic wax-up was previously completed. As the wax-up guided the periodontal care, it would now serve as a template for the functional positioning of the anterior maxillary teeth.
After the orthodontic positioning, teeth Nos. 8 through 10 had diastemas present. In addition, failing composite restorations were present on the teeth. The patient was treatment planned to restore the implant with a cement-retained crown. In addition, teeth Nos. 8 through 10 would receive stacked porcelain veneers. The initial treatment plan anticipated more restorative needs to restore anterior function. It is always beneficial when less tooth structure can be removed to achieve the planned esthetic result.
The preparation design was dictated by the diastemas and size of the failing restorations. These factors required “through the contact” preparations and some lingual margin placement (Figure 9, Figure 10 and Figure 11). A temporary abutment was prepared for the implant during the preparation appointment. The implant was surgically placed with respect for the hard tissue parameters. As a result, the soft tissue could be guided by the provisional restoration to have a similar architecture and quality of the surrounding teeth (Figure 12).18 It was now time to address the other key components of smile design for proper fabrication of the restorations.
Color
Color is often, and sometimes the only, important aspect for the patient. A good number of people would like whiter teeth, and this patient was one of them.19 The patient received an in-office whitening session after the periodontal surgery had healed. Two weeks were allotted for the color to stabilize to allow more certainty in matching the porcelain restorations.20,21
Central Incisor Length
A variety of factors influence the length of the central incisors. These factors include upper lip characteristics, lower lip position during smiling, lip position at rest, and the envelope of function. In this case, the diastemas needed to be closed and it was important to keep the width-to-length ratio at approximately 80%, an accepted proportion.22,23 This ratio would also influence the establishment of the golden proportion. In this proportion, a tooth appears 40% smaller than the tooth to its mesial and is pleasing to the eye. This is an apparent measurement when viewing the teeth from the direct anterior.24 A short lip will obviously display more tooth structure at rest as well during a smile. Vig and Brundo determined that women show an average of 3.4 mm at rest and men show 1.91 mm. In addition, the amount of tooth show at rest decreases with advancing age.25
The length of the incisor is also important in relation to the lower lip during speech. The lower lip must contact the edges of the incisors in a natural fashion. This occurs during the pronunciation of words beginning with the letters F and V. The contact should occur in the wet or inner vermilion border of the lip and not the dry or cutaneous portion.26 The length of the teeth must also be such that they do not interfere with the envelope of function. Excessive length may cause lateral excursive interferences, which could lead to restoration failure.
Position of the Incisal Edge
The position of the incisal edge is important for numerous reasons. It must be placed to coincide with the envelope of function of the anterior teeth. If it is positioned too lingually, it may cause interference to the mandibular incisors during the path of closure.27 The position must also be in harmony with the path of closure of the lower lip. Otherwise, the upper lip must strain to close around the maxillary teeth, and the lower lip will be obstructed. This position is also referred to as the neutral zone, a peri-oral tissue and muscle-defined position.28 The incisal edges also influence the formation of the incisal plane (Figure 13). It is desirable for the incisal plane to be slightly coronal to the posterior maxillary plane and parallel to the lower lip during a smile. The incisal edges should also be perpendicular to the maxillary midline (Figure 14).29 This patient had an asymmetric lower lip when smiling (Figure 15, Figure 16 and Figure 17).
All of these criteria were incorporated into the diagnostic wax-up. They were estimated from knowledge of the patient, mounted casts, and photographs. However, these positions were refined and tested in the mouth through the provisional restorations. The impressions of the final provisionals could then be cross-mounted. The ceramist made index stents to “copy” the length and incisal edge positions of the provisionals, therefore allowing the “patient-tested” positions to be transferred to the final restorations.
Conclusion
The demand for esthetic dental procedures should continue to grow in the years ahead, and many people come into the dental office knowing what can be accomplished for their appearance through esthetic care. When a complex situation is encountered, it is always best to first consider the end result. The parameters for each step should be identified to ensure a successful outcome. The patient and each member of an interdisciplinary team should all have the same goal in mind. This consistent approach will result in a predictable outcome.
Acknowledgment
Dr. Hess would like to thank Dental Arts Signature Laboratory for fabricating the restorations featured in this article. He would also like to thank Dr. Gary Starr for the orthodontic treatment and Dr. Don Franklin for the periodontal treatment.
References
1. Davis LG, Ashworth PD, Spriggs LS. Psychological effects of aesthetic dental treatment. J Dent. 1998;26(7):547-554.
2. Moy PK, Medina D, Shetty V, et al. Dental implant failure rates and associated risk factors. Int J Oral Max Implants. 2005;20(4): 569-577.
3. Petrone J, Fishell J, Berk NW, et al. Relationship of malocclusion severity and treatment fee to consumer’s expectation of treatment outcome. Am J Orthod Denofacial Orthop. 2003;124(1):41-45.
4. Meijering AC, Roetas FJ, Mulder J, et al. Patients’ satisfaction with different types of veneer restorations. J Dent. 1997;25(6):493-497.
5. Hess L. The biologic and restorative interface: improving periodontal health with contemporary materials and sound restorative dentistry. Contemporary Esthetics and Restorative Practice. 2005;9(3): 46-51.
6. Zimmer BW, Rottwinkel Y. Assessing patient-specific decalcification risk in fixed orthodontic treatment and its impact on prophylactic procedures. Am J Orthod Dentofacial Orthop. 2004;126(3):318-324.
7. Kao RT, Chu R, Curtis D. Occlusal considerations in determining treatment prognosis.J Calif Dent Assoc. 2000;28(10):760-769.
8. Dawson P. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St. Louis, Mo: Mosby; 1989:92-106.
9. Beyer JW, Lindauer SJ. Evaluation of dental midline position. Semin Orthod. 1998;4(3):146-152.
10. Cuoghi OA, Bertoz FA, de Mendonca MR, et al. Labiolingual and mesiodistal positioning of maxillary permanent incisors during the eruption process. J Clin Pediatr Dent. 2000;25(1):13-21.
11. O’Higgins EA, Kirschen RH, Lee RT. The influence of maxillary incisor inclination on arch length. Br J Orthod. 1999;26(2): 97-102.
12. Ramfjord SP, Ash MM. Occlusion. 4th ed. Philadelphia, Pa: WB Saunders Co; 1995:114-121.
13. Scacchi M. The development of the ITI dental implant system. Part 1: a review of the literature. Clin Oral Implants Res. 2000: 11(Suppl 1):8-21.
14. Sclar AG. Soft Tissue and Esthetic Considerations in Implant Therapy. Hanover Park, Il: Quintessence Publishing Co; 2003.
15. Rose LF, Mealy BL, Genco RJ, et al. Periodontics, Medicine, Surgery, and Implants. St. Louis, Mo: Mosby; 2004.
16. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal papilla. J Periodontal. 1992;63(12):995-996.
17. Straumann, Basic Information on the Surgical Procedure with the ITI Dental Implant System. 11/2002. Published by ITI Dental.
18. Carrion JB, Barbosa IR. Single implant supported restorations in the anterior maxilla. Int J Periodontics Restorative Dent. 2005;25(2):149-155.
19. Joiner A. The bleaching of teeth: a review of the literature. Online J Dent. Published online March 2006.
20. de Silva Gottardi M, Brackett MG, Haywood VB. Number of in-office light-activated bleaching treatments needed to achieve patient satisfaction. Quintessence Int. 2006;37(2):115-120.
21. Braun A, Jepsen S, Krause F. Spectrophotometic and visual evaluation of vital tooth bleaching employing different carbamide peroxide concentrations. Online Dent Mater. February 24, 2006.
22. Chiche GJ, Pinault A. Esthetics of Fixed Anterior Prosthodontics. Hanover Park, Il: Quintessence Publishing Co; 1994:23.
23. Wolfart S, Thormann H, Freitag S, et al. Assessment of dental appearance following changes in incisor proportions. Eur J Oral Sci. 2005;113(2):159-165.
24. Ascheim KW, Dale BG. Esthetic Dentistry:A Clinical Approach to Techniques and Materials. 2nd ed. St. Louis, Mo: Mosby; 2000:31.
25. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
26. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, Il: Quintessence Publishing Co; 1994:21.
27. Cranham J. The horizontal position of the maxillary incisal edge: the key to optimum esthetics, phonetics, and function. Contemporary Esthetics and Restorative Practice. 2006; 10(2):22-24.
28. Dawson P. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, Mo: Mosby; 1989:330.
29. Thomas JL, Hayes C, Zawaideh S. The effect of axial midline angulation on dental esthetics. Angle Ortho. 2003;73(4):359-364.
About the Authors
Leonard A. Hess, DDS
Private Practice
Monroe, North Carolina
Don Franklin, DDS, MS
Private Practice
Charlotte, North Carolina