Dental Sleep Medicine: It’s Not Voodoo That They Do Anymore
Allison M. DiMatteo, BA, MPS
One problem affects somewhere in the neighborhood of 67% of adults and another is estimated to affect between 17% and 20%. Both problems affect sufferers when they’re doing what they spend 30% of their time doing—sleeping. Sleep disordered breathing (SDB)—whether snoring or sleep apnea, respectively—are disruptive and potentially fatal for those who experience them. They’re bothersome to loved ones. What’s more, they’re among the most under-diagnosed conditions in health care today.
Considering that such a large percentage of our time is spent sleeping and that this time is important to our body’s health, ensuring that good quality sleep occurs without interruptions from SDB is now well recognized as an important component to maintaining overall systemic health. In fact, according to a 2006 report from the Institute of Medicine, sleep disorders and sleep deprivation represent a major unmet public health problem in America, with 50 million to 70 million people chronically suffering from a disorder of sleep that results in a wide range of deleterious health consequences, including increased risk of hypertension, diabetes, obesity, depression, heart attack, and stroke.1 Almost 20% of all serious car crash injuries in the general population are associated with driver sleepiness, independent of alcohol effects.1
According to Don Pantino, DDS, a past president of the American Academy of Dental Sleep Medicine (AADSM) who maintains a private practice in Islip, New York, it’s now recognized that fatigue and sleep disorders indeed played a significant role in such disasters as the Exxon Valdez oil spill, the Challenger Shuttle disaster, the Bopal India accidents, and the tragic commuter ferry accident in New York City a few years ago. Additionally, Pantino says that according to the congressional committee on sleep disorders—which is chaired by Dr. William Dement—sleep disorders and the problems attributed to them can be quantified in terms of lost wages and lost productivity into the billions of dollars.
"Studies show very clearly that sleep apnea—when left untreated—contributes to a number of negative sequelae," Pantino says. "It is very costly on our health care system. I always tell my patients that there’s a reason we spend a third of our lives sleeping, and if we’re not doing that correctly, then it’s reflected in our daytime quality of life."
Despite the increased numbers of sleep centers that have been introduced in the last 10 years—as well as the growing interest in the field of sleep medicine—it’s estimated that 90% of individuals with SDB never receive a diagnosis, says Mark J. Friedman, DDS, a professor of clinical dentistry and part-time faculty member at the University of Southern California School of Dentistry, who maintains a private practice that includes dental sleep medicine in Encino, California. Friedman says that because dentists see an individual patient on average twice a year—if not more frequently—they’re in a good position to help identify a huge population of patients who have signs and symptoms of SDB.
For those who’ve been practicing dental sleep medicine since the days it was considered voodoo, recent recognition of the acceptance of oral appliances as a first-line treatment for SDB is stopping some of the crossed-eyed looks dead in their tracks. And the fact that people’s lives are being changed for the better—with dramatic improvements in their health and how they feel each and every day—gives credence to what these health care pioneers have been doing for more than 15 years.
"Dentistry is following more of a medical model, and that can only do well to elevate our profession both in the way we provide our services and in how we are viewed by the public," Friedman says. "With the advent of dental sleep medicine, we can save people’s lives. You—as a dentist—by making an oral appliance could help prevent a stroke or a heart attack."
In 2007, the research, development and use of oral appliances and oral surgery for the treatment of SDB or other sleep-related conditions is gaining in popularity as well as acceptance. Clinicians trained in this area—and the laboratories that offer the appliances needed for sleep breathing therapies—can enhance and expand the level of care and service provided to patients. Important to such endeavors are education, training, and building a bridge with colleagues in other areas such as medicine and sleep centers in order to follow the most appropriate treatment protocol. Here, Inside Dentistry presents a snapshot of why it’s important, worthwhile, and satisfying to become knowledgeable about today’s dental sleep medicine.
Sleep Disorders & Treatments
Some of the anatomic features that may contribute to snoring and obstructive sleep apnea (OSA) are visible within the oral cavity and include macroglosia, a narrow mandibular arch, a high palatal vault, a large uvula, and enlarged tonsils. All of these are easily viewed during a routine dental examination, Friedman explains.
When talking about snoring, oral appliances and surgical procedures are the treatments used most, in addition to positional therapy, explains Jonathan Parker, DDS, whose private practice—the Snoring and Sleep Apnea Dental Treatment Center—is located in Saint Louis Park, Minnesota. If talking about a diagnosis of OSA, especially moderate to severe, the number one treatment of choice is continuous positive airway pressure (CPAP).
The CPAP machine introduces air into the patient’s nasal passage and uses positive pressure to open their airway, thereby enabling them to breathe, explains Michael DiTolla, DDS, director of clinical education for Glidewell Laboratories.
Surgery is generally recommended when it is determined that the site of obstruction is in specific areas. For example, if the site of obstruction for apnea is in the palate, then some form of palatal surgery may be effective, Parker says. If the site of obstruction is in multiple parts of the airway, or if the patient is not effectively treated with CPAP or oral appliance therapy, then maxillo-mandibular (telegnathic) surgery may be appropriate, he says.
Friedman says that among the other options for treating SDB—depending upon the diagnosis—are tongue retaining devices that move the tongue base forward in order to help splint the airway. Orthodontics to expand the dental arches and allow the tongue to posture in a more forward position and relieve some of the airway obstruction may also benefit some patients, Friedman says.
However, the AADSM last year announced its support of new guidelines that identified oral appliance therapy as an effective treatment for OSA.2 Those guidelines, which were issued by the American Academy of Sleep Medicine (a physician’s group) and published in the February 2006 issue of the journal SLEEP, indicate that oral appliance therapy (OAT) can be an ideal first-line therapy for mild to moderate cases of OSA or when CPAP is not a viable treatment option.2
The American Academy of Sleep Medicine did originally acknowledge a role for oral appliances in the treatment of SDB as early as 1995, Pantino says, although data available at that time was limited. Now, more than 10 years later, more data from randomized and nonrandomized trials are available, so a dentist’s involvement in the process is no longer reserved for the last option, he says.
Case reports on the topic of SDB advocate that the management of OSA with an oral appliance be handled by dentists trained and experienced in the overall care of oral health, temporomandibular joints, dental occlusion, and associated structures.3 In such cases, a mandibular advancement oral appliance has been the only non-surgical management modality for OSA when CPAP cannot be tolerated.3 Studies have shown that OAT is associated with improved upper airway stability during sleep.4
Bringing Dentistry into the Mix
Official organization of a dental sleep medicine discipline began nearly 16 years ago or more. Dental clinicians began to recognize that oral appliances worn at night were having a positive impact on a patient’s ability to sleep quietly through the night and/or experience better breathing. For Friedman and some other dental practitioners like him, his involvement in dental sleep medicine started while investigating his own sleep breathing problem and/or that of a loved one.
DiTolla observes that the field of dental sleep medicine continues to grow, although not as fast as he thinks it should based on the benefits that patients—and dental practices—can derive from it. He says that one of the reasons for this is that dentists aren’t exposed enough to this type of dentistry or even aware that it exists. Part of the responsibility falls with the dental schools, he says.
"There are advantages to expanding your procedure mix in this day of managed care plans," notes Charles Blair, DDS, founder of Dr. Charles Blair and Associates, Inc., a dental practice management consulting firm in Mount Holly, North Carolina. "The issue here is what kind of remuneration can you receive for the clock hours involved and the learning curve required for this type of niche area."
What will likely prove interesting—if not challenging—about this niche of cooperative dental/medical practice is that dental sleep medicine visits are not covered by dental insurance, according to Blair. What’s more, the medical claim form codes used for these services are different, he explains. For example, medical claim form codes include a variety of diagnostic and treatment codes—as well as a few appliance codes, whereas dental codes are reported only for treatment, Blair says.
Identifying Sufferers Is as Easy as Asking Questions
It’s relatively simple for dental clinicians to initiate the process of identifying patients who might benefit from the services of dental sleep medicine providers. Dentists with some training in dental sleep medicine can help identify individuals who have signs and symptoms of SDB, Friedman says, because some of the anatomic features that contribute to this condition are visible within the oral cavity, as previously mentioned. The patient’s body mass index and neck size are other anatomic variables that are used as part of a formal assessment for SDB, he says.
To begin the process of uncovering "tell tale" signs of sleep breathing disorders, Parker suggests asking every new patient—as well as hygiene patients during each visit—questions such as the following:
• Do you snore or have you been told you snore?
• Do you have trouble staying alert or awake during daily activities such as driving, reading, watching television, or in meetings?
• Do you wake feeling refreshed in the morning?
Friedman uses every hygiene appointment as an opportunity to ask patients:
• How do you sleep at night?
• Do you think you sleep well?
• Are you tired in the afternoon?
• Do you dream often?
• Do you sometimes wake up gasping or coughing?
• Does your bedtime partner say you pause in breathing, or that you toss and turn?
And while you might take personal pride in the fact that your patients fall asleep in your dental chair—meaning, you believe it’s a sign that you and your staff provide a relaxing and comfortable environment—Friedman says it could be a sign of something more serious. It may be that the patient didn’t get a good night’s sleep the night before.
Collaborate With Sleep Physicians
If more probing questions on a medical history questionnaire determine that a more severe SDB problem may exist, then consultation with a sleep medicine physician is appropriate. To practice the standard of care, dentists should become involved with a sleep laboratory that conducts sleep studies, as well as with a board certified sleep physician working at or in conjunction with that sleep center in order to render the sleep breathing disorder diagnosis.
According to Parker, collaboration between dentists and the primary physician or sleep medicine physician is important for providing the best quality of care for people with sleep breathing disorders. What’s more, he says that in most states the standard of care specifies that the diagnosis of a sleep breathing disorder (ie, snoring or sleep apnea) falls within the scope of medicine, while the treatment with oral appliances falls within the scope of dentistry.
"Even if a dentist is treating a patient just for snoring, that’s a medical diagnosis, so they really should have the physician involved in the diagnostic process before treatment is rendered," Parker explains. "If clinicians want to practice in the area of dental sleep medicine and they want to provide appropriate care for patients, then it’s vital for dentists to coordinate care with the sleep medicine physicians in their community."
Ambulatory Sleep Evaluations
If clinicians trained in dental sleep medicine do identify a patient potentially suffering from a SDB problem, an ambulatory evaluation could be used to determine if more testing is necessary. According to Friedman, specific FDA-approved ambulatory devices allow patients to have their breathing tested in their own home. The ambulatory evaluation device that Friedman uses—which is worn on the wrist and uses a probe over two fingers to read the patient’s peripheral artery tone (PAT)—determines whether blood vessels are dilated or constricted and measures respiratory disturbances, oxygen saturation, and actigraphy.5
The data is computer scored by the device itself. The dentist transmits the scores to the board certified sleep physician, Friedman says, who then provides an interpretation of whether the patient shows indications of having a mild problem or something more serious.
"If the respiratory indices as indicated by the ambulatory device are very mild or low, then the sleep physician will usually sign off and approve OAT," Friedman explains. "If the ambulatory screening test reveals values that indicate a more serious SDB problem, the patient would be referred to a qualified sleep physician for more formal testing, and that would probably include an overnight polysomnography (PSG) sleep study. Our present protocol is to have all patients referred for a PSG at the conclusion of our OAT because it is the gold standard for SDB testing."
Getting the Right Training
Most training in this area is conducted through coursework offered by the AADSM, although it is not the only source. The education and training sessions are held throughout the year, at the academy’s annual meeting, and during regionally-sponsored intensive three-day courses. Additionally, Pantino notes that all of the major dental meetings are now beginning to include lectures about dental sleep medicine.
According to Parker, if educational programs or presentations in dental sleep medicine are unbiased, they will present multiple appliances and explain how they work, as well as their respective advantages and disadvantages. Also, Friedman cautions those interested in attending programs about dental sleep medicine to "be a little weary of the potential bias, personal agendas, and priorities of the speakers that might not be consistent with those of the AADSM, which maintains a close alliance with the American Academy of Sleep Medicine (ie, the physician’s group)."
A comprehensive dental sleep medicine presentation will usually include:
• Pathophysiology of snoring and sleep apnea
• How to evaluate and diagnose a patient
• Medical evaluation, testing, and treatment of sleep breathing disorders
• How to coordinate care with sleep medicine physicians
• How oral appliances function
• Information on the most common oral appliances currently being used for sleep breathing disorders
• Insurance reimbursement
• Integrating dental sleep medicine services from a practice management perspective
Pantino explains that what sets dental sleep medicine apart from other aspects of practice is that clinicians must work in a truly interdisciplinary and collaborative manner. Dentists are not permitted to diagnose sleep disorders, he says, so they need to learn how to formulate relationships with area sleep centers and physicians, as well as how to navigate the medical insurance field.
Although passing the certification examination from the American Board of Dental Sleep Medicine is not required in order to practice in this niche area, Parker says that it is strongly recommended. Given annually, the multiple-part examination can be viewed at www.dentalsleepmed.com.
Thinking long term for the dental profession overall, Pantino notes that currently one-third of all dental schools in the United States provide students with some exposure to dental sleep medicine. It may be one or two hours, perhaps during post-graduate education, but it is catching on, he says.
"It takes a while to bring a new discipline into the curriculum, but the AADSM is working toward that goal through the proper channels and groups," Pantino explains. "I feel strongly that dental professionals have a major part to play in this area of patient care, and our profession should no longer be graduating dentists who aren’t knowledgeable about dental sleep medicine."
Conclusion
Dental sleep medicine is an area of dentistry that’s unique in its ability to allow clinicians to have an incredible impact on people’s lives, Parker believes. "We see patients every 6 to 12 months, and we have an opportunity to identify patients with sleep breathing disorders and guide them on a path to better health. Remember: only 10% of them have been diagnosed," he says.
According to Friedman, the increased awareness and interest in dental sleep medicine is consistent with current trends in the profession. It’s now well recognized that oral health has a significant impact on cardiovascular risk factors, and the services that dentists provide benefit their patients’ overall general health and well being. He says that dental sleep medicine fits neatly into this paradigm.
Pantino says that research is continually being published that shows a correlation between sleep apnea and heart attack, stroke, hypertension, depression, memory loss, and other conditions. Because SDB involves an anatomical situation of the upper airway—and considering that no one looks in more mouths than dentists do—Pantino believes that dentists have an opportunity unlike any other health care providers—with their long term and regular access to patients—to assist in the recognition, prevention, and treatment of these conditions.
"When we’re in dental school we’re taught to perform a complete oral cancer screening and evaluate the soft tissues. Most of us won’t treat that disease, but it is absolutely critical to our patients’ overall health and well being that we at least examine them regularly and screen for oral cancer," Pantino explains. "If the dental profession took the same tactic with sleep disorders and learned to evaluate patients with very large tongues, with scalloping on the border, with elongated palates and large uvula, then we would not only be impacting the quality of our patients’ lives, but also the quantity of their lives."
INTERVIEWEE CONTACT INFORMATION
(IN ALPHABETICAL ORDER)
• Charles Blair, DDS
charles@drcharlesblair.com
• Michael DiTolla, DDS
mditolla@glidewell-lab.com
• Mark J. Friedman, DDS
mfriedmandds@mac.com
• Don Pantino, DDS
dpantino@optonline.net
• Jonathan Parker, DDS
jparker@jparkerdds.com
1 Institute of Medicine. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Available at https://www.iom.edu/CMS/3740/23160/33668.aspx
2 American Academy of Dental Sleep Medicine. www.dentalsleepmed.org. Accessed September 15, 2006.
3 Lockerman LZ. Oral appliance management of obstructive sleep apnea: a case report. J Mass Dent Soc. 2006;55:18-20.
4 Ng AT, Gotsopoulos H, Qian J, Cistulli PA. Effect of oral appliance therapy on upper airway collapsibility in obstructive sleep apnea. Am J Respir Crit Care Med. 2003;168: 238-41.
5 Richards D. Dentists treating sleep apnea. CDA Journal. 2006;34:865-867.
SIDEBAR 1
About The American Academy of Dental Sleep Medicine
The American Academy of Dental Sleep Medicine (AADSM) is a professional membership organization that promotes the use and research of oral appliances and oral surgery for treating sleep disordered breathing.2 Established in 1991, the organization also provides training and resources for those professionals working directly with patients.
Members of the AADSM collaborate with colleagues to foster education about oral appliances and the role that dentists can play in the diagnosis and treatment of sleep-related breathing disorders. The academy develops ties with the medical community—particularly sleep medicine physicians and sleep centers—and other professional groups that play an integral part of the sleep disorders treatment and research team.2
The AADSM helps to educate dental practitioners through clinical meetings that make current ideas accessible and establishes and maintains appropriate treatment protocol. The group also conducts community outreach initiatives and works with the community toward increased public awareness of sleep disorders and the role dentists can play in recognizing and treating sleep breathing disorders.2
For more information, visit www.dentalsleepmed.org, or call 708-273-9366.
| Photos above courtesy of Mark J. Friedman, DDS | ||
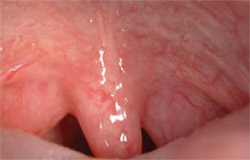 | 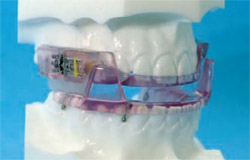 | |
| A microscope image of the oropharynx of a patient who has been diagnosed with severe obstructive sleep apnea demonstrates characteristic narrowing from a wide tongue base, enlarged uvula, and excessively thick soft palate. | The SomnoMed mandibular advancement splint (Denton, Texas) is one of many FDA approved devices that dentists use in oral appliance therapy to treat snoring and obstructive sleep apnea. | |
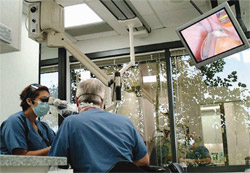 |  | |
| Mark Friedman, DDS, and his auxiliary use a surgical microscope (Global Surgical, St. Louis, MO) to conduct and record the oral exam that includes evaluation of the anatomy of the oropharynx. | Friedmanas office includes acoustic pharyngometry and rhinometry (Eccovision, Hood Laboratories, Pembroke, MA) for SDB screening. Readings are displayed on an LCD screen so patients can better understand how mandibular advancement improves the caliber of the upper airway. | |



