Preplanning for Preparation Design and Material Selection
Matt Roberts
With all of the new restorative material development that has transpired many dentists are uncertain about which material choice is most appropriate for their patient’s clinical situation. They end up selecting a restorative material when the case is already in the laboratory and the teeth have already been prepared—but not necessarily in a way that would be appropriate for the deal material. In many situations this results in the dentist having to make a compromise between material choice and esthetic results. As a profession, we need to expand dentists’ knowledge of the new restorative tools not only so that they can use the materials most beneficial to their patient but also create preparations that are appropriate for the chosen restorative material as well as the patient’s clinical needs.
Step One: The Diagnostic Wax-Up
After orthodontics and/or any necessary periodontal treatment are completed, a diagnostic wax-up is created.
A diagnostic wax-up using an additive-reductive technique, where contour is created by removing tooth structure in over-contoured areas and adding wax in under-contoured areas, defines the minimum amount of tooth surface that needs to be involved restoratively to accomplish the patient’s esthetic and functional goals. A clinician can quickly look at the stone model and see the boundaries of the additive areas in wax and the reductive areas marked in red.If contour changes are minimal, goals may be achieved with direct composite bonding or very conservative veneers combined with cosmetic recontouring of natural teeth and tooth whitening. Insituations where more tooth surface is involved, porcelain veneers or bonded three quarter crowns may best meet the patient’s needs. In many cases we see all of the surfaces of a tooth needing contour modification where full-coverage crowns are indicated. If there are edentulous spaces, implants and some type of fixed bridge are indicated.
Step Two: Determining the Ideal Restorative Material
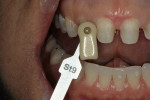
The color and condition of existingdentition as well as strength requirements and delivery modality (bonded or cemented) determine the ideal material choice. With high-strength core materials, there are fixed minimum thicknesses and traditional retentive form preparation designs that are appropriate for all situations. Bonded restorations, however, need to have thickness varied relative to the amount of color change required from the color of the existing underlying tooth structure.
Step Three: Creating the Ideal Preparation for the Chosen Restorative Material
Now that the amount of tooth covered by restorative material has been determined by completing a diagnostic wax-up, and a material has been selected based on existing tooth color, placement modality, and strength requirements, the preparation of the tooth must be done in an appropriate manner for the selected restorative material.
Etched and Bonded Restorations
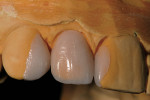
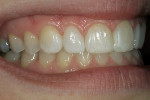
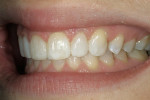
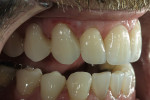
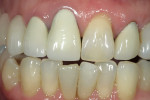
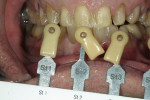
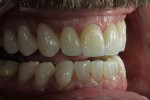
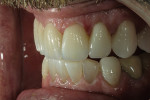
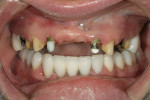
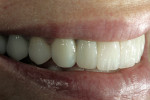
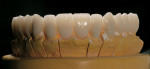
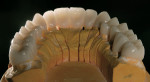
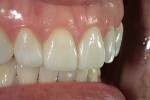
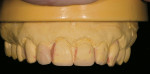
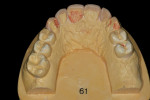
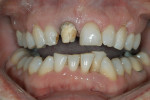
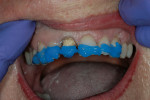
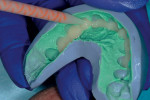
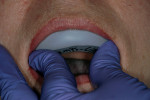
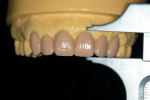
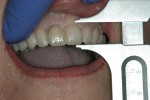
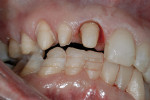
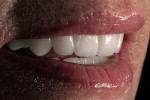
If changes being made to existing tooth contour are additive and the existing color is good, very little reduction of tooth structure is required. The enamel surface can be lightly prepared, and margins can be defined with a shallow chamfer as they extend to the gingival crest. With very limited-coverage restorations, such as interproximal diastema-closure veneers, margins may be left on the facial surface of an anterior tooth. In this situation a feathered margin preparation will facilitate achieving an invisible margin between enamel and ceramic (Figure 1; Figure 2; Figure 3; Figure 4A and Figure 4B).
Where reductive changes in tooth contour are needed, more aggressive preparation is required. The tooth must first be reduced to ideal contour, and then further reducted to allow room for the restorative ceramic.
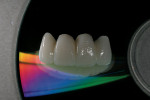
The amount of reduction required in additive or reductive zones depends on the amount of color change needed to achieve the final desired shade as well as the restorative system chosen. Bonded restorations are essentially a filter of underlying color. They achieve a natural appearance by allowing light to circulate through the natural tooth and modify the shade of the underlying dentin and enamel by filtering the color (Figure 5).
The amount of filtration that occurs is determined by the opacity and thickness of the restoration. If we observe a cross-section of a natural tooth, we see that the highest degree of chroma saturation and opacity exist deep within the dentinal structures, while the enamel itself remains a milky translucent layer that filters the underlying color of the dentin (Figure 6). If a great deal of color change is desired but the tooth is prepared too conservatively, opacity must be increased to achieve the desired shade.
Introducing too much opacity near the surface of the restoration inhibits the light circulation that occurs in natural teeth and results in a dead, opaque appearance (Figure 7). However, if the restorative thickness is increased in proportion to the amount of color change desired, a more translucent restorative material can still achieve the desired final shade, but will do so in a way that allows the natural light circulation and lifelike appearance to be achieved (Figure 8; Figure 9A and Figure 9B). This works well as long as the underlying color of the tooth structure stays in a non-offensive shade range.
Feldspathic restorations can be made very thin by using a refractory die technique but if they are less than 0.3 mm, they become difficult to handle without breaking. Pressed ceramic veneers generally require a minimum thickness of 0.6mm to 0.7 mm, although they may be thinned out a little in small areas without creating problems.
Cemented Restorations
When we see blue-black or gray-green colors, a layer of opacity must be used to block them out, then a warm dentine colored ceramic is used to hide the opacity and provide the desired chroma, and finally a layer of enamel-like material is used to filter the dentin ceramics. This sets up a natural system of light circulation and achieves nice esthetics. As expected, this requires quite a bit more room. Although bonded restorations can be used this way, curing the luting resin through an opaque layer is difficult, and the amount of reduction required for esthetic reasons puts the preparation into the dentin layer where adhesion is more difficult. In this situation, a zirconia or alumina core material with conventional resistance-form preparation becomes the material of choice. The ideal preparation for these restorative materials is very similar to that required for porcelain-fused-to-metal restorations. Ideally, 1.3 mm to 1.5 mm thickness on facial, lingual, and proximal surfaces, and 2 mm reduction occlusally in the posterior are desired. Margins should be slightly subgingival, and a shoulder preparation with rounded internal line angles should be used. It is extremely important that shoulder-bevel margins not be used. Because these restorations are designed on a computer and milled with a rotary instrument, sharp corners and sharp angular transitions into which the milling bur cannot reach should be avoided (Figure 10; Figure 11A, Figure 11B, Figure 11C and Figure 11D).
The amount of preparation necessary in any given area is equal to the amount of reduction contour desired plus the amount of restorative thickness necessary to achieve the desired optical results. In areas where additive changes are made, the amount of the additive contour change required is subtracted from the necessary restorative thickness, and the result is the amount of tooth preparation required. By approaching preparation design thiway we achievea situation where the preparations are oriented correctly in the final desired restorative position and there is an appropriate thickness of restorative material to achieve optimal esthetics. If only depth cuts are done into existing teeth without considering the contour changes desired, there may be inadequate reduction to achieve esthetic goals in some areas, and more tooth structure has been taken away than necessary in other areas. Using a silicone matrix created from the diagnostic wax-up can help with the visualization process (Figure 12, Figure 13 and Figure 14).
Mock-up and Preparation through Technique
A technique that simplifies preparation design and optimizes prepared tooth position involves using the silicone provisional matrix made from the wax-up to create a composite mock-up before preparation. To do this it is necessary to consult the additive-reductive wax-up model and locate all of the zones needing reductive contouring, and then in the patient’s mouth, prepare these areas enough so that they do not cause any interference in placing the silicone provisional matrix in the mouth. The teeth are then etched, a composite material is placed in the matrix, and then the matrix is fully seated in the patient’ mouth and allowed to cure, resulting in an intraoral mock-up based on the diagnostic wax-up. Tooth lengths are measured intraorally and compared to the diagnostic wax-up to make sure the matrix was fully seated. A functional and esthetic evaluation may be completed at this time before starting the final tooth preparation. Now depth cuts can be made into the mock-up to a depth that is appropriate for the selected restorative material. This technique results in prepared teeth that are ideally positioned for the final desired restorative position rather than being positioned in the preoperative position. It also prevents over-preparation in areas that are under-contoured preoperatively by covering them with a composite that fills out the tooth to ideal contour before the depth cuts are placed. This technique results in preparations that are ideally positioned for the final restorations, while being as conservative as possible. The amount of reduction needed for the chosen restorative material determines which depth-cutting bur is used. If bonded ceramic restorations are being used, a color evaluation of underlying dentin vs the patient’s desired shade for the final restorations is also considered when choosing the amount of reduction (Figure 15A and Figure 15B; Figure 16A, Figure 16B, Figure 16C, Figure 16D; Figure 17A and Figure 17B; Figure 18; Figure 19).
Conclusion
To provide ideal treatment for our patients, a great deal of preplanning, consultation, and coordination needs to occur with the entire restorative team. Although it may seem like more work up front, using good diagnostic and preparation techniques not only improves the quality of treatment, but actually saves time in the long run by eliminating repeat appointments for repreparation or redoing restorations entirely because the patient is not esthetically satisfied. The added benefit of conservation of tooth structure during treatment is of great value as well.
Acknowledgments
The author would like to acknowledge the clinical work of Dr. Tom Trinker of Columbia, South Carolina, and Dr. John Roberts of Twin Falls, Idaho.
About the Author
Matt Roberts
CMR Dental Lab
Idaho Falls, Idaho