Endodontic Complications of Esthetic Restorative Procedures
Ali Allen Nasseh, DDS, MMSc
Thanks to the mainstream media, the general public is increasingly aware of advances in esthetic dentistry. The availability of a complete smile makeover, as shown on many television shows, has created a sense of need among the public for a younger, brighter, healthier-looking smile. However, restorative procedures that improve a functional but esthetically displeasing smile are not without risk. Not only the esthetics of a case may not turn out to the patient’s full satisfaction, but neuromuscular and pulpal complications associated with such procedures can potentially result in acute and chronic pain and dysfunction. Such unexpected outcomes decrease the patient’s confidence in the rendered care and become a source of frustration for the patient and the dentist. The following case demonstrates the pulpal complications associated with a multiple-unit esthetic reconstruction to correct an occlusal problem. In addition, possible mechanisms of pulpal injury as a result of restorative procedures are reviewed and clinical suggestions are offered to potentially reduce the incidence of such complications.
Clinical Case
A 35-year-old woman was referred to the endodontic office for a consultation and emergency treatment of pain stemming from the maxillary and mandibular anterior area. Her chief complaint was intense pain in the entire upper and lower front teeth. The acute phase of the pain had started 6 weeks earlier, immediately after the definitive cementation of esthetic veneer restorations on teeth Nos. 5 through 12 and 21 through 28. However, the patient described the onset of moderate pain after the initial preparation for the veneers and throughout the provisional phase. She had no symptoms in these teeth before the restorative phase.
At the time of the emergency visit, the patient described intense spontaneous pain, thermal/air sensitivity, and chewing/touch pain, which had increased relentlessly during the past 6 weeks. The pain was localized bilaterally to the front part of the face. The patient’s occlusion was adjusted by the prosthodontist she had been referred to 2 weeks before this emergency visit. At the time of her visit to the prosthodontist, much of the veneers had chipped and fractured incisally. Despite the occlusal adjustment, the pain continued and increased in intensity, reaching a score of 10 on a scale of 0 to 10 during the past week.
During her emergency visit, the patient presented with a thick rope of utility wax covering all surfaces of the maxillary and mandibular anterior teeth and premolars. She was unable to speak because any movement, including opening the mouth and breathing through the mouth, elicited severe pain. She appeared lethargic and under the influence of narcotic pain medication prescribed by her referring dentist.
The patient’s husband described the necessity to turn off all air conditioning, including ceiling fans, at their home because any air flow would trigger intense pain for the patient. She had not been able to chew or eat regular food since the veneer preparations and was experiencing acute weight loss.
The patient recounted a visit to her family dentist 3 months earlier for an orthodontic consultation to straighten some misaligned anterior teeth. The long-standing malpositions had recently become an esthetic concern to her. Upon consultation, her family dentist recommended 16 units of veneers instead of orthodontic treatment to address her chief complaint. It was explained to her that shade improvement and tooth alignment could be addressed concurrently by veneers. She agreed to porcelain veneers on teeth Nos. 5 through 12 and 21 through 28. Preparations were made and the provisional veneers were placed. She claimed discomfort and severe sensitivity during the provisional stage and recalled losing the provisional veneers several times during the interim period. She also described thermal sensitivity during the provisional stage but was told that the symptoms would subside when the definitive restorations were cemented. She described pain and sensitivity throughout the preparation phase of the restorations and multiple injections of anesthetic to control the discomfort intraoperatively.
After final cementation of the veneers, the onset of acute symptoms and subsequent referral to the prosthodontist, the patient was found to be in traumatic occlusion. She manifested anterior occlusion and posterior disclusion in her occlusal plane. To relieve the extreme discomfort caused by this occlusion, the already chipped incisal edges of all of the mandibular veneers were completely ground off to their original occlusal plane, reestablishing the patient’s natural deep overbite. However, despite reestablishment of the original occlusion, the symptoms persisted and continued to increase during the ensuing 2 weeks.
At the time of the emergency visit, clinical testing revealed that all of the patient’s anterior teeth were extremely tender to touch. Even touching the teeth with an explorer elicited a severe pain reaction from the patient. Cold testing triggered intense and delayed pain reactions (longer than 5 minutes) in all of the veneered teeth. The occlusion was deemed not heavy in the anterior sextant and a deep overbite, reminiscent of the original occlusion, was present (Figure 1).
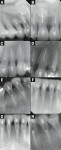
Radiographic examination of the teeth did not reveal any significant radiolucencies at this time. Impacted tooth No. 6 and a retained tooth C were present. All of the anterior teeth appeared free of decay or large interproximal restorations (Figure 2).
Because traumatic occlusion was previously addressed without alleviation of symptoms, it was decided to perform root canal therapy to address the refractory irreversible pulpitis by prioritizing treatment of the teeth with the most extreme responses first. The postoperative response of the other teeth and the patient’s feedback would then be monitored before doing root canal therapy on additional teeth. This treatment plan was designed to prevent unnecessary root canal therapy in the presence of multiple teeth with acute pulpitis, which could cause referred pain symptoms in adjacent teeth
Root canal therapy was first performed in the 4 mandibular incisors, which were extremely tender. Oral sedation with 0.5 mg triazolam and the use of bilateral block and intraosseous anesthesia allowed for complete patient comfort throughout the treatment. Maxillary infiltration anesthesia helped control the symptoms emanating from the maxillary teeth as a result of breathing or contact. To improve efficiency, the EndoSequence nickel titanium files (Brasseler USA, Savannah, GA) and their matching gutta percha cones and glass ionomer sealer were used in a mono-cone technique to complete the mandibular incisors in a single visit.
There was improvement in the patient’s symptoms. However, much of the acute pain still persisted. During the next 2 weeks, the patient made a total of 5 additional visits to address the remaining pain by thorough evaluation and clinical testing first, and receiving root canal therapy in 2 to 3 teeth at a time until the acute pain in her mouth was finally under control. At the end of this acute phase, root canal therapy was performed on 15 of the 16 veneered teeth (Figure 3). Once the root canal therapy and management of the acute pain was established, the patient was referred back to her prosthodontist for proper treatment planning and restoration of the root canal treated teeth and the restoration of a functional occlusion. It was explained to her that the establishment of proper anterior occlusion while addressing the current esthetic concerns would involve additional work on the posterior teeth and alterations of the vertical dimension to compensate for the overbite.
Background
The long-term effects of tooth preparation on pulp vitality and the incidence of pulp necrosis associated with operative procedures have been reported to be 13.3% with full-crown preparations compared with only 5.1% for partial veneer restorations.1 The incidence of pulpal necrosis in crown preparations increases to 17.7% in the presence of a core build-up compared with 0.5% in the control group of unrestored teeth.
Although pulpal complications occur in 5.1% of veneer cases, the acute nature of the symptoms in this case along with the high incidence of pulpal involvement in multiple teeth represents a highly unusual reaction to bonded restorations. It is important to review some of the scientific basis for normal pulp response to injury before making specific recommendations for techniques to avoid them.
Normal Pulpal Response to Injury
Untreated dental caries is the most common cause of pulpal disease; however, among the various forms of dental treatment, operative dental procedures are the most frequent cause of pulpal injury in human teeth.2 Three basic reactions tend to protect against insult to the pulp: (1) a decrease in the permeability of the dentin through dentinal sclerosis; (2) formation of new secondary and reparative dentin; (3) inflammatory and immune reactions in the pulp. The most common response to such localized injury is dentinal sclerosis.3
Dentinal sclerosis has the effect of decreasing dentin permeability, thereby sealing the pulp from potential irritants, such as bacteria and bacterial byproducts. Similarly, secondary and reparative dentin reduces dentinal permeability while creating more distance between the irritant and the pulp.4 Once bacteria or bacterial byproducts reach the pulp, inflammatory and immune reactions further attack and help destroy the antigens.
Pulpal reaction is observed as soon as bacteria reach the dentin.5 It is important to realize that the bacteria do not have to reach the actual pulp before pulpal changes begin taking place. Early changes occur as a response to the diffusion of the inflammatory stimuli into the pulp. Such substances include bacterial toxin, enzymes, antigens, chemotoxins, organic acids, and products of tissue destruction.4 Substances also pass outward from the pulp through the dentinal tubules into the carious lesion. Plasma proteins, immunoglobulin, and complement proteins have been found in carious dentin.6 Therefore, a dynamic interaction between the dentinal surface and the pulp exists at all times. As soon as the dentin is exposed, should the tubules be patent and permeable, an exchange takes place across the dentin, resulting in changes in the pulp.
Dentinal tubules are conical in nature. Therefore, the deeper the dentin is cut, the wider the diameter of the tubules and the larger the permeable area of the surface. Deeper preparations allow for more permeability and therefore a higher chance of bacterial contamination of the pulp.7
Luckily, there is a constant outward flow of fluid in the dentinal tubules, which essentially flushes them clean of such antigens.6 This outward flow is caused by the physiological presence of intrapulpal pressure, the pressure of blood circulating in the pulp and that of pulpal tissues on the walls. In the absence of this flow, a higher incidence of pulpal reactions to surface salivary contamination could potentially occur. Most pulpal reactions are a result of the contamination of the pulp by bacteria or bacterial byproducts.
The Role of Bacteria in Pulpal Injury
Today, we know that the cause of pulpal infection is always bacteria and/or bacterial byproducts. In the landmark study on germ-free mice by Kakehashi and colleagues, the animal’s pulps were completely unaffected despite deep restorations and even pulpal exposures that were left open to the oral cavity (the saliva of such animals contains no bacteria either).8 As long as they were not contaminated with bacteria, the pulps remained vital despite exposure to the oral cavity during a period of several months. In the absence of bacteria, restorative fillings were placed directly into the pulp chamber with very little tissue reaction from the pulp. This study demonstrates the importance of bacteria and bacterial antigens in pulpal reactions and further demonstrates the need for aseptic techniques during operative procedures. Another important study by Bergenholtz and Reit speculated on the cause of postoperative pain and sensitivity.9 In this study, restorative materials that were either bactericidal or prevented bacterial leakage through their margins resulted in the least amount of postoperative sensitivity. In contrast, bacteria were found in histological sections under all the restorative materials where postoperative pain was present. It was therefore proposed that the cause of postoperative pain in restored teeth has little to do with the toxicity of the material itself and more to do with the material’s ability to prevent bacterial leakage.
Acid Etching
Acid etching of dentin to enhance long-term adhesion has been questioned; furthermore, this practice greatly increases dentin permeability, enhancing bacterial penetration of the dentin.10 However, the direct effect of the acid on the pulp appears to be negligible, possibly as a result of the buffering of the acid by intratubular fluids found in dentin. Only in very deep preparations can the actual acid become the primary source of pulpal injury. Therefore, acid etching of dentin is generally not a primary cause of pulpal injury; however, the increased permeability caused by such action could potentially become a source of bacterial conduction into the pulp and be an indirect cause of injury.
Desiccation of Dentin
When freshly cut dentin is dried with a prolonged blast of air, a rapid outward flow of fluids is caused in the dentinal tubules. This fluid can draw along the odontoblasts into the tubules, virtually destroying them in the process.11 However, the desiccation of dentin by operatory procedures or with a blast of air does not injure the pulp.11 There are generally too few cells that die through this process to evoke a significant reaction. Furthermore, odontoblasts that die through this process are replaced by new ones from the cell-rich zone of the pulp, and in 1 to 3 months, reparative dentin is formed.
Thermal Injury
Production of heat during the restorative procedures is the most severe form of stress induced on the pulp.12 Thermal changes leading to pulpal injury can take place as a result of cutting of the dentin and enamel without a coolant and by using dull burs at low revolutions per minute (RPMs) with excessive cutting pressure. Blushing of the teeth during a crown preparation has also been attributed to thermal injury to the pulp. This occurs more readily if a ligamental injection has been used to anesthetize the tooth. The best way to avoid thermal injury of the pulp is by meticulous use of sharp burs at high speed, with light pressure, and adequate water coolant.
Effects of Local Anesthetics on the Pulp
Recent studies have shown the profound effect of vasoconstrictor-containing local anesthetics on pulpal blood flow. Kim and colleagues showed the significant reduction in pulpal blood flow after administration of lidocaine 2% with 1:100,000 epinephrine.13 Because the rate of oxygen use by the pulp is generally low this tissue can withstand a period of reduced blood flow. Research has shown this to be true for periods as long as 3 hours.14
Irreversible pulp damage resulting from tooth preparation is most likely caused by the release of substantial amounts of vasoactive agents, including but not limited to substance P into the extracellular compartment of the underlying pulp.6 During normal circumstances, these vasoactive substances are quickly removed from the pulp by the bloodstream. However, when blood flow to the pulp is drastically decreased or completely arrested, the removal process is greatly delayed and accumulation of these substances and other metabolic waste products may result in permanent damage to the pulp.15 It is therefore recommended to avoid ligamental injections of epinephrine-containing anesthetics in vital but compromised teeth requiring crown preparations.
Discussion
It is true that the exact cause of the severe pulpal reaction in this case may never be fully known. In the absence of dental decay, virgin teeth requiring veneers do not normally suffer irreversible damage from the preparations, even if the cutting is deep into dentin. However, when a combination of potentially caustic factors, such as the use of an epinephrine-containing ligamental injection, deep, heavy cutting into dentin, etching, desiccating, and allowing contamination of the permeable tubules before cementation is followed by traumatic occlusion, the pulps of patients with a lower physiologic compliance and capacity to recover from injury may become irreversibly inflamed. In such situations, multiple root canal therapy and pulpal extirpation may become the only choice to relieve symptoms.
Because the primary cause of postoperative pulpitis is bacterial contamination of the pulp through the dentinal tubules, immediate sealing of the freshly cut dentin with bonding agents may be a potential way of reducing this sensitivity from bacterial leakage.16
In general, the optimal approach to avoid pulpal complications is to avoid ligamental injections containing epinephrine and use sharp burs with light pressure at high RPMs. Using copious water coolant during the operative procedure is also very important to limit heat-induced pulpal injury. Most importantly, aseptic techniques such as using a rubber dam and dentin disinfection during the preparation and cementation of any restoration are of paramount importance. Furthermore, traumatic occlusion should be avoided at all cost in anterior restorations and teeth should be restored with proper posterior support to avoid accumulation and magnification of pulpal symptoms. In itself, occlusal trauma is generally not considered a cause of pulpal necrosis; however, it has been shown to increase neurogenic inflammation and create pulpal symptoms which could put an already inflamed pulp over the edge.17,18
Conclusion
The confluence of several potential factors of pulpal injury makes this case unique. Although each factor on its own is not enough to elicit such severe postoperative pulpal reaction, the combination of multiple factors in this case culminated into severe and irreversible pulpal injury requiring multiple root canal treatments. The primary cause of the pulpitis was probably bacterial in nature; however, the role of occlusion had a magnifying effect on the symptoms.
Each patient is unique and so is his or her individual response to seemingly innocuous treatments recommended by their healthcare professionals. The astute clinician pays close attention to proper case selection to decrease the chance of complications. Adhering to the basic biological and clinical care principals of occlusion and pulpal-periodontal health preservation can further optimize treatment outcome and decrease the chance of potential complications during elective esthetic procedures.
As clinicians, our primary goal should be to do no harm. Our adherence to sound scientific principles and the biological basis of our work can decrease the possibility of untoward treatment outcomes and enhance the quality of our treatment and the satisfaction and service we render our patients.
References
1. Felton D. Long term effects of crown preparation on pulp vitality. J Dent Res. 1989;68:1009. Abstract 1139
2. Brannstrom M, Lind PO. Pulpal response to early dental caries. J Dent Res. 1965;44:1045-1050.
3. Stanley HR, Pereira JC, Spiegel E, et al. The detection and prevalence of reactive and physiologic sclerotic dentin, reparative dentin and dead tracts beneath various types of dental lesions according to tooth surface and age. J Oral Pathol. 1983;12(4):257-289.
4. Bergenholtz G. Pathologic mechanisms in pulpal disease. J Endod. 1990;16(2):98-101.
5. Massler M. Pulpal reaction to dentinal caries. J Dent Res. 1967;17(2):441-460.
6. Okamura K, Maeda M, Nishikawa T, et al. Dentinal response against carious invasion: localization of antibodies in odontoblastic body and process. J Dent Res. 1980;59(8):1368-1373.
7. Pashley DH. Dentin permeability, dentin sensitivity, and treatment through tubule occlusion. J Endod. 1986;12(10):465-474.
8. Kakehashi S, Stanley HR, Fitzgerald RJ. The effects of surgical exposures of pulps in germ-free and conventional laboratory rats. Oral Surg Oral Med Oral Pathol. 1965;20:340-349.
9. Bergenholtz G, Reit C. Reactions of the dental pulp to microbial provocation of calcium hydroxide treated dentin. Scand J Dent Res. 1980;88(3):187-192.
10. Stanley HR, Going RE, Chauncey HH. Human pulp response to acid pretreatment of dentin and to composite restoration. J Am Dent Assoc. 1975;91(4):817-825.
11. Brannstrom M. Communication between the oral cavity and the dental pulp associated with restorative treatment. Oper Dent. 1984;9(2):57-68.
12. Zach L. Pulp liability and repair: effect of restorative procedures. Oral Surg Oral Med Oral Pathol. 1972;33(1):111-121.
13. Kim S, Edwall L, Trobridge H, et al. Effects of local anesthetics on pulpal blood flow in dogs. J Dent Res. 1984;63(5):650-652.
14. Olgart K, Gazelius B. Effects of adrenaline and felypressin (octapressin) on blood flow and sensory nerve activity on the tooth. Acta Odontol Scand. 1977;35(2):69-75.
15. Pashley DH. The influence of dentin permeability and pulpal blood flow on pulpal solute concentrations. J Endod. 1979;5:355-361.
16. Magne P, Urs B. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, Il; Quintessence Publishing; 2002.
17. De Carteret Edlin I. Pulpal necrosis as a sequel to occlusal trauma. Dent Pract Dent Rec. 1970;20(8):282-284.
18. Kvinnsland I, Heyerras K. Effect of traumatic occlusion on CGRP and SP immunoreactive nerve fibre morphology in rat molar pulp and periodontium. Histochemistry. 1992;97(2):111-120.
About the Author
Ali Allen Nasseh, DDS, MMSc
Clinical Instructor, Harvard School of Dental Medicine
Boston, Massachusetts
Assistant Professor, Tufts School of Dental Medicine
Boston, Massachusetts
Private Practice
Boston, Massachusetts