The Team Approach to Esthetic Immediate Implant Placement
Working together as a team, the periodontist and restorative dentist can provide an increased level of treatment outcomes. The team relationship also enhances their professional skills, treatment-planning ability, and the range of procedures, provisionals, and restorations they can offer their patients.
Immediate Placement Pros and Cons
Although it is not always advocated, there is clear evidence that immediate placement of implants can be extremely successful. Lang et al reported a 98.4% survival rate after at least 1 year for implants placed immediately into fresh extraction sockets. Their study reviewed 46 studies, nine of which were greater than 3 years in duration.1
However, in weighing the decision about proceeding with immediate placement on a given patient, there are a number of factors to be considered. Among the positives, immediate placement saves time, procedures, and cost; but most importantly, it preserves the cervical soft-tissue form and papilla form, which simplifies subsequent treatment. Negatives include the risk of infection and interproximal or facial bone loss; plus, there may first be a need for other.comprehensive procedures such as orthodontic therapy. As described by De Rouck,2 esthetic problems can arise with the facial plate related to the predictability of the facial gingival margin. The patient’s biotype and the remaining buccal plate should be considered. These factors and combining an overall comprehensive approach with treatment planning will improve esthetic outcomes with immediate placement.
Immediate Placement: Provisional Options
With good facial tissues and good interproximal tissues supporting the decision to proceed with immediate implant placement, the focus shifts to the provisional, which provides soft-tissue peri-cervical support but does not overload the implant. The problem with using removable retainers is that when they are removed, the cervical soft-tissue support is lost. They are also patient-dependent. A fixed retainer such as an immediate provisional on the implant, a cantilever off an adjacent tooth, or a wire composite splint is more predictable. It can support the facial gingival margin and the papilla. A custom healing abutment can help provide the cervical soft-tissue support using types of provisionals other than immediate implant supported provisionals.
Required Clinical Skills and Techniques
To perform immediate implant placement, practitioners must possess specific skills and be adept at techniques such as being able to perform minimally traumatic extractions—including using vertical extraction system. The clinicians should be able to graft both hard and soft tissues at the time of immediate placement and provide various options of provisionalization that preserve the gingival esthetics.
Vertical extraction of an incisor can be successful much of the time, but other extraction methods are commonly needed, too. These can include resecting the tooth facial-lingually with magnification to preserve the soft tissue and bone. Magnification should be supplied either with high-power loops or a microscope. Generally, magnification can improve surgical results with sharp dissection, minimization of trauma, decreased postsurgical pain, less scarring, and less need for gingivoplasty. Adhering to required surgical principles generally demands microsurgery with magnification—at least 4 to 4.5 times—and light.3 A study that supports healing with microsurgical principles reported on a microsurgical approach to periodontal regeneration. The authors compared incidences of membrane exposure using guided tissue regeneration (GTR) closure in 1995 without microsurgery and in 1999 with microsurgery using a microscope. The authors reported fewer exposures of those gortex membranes with microsurgery.4
Gingival augmentation involving connective tissue grafts (CTG) is typically indicated with esthetic implant sites in immediate implant placement due to facial horizontal dimensional changes that occur; in addition, the lack of alveolar/gingival volume results in titanium shadowing, unesthetic facial depression, and gingival recession. CTGs correct the bucco-lingual resorption in the anterior maxilla with immediate implant placement.
Immediate Implant Placement in the Literature
The literature on extraction sites suggests that immediate implant placement does not make a difference in resorption5 and it is the buccal plate that changes the most.6 A dog study comparing flap versus flapless surgery found 0.5 mm less horizontal facial bone resorption with a flapless protocol; however, there was still 1 mm of buccal plate resorption.7
A randomized blinded 9-year study of single-tooth replacement by immediate implant reported greater keratinized gingival widths, decreased probing depths, and that facial gingival levels were in line with adjacent teeth with CTGs.8
A retrospective study with 85 patients to assess soft-tissue and esthetic outcomes of single-tooth immediate implants placed without flap elevation in maxillary central and lateral incisor sites found that immediate implant placement without elevation of surgical flaps is associated with recession of the marginal mucosa; however, those changes were not seen with CTGs.9
In a 24-patient prospective study using flapless surgery, there was an average loss of volume of 1.063 mm in patients with no grafts and an average gain of 0.34 mm in those with CTGs.10
A prospective randomized study in 50 patients with periapical infected sites reported more gingival recession in the immediately placed implant group than the delayed placement group. No CTGs were placed in either group. The gingival margin was ideal in 61% of the immediate placement group versus 84% of the delayed placement group; 72% of both groups had full regeneration of the papilla.11 If CTGs had been placed in the immediate placement group the recession would not have occurred.
Patient Examples
Management of the following immediate implant cases was determined on a case-by-case basis depending on individual patient indications.
Case 1
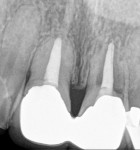
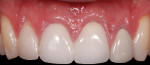
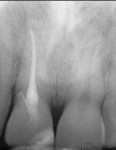
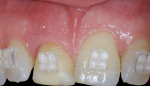
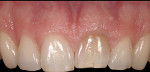
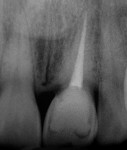
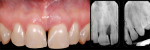
This patient presented with a non-restorable left central incisor due to external root resorption, as shown in the pre-treatment radiograph (Figure 1) and clinical photograph (Figure 2). The patient had good bone levels. The papilla positions were also good, but the cervical margins had some asymmetry with recession on the adjacent teeth. The goal was to preserve the papilla levels and the facial gingival margin level on the central incisors while also improving the gingival levels on the lateral incisors. Due to the patient’s cost concerns, the lateral incisors were not treated except for extending the CTG on the left central incisor only. A custom healing abutment was used to support the peri-cervical soft-tissue form.
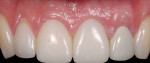
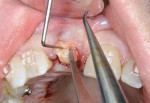
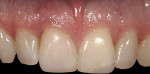
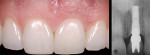
The adjacent central incisor crown was to be replaced, which made it logical to do a cantilever provisional restoration as an interim provisional for the implant. The tooth was extracted in a flapless protocol. The implant was placed; in addition, a CTG was performed using a tunnel approach. Two weeks later, the soft-tissue volume was thick and well preserved. The final lithium-disilicate restorations were cut back and layered; they were opaque enough to mask the darkness of the endodontically treated right central incisor. The CTG resulted in preserving the cervical soft-tissue root prominence and also corrected the recession on the left lateral incisor. The all-ceramic restorations and zirconium abutments made the implant indistinguishable from the adjacent natural tooth (Figure 3).
Case 2
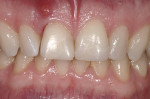
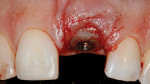
This was an esthetic high-risk case due to extremely high patient expectations and existing distal papilla bone loss. The patient, who had sustained a vertical root fracture of the right central incisor during a snowboarding accident, also presented with a facial fistula at mid-root level (Figure 4 and Figure 5).
The decision was made to use orthodontics to correct the occlusion and tooth position of the adjacent teeth. It was also decided to force erupt the hopeless lateral incisor and central incisor to improve the missing interproximal bone on the distal surface of the incisor. Forced eruption of the incisor also would move the fracture more coronal and create a healthy environment prior to implant placement. Treatment goals were to decrease inflammation and the fistula, overcompensate for recession, and improve osseous levels. The sinus tract progressively decreased as the tooth was force erupted (Figure 6). At the time of immediate placement, a CTG was also performed to preserve the facial ridge profile along with a custom healing abutment (Figure 7).
A provisional was placed on the implant at 3 months, which, like the custom healing abutment, continued to provide soft-tissue support. At 5 years, the gingival health levels were maintained, along with a highly esthetic outcome (Figure 8).
Case 3
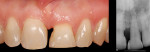
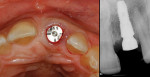
This case involved an ankylosed left central incisor. The patient’s chief complaint was that the incisor was dark and discolored (Figure 9 and Figure 10). Several possibilities were considered, including retaining the tooth or replacing it with an implant. The issue with retaining the incisor concerned the large pulpal canal and the need to aggressively prepare the tooth for a crown in order to mask the dark unesthetic dentin. Another concern was the long-term probability of external root resorption since it was ankylosed. The decision was made to extract and place an implant. The patient had good bone and good soft-tissue positions. The treatment plan was to extract and place the implant with an immediate protocol. The use of an immediate provisional was also considered, but the patient’s deep overbite and his desire to not have to be protective of the implant made the case for doing a bonded provisional. The incision design was done to allow for a facial flap but preserve the papilla. The extraction of the ankylosed incisor required magnification to dissect the tooth from the bone. The implant was placed and the site was grafted with hard and soft tissue. Figure 11 shows the implant, custom healing abutment, CTG, and closure with 7.0 vicryl sutures.
The final soft-tissue form was transferred with the impression by fabricating a custom impression coping, which was made with flowable composite and mimicked the cervical portion of the provisional restoration (Figure 12). The final restoration achieved the patient’s goal of matching the color and esthetic contours with the adjacent teeth. The gingival esthetics were ideal, making the implant undetectable from the natural dentition (Figure 13).
Case 4
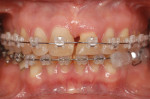
In this case, the patient had a large advanced periodontal defect on the mesial aspect of her left maxillary central incisor, and her central incisors were migrating facially from secondary occlusal trauma and periodontal bone loss (Figure 14). She came in for a second opinion after her restorative dentist recommended removal and immediate implant replacement. The interdisciplinary treatment plan, which involved immediate implant and immediate provisional, was developed with the prosthodontist, periodontist, and orthodontist. Her periodontal disease was not controlled, so nonsurgical periodontal therapy—periodontal fine scaling and root planing with the aid of a perioscope—was completed. Comprehensive orthodontics was then initiated to correct her malocclusion and to force erupt the left central incisor to correct the bony defect (Figure 15 and Figure 16).
After the orthodontic site development, the gingival levels and osseous biotype were ideal. The patient had a thick gingiva/osseous biotype, and the simultaneous use of a CTG with immediate placement was not necessary (Figure 17). The patient had an ideal situation for an immediate provisional—a Class I occlusion and a normal overbite/coupling relationship. The patient was informed not to function on the implant. The provisional at 2 months post-surgery had nice soft-tissue contours (Figure 18).
The final restorative treatment plan will include a porcelain veneer on the right central incisor when the patient has the implant final restoration. The papilla and embrasure space will then be closed. The interdisciplinary plan has resulted in conservative treatment with correction of the malocclusion, the patient’s periodontal disease, and the esthetic replacement of the left central incisor.
Conclusion
Esthetic immediate implants benefit from the interdisciplinary team. Decision-making is optimized with several team members. Using orthodontics along with adjunctive surgical procedures—eg, CTGs—and various provisionals is decided together. The ultimate goal is to achieve as much predictability as possible with each patient. Each case is dictated by the patient’s starting position, and, therefore, each case is managed uniquely. As colleagues evolve together in the team relationship—sharing ideas and information—it not only enhances their clinical skills but also their treatment-planning skills.
References
1. Lang NP, Pun L, Lau KY, et al. A systematic review on survival and success rates of implants placed immediately into fresh extraction sockets after at least 1 year. Clin Oral Implants Res. 2012;23 suppl 5:39-66.
2. De Rouck T, Collys K, Cosyn J. Single-tooth replacement in the anterior maxilla by means of immediate implantation and provisionalization: a review. Int J Oral Maxillofac Implants. 2008;23(5):897-904.
3. Koch K. The microscope. Its effect on your practice. Dent Clin North Am. 1997;41(3):619-626.
4. Cortellini P, Tonetti MS. Microsurgical approach to periodontal regeneration. Initial evaluation in a case cohort. J Periodontol. 2001;72
(4):559-569.
5. Covani U, Cornelini R, Barone A. Bucco-lingual bone remodeling around implants placed into immediate extraction sockets: a case series. J Periodontol. 2003;74(2):268-273.
6. Botticelli D. Berglundh T. Lindhe J. Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontal. 2004;31(10):820-828.
7. Blanco J, Nuñez V, Aracil L, et al. Ridge alterations following immediate implant placement in the dog: flap versus flapless surgery. J Clin Periodontol. 2008;35(7):640-648.
8. Bianchi AR, Sanfilippo F. Single-tooth replacement by immediate implant and connective tissue graft: a 1-9 year clinical evaluation. Clin Oral Implants Res. 2004;15(3):269-277.
9. Chen ST, Darby IB, Reynolds EC, Clement JG. Immediate implant placement postextraction without flap elevation. J Periodontol. 2009;80(1):163-172.
10. Grunder U. Crestal ridge width changes when placing implants at the time of tooth extraction with and without soft tissue augmentation after a healing period of 6 months: report of 24 consecutive cases. Int J Periodontics Restorative Dent. 2011;31(1):9-17.
11. Lindeboom JA, Tjiook Y, Kroon FH. Immediate placement of implants in periapical infected sites: a prospective randomized study in 50 patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(6):705-710.
About the Author
Bobby L. Butler, DDS
Affiliate Faculty Member
University of Washington School of Dentistry
Seattle, Washington
Private Practice,
Seattle, Washington
Greggory Kinzer, DDS
Faculty
Spear Education at the Scottsdale Center for Dentistry
Scottsdale, Arizona
Private Practice
Seattle, Washington