Making Implants Your First Option
Jon Julian, DDS
According to surveys mentioned in recent dental journals and magazines, only 5% to 10% of all general dentists are currently involved in surgically placing implants.1 However, more than 80% of general dentists are restoring some implant cases. Eventually all general dentists will be faced with the issue of performing hygiene and routine maintenance on prosthetically restored implants. They will also be faced with the issues of treating or referring implant patients when such problems as peri-implantitis or occlusal traumas arise. The sheer numbers of patients who are or will become implant candidates is growing exponentially. The aging population (baby boomers who are over the age of 50) are maintaining good health longer.2 These individuals are interested in preserving their health very actively, which means preserving their teeth or replacing their teeth with lifelike substitutes instead of full or partial dentures. To this end, more endodontic procedures are being performed to more existing teeth than ever before. However, decay and/or endodontic failure leads to more than 30% of 50- to 59? -year-olds having single or multiple posterior edentulous spaces.3
It has been estimated that more than 1 million people in the United States are missing one or more teeth.4 Many patients are unhappy with the fit, retention, appearance, and/or function of their existing removable dentures and partial dentures, and some are even unhappy with their fixed bridges. Many of these patients have settled for the basic dentistry that their dentists learned in dental school, even if both dentist and patient would like a better solution or a higher level of tooth replacement.
It could be suggested that potential implant cases are simply referred to specialists, but this does not happen in most practices for many reasons. Many general dentists have communicated to this author that the lack of experience and education of the general dentist in implantology causes a minimal number of refer-rals and contributes to communication gaps with the specialists. By educating the general dentist about implants, he or she can develop the skills to diagnose, treatment plan, and, when appropriate, refer the patient for treatment, or perform the treatment themselves. General practitioners must understand the current state of implant therapy as well as the choices currently available.
IMPLANT-RELATED CONCERNS
Implants have undergone several engineering and technological advancements in recent years. Today, implants can be placed easily and routinely in many patients with little trauma and an expected success rate of more than 95% over a period of 10 to 15 years.5 Implants can be used to replace single teeth or multiple teeth, and they can support fixed bridges or removable full dentures. In addition, they do not suffer from recurrent decay or endodontic problems. In this author’s opinion, implants have become the longest lasting, most stable, most functional, and the most natural long-term replacement for missing teeth. Nevertheless, implants are not real teeth and the inexperienced dentist should learn to manage a few key concerns.
Because implants are not real teeth, the nature of the tissue-to-abutment connection must be learned and understood. This connection consists of a mucopolysaccharide substance that glues the tissue to the metal or zirconia structures. This becomes a weak attachment but is successful in maintaining the health of the peri-implant tissue as long as it is not disturbed. It is this author’s opinion that routine probing with a periodontal probe around implants should be avoided so as not to damage this attachment. In addition, if a problem arises, successful pathology management needs to be well understood. The surface of the implant must be debrided and sterilized, then grafting, if indicated, can be performed. When grafting is not indicated, soft tissue healing can occur in a healthy environment. As the general dentist becomes more experienced, he or she will be able to differentiate the simple problems from the more complex. Hygienists will also learn to evaluate peri-implant tissue without probing through the delicate tissue to the abutment/crown complex junction. This education should filter from experienced clinicians, schools, and hygiene training programs. Therefore, it is very important for hygienists to keep up with new advances as well.
Secondly, because many different implant systems exist today, there is a confusing number of styles, sizes, parts, tools, coatings, and choices available. It is difficult for the experienced implant dentist to keep up with the variety of implants available. Without experience or education, the general dentist may struggle just to understand the implant process, let alone be willing and able to have the appropriate tools and parts available for connecting prosthetic parts.
This creates a complex dilemma for the dental profession. It is the author’s opinion that 90% of all general dentists are not trained to properly diagnose and treatment plan for implant therapy. They also are not comfortable providing recommendations or referrals for implant therapy for their patients. This is one of the main reasons why many patients are not offered or encouraged to have implant therapy. But if implants are planned, then coordinating the specialist with the referring general practitioner to think along parallel lines and to use the same or at least familiar brands of systems is complicated because there are dozens of implant companies out there. Each has their own variation of shapes, sizes, parts, and tools.
Follow-up care and maintenance are also poorly understood and not competently delivered to patients. In fact, as it now stands, it is very difficult to accomplish implant therapy to the satisfaction and benefit of patients on a routine basis. For this situation to improve, the general dentist must become educated on implant therapy.
When general dentists educate themselves on the benefits as well as the technical aspects of placing and restoring implants, they will be prepared to help their patients receive a higher quality of care. Whether that means surgically placing implants themselves or referring to a specialist, it will definitely increase the number of clinical cases in which implants are recommended. Only through education and experience will the general dentist develop the comfort level and skill level to appropriately diagnose and/or refer patients for implant therapy. This can become as routine as doing crown-and-bridge work, endodontics, dentures, and all other dental procedures that general dentists have grown accustomed to dealing with in their practices. If general dentists can visualize the benefits and value of implants, then they will want to take the steps necessary to provide patients with the option of implant therapy whenever tooth replacement is an option.
Single-Tooth Replacement
Single-tooth replacement can be accomplished in an atraumatic fashion without disturbing the adjacent teeth. Depending on the individual clinical situation, a flapless procedure can be accomplished in 30 minutes or less and the patient will feel less trauma than a conventional extraction or root canal. The final restoration can be placed in 4 months, and will mimic natural tooth form and function. Along with flapless procedures, small envelope flaps or full-flap procedures might be indicated according to the decision of the clinician. When the implant can be placed with a minimum of 25 Ncm torque, then stability would allow immediate temporization with a non-occluding temporary.
Sometimes when a tooth is extracted, an implant can be placed immediately into the extraction site. Again, when the clinical situation allows it, the implant can be immediately loaded for esthetics and tissue shaping. The clinician must be certain that there is no pathology present in the extraction site to ensure success. The way to accomplish this is by using a CO2 laser to sterilize the extraction site thoroughly because the laser energy kills all potential pathogens. This scenario also allows for placement of the final crown in 4 months.
Multiple-Tooth Replacement
Multiple teeth can be replaced by single implants (one implant per tooth) or by bridges. Good engineering, preplanning, and common sense are helpful when dealing with multiple-tooth replacement situations. This allows the clinician to restore a quadrant or even a full arch esthetically and functionally. With a little creative thinking, even unusual situations can be solved. When there is too little space for two implants but two teeth are being replaced, with the help of a good laboratory the final result can be functional and esthetic (Figure 1A; Figure 1B; Figure 1C; Figure 1D). In this example, two teeth are missing, but 9 mm of space is inadequate to place two implants. Therefore, a single implant supports a large abutment that, in turn, supports the all-ceramic crown shaped to appear as two crowns.
ESTHETICS
The anterior veneer or esthetic crown case can be accomplished as well as or better with implants than with bridges. Using the newest zirconium abutments allows the laboratory to match shades of pressed ceramic restorations to perfection. Whether a single implant for multiple teeth or multiple implants for multiple teeth are placed, the esthetic result can be natural and beautiful. Pretreatment wax-ups and surgical stents are a must for the best esthetic result.
THE IMPLANT-SUPPORTED DENTURE
Mandibular dentures have challenged dentists and their patients for many years. Lower dentures can be stabilized by a variety of attachments such as O-rings, hader bars, nylon clips, locator attachments, and other options, all anchored by two to four implants. There is a new type of implant-supported denture called SynCone® (Dentsply Friadent CeraMed, Lakewood, CO) that uses a friction-fit concept between a metal female housing in the denture and a metal male attachment anchored to the implants (Figure 2A; Figure 2B; Figure 2C; Figure 2D; Figure 2E). This design eliminates wearing out of parts. It also allows the denture to lightly touch the tissue on the ridge without allowing movement of the denture. Therefore, the patient will not experience any sore spots. Mandibular dentures require four implants while maxillary dentures require six implants. It is also possible to place the implants and attach the denture in a single appointment and the patient can either have a new denture made, or their existing denture can be used. With this type of support, the denture will allow the patient to chew any type of food.
CASE REPORT
The patient presented for a second opinion consultation. She had recently lost a fixed bridge in her upper left quadrant and was unsure about the treatment plan recommended by her dentist (a new bridge to replace the old one) (Figure 3A). When asked what she would like, she responded that she did not know but she wanted something that would work well and last a long time. It was pointed out to her that she exhibited a lack of room vertically and that her only remaining posterior abutment which was previously treated endodontically was now failing (tooth No. 15) (Figure 3B). We asked permission to take records (impressions, panoramic radiographs, a health history, and photographs) and set a time for a treatment plan consultation.
The patient and her husband returned the next day for the consultation, which included treatment options that would give her maximum function for the longest time (implants were one of our first recommendations). Yet she had no knowledge of implants as this had not been discussed with her previously. She saw photos of before-and-after treatments similar to hers. When she indicated she desired the solution offered, we spoke about finances. At this point, she made a commitment to long-term, high-value dentistry, including implants and crowns to establish a new vertical place of occlusion and provide her with individual, real teeth (Figure 3C and Figure 3D). The treatment consisted of establishing the new plane of occlusion with the acrylic temporaries patterned from the pretreatment wax-up. Crowns were placed on teeth Nos. 3, 6, 8, 9, 11, and 30; implant-supported individual crowns were placed on teeth Nos. 4, 5, and 12 through 14.
CONCLUSION
All of the previously mentioned scenarios are within the scope of the general dentist who possesses an appropriate amount of education and experience. The benefits include a more competent practitioner who has elevated his or her practice to a higher level of success, who can intelligently and knowingly communicate specific goals to any specialist and work with a single specialist or as part of a team, who sees implants as a first-order treatment plan to replace missing teeth, and who is willing to benefit his or her patients with a higher quality of service. Patients will realize the value of success over time. They will receive the function and the esthetics of real teeth. They can improve the quality of their lives if their general dentist will take the first step of taking courses to improve his or her own capabilities.
References
1. Dental Products Report 2003; Implant Survey.2. Guyer B, Freedman MA, Strobino DM, et al. Annual summary of vital statistics: trends in the health of americans during the 20th century. Pediatrics. 2000;106(6):1307-1317.
3. Christensen G. Chicago Dental SocietyMid Winter Conference: February 2004. Chicago, IL.
4. American Dental Association, 1997 Survey of Consumer Attitudes and Behaviors Regarding Dental Issues, Dental Habits of the US Population; US Dept of Health and Human Services, National Center for Health Statistics and National Institute of Dental Research.
5. Gunne J, Astrand P, Lindh T, et al. Tooth-implant and implant supported fixed partial dentures: a 10-year report. Int J Prosthodont. 1999;12(3):216-221.
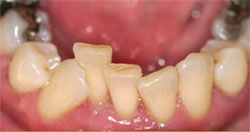 | 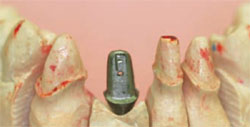 | |
| Figure 1A Crowded mandibular incisors. | Figure 1B Abutments on the working model. | |
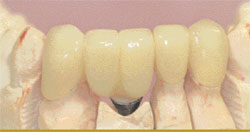 | 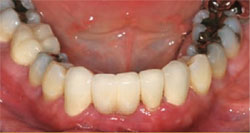 | |
| Figure 1C Two restored teeth on one abutment. | Figure 1D The final restorations placed in the mouth. | |
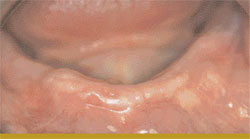 | 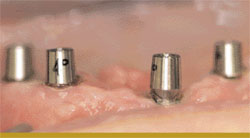 | |
| Figure 2A An edentulous lower ridge. | Figure 2B Four 4° SynCone® abutments placed. | |
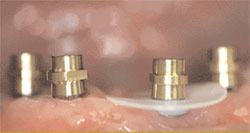 |  | |
| Figure 2C Four female SynCone® pick-up caps. | Figure 2D The newly relined denture with the SynCone®caps. | |
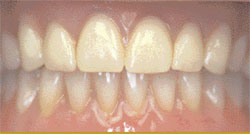 | ||
| Figure 2E The final implant-support denture. | ||
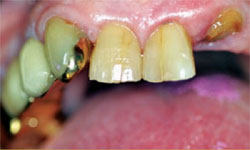 | 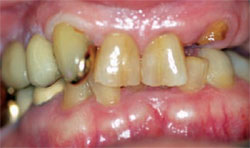 | |
| Figure 3A At the initial exam, the patient presented with a missing bridge. | Figure 3B Over-closed significant loss of vertical in full occlusion. | |
 |  | |
| Figure 3C Full-face view before treatment. | Figure 3D The full-face view after treatment. | |
| About the Auhtor | ||
 Jon Julian, DDS Jon Julian, DDS Private Practice McPherson, Kansas | ||




