Pandemic Influenza: What’s Real and What’s Not
Margaret I. Scarlett, DMD
Today’s experts talk about what you need to do to be prepared in your practice.
Seasonal influenza epidemics occur every year in the United States in varying degrees of severity. Between 1990 and 1999, flu epidemics caused approximately 36,000 deaths annually, primarily among the very young and the very old. Recently, heightened awareness triggered by reports of avian flu virus transmission to people in Asia has set plans in motion to respond to, and possibly prevent, an influenza pandemic that could cause illness and even death among millions in the United States and worldwide.
SEASONAL VS PANDEMIC INFLUENZA
According to the Centers for Disease Control and Prevention (CDC), seasonal (or common) flu is a respiratory illness that can be transmitted person to person. Most people have some immunity, and a vaccine is available. Pandemic flu is a virulent human influenza that causes a global outbreak (called pandemic) of serious illness. Because there is little natural immunity, the disease can spread easily from person to person. Currently, there is no pandemic flu.
In June 2005, the American Dental Association (ADA) considered a report by Albert H. Guay, DMD, ADA chief policy advisor, on pandemic flu and how dentists across the United States could respond in their community to a future epidemic.1 In this report, Dr. Guay states, “The threat of an influenza pandemic is real, and prediction of a pandemic’s onset or immediate containment remain impossible. Yet, this is not a reason for hysterics or panic. Instead, I urge dentists to pay attention to health reports from around the world, and to look for balanced information from reliable sources—not from alarmist opinions.”
Before panic sets in, relax and become informed. There is nothing to worry about, for now. But the threat is real enough to be prepared to respond, if necessary. Figure 1 shows where human cases of avian flu have occurred. So far, only one potential case of human-to-human transmission has been reported. Luckily, this version of the flu virus does not appear to be easily transmitted from human to human, but this could change.
Any flu pandemic is likely to start in a country where domestic birds are not well monitored. The disease could spread to migratory birds and then to humans. Next, the flu virus must mutate so that it can be readily transmitted from human to human. At that point, social isolation, possibly even quarantine (if necessary), and distribution of vaccine and antiviral medications will be key strategies for responding. But early detection is important. Mass cancellations in your dental practice could be a clue in the detection of an emerging epidemic, but they may also be indicative of seasonal flu. A quick call to your local or state health department can confirm if this is something new or if seasonal flu is widespread in your area.
Given the history of influenza pandemics and the variability in how pandemic flu may occur, the ADA report1 emphasizes that although the federal government has a number of agency-wide plans, there is no specific formula for responding at the local level. These plans must be customized depending on what unique situation could emerge and the most appropriate strategy for response.
“Local circumstances will dictate how dentists may respond,” Dr. Guay said. “An overriding principle is that most dental care is postponable, and patients with suspected infectious flu can have necessary dental care postponed until after the infectious stage is over. For ill patients who need emergency dental care, they should be referred to a central facility where people with acute and infectious respiratory conditions can be treated, similar to what is recommended for suspected active tuberculosis patients.”
Dr. Guay also reported to the ADA Board of Trustees, “The planning and integration of the primary response by dentists in the event of a bioterrorism attack or mass casualty event recommended to the state societies should be of great value in preparing dentists to aid in the event of an influenza pandemic.” He believes that dentists could be called upon to provide an array of services, including giving vaccinations, dispensing medications, providing medical care, and helping conduct surveillance. “Therefore,” he says, “dentistry should work to ensure that dentists, their staffs, and their families are given a high level of priority for receiving vaccines and medications in hard-hit areas.”
DENTAL OFFICES SHOULD BEGIN PREPARATIONS EARLY
At least two ADA councils are exploring special considerations for pandemic flu preparedness and response in the dental office. The US Public Health Service has been training its dentists on the administration of immunizations, although it is important to note that the authorization for dentists to administer vaccines is applicable only when the officer has been deployed to serve as a vaccine administrator and is part of an official activation of the commissioned corps for emergency response. For dentists in private practice, each state makes decisions about who can give injections for medical purposes, including vaccinations. Therefore, the inclusion of civilian dentists in pandemic vaccination or other vaccination plans would be primarily a state and local prerogative. Consideration is also being given to the possibility of using dental offices as temporary clinics if key medical centers are overwhelmed with patient care.
BE READY TO TAKE ACTION IF NECESSARY
What specific actions can you take to prepare for pandemic flu in advance?
- Have an information database back-up for your computerized records. This can be accomplished on a secure Web site for a fee or with your own tape or disk back-up systems. Make an extra copy and designate another staff member, in addition to yourself, to take a copy of the tapes or disks with them, should it be necessary to close your office. This may be useful for tracking and identifying cases of potential flu or pandemic flu, especially in the case of mass cancellations of appointments.
- Develop a plan of how you and your staff will work together. Talk to your family and have a communications plan in the event of a pandemic response. Let them know how you will communicate and where you will meet in the case of an emergency. For information about developing an office plan, access the Small Business Administration Web site: https://www.sba.gov/disaster_recov/prepared/getready.html. Another resource is by the Institute for Business and Home Safety entitled, “Open for Business: A Disaster Planning Toolkit,” which is available at https://www.ibhs.org/docs/openforbusiness.pdf .
The US Department of Health and Human Services (DHHS) and CDC also have developed a checklist to help medical offices and clinics improve their readiness to respond to pandemic flu. Many of the topics addressed in the checklist, which is modeled after a pandemic preparedness checklist for hospitals, are relevant to other outpatient settings, such as dental offices, which provide occasional or ongoing health care services. This checklist can be adapted to meet the unique needs of individual health care clinics or offices and is available at www.pandemicflu.gov.
Faith-based and community organizations undoubtedly will play an integral role in responding locally in the event of a pandemic, and dentists and their staff members may find themselves involved in these efforts as well. The DHHS and CDC have developed a checklist, also available at www.pandemicflu.gov, to assist community organizations with their planning.
WHAT ARE THE EXPERTS SAYING?
The CDC has many scientists involved in influenza research, and they have developed a software application, Flu Aid 2.0, that provides users with estimates for deaths, hospitalizations, and outpatient physician visits based on data from the last three pandemic flu cycles. The CDC estimates that a medium-level pandemic could produce up to 207,000 deaths in the first 6 months, and between 314,000 and 734,000 hospitalizations across the United States. A minimum of 18 to 42 million outpatient visits to hospitals would occur in an initial 9-month influenza outbreak. Estimates of the economic impact are between $71.3 and $116.5 billion.
“How badly a potential pandemic might affect the United States is anybody’s guess,” Dr. Guay states, “But we do know that our public health infrastructure in the United States is vastly different than in the past, when devastating influenza pandemics hit with little warning. By the time a threat is real, there will be information accessible to dentists. If there’s a case of avian flu anywhere in the world, the CDC and World Health Organization (WHO) will likely know the next day. This situation is not the same as the recent SARS epidemic, when emerging cases were initially kept secret.”1
One of the premier influenza experts in the country, Nancy Cox, PhD, is head of the Influenza Division at CDC and Director of WHO’s Collaborating Center for Influenza. In an attempt to learn what made a previous influenza epidemic so deadly, Cox and her team recently worked with colleagues outside the CDC to reconstruct the 1918 pandemic influenza virus that killed millions of people worldwide. They also worked in the highly secure CDC laboratory on an experiment that involved combining the current H5N1 (avian influenza A) virus with a currently known and contagious human flu virus.
“What we’re trying to determine is whether or not the avian flu virus genes and the human influenza genes can work together,” Cox says. The answer to this question could be critical for researchers everywhere who are working to prevent a future pandemic. “I greatly enjoy the significant scientific challenge of working on influenza, a disease of great public health importance caused by viruses that are constantly changing and surprising us,” she says. “Currently, the biggest challenge is preparing for the threat of pandemic influenza posed by the influenza A/H5N1 viruses circulating in poultry in Asia, Africa, Europe, and the Middle East. Although these viruses may not cause the next influenza pandemic, their widespread circulation and broad host range make them a particularly difficult challenge.”
WHERE TO FIND OUT MORE ABOUT AVIAN FLU
According to the WHO Weekly Epidemiological Record,2 although data were reported from the international community in different formats and with varying degrees of consistency and reliability, certain conclusions could still be drawn:
- New countries reporting human cases increased from four to nine after October 2005.
- Half of the cases occurred in people younger than 20 years of age, with 90% of the cases in people under 40 years of age.
- The overall case fatality rate was 56%. Case fatality was high in all age groups but was highest in persons aged 10 to 39 years.
- The case fatality profile by age group differs from that seen in seasonal influenza, in which mortality is highest in the elderly.
- The overall case fatality rate was highest in 2004 (73%), followed by 63% to date in 2006, and 43% in 2005.
- Assessment of mortality rates and the time intervals between symptom onset and hospitalization and between symptom onset and death suggests that the illness pattern has not changed substantially during the 3 years.
- Cases have occurred year-round. However, the incidence of human cases peaked in each of the 3 years in which cases have occurred during the period roughly corresponding to winter and spring in the northern hemisphere. If this pattern continues, an upsurge in cases could be anticipated starting in late 2006 or early 2007.
PANDEMIC PLANNING IN THE UNITED STATES AND WORLDWIDE
In early 2006, the United Nation Secretary-General, Kofi Annan, announced a seven-point plan for avian flu response:
- improving bird monitoring
- focusing on research in human animal contact
- minimizing pandemic impact
- ensuring access to medicines
- facilitating speedy vaccine discovery
- communicating effectively
- coordinating public health-care efforts with political leaders.
To speedily detect any novel influenza subtypes, including avian flu and any others that might emerge, WHO has at least four Reference and Research Centers on Influenza to track the disease around the world. The key is international collaboration and cooperation and the engagement of credible scientists in the response. Surveillance and early detection are the initial steps in understanding and ultimately containing an influenza outbreak. In the event of a pandemic, the United States will work collaboratively with WHO and other countries’ health ministries on detection, monitoring, and response.
Here in the United States, as elsewhere, it will be important to ensure a rapid and sustainable health care response in the event of pandemic flu. Beginning this year, DHHS Secretary Michael Leavitt held pandemic flu summits with key leaders in many states. Accompanying him was Julie Gerberding, MD, MPH, Director of the CDC. They met with public health experts, business leaders, education leaders, and representatives of faith-based communities. These meetings addressed the role of maintaining essential services and preparedness in the event of pandemic influenza based on the “National Strategy for Pandemic Influenza,”3 which was issued by the White House in November 2005 as a roadmap for the country’s overall response.
The “Implementation Plan for the National Strategy,”4 which was released by the President in May 2006, translates the “Strategy” into more than 300 actions for federal departments and agencies and sets clear expectations for state and local governments and other nonfederal entities. The “National Strategy” includes an overview of the threat of pandemic influenza, a description of the relationship of this document to other federal plans, and an outline of key roles and responsibilities during a pandemic.
In addition, the “HHS Pandemic Influenza Plan”5 specifies needs and opportunities to build robust preparedness for and in response to pandemic influenza. The preparations made for a pandemic today will have lasting benefits for the future. The goals of the national plan are to stop, slow, or otherwise limit the spread of a pandemic to the United States; to limit the domestic spread of a pandemic and mitigate disease, suffering, and death; and to sustain infrastructure and mitigate the impact on the US economy and other functions of society.
An accompanying volume, the “Public Health Guidance on Pandemic Influenza for State and Local Partners,”6 provides 11 supplements for more detailed and rapid response at the state and local levels. Major components of the critical preparedness and ready response actions include:
- Intensifying surveillance and collaborating on containment measures, both international and domestic.
- Stockpiling antivirals and vaccines and working with industry to expand capacity for production of these medical countermeasures.
- Creating a seamless network of federal, state, and local preparedness activities, including increasing health care surge capacity.
- Developing the public education and communications efforts that will be so critical to keeping the public informed.
Strategies outlined in the “HHS Plan”5 are based on an understanding of pandemics and influenza disease, guided by several overarching principles:
- Preparedness will require coordination among federal, state, and local governments and partners in the private sector. This includes your dental office.
- An informed and responsive public is essential for minimizing the health effects of a pandemic and the resulting consequences for our citizens.
- Domestic vaccine and production capacity sufficient to provide vaccine for the entire US population is critical.
- Quantities of antiviral drugs sufficient to treat 25% of the US population should be stockpiled.
- Sustained human-to-human transmission anywhere in the world will be the triggering event to initiate a pandemic response by the United States.
- When possible and appropriate, basic public health measures will be used to reduce person-to-person viral transmission and prevent or delay influenza outbreaks.
- At the start of a pandemic, a vaccine—which will initially be in short supply—will be procured and distributed to state and local health departments for the immunization of predetermined priority groups.
- At the onset of a pandemic, antiviral drugs from public stockpiles will be distributed to predetermined priority groups.
Congress recently allocated $225 million for addressing identified gaps in pandemic influenza preparedness planning. This funding is part of $350 million included in emergency appropriations for upgrading state and local pandemic influenza preparedness passed by Congress in December 2005.
“These funds will build on the work begun at the summits and help local, tribal, territorial, and state public health officials as they undertake critical preparedness planning that communities must do themselves,” Secretary Leavitt said. Grants will be awarded to all 50 states, the District of Columbia, three local jurisdictions (New York City, Chicago, and Los Angeles County), five US Territories, and three Freely Associated States of the Pacific.
CONCLUSION
There is no way to predict whether influenza A/H5N1 or another viral strain will cause the next pandemic or when it will hit, but most experts agree that such an event is not only likely, but certain. Because the threat is real, dentists should take every opportunity to prepare. Working together, state dental societies and local health departments can help develop a framework to guide dentists in providing valuable information and assistance to people in the event of pandemic flu.
References
1. Guay AH. Influenza pandemic. Available at: https://www.ada.org/prof/resources/topics/report_influenza.pdf. Accessed August 29, 2006.2. World Health Organization. Epidemiology of WHO-confirmed human cases of avian influenza A(H5N1) infection. Wkly Epidemiol Rec. 2006;81(26):249-260. Available at: https://www.who.int/csr/disease/avian_influenza/guidelines/en. Accessed August 29, 2006.
3. National Strategy for Pandemic Influenza. Available at: https://www.whitehouse.gov/homeland/pandemic-influenza.html. Accessed August 29, 2006.
4. Implementation Plan for the National Strategy for Pandemic Influenza. Available at: https://www.whitehouse.gov/homeland/pandemic-influenza-implementation.html. Accessed August 29, 2006.
5. US Department of Health and Human Services. HHS pandemic influenza plan. Available at: https://www.hhs.gov/pandemicflu/plan/. Accessed August 29, 2006.
6. US Department of Health and Human Services. Public health guidance on pandemic influenza for state and local partners. Available at: https://www.hhs.gov/pandemicflu/plan/part2.html. Accessed August 29, 2006.
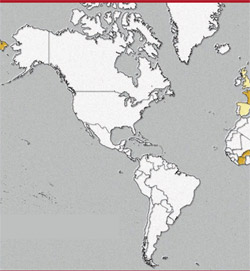 | 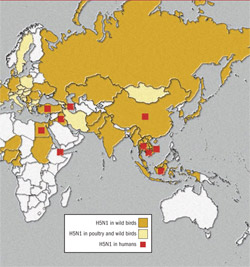 | |
| Figure 1 The red dots on the map show where human cases of avian flu have occurred. | (Map courtesy of the US Department of Health and Human Services.) | |
| About the Author | ||
| Margaret I. Scarlett, DMD President Scarlett Consulting Atlanta, Georgia | ||



