Restoration of Hypoplastic Enamel Defects: Methodology and Instrumentation
Robert A. Lowe, DDS
One challenging area of elective esthetic dental treatment for the restorative dentist is hypocalicified enamel defects in the esthetic zone. This problem is magnified when the defects are prominently displayed in the middle of a maxillary central incisor. Some of these defects can be treated with microabrasion1-3 if they are on the enamel surface only (eg, demineralization from orthodontic brackets). However, if the defect spans the thickness of the enamel to the dentino-enamel junction, microabrasion will not be effective. To remove these unsightly defects mechanically with a bur or hard tissue laser and restore them with direct composite is usually the conservative treatment of choice. The challenge is for the restorative dentist to create a restoration for these areas that blends esthetically with the surrounding natural tooth structure and, at the same time, is as conservative as possible in tooth preparation. This article will discuss some principles of esthetic treatment planning for direct anterior composites that can be applied to many different clinical situations that occur in everyday practice.
Maxillary Anterior Tooth Morphology
Maxillary anterior teeth, the heart of the esthetic zone, are tri-planar by nature from both the facial and proximal aspects. Proximal facial line angles are positioned so that portions of the mesial and distal surfaces are visible from the straight-on facial perspective. Prominence of these line angles and lobal concavities (the prominent middle lobe being the largest of the 3) on the facial surface make the facial anatomy of the maxillary central and lateral incisors come alive. Three distinct proximal planes are seen in a facial view of the maxillary central incisor:
- From the exit of the periodontium to the apical boundary of the contact zone;
- From the apical boundary of the contact zone to the apical extent of the incisal embrasure; and
- From the apical extent of the incisal embrasure to the incisal edge.
The contact zone is the area between adjacent teeth where they appear to touch. The actual proximal contact is only a small portion of the contact zone located toward its incisal boundary. A proximal view of a maxillary central incisor shows the 3 distinct planes of the facial surface:
- From the exit of the periodontium to the height of contour (approximately 1 mm);
- From the height of contour to the junction of the middle and incisal one thirds; and
- From the junction of the middle and incisal one thirds to the incisal edge.
The creation of the third plane (incisal plane) toward the palatal aspect is crucial for both function and esthetics.4
Histologic Creation of an Esthetic Direct Composite Restoration
To duplicate the esthetics of nature in teeth using composite materials, it is the opinion of the author that the restorative dentist must understand the histologic difference in the clinical appearance of enamel and dentin. It is clinically difficult in most situations to simply choose one body shade of composite that matches all areas of the tooth to be restored, even with the so-called chameleon effect.5-7 The inherent opacities of dentin and enamel histologically require that different opacities of composite material be used as a specific replacement for each tissue type. A more opacious material is required for a dentin replacement, whereas a more translucent material is needed to replace enamel. The goal is that some of the dentin layer will be visible through transparent enamel and create a depthof color in the restoration. Many composite materials, as the one used in this clinical case (Premise™, Kerr Corporation, Orange, CA), give dentists options in opacities for the various Vita® shades (Vident, Brea, CA) as well as transparent enamels to create incisal effects.
Mopper described a technique for creating invisible Class III and Class IV composite restorations by creating a long bevel and feathering out the composite material to a knife-edge to make the margins disappear.8 This technique takes advantage of the translucent nature of composite material as its thickness decreases, thereby allowing the natural tooth color underneath to blend as the restorative material reaches the preparation margin. The secondary benefit of the long bevel (≥ 2 mm to 3 mm) is to increase the micromechanical retention of the restorative material itself. When restoring an anterior incisal edge, it is the opinion of the author that functional stress requires a preparation with more surface area to retain the restorative material successfully without fracture.
The next step is to determine where to place the restorative margins so that they will more readily blend or disappear. A good comparison is how a plastic surgeon hides incisions (scars) when performing facial procedures. The incisions are placed parallel to the natural folds or contours of the skin so that they are camouflaged and blend with the patient’s natural facial contours. This idea should then be carried over to the restorative margin of a composite restoration, which is actually a scar on the surface of the tooth. With this idea, the best anatomical place to hide that scar is the facial proximal line angles of the tooth where the facial plane meets the proximal surfaces. Parameters can now be formed for margin placement based on maximum esthetics, which will also create better microretentive form for the restoration.
The only restorative margin that can be more difficult is the one joining the mesio-proximal to the disto-proximal that crosses the facial surface of the tooth. Remembering the 3-plane nature of the facial surface, it is best to try and place the margin at the intersection of these planes when possible. Straight-line margins are more difficult to hide than slightly curved, or tortuous (wavy) ones; therefore, connecting the proximal line angles with a straight line across the facial surface should be avoided whenever possible.
Case Report
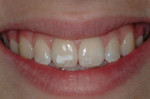
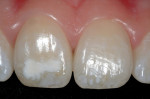
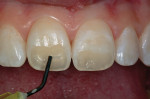
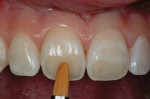
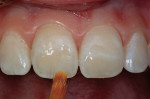
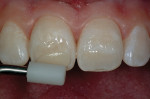
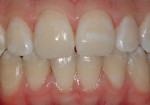
This teenaged patient (Figure 1 and Figure 2) presented with hypoplastic defects on the facial surfaces of teeth Nos. 8 and 9. Typically, these patients are very self-conscious about the appearance of their “front teeth” and an esthetic, conservative solution for this problem will help elevate the patient’s self esteem and self-confidence at an important stage in his or her social development. Upon clinical inspection, it is important to note that there was a minimal amount of dehydration present in the patient’s adjacent teeth. A good reference is to take digital preoperative photos of the patient’s unretracted smile as well as a full-arch retracted view. These photos can then be downloaded and printed for reference during the procedure, since the surrounding teeth may become more dehydrated during the actual placement of the restorative materials. Referring to the preoperative photographs will help avoid matching the restorations to the overdehydrated appearance of the neighboring teeth as the procedure progresses.
Tooth Preparation and Treatment of the Enamel and Dentin Surfaces
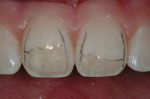
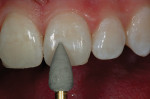
The operative plan (Figure 3) was outlined on the facial surfaces of teeth Nos. 8 and 9 using a sharp, sterilized No. 2 pencil. Note the positions of the facial proximal line angles and the planned margin placement to join the mesio-proximal to the disto-proximal margins.
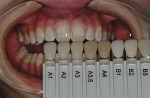
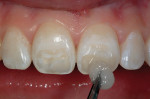
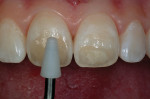
After placement of local anesthesia, a small 1¾–round diamond was used to remove the hypoplastic defects to the dentino-enamel junction (Figure 4). A pointed diamond instrument was used to create the bevels around the preparation and extend them to the outlined parameters. It is important to note in the incisal portion of the preparation that creation of the bevel also means removal of tooth structure in the anterior-posterior dimension. Creating enough space for the application of both dentin replacement and enamel replacement is critical to esthetic success. If this area of the tooth is not reduced enough in the palatal direction, the result will be removal of the enamel layer during the finishing and contouring process. It is important to anticipate the amount of space (approximately 1 mm) needed to place both histologic layers on top of one another to create the proper optical effect without producing an overcontoured restoration. It is easier to choose the appropriate shade for the dentin replacement after completion of the preparation because the surface hypocalicification has already been prepared away (Figure 5).
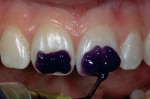
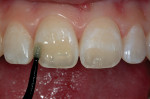
Once shade selection was completed, the restorative process began. First, both preparations were etched with 37% phosphoric acid for 15 seconds (Figure 6). Then, the etchant was rinsed off of the preparations vigorously for at least another 15 seconds. The preparations were thoroughly dried, then rewetted with a desensitizer (AcQuaSeal™ G, AcquaMed Technologies, Inc, Batavia, IL) (Figure 7) and high-volume suction was placed within 1 mm of the prepared surfaces for 2 seconds (Figure 8), then removed. This created a perfect, moist surface to place a hydrophilic primer. It was not overly desiccated (collapsed collagen) and not too moist. A fifth-generation dentin bonding adhesive (Optibond® Solo Plus™, Kerr Corporation) was copiously placed with a microapplicator and agitated into the prepared surface (Figure 9). After air thinning and evaporation of the solvent (ethanol), the adhesive was light-cured according to the manufacturer’s instructions.
Restorative Sequence and Placement
The first step in the restorative process was to place a thin (< 0.5 mm) layer of flowable composite (shade A3 or A3.5) on the surface of the entire preparation (Revolution® Formula 2™, Kerr Corporation, was used in this case) (Figure 10). The shade was not critical because of the thinness of this layer. Upon curing, the flowable resin created a sticky surface on which to place additional increments of microhybrid composite. A sable artist’s brush was used to thin out the flowable composite layer before curing (Figure 11). In some cases, the flowable layer can be used to opaque out any remaining undesirable color on the remaining dentin and create a common color to the underground before additional composite application. After curing of the flowable layer, the chosen shade of dentin replacement (in this case, A2) was syringed to place on the facial surface (Figure 12).
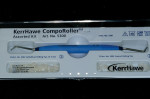
One of the challenges with direct composite placement has always been the creation of layers with uniform thickness, contour, and homogeneity. This has been traditionally difficult to perform using a bulk-fill technique and a composite spatula. A unique composite placing instrument called a Comporoller™ (Kerr Corporation) (Figure 13) was used in the incremental placement of the composite materials for this case and demonstrates a reliable method to develop these layers quickly with the correct contours so that the amount of contouring and finishing postplacement is greatly reduced.
The disposable cone tip of the instrument was used to flatten and spread the dentin increment in the mesio-distal and cervico-incisal directions (Figure 14). A good analogy for the proper use of this instrument is like applying paint on a wall with a paint roller or rolling a piece of dough into a thin piecrust. Changing the direction of the instrument slightly while rolling the composite will spread the material evenly and uniformly over the prepared surface. After shaping the dentin increment during placement the increment was light-cured for 20 seconds. At this point, the facial contour of dentin increment was still palatal to the intended final facial position of the completed restoration. This was to allow the space required for the enamel increment in the facial-lingual (palatal) dimension to bring the completed restoration to full contour. With the dentin increment cured, composite tints were placed and cured before placement of the transparent enamel layer to create internal effects similar to those created by a ceramist. Because there was a degree of what the author calls an “enamel whitewash” appearance to the patient’s natural teeth, a thin layer of white composite tint was interposed between the dentin and enamel layers to duplicate this effect (Figure 15). A good idea is to reference the preoperative photograph to determine the concentration or amount of tint to be placed. After spreading the white composite tint with the artist’s brush, it was light-cured for 10 seconds. Next, the enamel layer was dispensed and then contoured using the cylinder end of the composite placing instrument (Figure 16). The cone end was used to create line angles (Figure 17) and texture as the material was uniformly spread across the facial surface. When the contours were completed, the surface could be uniformly smoothed using the artist’s brush, if necessary. The final increment of the restoration was light-cured according to the manufacturer’s specifications.
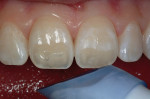
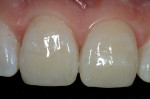
An 8-fluted composite finishing bur can be used to smooth any marginal discrepancies, but the author has found that the use of the Comporoller greatly reduces the need for gross rotary contouring and finishing. Medium and fine composite polishers can be used to create reflectivity and surface texture to the completed restoration (Figure 18). The final luster was accomplished using an Occlubrush® cup (Kerr Corporation). A surface sealant was then applied after a 5-second etch with 37% phosphoric acid to clean the surface of the restoration. Figure 19 and Figure 20 show the completed views of the restorations on teeth Nos. 8 and 9, eliminating the hypoplastic defects and creating esthetic harmony with the surrounding environment.9-12
Conclusion
A clinical case has been presented showing a step-by-step approach to esthetically repairing deep hypoplastic enamel defects using composite resin. Proper preparation design and bevel placement are critical to maximize esthetic results. A unique composite placement instrument was used that allows for expedient and uniform placement of direct composite materials creating beautiful esthetic results.
References
1. Croll TP, Helpin ML. Enamel microabrasion: a new approach. J Esthet Dent. 2000;12(2):64-71.
2. Croll TP. Enamel microabrasion: observations after ten years. J Am Dent Assoc. 1997;128(Suppl):45S-50S.
3. Croll TP. Combining resin composite bonding with enamel microabrasion. Quintessence Int. 1996;27(10):669-671
4. Lowe RA. Provisionalization: mastering the morphology. Dental Products Reports.2003;37(8):56-58.
5. Nash RW. Freehand composite veneering—the direct option. Pract Periodontics Aesthet Dent. 1994;6(3):89-95.
6. Fahl N Jr. Predictable aesthetic reconstruction of fractured anterior teeth with composite resins: a case report. Pract Periodontics Aesthet Dent. 1996;8(1):17-31.
7. Lowe RA. A unique matrix option for anterior direct composite veneers. Contemp Esthet Restorative Pract. 2005;9(6):46-50.
8. Mopper KW, Nash RW. Freehand bonding makes a comeback. Cosmetic Dentistry for GPs. 1991;4(12):2-4.
9. Lowe RA. Long-term provisionals for transitional dentition using direct composites. Dental Products Reports. 2002;36(3):64-65.
10. Lowe RA. The restoration of maxillary anterior teeth using microfil and microhybrid composites:a clinical comparison. Contemp Esthet Restorative Pract. 2002;6(1):52-53.
11. Dietschi D. Free hand composites: a key to anterior esthetics. Pract Periodontics Aesthet Dent. 1995;7(7):15-25.
12. Fahl N. Achieving ultimate anterior esthetics with a new microhybrid composite. Compend Contin Educ Dent. 2000;26(suppl):4-13.
About the Author
Robert A. Lowe, DDS
Private Practice
Charlotte Center for Cosmetic Dentistry
Charlotte, North Carolina