Comparison of Load-Fatigue Performance of Posterior Ceramic Onlay Restorations under Different Preparation Designs
Abstract
OBJECTIVE: The objective of this study was to evaluate the load-fatigue performance of posterior ceramic onlay restorations relative to two variables: preparation design (with or without buccal veneers); and the existing amount of tooth structure (non-worn tooth, worn tooth). METHODS: Sixty extracted third molars were divided into five groups. One group received a mesial-occlusal-distal (MOD) gold onlay restoration (control). The other four experimental groups were prepared for ceramic onlay restorations. Two of the groups additionally received 2-mm occlusal reduction to simulate occlusal wear. All restored teeth were subjected to thermocycling prior to fatigue testing. A fatigue load of 150 N was applied on the occlusal surface at a frequency of 1.2 hz, at an angle of 135 degrees to the long axis of the tooth. Specimen failure was defined as the occurrence of crack propagation in the luting cement layer. This was monitored by the strain gauge on the specimen. RESULTS: All specimens restored on worn tooth had significantly lower fatigue failure cycle counts than those of non-worn tooth. The fracture mode analysis revealed that ceramic fracture tended to be demonstrated only in the group of worn tooth groups. CONCLUSIONS: The addition of a buccal veneer.component had no significant effect on the load-fatigue performance of posterior ceramic onlay restorations, but the existing amount of tooth structure did have a significant effect on the load-fatigue performance of posterior ceramic onlay restorations. Catastrophic failures (ceramic fracture) occurred only in the group of worn tooth.
Keywords: ceramic onlay restoration, cusp-covering restoration, load fatigue, tooth preparation
Dentistry has benefited from tremendous advances in technology, techniques, and materials. While metal restorations have been an outstanding treatment option for posterior teeth—as demonstrated by their
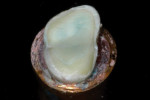
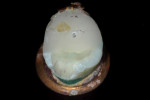
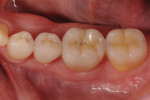
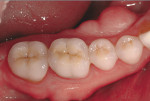
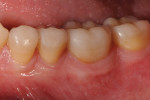
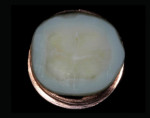
long-term success1-3—their use,.compared to that of metal-ceramic and all-ceramic restorations, has decreased over the past decade due to patients’ interest in tooth-colored restorations. Posterior ceramic onlay restorations are considered to be a conservative treatment modality that provides an esthetic treatment option, as it requires minimal tooth preparation (Figure 1, Figure 2, Figure 3, Figure 4 and Figure 5). Several studies have reported the clinical success rate with posterior ceramic restorations to be between 92% and 97%, with observation periods of up to 5 years,4-8 and 94%9 to 98%10 at the 7-year and 8-year intervals, respectively. Despite their high clinical success rate, various factors—such as the adhesive potential of the remaining tooth structure, tooth morphology, ceramic thickness, aberrant function, and geometry of preparation—can affect the long-term prognosis of restorations. In general, the tooth preparation design of ceramic onlay has been adapted from cast metal preparation designs, with the main alteration being additional occlusal reduction.11 The physical characteristics of ceramic make it very strong in.compression but low in resistance to tension.12 Ceramic onlays are inherently breakable and must rely on adequate bonding to the remaining tooth structure. It is well known that predictable enamel bonding favorably influences the predictability of ceramic onlays. When ceramic restorations were bonded partially to enamel but mostly to dentin, there was an increased risk of restoration failures.13,14
In clinical situations, there may not always be an ideal amount of existing tooth structure. For example, patients exhibiting occlusal attrition and/or erosion present with a loss of occlusal tooth structure. The preparation design on worn teeth does not provide the same anatomic occlusal configuration of enamel and dentin to endorse optimal adhesive bonding. Because the amount of remaining enamel in posterior teeth is proportional to the amount of occlusal reduction required for the tooth preparation, the progressive thinning of enamel may cause more dentin structure to be exposed. In addition, previous studies revealed that tooth preparation design appeared to be the major cause for posterior tooth fracture15; as the width and the depth of the tooth preparation increased, the strength of the remaining tooth structure diminished.16,17
Fatigue failure is a major type of load failure that dental restorations experience in the oral environment.18 The purpose of this study was to evaluate load-fatigue performance of posterior onlay restorations in relation to two variables: 1) preparation designs—with and without a buccal veneer.component; and 2) the existing amount of tooth structure (no-worn tooth and worn tooth). The first null hypothesis held that there would be no difference between the preparation designs with or without a buccal veneer.component on the load-fatigue performance of the posterior ceramic onlay restorations. The second null hypothesis was that the existing amount of tooth structure had no effect on the load-fatigue performance of posterior ceramic onlay restorations.
Materials and Methods
Sixty extracted human third molars were selected on the basis of their relatively large surface areas, as they would resist fracture when stressed and had diverging roots, which resist removal from the embedding acrylic resin during testing. Immediately following the extraction, the teeth were cleaned of surface debris, disinfected in 0.5% sodium hypochlorite, and kept in this liquid until the study was performed. Teeth were then selected from the liquid based on the following criteria: they were intact and lacked cracks or fractures in the crown; they contained no evidence of caries; and they had no prior restorations. The bucco-lingual, mesio-distal, and occluso-cervical dimensions of the teeth were measured using a digimatic caliper accurate to within 0.01 mm (Mitutoyo series 551; Mitutoyo USA, www.mitutoyo.com). Three measurements were made at the greatest bucco-lingual, mesio-distal, and occluso-cervical widths of the specimens, and the averages were determined. Overall, tooth sizes were within a 10% deviation. The roots of the selected teeth were notched for retention with a high-speed handpiece and diamond rotary cutting instrument (KS-1, Brasseler USA, www.brasselerusa.com). The teeth were then attached to a dental surveyor (J.M. Ney Co., www.jmney.com) rod using a sticky wax (Kerr sticky wax, Kerr Dental, www.kerrdental.eu) on a vertically prepared surface so that the long axis of the teeth would be parallel to the surveyor rod. The teeth were lowered into the copper cylinder and positioned in the center of the cylinder with the buccal cementoenamel junction 3 mm above the top of the copper-mounting cylinder. Premixed autopolymerizing resin (Pattern Resin™, GC America Inc., www.gcamerica.com) was injected into the cylinder until it was completely full. After acrylic resin polymerization, the dental surveyor rod was detached and the specimens of teeth were stored in distilled water at room temperature.
The mounted teeth were allocated into five total groups (n = 12); three of the groups were treated as a non-worn occlusal surface and the other two groups were additionally reduced 2 mm at the occlusal surface to simulate occlusal wear. The control group (C) was a mesial-occlusal-distal (MOD) gold onlay. The four experimental groups were: NT—non-worn tooth without a buccal veneer; NT-V—2-mm occlusal reduction on a non-worn occlusal surface, non-worn tooth with a buccal veneer; WT—2-mm occlusal reduction on a non-worn occlusal surface, worn tooth without a buccal veneer; and WT-V—2-mm occlusal reduction on a simulated worn occlusal surface, worn tooth with a buccal veneer (Figure 6). Specimens in group C were prepared with the following principles for cast metal partial coverage restorations19: a 1.5-mm functional cusp and 1-mm non-functional cusp reduction (330MWV, KS7; Brasseler USA); and a 0.5-mm occlusal shoulder on a functional cusp (KS0, KS0F; Brasseler USA). A 2.5-mm isthmus was prepared, and the pulpal floor was prepared to a depth of 2.5 mm from the occlusal cavosurface margin. The bucco-lingual widths on the mesial and distal boxes were similar to the occlusal isthmus width. Each box had a gingival floor width of 1.5 mm mesio-distally and an axial wall height of 2 mm. Finish lines were prepared with 90-degree cavosurface angles. Final beveling and finishing was done with rotary (170L, 169L; Brasseler USA) and hand instrumentation (enamel hatchet, CP ½, Hu-Friedy, www.hu-friedy.com).
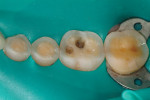
The remaining groups were all prepared for posterior ceramic onlay restorations with the following criteria: group NT and group WT received a 2-mm occlusal reduction, maintaining cusp steepness of 45 degrees relative to the occlusal surface (330MWV, KS7, KS0, KS0F; Brasseler USA). Group NT-V and group WT-V received a 2-mm occlusal reduction, maintaining cusp steepness of 45 degrees relative to the occlusal surface with an addition of a buccal veneer that extended from the mesio-buccal line angle to the disto-buccal line angle. Depth-cutting diamond burs were used to standardize the depth of the veneer preparations so as to achieve a 0.3-mm deep reduction cervically and a 0.5-mm reduction mid-buccally and occlusally. A bevel was added at the junction of the veneer and occlusal reduction (330MWV, KS7, KSO, KSOF, 828—0.3 mm and 0.5 mm; Brasseler USA). All specimens were prepared using a high-speed electric handpiece (KaVo Dental Corp., www.kavo.com) and diamond rotary cutting instrument and carbide burs under cool water irrigation. Following tooth preparation, the thickness of circumferential remaining enamel on the occlusal surface was measured under an optical microscope x10 magnification (Wolfe® Contour Cordless Binocular Microscope, Carolina Biological Supply, www.carolina.com). The four measurements using a digital caliper accurate to within 0.025 mm (Mitutoyo series 551, Mitutoyo USA) on the mid-width of facial, lingual, mesial, and distal were measured, and the average of the remaining enamel thickness were calculated and recorded (Figure 7 through Figure 9).
An impression of each prepared tooth was made with light- and heavy-body polyvinyl siloxane (PVS) impression material (Impressiv™, Cosmodent, www.cosmedent.com) using a dual-phase single-stage technique according to the manufacturer’s instructions. After 24 hours the impressions were poured with a vacuum-mixed die stone (ETI Empire Direct, www.etiempiredirect.com) and allowed to set for 24 hours. The stone cast was recovered and inspected for any defects under x10 magnification. For the gold onlay, one coat of die hardener (Stone Die and Plaster Hardener Resin, George Taub Products and Fusion Co., Inc., www.taubdental.com) was applied to each stone die, and three coats of die spacer were applied to the cavity surfaces, each 8 microns thick (Tru-fit® Die Spacer, George Taub Products and Fusion Co., Inc.). Care was taken to ensure that the finish line was not covered. The gold was cast (AuriumX, Aurium® Research, www.aurium-alloys.com ) using a broken arm-casting machine (Pro-Craft Centrifugal, Grobet, www.deltaonelapidary.com). For the ceramic onlays, two coats of die spacer (Rem-e-die, Ivoclar Vivadent, www.ivoclarvivadent.us) were utilized. A custom pattern was used to provide a standardized notch location on the waxed onlay where the fatigue load was applied. This standardized notch was created on the wax pattern using the specimen’s cementoenamel junction as a standardized reference point and then waxed to 10 mm in total occluso-cervical height. The fatigue load was applied at this notch. The notch simulated a contact point similar to the junction of the central fossa and the most inferior point of the buccal triangular ridge. After waxing, each pattern was transferred back to its working die and the pattern margins refined under x10 magnification. Sprue formers were attached to the patterns with four patterns placed into each investment ring. All of the wax patterns were invested in a phosphate bound investment material for the gold specimens (Ceramigold, Whip Mix, www.whipmix.com) and IPS PressVest Investment Material (Ivoclar Vivadent). Ceramic veneers (IPS Empress®, Ivoclar Vivadent) were pressed according to the manufacturer’s protocol. The burnout furnace cycle (Grobet™ USA, www.grobetusa.com) used a two-stage burnout at 255°C for 30 minutes and up to 848°C with a hold time of 60 minutes. The ceramic investments were transferred to the P 300 ceramic furnace (Ivoclar Vivadent). A pressable ceramic (IPS Empress) was utilized to cast the restorations with VP1989/4 ingot material using a temperature of 915°C and a holding time of 20 minutes. Divestment was performed using 50-micrometer
aluminum oxide airborne particle abrasion at 50 psi. The ceramic onlay fit was verified using green aerosol (Occlude, Pascal International, www.pascalinternational.net) sprayed over the stone die. All restorations were adjusted and refitted to the master dies by removing interferences on the internal aspects of the restorations. High spots on the ceramic onlays were removed using a medium-grit diamond rotary cutting instrument.
Specimen cementation included mechanical debridement using aluminous oxide abrasion (PrepStart, Danville Materials, www.danvillematerials.com) with a particle size of 27 µm at 40 psi at a distance of 2 mm from the tooth surfaces.20 The control group was cemented with zinc phosphate cement (Fleck’s® Zinc Cement, www.pattersondental.com). For the ceramic restorations, the prepared teeth were etched for 15 seconds with 37% phosphoric acid, (Scotchbond™ Etchant, 3M ESPE, www.3MESPE.com) rinsed for 10 seconds, and dried sparingly. The bonding agent (ONE-STEP®, Bisco, Inc., www.bisco.com) was applied to specimens in two coats for 15 seconds and gently air-dried. The intaglio surfaces of the ceramic onlays were treated with 9.5% hydrofluoric acid (Porcelain Etching Gel, Ultradent Products, Inc., www.ultradent.com) for 90 seconds, then silanated with ceramic primer (Scotchbond™ Primer, 3M ESPE). The ceramic onlays were luted with dual-polymerizing. Composite resin cement (RelyX™ ARC, 3M ESPE). The restorations were held in place for the duration of the manufacturer’s commended setting time under finger pressure and simultaneously photopolymerized with a light intensity of 480 nm and a power of 1,100 mW/cm2 (±10%)(Optilux®, Kerr Corp.) for a 5-second burst; then the excess was removed to mimic intraoral conditions. Specimens were then fully polymerized for 40 seconds on all surfaces. The remaining excess was removed with a #12 Bard-Parker™ blade (BD Medical, www.bd.com) and all restoration margins were polished with fine polishing discs (Sof-Lex™, 3M ESPE). The bonded specimens were stored in water at room temperature for 24 hours before thermal cycling. Restored specimens were then thermocycled (RM20, Lauda, Artisan Scientific Corporation, www.artisan-scientific.com) between water temperatures of 5°C and 55°C for 5,000 cycles with a 1-minute dwell time at each temperature to simulate intraoral conditions prior to fatigue testing.
Specimen failure was defined as the point at which preliminary failure or propagation of a crack in or around the luting cement layer occurs. This was monitored by the strain gauge on the specimen. Strain gauge technology has been used to measure changes in tooth deformation or micro-movement of indirect restorations.21-23 The gauge connects as one arm of a Wheatstone Bridge circuit. Voltage output from this circuit is proportional to the movement of the restoration margin in relation to the tooth, as measured by the gauge.22 Amplitude of the strain gauge is small and regular initially, indicating that movement of the ceramic restoration and tooth during loading is elastic. However, as failure in the cement layer or bonding interface is enlarged, the movement increases, and the magnitude goes beyond the detection range of the strain gauge. This point was used as an indication of preliminary failure. A strain gauge (model EA-06-062AP-120 LE, Vishay Precision Group, Inc., www.vishaypg.com) was placed on the palatal surface of the restoration-tooth interface. Luting of the strain gauge was achieved with a strain-gauge adhesive (3M™ Scotch-Weld™ Epoxy Adhesive DP460, 3M ESPE). This process ensured that the strain-gauge grid would be centered over the restoration-tooth interface. The strain-gauge adhesive was allowed to set for a minimum of 24 hours before fatigue testing. Following the set of the adhesive, tray adhesive (Caulk® Tray Adhesive, DENTSPLY Caulk, www.caulk.com) was painted over the strain gauge to ensure water exclusion during the fatigue test. Specimens were tested under fatigue load with a specialized loading machine (Coil Cycler, Proto-Tech, www.proto-tech.com). To closely approximate in vivo loading conditions, each specimen was subjected to a fatigue load of 150 N at a frequency of 72 cycles per minute. The mean of the physiological masticatory force has been reported to be in the range of 100 N to 400 N for the posterior dentition, and the frequency of the loading device, which conforms to the masticatory rate, has been reported to be in the range of 60 to 120 strokes per minute.24 Therefore, the force applied falls with the limits of normal human bite forces and chewing cycles.25 The load was applied at a 135-degree angle to the long axis of the tooth to simulate an appropriate bending motion of the restorations. All specimens were immersed in a room temperature water bath during the fatigue loading. Evidence of preliminary failure was recorded with. Computer software (Data Acquisition System Laboratory, Microstar Laboratories,
www.mstarlabs.com). After a cycle of preliminary fatigue failure was recorded, the specimens were examined under an optical microscope (Wolfe Contour Cordless Binocular Microscope) to examine for failure in the ceramic restorations. Thereafter, the specimens were loaded until catastrophic failure in ceramic restoration was reached. The number of cycles to complete fatigue failure was recorded, and all restorations were inspected under x10 magnification to obtain the failure type. The catastrophic failure was classified in accordance with one of the following mode criteria: an adhesive failure along the ceramic surface (Type I); a mixture of adhesive failure in ceramic and tooth fracture (Type II); a cohesive failure of ceramic fracture at loading area (Type III); and intact restoration (Type IV).
The normality of data distribution of preliminary failure cycle counts was verified using r-program statistical software (www.r-project.org). Then, the numbers of cycles to preliminary failure in all groups were analyzed using the non-parametric Kruskal-Wallis test with Bonferroni correction (α = .05) to evaluate differences among the testing groups. In addition, the relationship between the numbers of cycles to preliminary failure and the amount of circumferential remaining enamel thickness on occlusal surface was analyzed.
Results
The mean values and standard deviation of the number of cycles to preliminary fatigue failure and complete fatigue failure cycles are shown in Table 1. The data distribution of fatigue failure cycle counts revealed non-normality distribution. Therefore, the power of the Kruskal-Wallis tests was computed using the extended average X and Y power estimates.26 It was revealed that the computed power of the present study was 0.85. A significant difference was found among all testing groups with respect to the number of cycles to preliminary failure (P < 0.001). Group C, group NT, and group NT-V had significantly higher preliminary fatigue failure cycle counts than the worn groups, WT and WT-V (P < 0.001). No significant difference was found between groups C, NT, and NT-V. In addition, no significant difference was detected between groups WT and WT-V.
The mean (SD) of the width of circumferential remaining enamel thickness on the occlusal surface were as follows: group NT (1.69 [0.44]), group NT-V (1.53 [0.10]), group WT (0.97 [0.17]), and group WT-V (0.96 [0.11]). An ordinary least squares linear regression model was performed on each group, comparing the amount of circumferential remaining enamel thickness on the occlusal surfaces. Two distinct data clouds resulted when plotted together comparing the group of non-worn tooth and the group of worn tooth. There was a significant linear correlation between the preparation designs and the amount of circumferential remaining enamel thickness on occlusal surfaces (P < 0.05). The fracture mode analysis revealed that ceramic fractures tended to demonstrate in group WT (Figure 10) and group WT-V (Figure 11).
Discussion
Two different existing tooth structures of posterior teeth, a non-worn and a worn tooth group, were evaluated. The second null hypothesis was rejected, as the fatigue failure cycle counts of the group of worn tooth were significantly lower than that of the non-worn tooth. The deterioration of load-fatigue performance of ceramic onlay restorations on worn teeth may derive from a lesser amount of enamel bonding surface. The worn groups demonstrated the thickness of the circumferential remaining enamel at approximately 32% to 49% lower than that of non-worn groups. Enamel is an intrinsically dry substrate, which contains 92% inorganic hydroxyapatite by volume; therefore, an insignificant amount of water is present in the body of the enamel substrate. This prevents water contamination within the monomers when the adhesive materials are photopolymerized.27 Previous studies indicated that decreasing the peripheral enamel seal and the enamel bonding surface caused the deleterious effects of the bonding interface between the restoration and the tooth over time.28,29 If the bonding interfaces have deteriorated, the bond’s ability to transfer stresses from the restoration to the tooth will be less effective. Thus, the fatigue resistance of restorations may be diminished. Enamel structure is a tightly packed mass of hydroxyapatite crystals known as enamel rods. These rods are larger when oriented in their most occlusal position and orientation. As the preparation moves apically through the tooth the rods begin to change orientation and become smaller, and tensile stresses increase. This may have a direct impact on bond predictability.30 The present finding was consistent with previous reports. Another factor that could affect the fatigue performance of the worn tooth was the involvement of compromised dentin structure. The bonding mechanism to dentin is more comeplicated than it is to enamel due to the complex histological structures and variable composition of dentin itself. Dentinal tubules are arranged in organic matrixes that consist primarily of collagen, which is intimately connected with the pulp tissue, and numerous fluid-filled tubules transverse through dentin from the pulp to the dentinoenamel junction.31 Previous studies showed that the bond strength of the restoration to the deep dentin substrate (peritubular) was statistically decreased compared to the superficial dentin (intertubular).32,33 As the occlusal reduction approaches the pulp, the bond strength of dentin might be decreased.
It has been debated whether slow-crack propagation in the ceramic was the primary cause for the failure of the all-ceramic restorations. The strength of ceramic to resist occlusal shear load resulted from a reinforcement bond from the underlying tooth structure. If the reinforcement bond failed, the ceramic would break because of its relatively low flexural strength.21 The present study found that ceramic onlays were intact after preliminary failure occurred, and no cracks in ceramic were found. These ceramic onlays might have failed secondary to adhesive failure of the luting cement. It was also interesting to note that the load fatigue performance of gold onlay restorations with mechanical retentive features performed similarly to the ceramic-bonded onlay restorations on non-worn teeth. The loading machine was stopped at 100,000 cycles, as the significant differences among the testing groups were found within these numbers of cycles. The specimens of gold onlay restorations and a group of non-worn tooth with a buccal veneer were also stopped at this number of cycles. Perhaps, a higher number of cycles may have yielded different results between those two groups. Including a buccal veneer component is a viable alternative clinically to control esthetics, primarily color, and contour. The present study indicated that an addition of a buccal veneer component did not significantly affect the number of cycles to fatigue failure. A buccal veneer component did not enhance adhesion nor reduce the potential for adhesive failure.
There are several limitations to this study. The results of this study are applicable to only the veneering ceramic and luting system that was evaluated. It has been recom mended that occlusal thickness of all-ceramic restorations be 1.5 mm to 2 mm to provide adequate bulk for strength. In the present study, the ceramic thickness of all specimens was in the range of the r.commendation; however, unequal ceramic thicknesses among testing groups developed as a result of different occlusal reductions. All specimens were non-axial load at 135 degrees, which was intended to disadvantage the adhesive bonding interface, thus stressing the adhesive interface and allowing for an increase in the bending moment. The embedding method did not simulate clinical tooth mobility and, therefore, might represent a different biomechanic situation compared to that in the oral cavity. The use of finger pressure to seat the restoration was not standardized; however, this technique is clinically applicable. These influences on parameters need to be considered in future research.
Conclusion
Within the limitations of this in vitro study, the addition of a buccal veneer component had no significant effect on the load-fatigue performance of posterior ceramic onlay restorations, while the existing amount of tooth structure did have a significant effect on the load-fatigue performance of posterior ceramic onlay restorations. Catastrophic failures (ceramic fracture) occurred only in the group of worn tooth.
Clinical Implications
When vertical tooth preparation depth minimizes the amount of circumferential enamel thickness on the occlusal surface and involves compromised dentin structure, ceramic bonded onlay restorations may be contraindicated.
Acknowledgment
The authors would like express their gratitude to Dr. Keith Phillips for his contribution and 3M ESPE and Ivoclar Vivadent for the donation of their materials in this study. The Empress onlays were fabricated at Rory Dental and Technical Art, Seattle, Washington. We are grateful to Mr. Claudio Bucceri and his team for their valuable technical skills. The photographs and drawings were prepared with assistance from Scott Rogerson and Brent Rosenburgh.
Disclosure
The authors received material support from 3M ESPE and Ivoclar Vivadent.
References
1. Donavan T, Simonsen RJ, Guertin G, et al. Retrospective clinical evaluation of 1,314 cast gold restorations in service from 1 to 52 years. J Esthet Restor Dent. 2004;16(3):194-204.
2. Stoll R, Sieweke M, Pieper K, et al. Longevity of cast gold inlays and partial crowns—a retrospective study at a dental school clinic. Clin Oral Investig. 1999;3(2):100-104.
3. Studer SP, Wettstein C, Lehner C, et al. Long-term survival estimates of cast gold inlays and onlays with their analysis of failures. J Oral Rehabil. 2000;27(6):461-472.
4. Fradeani M, Aquilano A, Bassein L. Longitudinal study of pressed glass-ceramic inlays for four and a half years. J Prosthet Dent. 1997;78(4):346-353.
5. Kaytan B, Onal B, Pamir T, Tezel H. Clinical evaluation of indirect resin composite and ceramic onlays over a 24-month period. Gen Dent. 2005;53(5):329-334.
6. Naeselius K, Arnelund CF, Molin MK. Clinical evaluation of all-ceramic onlays: a 4-year retrospective study. Int J Prosthodont. 2008;21(1):40-44.
7. Studer S, Lehner C, Brodbeck U, Scharer P. Short-term results of IPS-Empress inlays and onlays. J Prosthodont. 1996;5(4):277-287.
8. Van Dijken JW, Hasselrot L, Ormin A, Olofsson AL. Restorations with extensive dentin/enamel-bonded ceramic coverage. A 5-year follow-up. Eur J Oral Sci. 2001;109(4):222-229.
9. Felden A, Schmalz G, Federlin M, Hiller KA. Retrospective clinical investigation and survival analysis on ceramic inlays and partial ceramic crowns: results up to 7 years. Clin Oral Investig. 1998;2(4):161-167.
10. Kramer N, Frankenberger R. Clinical performance of bonded leucite-reinforced glass ceramic inlays and onlays after eight years. Dent Mater. 2005;21(3):262-271.
11. Etemadi S, Smales RJ, Drummond PW, Goodhart JR. Assessment of tooth preparation designs for posterior resin-bonded porcelain restorations. J Oral Rehabil. 1999;26(9):691-697.
12. Craig R. Restorative dental materials. 12th ed. St Louis: Mosby;2006:43.
13. Layton D, Walton T. An up to 16-year prospective study of 304 porcelain veneers. Int J Prosthodont. 2007;20(4):389-396.
14. Peumans M, De Munck J, Fieuws S, et al. A prospective ten-year clinical trial of porcelain veneers. J Adhes Dent. 2004;6(1):65-76.
15. Eakle WS, Maxwell EH. Braly BV. Fractures of posterior teeth in adults. J Am Dent Assoc. 1986;112(2):215-218.
16. Mondelli J, Steagall L, Ishikiriama A, et al. Fracture strength of human teeth cavity preparations. J Prosthet Dent. 1980;43(4):419-422.
17. Sheth JJ, Fuller JL, Jensen ME. Cuspal deformation and fracture resistance of teeth with dentin adhesives and composites. J Prost Dent. 1988;60(5):560-569.
18. Braem M, Lambrechts P, Vanherle G. Clinical relevance of laboratory fatigue studies. J Dent. 1994;22(2):97-102.
19. Tucker RV. Class 2 inlay cavity procedures. Oper Dent. 1982;7(2):50-54.
20. Chaiyabutr Y, Kois JC. The effects of tooth preparation cleansing protocols on the bond strength of self-adhesive resin luting cement to contaminated dentin. Oper Dent. 2008;33(5):556-563.
21. Chaiyabutr Y, Phillips KM, Ma, PS, Chitswe K. A. Comparison of load-fatigue testing of ceramic laminated veneer with two different preparation designs. Int J Prosthodont. 2009;22(6): 573-575.
22. Libman WJ, Nicholls JI. Load fatigue of teeth restored with cast posts and cores and complete crowns. Int J Prosthodont. 1995;8(2):155-161.
23. Shor A, Nicholls JL, Phillips KM, Libman WJ. Fatigue load of teeth restored with bonded direct. Composite and indirect ceramic inlays in MOD class II cavity preparations. Int J Prosthodont. 2003;16(1):64-69.
24. Graf H. Bruxism. Dent Clin North Am. 1969;13(3):659-665.
25. Gibbs CH, Mahan PE, Lundeen HC, et al. Occlusal forces during chewing-influences of biting strength and food consistency. J Prosthet Dent. 1981;46(5):561-567.
26. Mahoney M, Magel R. Estimation of the power of the Kruskal-Wallis test. Biometrical Journal (Biometrische Zeitschrift) 1996;38(5):613-630.
27. Koenigswald PL, Clemens WA. Levels of complexity in the microstructure of mammalian enamel and their application in studies of systematic. Scanning Microsc. 1992;6(1):195-218.
28. Abdalla AI, Feilzer AJ. Four-year water storage of a total-etch and two self-etching adhesives bonded to dentin. J Dent. 2008;36(8):611-617.
29. Gamborgi GP, Loguercio A, Reis A. Influence of enamel border and regional variability on durability of resin–dentin bonds. J Dent. 2007;35(5):371-376.
30. Skobe Z, Stern S. The pathway of enamel rods at the base of cusps of human teeth. J Dent Res. 1980;59(6):1026-1032.
31. Pashley D, Okabe A, Parham P. The relationship between dentin microhardness and tubule density. Endo Dent Traumatol. 1985;1(5):176-179.
32. Marques de Melo R, Galhano G, Barbosa SH, et al. Effect of adhesive system type and tooth region on the bond strength to dentin. J Adhes Dent. 2008;10(2):127-133.
33. Sattabanasuk V, Shimada Y, Tagami J. The bond of resin to different dentin surface characteristics. Oper Dent. 2004;29(3):333-341.
About the Authors
Dean E. Kois, DMD, MSD
Private Practice
Seattle, Washington
Yada Chaiyabutr, DDS, MSD, DSc
Affiliate Instructor, Department of Restorative Dentistry
School of Dentistry, University of Washington
Seattle, Washington
Private Practice
Seattle, Washington
John C. Kois, DMD, MSD
Affiliate Professor, Department of Restorative Dentistry
School of Dentistry, University of Washington
Seattle, Washington
Private Practice
Seattle, Washington


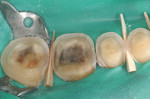


![Figure 9 Figure 9 Schematic representative of an average thickness of circumferential remaining enamel, calculated by measuring the greatest width of each side ([buccal (a) + mesial (b) + lingual (c) + distal (d)]/4).](/media/thumbnail/13167/150x150)