The Use of Resin-Modified Glass Ionomer Liners Under Composite Resins: Should They be Used to Help Control Microleakage?
Gary Alex, DMD
Specific direct resin composites have been shown to be reasonably predictable alternatives to amalgam, assuming they are utilized in the appropriate clinical situation and are properly placed. In fact, the increasing demand for tooth-colored restorations, conservation of tooth structure, and cosmetic dental procedures has encouraged the widespread use of these restorations.1,2
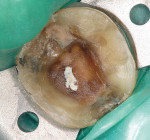
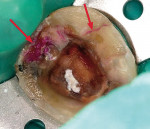
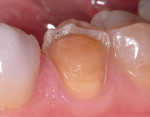
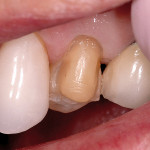
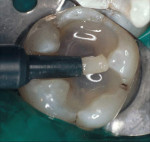
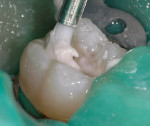
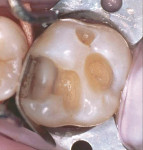
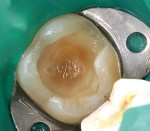
The clinical success of direct composites is due in pbody to material improvements and dramatic advances in adhesive technology.3 However, like all dental restorations, the long-term success of direct composites is contingent upon many factors, including their ability to resist microleakage. Inadequate marginal sealing can contribute to secondary caries, marginal staining, sensitivity, pulpal involvement, breakdown of the adhesive interface, and eventual restoration failure. While current adhesive techniques and materials have the potential to virtually eliminate microleakage at the enamel/restoration interface, consistent and long-term control of microleakage at the dentin/restoration interface is still a significant clinical challenge (Figures 1, Figure 2, Figure 3 and Figure 4).
Dentin vs. Enamel
The reason clinicians can generally bond so predictably to enamel, but not nearly as predictably to dentin, is because of the morphologic, histologic, and compositional differences between the 2 substrates.4 Dentin is a highly variable substrate. Superficial, middle, and deep dentin can be quite different in their structural and chemical composition.5 Enamel, on the other hand, is quite consistent throughout and is also a significantly more mineralized tissue than dentin. The inorganic content of mature enamel is approximately 96% hydroxyapatite by weight, the remainder being water and organic material. Dentin is approximately 70% hydroxyapatite by weight, 18% organic material (mainly collagen), and 12% water.6 These percentages are not consistent and can vary significantly depending upon a number of factors, including dentin depth, age of the teeth, and history of tooth trauma and/ or pathology.7 This, coupled with the relatively high water content of dentin, presents a significant challenge for consistent and reliable long-term bonding. This is not to say that clinicians cannot generate stable and strong initial bonds to dentin. On the contrary, numerous studies have shown that many current adhesive systems are capable of producing bond strengths to dentin that equal or surpass those of acid-etched enamel controls.8-12
The problem is that most of these are short-term studies (i.e., often 24 hours), and clinicians need to think long-term. It is of concern that the literature is replete with longer-term studies (both in vitro and in vivo) that demonstrate a worrisome trend toward eventual breakdown of the dentin/adhesive interface.13-19 The clinical problem of porcelain veneers sometimes de-bonding over time when preparations are largely in dentin (Figures 5 and Figure 6) may be attributed to the variability in bonding to dentin. In contrast, rarely is veneer de-bonding a problem when preparations are largely in enamel.
When a Class II composite fails clinically due to recurrent caries, the failure is rarely at the enamel/restorative interface. This author has observed that it is frequently at the dentin and/or cementum interface with the composite where the failure occurs. While today’s dentin bonding agents have come a long way and are generally very good, perhaps they are not quite as good as we think they are, at least over the long term. Microleakage, nanoleakage, hydrolysis, dentin permeability, pulpal pressure, shrinkage stress, “water tree” formation, insufficient hybrid layer formation, phase separation, dentin tubule orientation, occlusion, enzymes released by bacteria, and operator error have all been implicated as potential causes of deterioration of the dentin/adhesive interface over time.2,15,18,20-25
Minimizing Microleakage and/or Nanoleakage
While it appears there could be many reasons the dentin/adhesive interface might fail, I personally believe that microleakage and/or nanoleakage are of major significance. I have also come to the disappointing conclusion that dentin bonding agents, in and of themselves, cannot predictably prevent long-term microleakage. I do not make this statement lightly. I base my assumption on personal testing, years of careful clinical observation, the reading of hundreds of research papers, and discussions with dozens of friends and colleagues actively involved with adhesive and materials research. Recent and very comprehensive literature reviews by Hilton, DeMunck, and Ferrari strongly support my position.18,26-28
The question then, as it relates to this bodyicle, is: What clinical protocols can help us minimize microleakage when placing direct composites? One common clinical technique thought to reduce microleakage when placing direct composite restorations is the use of flowable composites. With this technique, a flowable composite—which is minimally filled—is placed in a thin layer after a dentin bonding agent has been placed but prior to placing a more heavily filled composite restorative (Figure 7). In principal, flowable composites, by virtue of their low viscosity, are able to get into all of the “nooks and crannies” of the preparation. This may facilitate the adaptation of the higher viscosity composites that are subsequently placed. One could also argue that flowable composites, which have a relatively low modulus of elasticity (i.e., they are flexible), are able to act as stress reducing liners. However, this potential benefit could be offset by increased polymerization shrinkage stress due to the significant amount of unfilled resin found in flowables relative to filler load.29 The literature is equivocal regarding the use of flowables under direct composite restorations in terms of reducing microleakage, with some studies strongly supporting this technique and others showing no benefit.30-35 Irregardless of the research, this technique has been used with generally good success by many dentists, including me. With that said, I personally believe there is yet a better alternative.
My personal belief is that the utilization of resin-modified glass ionomers is the easiest and most predictable way to manage microleakage under direct composites. The literature is replete with in vivo and in vitro studies supporting this belief.35-48 I specifically like resin-modified glass ionomer liners that require no preconditioning of the dentin prior to use (e.g., Vitrebond™, 3M™ ESPE™, St. Paul, MN; Fuji Lining™ LC, GC America, Inc., Alsip, IL). These resin-modified glass ionomer liners have the ability to both micromechanically and chemically interact with dentin.49 They are easy to mix and place, release high sustained levels of fluoride,50 have antimicrobial properties,51,52 have very low solubility,53,54 and have a favorable modulus of elasticity and coefficient of thermal expansion and contraction (i.e., similar to that of dentin).55 There is also anecdotal evidence from clinicians reporting a significant reduction in postoperative sensitivity after switching from flowable composite to resin-modified glass ionomer liners. It is hard to tell if these reports are due to the specific properties of resin-modified glass ionomers or differences in technique sensitivity during placement. The success of a flowable composite’s bond to dentin is highly contingent upon the operator’s ability to first correctly place a dentin bonding agent. A resin-modified glass ionomer such as Vitrebond is placed with no preconditioning of the dentin, so it is much less technique sensitive in this regard. Some other resin-modified glass ionomer restorative materials exist that do require preconditioning of the dentin with a polyacrylic acid derivative for optimal performance.
Suggested Technique
The direct composite placement protocol I recommend and have used successfully for many years is the following:
1. After the preparation is complete, clean the dentin and enamel surfaces with slurry of fine pumice and water. I use disposable Pumice Preppies™ (Whip Mix Corp., Louisville, KY) for this on an ICB® Brush (Ultradent Products, Inc., South Jordan, UT). These small brushes are excellent for getting into the internal aspects of your preparation (Figure 8). I do not recommend the use of an antimicrobial at this point, because in-house studies at 3M ESPE have shown that some antimicrobials may have an adverse effect on the bonding of the resin-modified glass ionomer.56 In any case, the resin-modified glass ionomer to be placed is—in and of itself—antimicrobial.
2. Wash thoroughly with an air/water spray and quick air-dry.
3. Mix and place a thin layer (i.e., .50 mm or so) of Vitrebond. Box areas in Class II restorations (Figure 9) and locations where the external preparation margin ends in dentin and/or cementum are pbodyicularly vulnerable to microleakage and should be addressed. I generally prefer a “closed sandwich technique”; i.e., I leave the resin-modified glass ionomer liner just short of the external margin. I also like to place Vitrebond in deep or uneven areas and often at the dentino-enamel junction (Figures 10 and Figure 11). The material is also useful for blocking out undercuts and/or filling small defects during crown preparation.
4. Light polymerize for 20 seconds. If you feel you missed an area or would like to add more resin-modified glass ionomer, you can do so and light polymerize again.
5. At this point, you can continue with your usual bonding protocol and materials. I personally use a 2-step total-etch system at this juncture. I know I am achieving a good etch of the enamel and the “wet bonding” protocol,57 as it relates to dentin, is much less of a concern because a substantial amount of the dentin is covered by the resin-modified glass ionomer.
Conclusion
The trend in adhesive dentistry has been toward the simplification of adhesive systems and clinical protocol. However, caution is urged because the cost of simplification may be compromise. Long-term bonding to phosphoric acid-etched enamel surfaces has proven to be very reliable and predictable; long-term bonding to dentin is not as predictable, regardless of the adhesive system used. The concept espoused by some that we can consistently create a long-term hermetic seal of the dentin with a dentin bonding agent alone is a myth.3 My suggestion to the busy clinician is to re-visit the use of resin-modified glass ionomers as a way to increase the predictability, comfort, and longevity of direct composite restorations.
References
1. Cosmetic dental services expanding. Dent Prod Rep. 1998;1:34.
2. Allen EP, Brodine AH, Cronin RJ Jr., et al. Annual review of selected dental literature: report of the Committee on Scientific Investigation of the American Academy of Restorative Dentistry. J Prost Dent. 2005;94(2):146-76.
3. Alex G. Adhesive dentistry: where are we today? Compend Contin Educ Dent. 2005; 26(2):150, 152-5.
4. Alex G. Adhesive dentistry in the new millennium. Oral Health. 2000;59-64.
5. Gwinnett AJ. Bonding basics: What every clinician should know. Esthetic Dent Update. 1994;5(2): 35-41.
6. Van Meerbeek B, Lambrechts P, Inokoshi S, et al. Factors affecting adhesion to mineralized tissues. Oper Dent. 1992;Suppl 5:111-24.
7. Pashley DH. Clinical correlations of dentin structure and function. J Prosthet Dent. 1991;66(6):777-81.
8. Miyazaki M, Iwasaki K, Onose H, et al. Enamel and dentin bond strengths of single application bonding systems. Am J Dent. 2001;14(6):361-6.
9. Shear bond strength of Herculite XRV to dentin and cut enamel by 26 adhesives. CRA Newsletter. 2000;24(11):1.
10. Inoue S, Vargas MA, Abe Y, et al. Microtensile bond strength of eleven contemporary adhesives to enamel. Am J Dent. 2003;16(5): 329-34.
11. Inoue S, Vargas MA, Abe Y, et al. Microtensile bond strength of eleven contemporary adhesives to dentin. J Adhes Dent. 2001;3(3): 237-45.
12. De Munck J, Van Meerbeek B, Satoshi I, et al. Microtensile bond strengths of one and two-step self-etch adhesives to bur-cut enamel and dentin. Am J Dent. 2003;16(6):413-20.
13. Hashimoto M, Ohno H, Kaga M, et al. Resin-tooth adhesive interfaces after long-term function. Am J Dent. 2001;14(4):211-5.
14. Gwinnett AJ, Yu S. Effect of long-term water storage on dentin bonding. Am J Dent. 1995; 8(2):109-11.
15. Hashimoto M, Ohno H, Kaga M, et al. In vivo degradation of resin-dentin bonds in humans over 1 to 3 years. J Dent Res. 2000;79(6): 1385-91.
16. Meiers JC, Young D. Two-year composite/ dentin bond stability. Am J Dent. 2001; 14(3):141-4.
17. Okuda M, Pereira PN, Nakajima M, et al. Relationship between nanoleakage and long-term durability of dentin bonds. Oper Dent. 2001;26(5): 482-90.
18. De Munck J, Van Landuyt K, Oeumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84(2):118-32.
19. Koshrio K, Inoue S, Tanaka T, et al. In vivo degradation of resin-dentin bonds produced by a self-etch vs. a total-etch adhesive system. Eur J Oral Sci. 2004;112(4): 368-75.
20. Tay FR, Frankenberger R, Krejci I, et al. Single-bottle adhesives behave as permeable membranes after polymerization. I. In vivo evidence. J Dent. 2004;32(8):611-21.
21. Hashimoto M, Ho S, Tay FR, et al. Fluid movement across the resin-dentin interface during and after bonding. J Dent Res. 2004;83(11): 843-8.
22. Santerre JP, Shajii L, Leung BW. Relation of dental composite formulations to their degradation and the release of hydrolyzed polymeric-resin-derived products. Crit Rev Oral Biol Med. 2001;12(2):136-51.
23. Pashley DH, Tay FR, Yiu C, et al. Collagen degradation by host-derived enzymes during aging. J Dent Res. 2004;83(3):216-21.
24. Finger WJ, Balkenhol M. Practitioner variability effects on dentin bonding with an acetone-based one-bottle adhesive. J Adhes Dent. 1999;1(4):311-4.
25. Purk JH, Dusevich V, Glaros A, et al. In vivo versus in vitro microtensile bond strength of axial versus gingival cavity preparation walls in Class II resin-based composite restorations. J Am Dent Assoc. 2004;135(2):185-93.
26. Hilton, TJ. Can modern restorative procedures and materials reliably seal cavities? In vitro investigations. Pbody 1. Am J Dent. 2002;15(3):198-210.
27. Hilton, TJ. Can modern restorative procedures and materials reliably seal cavities? In vitro investigations. Pbody 2. Am J Dent. 2002;15(4):279-89.
28. Ferrari M, Garcia-Godoy F. Sealing ability of new generation adhesive-restorative materials placed on vital teeth. Am J Dent. 2002; 15(2):117-28.
29. Braga RR, Hilton TJ, Ferracane JL. Contraction stress of flowable composite materials and their efficacy as stress-relieving layers. J Am Dent Assoc. 2003;134(6):721-8.
30. Frankenberger R, Kramer N, Pelka M, et al. Internal adaptation and overhang formation of direct Class II resin composite restorations. Clin Oral Investig. 1999;3(4):208-15.
31. Chuang SF, Jin YT, Liu JK, et al. Influence of flowable composite lining thickness on Class II composite restorations. Oper Dent. 2004;29(3):301-8.
32. Attar N, Turgut MD, Gungor HC. The effect of flowable resin composites as gingival increments on the microleakage of posterior resin composites. Oper Dent. 2004;29(2): 162-7.
33. Leevailoj C, Cochran MA, Matis BA, et al. Microleakage of posterior packable resin composites with and without flowable liners. Oper Dent. 2001;26(3):302-7.
34. Jain P, Belcher M. Microleakage of Class II resin-based composite restorations with flowable composite in the proximal box. Am J Dent. 2000;13(5):235-8.
35. Hagge MS, Lindemuth JS, Mason JF, et al. Effect of four intermediate layer treatments on microleakage of Class II composite restorations. Gen Dent. 2001;49(5):489-95.
36. Sidhu SK, Henderson LJ. In vitro marginal leakage of cervical composite restorations lined with a light-cured glass ionomer. Oper Dent. 1992;17(1):7-12.
37. Wibowo G, Stockton L. Microleakage of Class II composite restorations. Am J Dent. 2001;14(3):177-85.
38. Gupta S, Khinda VI, Grewal N. A comparative study of microleakage below cemento-enamel junction using light cure and chemically cured glass ionomer cement liners. J Indian Soc Pedod Prev Dent. 2002;20(4):158-64.
39. Aboushala A, Kugel G, Hurley E. Class II composite resin restorations using glass-ionomer liners: microleakage studies. J Clin Pediatr Dent. 1996;21(1):67-70.
40. Dietrich T, Kraemer M, Losche GM, et al. Influence of dentin conditioning and contamination of the marginal integrity of sandwich Class II restorations. Oper Dent. 2000;25(5):401-10.
41. Murray PE, About I, Franquin JC, et al. Restorative pulpal and repair responses. J Am Dent Assoc. 2001;132(4): 482-91.
42. Beznos C. Microleakage at the cervical margin of composite Class II cavities with different restorative techniques. Oper Dent. 2001; 26(1):60-9.
43. Besnault C, Attal JP. Simulated oral environment and microleakage of Class II resin-based composite and sandwich restorations. Am J Dent. 2003;16(3):186-90.
44. Aboush YE, Torabzadeh H. Clinical performance of Class II restorations in which resin composite is laminated over resin-modified glass ionomer. Oper Dent. 2000;25(5): 367-73.
45. Retief DH, McCaghren RA, Russell CM. Microleakage of Vitrebond/P-50 Class II restorations. Am J Dent. 1992;5(3):130-2.
46. Sidhu SK, Henderson L. Microleakage of cervical composite restorations lined with light-cured glass ionomers. J Dent Res. 1990;69(4):Abstract #102.
47. Loguercio AD, Alessandra R, Mazzocco KC, et al. Microleakage in class II composite resin restorations: total bonding and open sandwich technique. J Adhes Dent. 2002;4(2):137-44.
48. Guan J, Williams PT, Stockton L. Microleakage in Class II composite restorations. J Dent Res. 2002;81(Special Issue A): Abstract #3360.
49. Yoshida Y, Van Meerbeek B, Nakayama Y, et al. Evidence of chemical bonding at biomaterial-hard tissue interfaces. J Dent Res. 2000; 79(2):709-14.
50. Mitra SB. In vitro fluoride release from a light-cured glass-ionomer liner/base. J Dent Res. 1991;70(1): 75-8.
51. DeSchepper EJ, Thrasher MR, Thurmond BA. Antibacterial effects of light-cured liners. Am J Dent. 1989;2(3):74-6.
52. Scherer W, Lippman N, Kaim J, et al. Antimicrobial properties of VLC liners. J Esthet Dent. 1990;2(2):31-2.
53. Powell LV, Gordon GE, Johnson GH. Clinical comparison of Class V composite and glass ionomer restorations. Am J Dent. 1992;5(5):249-52.
54. Croll TP. Visible light-hardened glass-ionomer cement base/liner as an interim restorative material. Quintessence Int. 1991; 22(2):137-41.
55. Mitra SB, Conway WT. Coefficient of thermal expansion of some methacrylate modified glass ionomers. J Dent Res. 1994;73:218: Abstract #944.
56. Mitra S. Personal Conversation.
57. Kanca J 3rd. Improving bond strength through acid etching of dentin and bonding to wet dentin surfaces. J Am Dent Assoc. 1992;123(9):35-43.
About the Author
Gary Alex, DMD
Private Practice
Huntington, NY